Professional Documents
Culture Documents
ECG - Pacemakers Presentation
Uploaded by
Rofi Irman0 ratings0% found this document useful (0 votes)
18 views55 pagesok
Original Title
Pacemakers 2013 12 -7 (a)
Copyright
© © All Rights Reserved
Available Formats
PPT, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentok
Copyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
18 views55 pagesECG - Pacemakers Presentation
Uploaded by
Rofi Irmanok
Copyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
You are on page 1of 55
Muhammad Diah
Instalasi Kateterisasi Jantung
Cardiology Sub Div, Depart Internal Medicene
RSUD Zainoel Abidin, Banda Aceh
Cardiology Sub Div, Depart Internal Medicene
RSHM Palembang
1
ECG - Pacemakers
2013-12-7. M.Diah 2
*First described in 1952
*Introduced into clinical practice in 1960
*First endocardial defibrillators in 1980
*1991 in USA 1 million people had permanent
pacemakers
*Now
- Approximately 3 million with pacemakers
- Approximately 1 million with ICD device
2013-12-7. M.Diah 3
*Indications
*Basics, Pacemaker Components and Code
*ECG in Pacemaker
2013-12-7. M.Diah 4
*Provides electrical stimuli to cause cardiac
contraction when intrinsic cardiac activity is
inappropriately slow or absent
*Sense intrinsic cardiac electric potentials
* Stimulate cardiac depolarization
* Sense intrinsic cardiac function
* Respond to increased metabolic demand by
providing rate responsive pacing
* Provide diagnostic information stored by the
pacemaker
2013-12-7. M.Diah 7
Clinical Indication
for Pacer
1. Symptomatic bradycardia
2. Symptomatic heart block
- 2
nd
degree heart block
- 3
rd
or complete heart block
- Bifasicular or transfasicular bundle
branch blocks.
3. Prophylaxis
2013-12-7. M.Diah 8
*
*Pulse Generator
*Electronic Circuitry
*Lead System
2013-12-7. M.Diah 9
Lead
Pace
2013-12-7. M.Diah 10
* Subcutaneous or submuscular
* Lithium battery
* 4-10 years lifespan
* long life and gradual decrease in power
sudden pulse generator failure is an
unlikely cause of pacemaker malfunction
2013-12-7. M.Diah 11
PPM
2013-12-7. M.Diah 12
* Sensing circuit
* Timing circuit
* Output circuit
2013-12-7. M.Diah 13
Bipolar
*Lead has both negative,
(Cathode) distal and
positive, (Anode) proximal
electrodes
*Separated by 1 cm
*Larger diameter: more
prone to fracture
*Compatible with ICD
Unipolar
* Negative (Cathode)
electrode in contact
with heart
* Positive (Anode)
electrode: metal casing
of pulse generator
* Prone to oversensing
* Not compatible with
ICD
*current travels only a
short distance
between electrodes
*small pacing spike:
<5mm
2013-12-7. M.Diah 14
+
-
Anode
Cathode
*current travels a
longer distance
between electrodes
*larger pacing spike:
>20mm
2013-12-7. M.Diah 15
-
Anode
Cathode
+
-
2013-12-7. M.Diah 16
I
Chamber
Paced
II
Chamber
Sensed
III
Response
to Sensing
IV
Programmable
Functions/Rate
Modulation
V
Antitachy
Function(s)
V: Ventricle V: Ventricle T: Triggered
P: Simple
programmable
P: Pace
A: Atrium A: Atrium I: Inhibited
M: Multi-
programmable
S: Shock
D: Dual (A+V) D: Dual (A+V) D: Dual (T+I) C: Communicating D: Dual (P+S)
O: None O: None O: None R: Rate modulating
O: None
S: Single
(A or V)
S: Single
(A or V)
O: None
*1
st
letter chamber paced
*2
nd
letter chamber sensed
*3
rd
letter Response to chamber sensed
2013-12-7. M.Diah 18
*AAT
*Paces atria
*Senses atria
*Triggers generator to fire if atria sensed
*VVI
Ventricular Pacing : Ventricular sensing; intrinsic
QRS Inhibits pacer discharge
*VVIR
As above + has biosensor to provide Rate-
responsiveness
2013-12-7. M.Diah 19
*DDD
Paces + Senses both atrium + ventricle,
intrinsic cardiac activity inhibits pacer d/c, no
