Professional Documents
Culture Documents
ANFIS GINJAL, Herianto
Uploaded by
Rofi Irman0 ratings0% found this document useful (0 votes)
44 views82 pagesmedical
Copyright
© © All Rights Reserved
Available Formats
PPT, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentmedical
Copyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
44 views82 pagesANFIS GINJAL, Herianto
Uploaded by
Rofi Irmanmedical
Copyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
You are on page 1of 82
Herianto
DIVISI GINJAL HIPERTENSI
DEPARTEMEN PENYAKIT DALAM FK UNSRI/RSMH
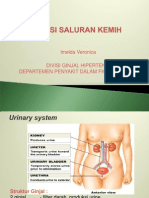
Struktur Ginjal :
2 ginjal - filter darah, produksi urine
2 ureter - transpor urine (ginjal ke bladder)
bladder - reservoir of urine
uretra - transpor urine
letak retroperitoneal, pd
dinding posterior
abdominal
Terletak dari T12-L3
vertebral columna,
disamping m. psoas
major
Bagian superior
dilindungi iga 11, 12
Ginjal kanan lebih
rendah dari kiri (karena
terdapat lobus kanan
hepar)
Ukuran 12 x 5 x 2,5 cm
Berat 150 gram
Seperti kacang, warna
merah coklat
kidney levels berubah
sewaktu respirasi dan
perubahan postural
1. renal fascia (outer)
flexible, pergerakan ginjal
saat respirasi
Ditutupi oleh lapisan lemak
2. perirenal fat (middle layer)
protective cushion
3. renal capsule (innermost)
Lapisan serat kolagenbarrier
thd trauma, infeksi dsb.
Martini p 953
Luar; korteks, dalam:
medulla
6-18 conical renal
pyramids
apex - renal papilla
projects into the renal
sinus
renal columns
extend from cortex
inward to renal sinus
between adjacent renal
pyramids
granular texture similar
to that of the cortex
ureter masuk ke sinus
renalismeluas ruang-
renal pelvis
pelvis bercabang 2-3
major calyces 6-8
minor calyces
Tiap minor calyx terdapat
papilla pyramid renalis
Duktus di papilla
menghubungkan dinding
calyx dan hasil urine dari
korteks
Urine melalui calyces
menuju ureter
Berasal dari aorta abdominalis, arteri renalis masuk ke hilus
ginjal dan bercabang:
1. Arteri interlobaris- melewati renal columns and reach
junction between medulla and cortex
2. Arteri arkuata melengkung, berjalan di antara piramid
3. Interlobular arteriole tersusun paralel dalam korteks dan
membentuk arteriole aferen
Peritubular capillaries bersatu membentuk interlobular veins,
arcuate vein, interlobar vein, renal vein
Vena renalis keluar dari hilus dan masuk ke Vena cava
inferior
= unit fungsinal ginjal 1 juta/ginjal
Tubular components:
1. Glomerular (Bowmans) capsule double-walled cup
simple squamous epithelium
2. Proximal convoluted tubule - coiled 1
st
section
simple cuboidal epithelium with microvilli
3. Loop of Henle - hair-pin loop
thin descending limb, thick ascending limb
4. Distal convoluted tubule - last section
simple cuboidal epithelium
specialised region - Juxta glomerular apparatus
Distal convoluted tubule opens into the collecting system
collecting ducts papillary ducts
minor calyx
Made up of blood vessels:
1. Glomerulus - network of capillaries within Bowmans
capsule
2. Afferent arteriole - leading into glomerulus
3. Efferent arteriole - leading out of glomerulus
4. Peritubular capillaries - surrounding tubules
5. Vasa recta - specialised loops of blood vessels around
long Loop of Henle (juxtamedullary nephrons)
Transpor urine dari ginjal ke
vesica urinaria
Panjang20-30 cm
Dinding ototperistaltik,
mendorong urine ke v.u
retroperitoneal
pressure in the bladder
compresses ureter, helps
prevent backflow of urine
(physiological valve) - still
allows urine to flow into the
bladder
Organ kantung berotot
retroperitoneal, posterior pubic symphysis
Kapasitas ~ 300-400 ml (max = 1000 ml)
Saat kosong: seperti balon kempis, rugae
Laki-laki: anterior rektum, di atas prostat
Perempuan: inferior uterus. Anterior vagina
superior surfaces -
peritoneum
middle umbilical ligament -
superior border to umbilicus
lateral umbilical ligaments -
sides of bladder to umbilicus
At base, tough ligamentous
bands anchor bladder to
pelvic and pubic bones
Trigone : triangular area
bounded by openings of
ureters and exit to urethra
cystitis - inflammation of the
bladder wall
Female ~ 4cm long
opens to exterior between
clitoris and vaginal
opening
Male ~ 20 cm long
passes through prostate
gland
pierces urogenital
diaphragm
enters penis and extends
throughout length
opens at urethral orifice
Reseptor terstimulasi bila:
terisi ~ 200 ml
Serabut aferen ke s.c.
