Professional Documents
Culture Documents
Dr. Irbab Hawari
Uploaded by
irbabhmd0 ratings0% found this document useful (0 votes)
36 views25 pagesLecture about COPD and its management comprehensively
Original Title
Copd
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentLecture about COPD and its management comprehensively
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
36 views25 pagesDr. Irbab Hawari
Uploaded by
irbabhmdLecture about COPD and its management comprehensively
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 25
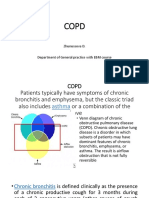
COPD
dr. Irbab Hawari
Symptoms and Signs
• Cough, usually worse in the mornings and
productive of a small amount of colorless
sputum
• Breathlessness: The most significant symptom,
but usually does not occur until the sixth
decade of life
• Wheezing: May occur in some patients,
particularly during exertion and exacerbations
• Hyperinflation (barrel chest)
• Wheezing – Frequently heard on forced and
unforced expiration
• Diffusely decreased breath sounds
• Hyperresonance on percussion
• Prolonged expiration
(in severe disease)
• Tachypnea and respiratory distress with
simple activities
• Use of accessory respiratory muscles and
paradoxical indrawing of lower intercostal
spaces (Hoover sign)
• Cyanosis
• Elevated jugular venous pulse (JVP)
• Peripheral edema
Certain characteristic :
Chronic Bronchitis
• Patients may be obese
• Frequent cough and expectoration are typical
• Use of accessory muscles of respiration is
common
• Coarse rhonchi and wheezing may be heard
on auscultation
• Patients may have signs of right heart failure
(ie, cor pulmonale), such as edema and
cyanosis
Certaim characteristics:
Emphysema
• Patients may be very thin with a barrel chest
• Patients typically have little or no cough or
expectoration
• Breathing may be assisted by pursed lips and
use of accessory respiratory muscles; patients
may adopt the tripod sitting position
• The chest may be hyperresonant, and
wheezing may be heard
• Heart sounds are very distant
Diagnosis
• The formal diagnosis of COPD is made with
spirometry; when the ratio of forced
expiratory volume in 1 second over forced
vital capacity (FEV1/FVC) is less than 70%
• Severity
– Stage I (mild): FEV1 80% or greater of predicted
– Stage II (moderate): FEV1 50-79% of predicted
– Stage III (severe): FEV1 30-49% of predicted
– Stage IV (very severe): FEV1 less than 30% of
predicted or FEV1 less than 50% and chronic
respiratory failu
• Chest radiograph : Emphysema
– Flattening of the diaphragm
– Increased retrosternal air space
– A long, narrow heart shadow
– Rapidly tapering vascular shadows accompanied
by hyperlucency of the lungs
– Radiographs in patients with chronic bronchitis
show increased bronchovascular markings and
cardiomegaly
• Chest Radiograph : Bronchitis
– Chronic bronchitis is associated with increased
bronchovascular markings and cardiomegaly.
Differential Diagnosis
• CHF
• Chronic asthma
Treatment
• The goal of COPD management is to improve a
patient’s functional status and quality of life
by preserving optimal lung function,
improving symptoms, and preventing the
recurrence of exacerbations.
• Diet
Inadequate nutritional status associated with low
body weight in patients with COPD is associated
with impaired pulmonary status, reduced
diaphragmatic mass, lower exercise capacity, and
higher mortality rates.
• Smoking Cessation
• Bronchodilator
Bronchodilators are the backbone of any COPD
treatment regimen. They work by dilating airways,
thereby decreasing airflow resistance. This
increases airflow and decreases dynamic
hyperinflation.
• Beta 2-agonist and cholinergic antagonist
– Beta2-agonist bronchodilators activate specific B2-
adrenergic receptors on the surface of smooth
muscle cells, which increases intracellular cyclic
adenosine monophosphate (cAMP) and smooth
muscle relaxation.
