Professional Documents
Culture Documents
CH 26
Uploaded by
Jann Zaniel Allayne RiOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
CH 26
Uploaded by
Jann Zaniel Allayne RiCopyright:
Available Formats
Chapter 26: Urine Formation By the Kidneys. I.
Glomerular Filtration, Renal Blood Flow and Their Control
Guyton and Hall, Textbook of Medical Physiology, 12th edition
Multiple Functions of the Kidney Excretion of Metabolic Waste Products, Foreign Chemicals, Drugs, and Hormone Metabolites a. Eliminate waste products of metabolism that are no longer needed ( i.e. urea, creatinine, uric acid, hb breakdown products) b. Also rapidly eliminate most toxins, pesticides, drugs, food additives
Functions (cont.) Regulation of Water and Electrolyte Balances a. For homeostatsis, excretion of electrolytes must match intake
b. Governed mostly by eating habits
Functions (cont.) Regulation of Arterial Pressure a. By excreting variable amounts of sodium and water b. Short-term-by secreting hormones and vasoactive factors (i.e. renin) Glucose Synthesis
a. Gluconeogenesis-synthesize glucose from amino acids and other precursors during prolonged fasting.
Functions (cont.) Regulation of Acid-Base Balance a. By excreting acids and by regulating the body fluid buffer stores
b. Kidney is the only means of eliminating sulfuric and phosphoric acids (generated by the metabolism of proteins
Functions (cont.) Regulation of Erythrocyte Production a. Secretes erythropoietin which stimulates the production of red blood cells
Regulation of 1,25-Dihydroxyvitamin D3 Production
a. Produces the active form (calcitriol)
b. Calcitriol is necessary for the normal calcium deposition in bone and calcium reabsorption by the gastrointestinal tract
Physiologic Anatomy of the Kidneys General Organization of the Kidneys and Urinary Tract
Fig. 26.2 General Organization of the Kidneys and Urinary System
Physiologic Anatomy of the Kidneys Renal Blood Supply
Fig. 26.3 Renal Blood Supply
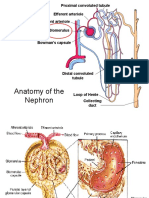
Physiologic Anatomy of the Kidneys The Nephron-functional unit of the kidney a. b. c. d. e. f. g. Each kidney contains 800,000-1,000,000 Decrease with age or injury (cannot be replaced) Contains the glomerulus (Bowmans capsule) Proximal and distal convoluted tubules Loop of Henle Macula densa Collecting ducts
Physiologic Anatomy of the Kidneys
Figure 26.4 Basic tubular segments of the nephron
Physiologic Anatomy of the Kidneys Regional Differences in Nephron Structure: Cortical and Juxtaglomerular Nephrons
Figure 26.5 Cortical and juxtaglomerular nephrons
Physiologic Anatomy of Urinary Bladder Micturition-process by which the urinary bladder empties when it becomes filled a. The bladder fills progressively until the tension within the walls rises above a threshold level b. The micturition reflex empties the bladder or stimulates a conscious desire to urinate c. It is an autonomic reflex that can be altered by centers in the cerebral cortex
Physiologic Anatomy of Urinary Bladder Bladder Anatomy-smooth muscle chamber composed of two main parts: a. Body-where the urine collects b. Neck-funnel shaped extension which connects with the urethra The smooth muscle of the bladder is the detrusor muscle and its contraction is a major step in emptying the bladder.