activity: trigger d/c
*DDDR
As above but adds rate responsiveness to
allow for exercise
*VVI
*Paces ventricle
*Senses ventricle
*Inhibited by a sensed ventricular event
2013-12-7. M.Diah 20
When the need for oxygenated blood increases,
the pacemaker ensures that the heart rate
increases to provide additional cardiac output
Adjusting Heart Rate to Activity
Normal Heart Rate
Rate Responsive Pacing
Fixed-Rate Pacing
Daily Activities
* Wallet card: 5
letter code
* CXR: code visible
* Single lead in
ventricle: VVI
* Separate leads
DDD or DVI
2013-12-7. M.Diah 21
*VVI - lead lies in
right ventricle
*Independent of atrial
activity
*Use in AV conduction
disease
2013-12-7. M.Diah 22
2013-12-7. M.Diah 23
VVI / 60
*Typically in pts with
nonfibrillating atria and
intact AV conduction
*Native P, paced P, native
QRS, paced QRS
*ECG may be interpreted
as malfunction when
none is present
*May have fusion beats
2013-12-7. M.Diah 25
Rate = 60 bpm / 1000 ms
A-A = 1000 ms
AP
VP
AP
VP
V-A AV V-A AV
2013-12-7. M.Diah 26
Atrial Pace, Ventricular Pace (AP/VP)
Atrial Spike
Ventricular Spike
*
Rate = 60 ppm / 1000 ms
A-A = 1000 ms
AP
VS
AP
VS
V-A AV V-A AV
2013-12-7. M.Diah 29
Atrial Pace, Ventricular Sense (AP/VS)
AS
VP
AS
VP
Rate (sinus driven) = 70 bpm / 857 ms
A-A = 857 ms
2013-12-7. M.Diah 30
Atrial Sense, Ventricular Pace (AS/ VP)
V-A AV AV V-A
Rate (sinus driven) = 70 bpm / 857 ms
Spontaneous conduction at 150 ms
A-A = 857 ms
AS
VS
AS
VS
V-A AV AV V-A
2013-12-7. M.Diah 32
Atrial Sense, Ventricular Sense (AS/VS)
*EKG abnormalities due to
*Failure to output
*Failure to capture
*Sensing abnormalities
*Operative failures
*Definition
*No pacing spike present despite indication to
pace
*Etiology
*Battery failure, lead fracture, break in lead
insulation, oversensing, poor lead connection,
cross-talk
*Atrial output is sensed by ventricular lead
*Definition
*Pacing spike is not followed by either an atrial or
ventricular complex
*Etiology
*Lead fracture or dislodgement, break in lead
insulation, elevated pacing threshold, MI at lead
tip, drugs, metabolic abnormalities, cardiac
perforation, poor lead connection
*Oversensing
*Senses noncardiac electrical activity and is inhibited from
correctly pacing
*Etiology
*Muscular activity (diaphragm or pecs), EMI, cell phone
held within 10cm of pulse generator
*Undersensing
*Incorrectly misses intrinsic depolarization and paces
*Etiology
*Poor lead positioning, lead dislodgement, magnet
application, low battery states, MI
Due to pacemaker placement
*Pneumothorax
*Pericarditis
*Perforated atrium or ventricle
*Dislodgement of leads
*Infection or erosion of pacemaker pocket
*Infective endocarditis (rare)
*Venous thrombosis
Pacemaker syndrome
*Patient feels worse after pacemaker placement
*Presents with progressive worsening of CHF symptoms
*Due to loss of atrioventricular synchrony, pathway now
reversed and ventricular origin of beat
*Can interfere with function of pacemaker or
ICD
*Device misinterprets the EMI causing
*Rate alteration
*Sensing abnormalities
*Asynchronous pacing
*Noise reversion
*Reprogramming
Examples
*Metal detectors
*Cell phones
*High voltage power lines
*Some home appliances (microwave)
*Intensity of electromagnetic field decreases inversely
with the square of the distance from the source
*Newer pacemakers and ICDs are being built with
increased internal shielding
*CC: Chills, rigors
*HPI:
*65 yom c/o fevers, chills, rigors x 1 day.
Positive n/v and anorexia. Pt states he
had recent pacemaker insertion 4 days
ago for an arrhythmia.
*PMH:
*HTN
*Arrythmia
*Hypercholesterolemia
*PSHx:
*As stated above
*
*Physical exam
*Temp 101.2, HR 110, BP 90/55
*EKG
*Diagnosis?