– Anticholinergic drugs compete with acetylcholine
for postganglionic muscarinic receptors, thereby
inhibiting cholinergically mediated bronchomotor
tone, resulting in bronchodilation
• Management of Inflammation
– Steroid is effective in acute exacerbation
– the use of oral steroids in persons with chronic
stable COPD is widely discouraged,
– inhaled corticosteroids should be used only in
conjunction with a long-acting beta agonist.
• Management of infection
– In patients with COPD, chronic infection or
colonization of the lower airways is common from S
pneumoniae, H influenzae, and M catarrhalis. In
patients with chronic severe airway obstruction, P
aeruginosa infection may also be prevalent.
– Empiric antimicrobial therapy is recommended in
patients with an acute exacerbation
– In a study by Daniels et al, the addition to doxycycline
to corticosteroids was found to somewhat improve
treatment for acute exacerbation of COPD (AECOPD).
• Oxygen Therapy and Hypoxemia
Thank You
You might also like
- Zhunussova DDocument18 pagesZhunussova DAnanth Sai BadetiNo ratings yet
- 1 - CopdDocument40 pages1 - Copdvmj8tyh5dsNo ratings yet
- CopdDocument41 pagesCopdneelumshaukatNo ratings yet
- Chronic Obstructive Pulmonary Disease (COPD) : Assistant Professor:Tong JinDocument39 pagesChronic Obstructive Pulmonary Disease (COPD) : Assistant Professor:Tong JinEINSTEIN2DNo ratings yet
- COPD Treatment and Dental CareDocument42 pagesCOPD Treatment and Dental CareAnoos rabayarabayaNo ratings yet
- COPD Chronic Airway DiseaseDocument29 pagesCOPD Chronic Airway DiseaseVivienneNo ratings yet
- Respi CopdDocument90 pagesRespi CopdJosephine IsonNo ratings yet
- Chronic Obstructive Pulmonary Disease: Joshi MarmikDocument27 pagesChronic Obstructive Pulmonary Disease: Joshi MarmikRaj DuraiNo ratings yet
- Chronic Obstructive Lung Disease (COPD) : Is An Obstructive Lung Diseases in Which Irreversible Lung Damage Has OccuredDocument25 pagesChronic Obstructive Lung Disease (COPD) : Is An Obstructive Lung Diseases in Which Irreversible Lung Damage Has OccuredOmar AbdillahiNo ratings yet
- 13.acute Respiratory FailureDocument34 pages13.acute Respiratory Failurekarim hassan100% (1)
- Copd (Chronic Obstructive: Pulmonary Disease)Document68 pagesCopd (Chronic Obstructive: Pulmonary Disease)sinan kNo ratings yet
- Chronic Obstructive Pulmonary Disease: by Abhinay Sharma Bhugoo Ml-610Document62 pagesChronic Obstructive Pulmonary Disease: by Abhinay Sharma Bhugoo Ml-610abhinay_1712No ratings yet
- 16 Martie - Curs BPOC - SlideDocument95 pages16 Martie - Curs BPOC - Slidejonah1024No ratings yet
- COPDDocument41 pagesCOPDsanalcrazy100% (3)
- COPD CaseDocument73 pagesCOPD CaseTony DawaNo ratings yet
- COPD Causes, Symptoms, and TreatmentDocument29 pagesCOPD Causes, Symptoms, and TreatmentsivaNo ratings yet
- Student Copy of COPD Lecture NotesDocument8 pagesStudent Copy of COPD Lecture NotesMary MarshNo ratings yet
- C.O.P.D: (Chronic Obstructive Pulmonary Disorder)Document47 pagesC.O.P.D: (Chronic Obstructive Pulmonary Disorder)KrystelNo ratings yet