Fig. 26.6 Anatomy of the urinary bladder in males and females
Innervation of the Bladder-pelvic nerves through the saccral plexus
Fig. 26.7 Innervation of the urinary bladder
Transport of Urine No significant changes in urine composition from the renal calyces to the ureters to the bladder Peristaltic contractions in the smooth muscle of the ureter are enhanced by parasympathetic stimulation and inhibited by sympathetic stimulation
Micturition Reflex
Fig. 26.8 Normalcystometrogram showing acute pressure waves caused by micturition reflexes
Micturition Reflex
As the bladder fills, micturition contractions occur
Initiated by stretch receptors in the bladder
When partially filled, the contractions relax spontaneously
The reflex is self-regenerative
Micturition Reflex
Reflex is a Single Complete Cycle
a. Progressive and rapid increase of pressure
b. A period of sustained pressure
c. Return of the pressure to the basal tone
Urine Formation
Fig. 26.9 Basic kidney processes that determine the composition of urine
Urine Formation Sum of three renal processes
A. The substance is freely filtered but not reabsorbed
B. The substance is freely filtered but part is reabsorbed C. The substance is freely filtered but not excreted because all is reabsorbed. D. The substance is freely filtered but is not reabsorbed but secreted from the peritubular capillaries into the renal tubules
Fig. 26.10
Glomerular Filtration Composition of the Filtrate a. Protein free and cell free b. Salts and organic molecules are similar to those in plasma c. Does not include calcium and fatty acids that are bound to proteins
Glomerular Filtration (cont.) GFR (Glomerular Filtration Rate) a. Determined by (1) the balance of hydrostatic and colloid osmotic forces acting on the capillary membrane, and (2) the product of the permeability and filtering surface area of the capillaries b.
Glomerular Capillary Membrane
Consists of Three Major Layers
a. Endothelium of the capillary
b. Basement membrane
c. Layer of epithelial cells (podocytes)
Fig. 26.11 A: Basic ultrastructure of the glomerular capillaries; B: Cross-section of the capillary membrane and its major components
Membrane (cont.) Filterability of Solutes is Inversely Related to Their Size
Table 26.1 Filterability of substances by glomerular capillaries based on molecular weight
Substance Water Sodium Glucose Inulin Myoglobin Albumin
Molecular Weight 18 23 180 5,500 17,000 69,000
Filterability 1.0 1.0 1.0 1.0 0.75 0.005
Membrane (cont.) Negatively Charged Large Molecules Are Filtered Less Easily Than Positively Charged Molecules of Equal Molecular Size
Fig. 26.12 Effect of molecular radius and electrical charge of dextran on its filterability by glomerular capillaries
Determinants of the GFR GFR is determined by (1) sum of the hydrostatic and colloid forces across the glomerular membrane (net filtration pressure), and (2) the glomerular capillary filtration coefficient.
Fig. 26.13
Determinants of the GFR
Increased glomerular capillary filtration coefficient increases GFR
Increased Bowmans capsule hydrostatic pressure decreases GFR Increased glomerular capillary colloid osmotic pressure decreases GFR
Fig. 26.14 Increase in colloid osmotic pressure in plasma flowing through the glomerular capillary.
Determinants of the GFR (cont.) Increased glomerular capillary hydrostatic pressure increases GFR
Fig. 26.15 Effect of change in afferent or efferent arteriole resistance on GFR and renal flow.
Renal Blood Flow Renal Blood Flow and Oxygen Consumption
Fig. 26.16 Relationship between sodium reabsorption and oxygen consumption
Renal Blood Flow (cont.) Determinants of Renal Blood Flow
Table 26.3 Approximate pressures and vascular resistances in the circulation of a normal kidney
Percentage of Total Renal Vascular Resistance
Vessel
Beginning
End
Renal Artery
100
100
Interlobar, arcuate, and interlobular arteries
Afferent arteriole Glomerular capill. Efferent arteriole Peritubular capill. Interlobar, arcuate, and interlobular veins Renal vein
Approx. 100
85
16
85 60 59 18 8 4
60 59 18 8 4 Approx. 4
26 1 43 10 4 0
Physiologic Control of GFR and Renal Blood Flow Sympathetic Nervous System Activation Decreases GFR Hormonal and Autacoid Control of Renal Circulation
Hormone or Autacoid
Norepinephrine Epinephrine Endothelin Angiotensin II
Effect on GFR
Decreases Decreases Decreases Constricts efferent arterioles
Endothelian NO
Prostaglandins
Increases
Increases
Autoregulation of GFR and Renal Blood Flow
Fig. 26.17 Autoregulation of renal blood flow and GFR but lack of autoregulation of urine flow during changes in renal arterial pressure
Tubuloglomerular Feedback and Autoregulation of GFR
Links changes in NaCl concentration at the macula densa with the control of renal arteriolar resistance Two components a. An afferent arteriolar feedback mechanism b. An efferent arteriolar feedback mechanism
Fig. 26.18 Structure of the juxtaglomerular apparatus, demonstrating its possible feedback role in the control of nephron function.