*
*Pocket Infection
*Pacemaker insertion is a surgical procedure
*1% risk for bacteremia
*2% risk for pocket infection
*Usually occurs within 7 days of pacemaker
insertion
*May have tenderness and redness over
pacemaker site
*
*CC: SOB
*HPI:
*65 yom states he had onset of shortness
of breath and left sided pleuritic chest
pain. Pt states he awoke with pain and
difficulty breathing. Had pacemaker
placed yesterday.
*PMHx:
*HTN, Diabetes, Hypercholesterolemia,
Arrythmia, CAD
*PSHx:
*Pacemaker, left knee surgery, b/l
cataract
*
*Physical Exam
*BP 146/85, HR 80s, RR 30s, O2 Sat 88%
*Lungs
* Decreased breath sounds on left
*EKG
*Diagnosis?
*
*Pneumothorax
*Occurs during cannulation of central veins
*Incidence
*Cardiologist dependent
*Treatment
*Small or asymptomatic observation
*Large or symptomatic Chest tube
*
*CC: Cardiac arrest
*HPI: 59 yom found on couch. Wife states they
were watching TV when patient let out a moan
and then became unconscious. She states, he
has a bad heart and had something put in a
few years ago.
*PMHx: unknown
*Meds: bottles in bathroom
*
*Physical Exam
*Airway patent, no visible chest rise, no
pulses
*Generally: cool, clammy, diaphoretic
*EKG:
*Diagnosis?
*
*Cardiac Arrest with ICD (V-fib)
*2% annual incidence with ICD
*Etiology
*ICD delivered predetermined shocks for
identified event and patient failed to respond
*ICD failed to recognize event and failed to shock
appropriately
* Failure to sense, lead fracture, EMI, inadvertent ICD
deactivation
*
*Cardiac Arrest with ICD
*Treat using ACLS protocols
*Secure airway
*CPR
*Defibrillate/shock as warranted
* Keep sternal pad 10 cm away from pulse generator
*Meds
You might also like
- How Your Diet Affects Your BrainDocument2 pagesHow Your Diet Affects Your BrainRusso Dalmasso50% (2)
- Temporary PacemakerDocument35 pagesTemporary Pacemakerromeorobin07No ratings yet
- Introduction To Electrophysiology: What Are They DOING Over There?!Document51 pagesIntroduction To Electrophysiology: What Are They DOING Over There?!Mahendrakumar ManiNo ratings yet
- IndicationsDocument3 pagesIndicationsAbubakr ElsediqqNo ratings yet
- Sistem Medis Berbasis Komputer: ElectrocardiographyDocument34 pagesSistem Medis Berbasis Komputer: ElectrocardiographywendraNo ratings yet
- Pacemaker.docxDocument5 pagesPacemaker.docxMuhammad Umer SaeedNo ratings yet
- Day 3 - APPEC 2021Document413 pagesDay 3 - APPEC 2021GaurieNo ratings yet
- Anaesthesia Management of Patient of PacemakerDocument92 pagesAnaesthesia Management of Patient of PacemakerSiva KrishnaNo ratings yet
- PacemakerDocument52 pagesPacemakerPraveena RNo ratings yet
- Chapther 2122Document11 pagesChapther 2122Masia Angela Miranda CollantesNo ratings yet
- Cardiac Implantable Electronic DevicesDocument49 pagesCardiac Implantable Electronic DevicespriyathasanNo ratings yet
- Guide to Cardiac Pacemaker Indications and ImplantationDocument23 pagesGuide to Cardiac Pacemaker Indications and ImplantationMonica Trifitriana100% (1)
- 20 Blok 15 Tahun 2015 SVT DysrrhytmiasDocument69 pages20 Blok 15 Tahun 2015 SVT Dysrrhytmiaswarriordc1995No ratings yet
- Sugiyono, S.Kep., Ners., M.KepDocument48 pagesSugiyono, S.Kep., Ners., M.KepHervin RamadhaniNo ratings yet
- Ekg NersDocument42 pagesEkg NerstaufikbaesajaNo ratings yet
- TB causes constrictive pericarditis, diagnosis via echocardiographyDocument24 pagesTB causes constrictive pericarditis, diagnosis via echocardiographyAli SohailNo ratings yet
- Cardiac DysrhythmiasDocument9 pagesCardiac DysrhythmiasMandy JameroNo ratings yet