motor neurons di dinding
vesica urinaria
Kontraksi m. detrusor dan
meningkatkan tekanan
Relaksasi internal and
external sphincter -
external
Jika external sphincter
tidak relaksasi, internal
sphincter tertutup dan
dinding vu relaksasi
Jika volume >500 ml,
refleks mictie cukup untuk
kontraksi sphincter interna
dan relaksasi sphincter
externa
Fungsi Ginjal :
1. Mengeluarkan kotoran dari tubuh (urine)
2. Mengatur keseimbangan cairan, maintenance
homeostasis
FUNGSI EKSKRESI
Mempertahankan osmolalitas plasma sekitar 285 mOsmol
Mempertahankan volume dan tekanan darah dengan
mengatur ekskresi Na
Mempertahankan konsentrasi plasma elektrolit
Mempertahankan pH plasma sekitar 7,4
Mengekskresikan produk akhir nitrogen dari metabolisme
protein (urea, asam urat dan kreatinin)
Ekskresi ebagian besar obat
FUNGSI NONEKSKRESI
Sintesis dan aktivasi hormon: Renin, eritropoetin, vitamin D,
prostaglandin,
degradasi hormon polipeptida, insulun, glukagon,
parathormon, prolaktin, hormon pertumbuhan, ADH dan
hormon gastrointestinal
Menyaring 200 L darah /hari, memungkinkan toksin-
toksin, sampah metabolik dan ion excess keluar dari
tubuh lewat urin
Meregulasi volume dan zat-zat kimia yang terbentuk
oleh darah
Mengatur keseimbangan antara air dan garam, juga
asam dan basa
Gluconeogenesis selama puasa
Menghasilkan renin untuk membantu regulasi tekanan
darah dan eritropoetin untuk merangasang produksi sel-
sel darah merah
Aktivasi vitamin D
Renal corpuscle Terdiri atas glomerulus dan kapsul
Bowman
Endotel Glomerular fenestrated epithelium that
allows solute-rich, virtually protein-free filtrate to pass
from the blood into the glomerular capsule
Figure 25.4b
Bagian distal portion dari distal tubulus convoluted yang
dekat ke collecting ducts
Terdapat dua jenis sel penting, yaitu:
Intercalated cells
Sel-sel Kuboid dengan microvilli
Berfungsi pada maintain keseimbangan asam basa tubuh
Principal cells
Sel-sel kuboid tanpa microvilli
Membantu maintain cairan tubuh dan keseimbangan garam
Cortical nephrons 85% of nephrons; lokasi pada
cortex
Juxtamedullary nephrons:
Berlokasi di cortex-medulla junction
Mempunyai loops of Henle yang menginvasi ke dalam
medulla
Mempunyai segmen yang ketebalan lebih extensive
Berperan dalam produksi konsentrasi urin
Figure 25.5b
Every nephron has two capillary beds
Glomerulus
Peritubular capillaries
Each glomerulus is:
Fed by an afferent arteriole
Drained by an efferent arteriole
Blood pressure in the glomerulus is high because:
Arterioles are high-resistance vessels
Afferent arterioles have larger diameters than efferent
arterioles
Fluids and solutes are forced out of the blood throughout
the entire length of the glomerulus
Figure 25.5a
Afferent and efferent arterioles offer high resistance to
blood flow
Blood pressure declines from 95mm Hg in renal arteries
to 8 mm Hg in renal veins
Resistance in afferent arterioles:
Protects glomeruli from fluctuations in systemic blood
pressure
Resistance in efferent arterioles:
Reinforces high glomerular pressure
Reduces hydrostatic pressure in peritubular capillaries
Where the distal tubule lies against the afferent
(sometimes efferent) arteriole
Arteriole walls have juxtaglomerular (JG) cells