- Chronic Obstructive Pulmonary Disease (COPD)Document23 pagesChronic Obstructive Pulmonary Disease (COPD)akoeljames8543No ratings yet
- Asthama & COPDDocument84 pagesAsthama & COPDAbdullah BhattiNo ratings yet
- It 8 Restrictive Pulmonary Diseases - RouDocument43 pagesIt 8 Restrictive Pulmonary Diseases - RoududidumNo ratings yet
- COPDDocument11 pagesCOPDSherree HayesNo ratings yet
- Obstructive Pulmonary DiseasesDocument42 pagesObstructive Pulmonary Diseasesbessan alfqeatNo ratings yet
- Chronic Obstructive Pulmonary Disease (COPD)Document51 pagesChronic Obstructive Pulmonary Disease (COPD)api-19641337No ratings yet
- Week 5 Respiratory EmergencyDocument61 pagesWeek 5 Respiratory EmergencyArmand Bong SantiagoNo ratings yet
- Chest AyuDocument70 pagesChest AyuAbebe GelawNo ratings yet
- Copd by Musa Afridi 17-029Document6 pagesCopd by Musa Afridi 17-029Essa AfridiNo ratings yet
- Gold and Gina Guideline For Copd and AsthmaDocument56 pagesGold and Gina Guideline For Copd and AsthmaSomnath Das GuptaNo ratings yet
- Asma Dan Penyakit Paru Obstruktif KronisDocument34 pagesAsma Dan Penyakit Paru Obstruktif KronisAtikah ArifahNo ratings yet
- Pulmonary EmphysemaDocument20 pagesPulmonary EmphysemaAbigailNo ratings yet
- 4 5850649646552060844Document29 pages4 5850649646552060844mosaNo ratings yet
- CopdDocument47 pagesCopdIsmail AbdulNoorNo ratings yet
- Chapter 4 HTDocument52 pagesChapter 4 HTtesfamichael mengistuNo ratings yet
- Management of COPD: Causes, Symptoms, TreatmentDocument47 pagesManagement of COPD: Causes, Symptoms, TreatmentMegha VadanereNo ratings yet
- Pulmonary Eval Amd LabDocument58 pagesPulmonary Eval Amd LabSara DuranNo ratings yet
- Obstructive Disorders: Dr. Suman SherazDocument45 pagesObstructive Disorders: Dr. Suman SherazSalman KhanNo ratings yet
- Chronic Obstructive Pulmonary DiseaseDocument45 pagesChronic Obstructive Pulmonary DiseaseAlexander Santiago ParelNo ratings yet
- Patient Prep: Follow Guidelines On P. 65 of Clinical PacketDocument4 pagesPatient Prep: Follow Guidelines On P. 65 of Clinical PacketKatherine AmbrosiaNo ratings yet
- CopdDocument89 pagesCopdVijayalaxmi KathareNo ratings yet
- Merged 37Document21 pagesMerged 37abdulkreemsalem4No ratings yet
- Chronic Obstructive Pulmonary Disease: Presented byDocument25 pagesChronic Obstructive Pulmonary Disease: Presented byChinni 12599No ratings yet
- Anaesthesia and CopdDocument7 pagesAnaesthesia and CopdAshish PandeyNo ratings yet
- Pulmonary and Critical Care Medicine In-Training ObjectivesDocument12 pagesPulmonary and Critical Care Medicine In-Training ObjectiveshectorNo ratings yet
- Respiratory Failure Results From Inadequate Gas ExchangeDocument7 pagesRespiratory Failure Results From Inadequate Gas ExchangeJiezl Abellano AfinidadNo ratings yet
- Pulmonary Vascular Disorders and Respiratory FailureDocument5 pagesPulmonary Vascular Disorders and Respiratory FailureTrishia GuillermoNo ratings yet
- Copd PDFDocument28 pagesCopd PDFDarawan MirzaNo ratings yet
- COPD Student Lec DR Atef Alkarn 6-2022Document42 pagesCOPD Student Lec DR Atef Alkarn 6-2022mohamed albnaNo ratings yet