- Heart Disease: Understanding ArrhythmiaDocument9 pagesHeart Disease: Understanding ArrhythmiaDayasoruban SanmugamNo ratings yet
- Cardiac Catheterization: Pacemaker, Rfa, Nerve Block: Sehrish ManzoorDocument32 pagesCardiac Catheterization: Pacemaker, Rfa, Nerve Block: Sehrish ManzoorZainNo ratings yet
- Cardiac pacing guide for beginnersDocument89 pagesCardiac pacing guide for beginnerssandwhale056No ratings yet
- Introduction Definition: Types of PacemakersDocument8 pagesIntroduction Definition: Types of PacemakersPrasann RoyNo ratings yet
- Case Study on Pacemakers: How They Work and Their BenefitsDocument6 pagesCase Study on Pacemakers: How They Work and Their BenefitsBalamuruganNo ratings yet
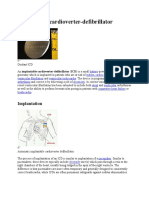
- Implantable CardioverterDocument5 pagesImplantable CardioverterpratonyNo ratings yet
- PACING ASSESSMENTDocument4 pagesPACING ASSESSMENTRuba RizikNo ratings yet
- ElectrocardiographyDocument4 pagesElectrocardiographyJho BuanNo ratings yet
- Plante PacemakersDocument57 pagesPlante Pacemakersdragon66No ratings yet
- 12 Lead ECG - DX TestDocument1 page12 Lead ECG - DX Testsnivelb3No ratings yet
- SBM1403 unit1Document64 pagesSBM1403 unit1Balasaraswathi SNo ratings yet
- Heart Defect PDFDocument6 pagesHeart Defect PDFRosemaryCastroNo ratings yet
- Temporary Pacemaker Settings and CareDocument51 pagesTemporary Pacemaker Settings and Carewaqas_xsNo ratings yet
- PacemakersDocument22 pagesPacemakersapi-3757838No ratings yet
- Peri-Operative Cardiac Arrhythmias - Part 1Document14 pagesPeri-Operative Cardiac Arrhythmias - Part 1jhonjrodriNo ratings yet
- A Review On Pacemakers: Device Types, Operating Modes and Pacing Pulses. Problems Related To The Pacing Pulses DetectionDocument12 pagesA Review On Pacemakers: Device Types, Operating Modes and Pacing Pulses. Problems Related To The Pacing Pulses DetectionsdekapureNo ratings yet
- Cardiac Arrhythmias in ChildrenDocument50 pagesCardiac Arrhythmias in ChildrenNorhafizah AhmadNo ratings yet
- ECG Intro With Ref To QT Interval FinalDocument59 pagesECG Intro With Ref To QT Interval FinalGeorge VergheseNo ratings yet
- ECG in Emergency MedicineDocument228 pagesECG in Emergency MedicineBobbyGustafsonNo ratings yet
- Arrhythmias - : Normal HeartbeatDocument4 pagesArrhythmias - : Normal HeartbeatToni Baskoro KristantoNo ratings yet
- Pace MakerDocument9 pagesPace MakerTridib RNo ratings yet
- Heart Sounds, Pacemakers & DefibrillatorsDocument28 pagesHeart Sounds, Pacemakers & DefibrillatorsJack OneNo ratings yet
- Main Applications of ECG DiagnosisDocument19 pagesMain Applications of ECG DiagnosisMaria Rowena O. SalvoNo ratings yet
- EKG Interpretation NursingDocument14 pagesEKG Interpretation NursingTanya ViarsNo ratings yet
- Supplementary Material 4.3 Cardiac Rhythm Disorders-2Document14 pagesSupplementary Material 4.3 Cardiac Rhythm Disorders-2Andrea Love PalomoNo ratings yet
- (Corrected) Cardiac Monitoring and DefibrillatorDocument28 pages(Corrected) Cardiac Monitoring and DefibrillatorConrad DaabuNo ratings yet
- Pacemaker InformatiiDocument4 pagesPacemaker InformatiiAndreea MitranNo ratings yet
- Electrocardiogram: Click To Edit Master Subtitle StyleDocument49 pagesElectrocardiogram: Click To Edit Master Subtitle StyleJaily O. MarianoNo ratings yet
- PacemakerDocument24 pagesPacemakerLAWKUSH KUMARNo ratings yet
- Cardiac Pacing For The SurgeonsDocument46 pagesCardiac Pacing For The SurgeonsRezwanul Hoque BulbulNo ratings yet