Enlarged, smooth muscle cells
Have secretory granules containing renin
Act as mechanoreceptors
Macula densa
Tall, closely packed distal tubule cells
Lie adjacent to JG cells
Function as chemoreceptors or osmoreceptors
Mesanglial cells:
Have phagocytic and contractile properties
Influence capillary filtration
Figure 25.6
Filter that lies between the blood and the interior of the
glomerular capsule
It is composed of three layers
Fenestrated endothelium of the glomerular capillaries
Visceral membrane of the glomerular capsule
(podocytes)
Basement membrane composed of fused basal
laminae of the other layers
Figure 25.7a
Figure 25.7c
The kidneys filter the bodys entire plasma volume 60
times each day
The filtrate:
Contains all plasma components except protein
Loses water, nutrients, and essential ions to become
urine
The urine contains metabolic wastes and unneeded
substances
Urine formation
and adjustment of
blood composition
involves three
major processes
Glomerular
filtration
Tubular
reabsorption
Secretion
Figure 25.8
Principles of fluid dynamics that account for tissue fluid
in all capillary beds apply to the glomerulus as well
The glomerulus is more efficient than other capillary
beds because:
Its filtration membrane is significantly more permeable
Glomerular blood pressure is higher
It has a higher net filtration pressure
Plasma proteins are not filtered and are used to maintain
oncotic pressure of the blood
The pressure responsible for filtrate formation
NFP equals the glomerular hydrostatic pressure (HP
g
)
minus the oncotic pressure of glomerular blood (OP
g
)
combined with the capsular hydrostatic pressure (HP
c
)
NFP = HP
g
(OP
g +
HP
c
)
The total amount of filtrate formed per minute by the
kidneys
Factors governing filtration rate at the capillary bed are:
Total surface area available for filtration
Filtration membrane permeability
Net filtration pressure
GFR is directly proportional to the NFP
Changes in GFR normally result from changes in
glomerular blood pressure
Figure 25.9
If the GFR is too high:
Needed substances cannot be reabsorbed quickly
enough and are lost in the urine
If the GFR is too low:
Everything is reabsorbed, including wastes that are
normally disposed of
Three mechanisms control the GFR
Renal autoregulation (intrinsic system)
Neural controls
Hormonal mechanism (the renin-angiotensin system)
Under normal conditions, renal autoregulation maintains
a nearly constant glomerular filtration rate
Autoregulation entails two types of control
Myogenic responds to changes in pressure in the
renal blood vessels
Flow-dependent tubuloglomerular feedback senses
changes in the juxtaglomerular apparatus
When the sympathetic nervous system is at rest:
Renal blood vessels are maximally dilated
Autoregulation mechanisms prevail
Under stress:
Norepinephrine is released by the sympathetic
nervous system
Epinephrine is released by the adrenal medulla
Afferent arterioles constrict and filtration is inhibited
The sympathetic nervous system also stimulates the
renin-angiotensin mechanism
Is triggered when the JG cells release renin
Renin acts on angiotensinogen to release angiotensin I