- Asthma and COPDDocument47 pagesAsthma and COPDSamuelVilbrunNo ratings yet
- Copd CalDocument30 pagesCopd Calwheeyycoldandhot55No ratings yet
- Approach To Chronic CoughDocument31 pagesApproach To Chronic CoughNoreen Ooi Zhi MinNo ratings yet
- COPD (Chronic Obstructive Pulmonary Disease)Document16 pagesCOPD (Chronic Obstructive Pulmonary Disease)Maurine OmondiNo ratings yet
- Emphysema Fall 2019Document3 pagesEmphysema Fall 2019Mary MarshNo ratings yet
- Anaesthesia For Patients With COPD: University College of Medical Sciences & GTB Hospital, DelhiDocument76 pagesAnaesthesia For Patients With COPD: University College of Medical Sciences & GTB Hospital, DelhiRINI100% (1)
- DyspneaDocument86 pagesDyspneaJorianditha RamadhanNo ratings yet
- 418-M1-Cu 5 Resp. Emergencies 2Document12 pages418-M1-Cu 5 Resp. Emergencies 2Paradillo Regatuna LesterNo ratings yet
- Dyspnea or Breathlessness Is Defined As The Feeling of An Uncomfortable Need To BreatheDocument33 pagesDyspnea or Breathlessness Is Defined As The Feeling of An Uncomfortable Need To Breatheapi-19641337No ratings yet
- Chronic Illness Module OutcomesDocument12 pagesChronic Illness Module OutcomesOmar IzzoNo ratings yet
- Update MX of COPDDocument60 pagesUpdate MX of COPDNusrat JahanNo ratings yet
- Bronchial HygieneDocument37 pagesBronchial HygieneRayan MohhamadNo ratings yet
- Asthma: Symptoms, Treatments, and Medication for Asthma and BronchitisFrom EverandAsthma: Symptoms, Treatments, and Medication for Asthma and BronchitisNo ratings yet
- Respiratory PhysiologyDocument57 pagesRespiratory PhysiologyirbabhmdNo ratings yet
- Premature EjaculationDocument19 pagesPremature EjaculationirbabhmdNo ratings yet
- Fisiologi NeuronDocument39 pagesFisiologi NeuronMuzayyanatulhayat ARNo ratings yet
- Immunology ReviewDocument14 pagesImmunology ReviewirbabhmdNo ratings yet
- Premature EjaculationDocument19 pagesPremature EjaculationirbabhmdNo ratings yet
- Irbab HawariDocument15 pagesIrbab HawariRatna PermatasariNo ratings yet
- Regulation of Acid Base Balance by The Kidneys: Irbab HawariDocument26 pagesRegulation of Acid Base Balance by The Kidneys: Irbab HawariirbabhmdNo ratings yet
- Regulation of Acid Base Balance by The Kidneys: Irbab HawariDocument26 pagesRegulation of Acid Base Balance by The Kidneys: Irbab HawariirbabhmdNo ratings yet
- Acupuncture in Pain ManagementDocument4 pagesAcupuncture in Pain ManagementfredyNo ratings yet
- Advance Directive (Netről)Document5 pagesAdvance Directive (Netről)dnl60% (1)
- Upcoming Expo in 2023Document4 pagesUpcoming Expo in 2023sandeep DwivediNo ratings yet
- Construction Dust Toolbox TalkDocument2 pagesConstruction Dust Toolbox TalkPravin GowardunNo ratings yet
- Nursing Care Planning (Easy)Document289 pagesNursing Care Planning (Easy)Kim Gomez100% (6)
- Fox Et Al 2022 Dental Extractions Under General Anesthesia New Insights From Process MiningDocument9 pagesFox Et Al 2022 Dental Extractions Under General Anesthesia New Insights From Process Miningmuharrimah rimaNo ratings yet