- Engineering College Medical Electronics Unit Explains Types of PacemakersDocument20 pagesEngineering College Medical Electronics Unit Explains Types of PacemakersMohammed Mian ANo ratings yet
- Permanent Pacemaker: Supervisor: DR Pipin Ardhianto SPJP (K), FihaDocument67 pagesPermanent Pacemaker: Supervisor: DR Pipin Ardhianto SPJP (K), Fihapelantikan ppnirsdkNo ratings yet
- Major Project Phase 1 Report CloudDocument35 pagesMajor Project Phase 1 Report CloudPraj CNo ratings yet
- The Heart'S Conduction System and "Natural Pacemaker "Document8 pagesThe Heart'S Conduction System and "Natural Pacemaker "merin sunilNo ratings yet
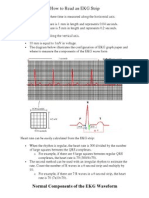
- How To Read An EKG StripDocument9 pagesHow To Read An EKG StripRavi PandeNo ratings yet
- Normal Sinus RhythmDocument13 pagesNormal Sinus RhythmJackson Yovin ChellyadhasNo ratings yet
- Sinus Node Blocks DiagnosticDocument48 pagesSinus Node Blocks DiagnosticOlga GoryachevaNo ratings yet
- ECT Pacemaker 2004Document7 pagesECT Pacemaker 2004Cindra ElvanNo ratings yet
- DR Amao Core Principles of Interpreting Ecg TracingDocument39 pagesDR Amao Core Principles of Interpreting Ecg Tracingdan ekelemeNo ratings yet
- Electrocardiogram (ECG or EKG) : Danilyn R. Cenita Paula M. PauloDocument41 pagesElectrocardiogram (ECG or EKG) : Danilyn R. Cenita Paula M. PauloDhanNie CenitaNo ratings yet
- Ecg Basic ConceptsDocument18 pagesEcg Basic ConceptsDaniel SolonyaNo ratings yet
- Ccu Survival GuideDocument10 pagesCcu Survival Guideomegasauron0gmailcom100% (1)
- Spring 2014 NewsletterDocument5 pagesSpring 2014 Newsletterapi-236445988No ratings yet
- ECG/EKG Interpretation: An Easy Approach to Read a 12-Lead ECG and How to Diagnose and Treat ArrhythmiasFrom EverandECG/EKG Interpretation: An Easy Approach to Read a 12-Lead ECG and How to Diagnose and Treat ArrhythmiasRating: 5 out of 5 stars5/5 (2)
- Polymyalgia RheumaticaDocument26 pagesPolymyalgia RheumaticaRofi IrmanNo ratings yet
- Chronic Kidney Disease: Rizki Aliana AgustinaDocument85 pagesChronic Kidney Disease: Rizki Aliana AgustinaRofi IrmanNo ratings yet
- Latinis, K., Et Al: The Washington Manual Rheumatology Subspecialty Consult., LWWDocument18 pagesLatinis, K., Et Al: The Washington Manual Rheumatology Subspecialty Consult., LWWRofi IrmanNo ratings yet
- Defining Arthritis: Arth + It IsDocument82 pagesDefining Arthritis: Arth + It IsRofi IrmanNo ratings yet
- Skill Lab CT-Scan Technique and InterpretationDocument137 pagesSkill Lab CT-Scan Technique and InterpretationRofi Irman100% (1)
- Guidelines Valvular Heart Dis FTDocument46 pagesGuidelines Valvular Heart Dis FTIsman SandiraNo ratings yet
- Defining Arthritis: Arth + It IsDocument82 pagesDefining Arthritis: Arth + It IsRofi IrmanNo ratings yet
- Polymyalgia.H SDocument33 pagesPolymyalgia.H SRofi IrmanNo ratings yet
- Unusual Case of Tuberculous Pleural Effusion and Abdominal MassDocument4 pagesUnusual Case of Tuberculous Pleural Effusion and Abdominal MassRofi IrmanNo ratings yet
- Hepatitis AutoimunDocument32 pagesHepatitis AutoimunRofi IrmanNo ratings yet
- Chronic Kidney Disease: Rizki Aliana AgustinaDocument85 pagesChronic Kidney Disease: Rizki Aliana AgustinaRofi IrmanNo ratings yet
- Hematemesis PDFDocument7 pagesHematemesis PDFkevin_jawanNo ratings yet
- HemangiomaDocument16 pagesHemangiomaRofi IrmanNo ratings yet
- Bahan Refrat2 PAI 7Document78 pagesBahan Refrat2 PAI 7Rofi IrmanNo ratings yet
- Disseminated Intravascular Coagulation: Treat The Cause, Not The Lab ValuesDocument9 pagesDisseminated Intravascular Coagulation: Treat The Cause, Not The Lab Valuesboris_beroizaNo ratings yet