Angiotensin I is converted to angiotensin II
Angiotensin II:
Causes mean arterial pressure to rise
Stimulates the adrenal cortex to release aldosterone
As a result, both systemic and glomerular hydrostatic
pressure rise
Renin release is triggered by:
Reduced stretch of the granular JG cells
Stimulation of the JG cells by activated macula densa
cells
Direct stimulation of the JG cells via
1
-adrenergic
receptors by renal nerves
Angiotensin II
Figure 25.10
LFG/GFR adalah mengukur berapa banyak filtrat yang
dihasilkan oleh glomerulus
Merupakan pengukuran paling baik untuk menilai fungsi
eksresi
Filtrasi dipengaruhi oleh aliran plasma , perbedaan
tekanan, luas permukaan kapiler, dan permeabilitas
kapiler
LFG merupakan jumlah dari hasil semua nefron (rata-
rata 1 juta tiap ginjal)
Rumus Homer Smith untuk mengukur renal klirens :
C = U X V
P
C = Klirens
U = Konsentrasi zat marker dalam urin
V = Volume urin
P = Konsentrasi zat marker dalam plasma
You might also like
- sp2 BatamDocument26 pagessp2 BatamRofi IrmanNo ratings yet
- Gejala Saluran NafasDocument48 pagesGejala Saluran NafasRofi IrmanNo ratings yet
- Gejala Saluran NafasDocument48 pagesGejala Saluran NafasRofi IrmanNo ratings yet
- ISKEMIA JANTUNGDocument79 pagesISKEMIA JANTUNGRofi IrmanNo ratings yet
- Bab IIDocument38 pagesBab IITirzaa KaihatuNo ratings yet
- MDR TB - LDocument90 pagesMDR TB - LRofi IrmanNo ratings yet
- Cronic Pulmonary InfectionDocument7 pagesCronic Pulmonary InfectionRofi IrmanNo ratings yet
- Sejarah ImmunologiDocument55 pagesSejarah ImmunologiRofi IrmanNo ratings yet
- CAIRANDocument123 pagesCAIRANRofi IrmanNo ratings yet
- Lupus Nefritis, A. HarisDocument36 pagesLupus Nefritis, A. HarisRofi IrmanNo ratings yet
- Bronkoskopi LDocument121 pagesBronkoskopi LRofi Irman100% (1)
- Tumor Paru LDocument31 pagesTumor Paru LRofi IrmanNo ratings yet
- Agd LDocument77 pagesAgd LRofi IrmanNo ratings yet
- Penatalaksanan BPH Konservatif: AntoniDocument20 pagesPenatalaksanan BPH Konservatif: AntoniRofi IrmanNo ratings yet
- ANFIS GINJAL, HeriantoDocument82 pagesANFIS GINJAL, HeriantoRofi IrmanNo ratings yet
- Anemia Pada PGKDocument45 pagesAnemia Pada PGKRofi IrmanNo ratings yet
- CAIRANDocument123 pagesCAIRANRofi IrmanNo ratings yet
- Tumor Paru LDocument31 pagesTumor Paru LRofi IrmanNo ratings yet
- DM Nefropati, Edy NRDocument27 pagesDM Nefropati, Edy NRRofi IrmanNo ratings yet
- GINJALDocument97 pagesGINJALRofi IrmanNo ratings yet
- Hipertensi Dalam Kehamilan, Nelda AsDocument41 pagesHipertensi Dalam Kehamilan, Nelda AsRofi IrmanNo ratings yet
- Hipertensi LubisDocument55 pagesHipertensi LubisRofi IrmanNo ratings yet
- Bronkoskopi LDocument121 pagesBronkoskopi LRofi Irman100% (1)
- Penatalaksanan BPH Konservatif: AntoniDocument20 pagesPenatalaksanan BPH Konservatif: AntoniRofi IrmanNo ratings yet
- Terapi Konservatif Uropati Obstruktif Akibat Keganasan Prostat RefratDocument2 pagesTerapi Konservatif Uropati Obstruktif Akibat Keganasan Prostat RefratRofi IrmanNo ratings yet
- Agd LDocument77 pagesAgd LRofi IrmanNo ratings yet
- Sepsis (L)Document84 pagesSepsis (L)Rofi IrmanNo ratings yet
- Anemia Hemolitik RofiDocument68 pagesAnemia Hemolitik RofiRofi IrmanNo ratings yet