- FDA Compliance Policy Guides CPG Sec. 555Document2 pagesFDA Compliance Policy Guides CPG Sec. 555Jose LopezNo ratings yet
- 118 A Chapter 2.1 - RESPONSES TO ALTERED VENTILATORY FUNCTION (CARDIOMYOGRAPHY)Document8 pages118 A Chapter 2.1 - RESPONSES TO ALTERED VENTILATORY FUNCTION (CARDIOMYOGRAPHY)Joanna Taylan100% (1)
- Devina Singh 2023 SBA Human and Social BiologyDocument38 pagesDevina Singh 2023 SBA Human and Social BiologyDevina SinghNo ratings yet
- The Effect of Fear Perceptions On Cigarette Pack Image Messages On The Intention To Stop Smoking Students Faculty of Sharia and LawDocument11 pagesThe Effect of Fear Perceptions On Cigarette Pack Image Messages On The Intention To Stop Smoking Students Faculty of Sharia and LawFelysia DianniNo ratings yet
- An Introduction To Basic Medical English Terminology 1Document346 pagesAn Introduction To Basic Medical English Terminology 1bbbanyi100% (2)
- Case Report Serous MeningitisDocument39 pagesCase Report Serous MeningitismissyoanNo ratings yet
- Daftar Pustaka Asma Dan PpokDocument7 pagesDaftar Pustaka Asma Dan PpokJames McmillanNo ratings yet
- Gr4.health Teachers Guide JPDocument196 pagesGr4.health Teachers Guide JPMark Anthony SevilloNo ratings yet
- Barbados Study1994Document9 pagesBarbados Study1994JULIO COLAN MORANo ratings yet
- Normal Labour VIDEO + Module Final (5th June 2020)Document99 pagesNormal Labour VIDEO + Module Final (5th June 2020)Adam Chung100% (1)
- Mylan Vs Biogen '514 Tecfidera IPR InstitutionDocument47 pagesMylan Vs Biogen '514 Tecfidera IPR InstitutionTradeHawkNo ratings yet
- Screening IndustryDocument2 pagesScreening Industryrahaman.maNo ratings yet
- Selexipag 1-29-2016 (Richard Wells)Document49 pagesSelexipag 1-29-2016 (Richard Wells)Aditya MadhavpeddiNo ratings yet
- Health Care Delivery SystemDocument16 pagesHealth Care Delivery SystemUdaya Sree100% (4)
- Medicine CPDProvider v2Document23 pagesMedicine CPDProvider v2PRC Board100% (1)
- Critical Analysis of an OT Field of PracticeDocument5 pagesCritical Analysis of an OT Field of Practicesidney drecotteNo ratings yet
- Foreign and Local Literature on the Global Illegal Drug TradeDocument12 pagesForeign and Local Literature on the Global Illegal Drug TradeAkoo Si EarlNo ratings yet
- Routes of Drug AdministrationsDocument12 pagesRoutes of Drug AdministrationsKena SamuelNo ratings yet
- Respiratory SystemDocument104 pagesRespiratory SystemKatisha JosephNo ratings yet
- Administering Intradermal InjectionsDocument5 pagesAdministering Intradermal InjectionsJustine CagatanNo ratings yet
- OSHA 3110 - Access To Medical and Exposure RecordsDocument8 pagesOSHA 3110 - Access To Medical and Exposure RecordsWahed Mn ElnasNo ratings yet
- HPSP FlyerDocument2 pagesHPSP FlyerHema LaughsalotNo ratings yet
- Diabetic Foot Ulcer and Treatment: A Review of Progress and Future ProspectsDocument6 pagesDiabetic Foot Ulcer and Treatment: A Review of Progress and Future ProspectsEditor IJTSRDNo ratings yet
- Nutrioil Omnibus Product PresentationDocument25 pagesNutrioil Omnibus Product PresentationAngela Aseron DalmacioNo ratings yet