- VWDDocument126 pagesVWDAlfian Rizki MaulanaNo ratings yet
- PsioriasisDocument8 pagesPsioriasisRofi IrmanNo ratings yet
- PsioriasisDocument8 pagesPsioriasisRofi IrmanNo ratings yet
- DEMO, SXGA, MP90, Initial, D.0x.xx, Rev XXXDocument25 pagesDEMO, SXGA, MP90, Initial, D.0x.xx, Rev XXXahmadba70No ratings yet
- The Conceptualization of Emotions Across Cultures: A Model Based On Interoceptive NeuroscienceDocument14 pagesThe Conceptualization of Emotions Across Cultures: A Model Based On Interoceptive NeurosciencepartoNo ratings yet
- February Month Brain DiscussionDocument63 pagesFebruary Month Brain DiscussionJulyhathul KuraishiNo ratings yet
- Growth and DevelopmentDocument21 pagesGrowth and DevelopmentKarl Sean UbinaNo ratings yet
- Adaptasi Biota LautDocument19 pagesAdaptasi Biota LautBudhi Agung Prasetyo100% (1)
- Cranial NervesDocument118 pagesCranial NervesGan'sNo ratings yet
- KIT CD117 A Review On Expression in Normal and Neoplastic TissuesDocument16 pagesKIT CD117 A Review On Expression in Normal and Neoplastic TissuesVlado VladNo ratings yet
- Veta 3 - Datasheet - ENG - 20210315Document2 pagesVeta 3 - Datasheet - ENG - 20210315JuanNo ratings yet
- Identify The Part of The BrainDocument2 pagesIdentify The Part of The BrainClement Mar ClimacoNo ratings yet
- The Digestive System ExplainedDocument20 pagesThe Digestive System ExplainedRoy JarlegoNo ratings yet
- 22.3 Anatomy Study Resources - A PDFDocument3 pages22.3 Anatomy Study Resources - A PDFNothingNo ratings yet
- Animal KingdomDocument30 pagesAnimal KingdomRupa MitraNo ratings yet
- Hematological and Metabolical Aspects From Laboratory MediDocument109 pagesHematological and Metabolical Aspects From Laboratory MediNadirNo ratings yet
- Course Outline For 125:355, Physiological Systems For Biomedical EngineersDocument2 pagesCourse Outline For 125:355, Physiological Systems For Biomedical EngineersbillNo ratings yet
- Levels of Organization Power Point and ActivityDocument8 pagesLevels of Organization Power Point and ActivityJudy RianoNo ratings yet
- Ed 4 PHARMACOGNOSY PDFDocument52 pagesEd 4 PHARMACOGNOSY PDFShubham Sabale PatilNo ratings yet
- Biological Effects of Microwaves and Radio Frequency RadiationDocument25 pagesBiological Effects of Microwaves and Radio Frequency RadiationMichael Janitch100% (2)
- The Problem and Its BackgroundDocument43 pagesThe Problem and Its BackgroundkjjkjkljkjjklNo ratings yet
- Ectopic Case StudyDocument38 pagesEctopic Case StudyMicah LangidenNo ratings yet
- TonsillectomyDocument27 pagesTonsillectomyRho Vince Caño MalagueñoNo ratings yet
- Charnley Ankle ArthrodesisDocument12 pagesCharnley Ankle Arthrodesisdr_s_ganeshNo ratings yet
- HRM4 Run Instructions ML12Document26 pagesHRM4 Run Instructions ML12igidaNo ratings yet
- Dental and anesthesia procedures and equipmentDocument56 pagesDental and anesthesia procedures and equipmentVijay RanaNo ratings yet
- Molecules of Life: Carbs, Lipids, Proteins & EnzymesDocument102 pagesMolecules of Life: Carbs, Lipids, Proteins & Enzymeskavya nandhiNo ratings yet
- Case StudyDocument6 pagesCase StudySarah McKayNo ratings yet
- Rheumatic Heart Disease PathophysiologyDocument3 pagesRheumatic Heart Disease Pathophysiologyjethro sanchez100% (1)
- Photo Chemistry of VisionDocument107 pagesPhoto Chemistry of VisionPhysiology by Dr Raghuveer100% (1)
- Enls V 4 0 Protocol Coma FinalDocument16 pagesEnls V 4 0 Protocol Coma Finalsucipto suciptoNo ratings yet
- Overview of Nervous SystemDocument63 pagesOverview of Nervous SystemMAHARANI100% (1)