Decreased macula densa NaCl causes dilation of afferent arterioles and increased renin release
Fig. 26.19
Myogenic Autoregulation of Renal Blood Flow and GFR a. Ability of blood vessels to resist stretching during increased arterial pressure
b. Stretch allows the release of calcium from ECF into the cells causing them to contract
High protein intake and increased blood glucose also increase renal blood flow
You might also like
- OPD census report for Feb 2018 with leading casesDocument1 pageOPD census report for Feb 2018 with leading casesJann Zaniel Allayne RiNo ratings yet
- Ankle SprainDocument55 pagesAnkle SprainJann Zaniel Allayne RiNo ratings yet
- CH 29Document39 pagesCH 29Jann Zaniel Allayne RiNo ratings yet
- CH 28Document22 pagesCH 28Jann Zaniel Allayne RiNo ratings yet
- Report in Inborn Errors of Urea SynthesisDocument29 pagesReport in Inborn Errors of Urea SynthesisJann Zaniel Allayne RiNo ratings yet
- Guyton and Hall Textbook Chapter 25: Body Fluid Compartments and Fluid BalanceDocument19 pagesGuyton and Hall Textbook Chapter 25: Body Fluid Compartments and Fluid BalanceJann Zaniel Allayne RiNo ratings yet
- CH 30Document26 pagesCH 30Jann Zaniel Allayne RiNo ratings yet
- CH 27Document40 pagesCH 27Jann Zaniel Allayne RiNo ratings yet
- ChromatographyDocument3 pagesChromatographyJann Zaniel Allayne RiNo ratings yet
- Congestive Heart FailureDocument2 pagesCongestive Heart FailureJann Zaniel Allayne RiNo ratings yet
- Nerves and Muscles Both Initiate Their Activity Based On DepolarisationDocument1 pageNerves and Muscles Both Initiate Their Activity Based On DepolarisationJann Zaniel Allayne RiNo ratings yet
- Nerves and Muscles Both Initiate Their Activity Based On DepolarisationDocument1 pageNerves and Muscles Both Initiate Their Activity Based On DepolarisationJann Zaniel Allayne RiNo ratings yet
- DyosaakoDocument4 pagesDyosaakoJann Zaniel Allayne RiNo ratings yet
- Cefazolin for Skin and Moderate Bacterial InfectionsDocument5 pagesCefazolin for Skin and Moderate Bacterial InfectionsJann Zaniel Allayne RiNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (894)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Medical Diagnosis: Chronic Kidney Disease Stage 5Document4 pagesMedical Diagnosis: Chronic Kidney Disease Stage 5Hadeer Mahmoud Abuslima100% (1)
- Renal Disease PresentationDocument17 pagesRenal Disease Presentationapi-292524690No ratings yet
- Edexcel IGCSE BiologyDocument11 pagesEdexcel IGCSE BiologytopsyisgayNo ratings yet
- Kidney TendernessDocument13 pagesKidney TendernessmariyamNo ratings yet
- Renal Function Tests 1 PDFDocument56 pagesRenal Function Tests 1 PDFCharles Bryahn OkoboiNo ratings yet
- Hubungan Dukungan Keluarga Dengan Kepatuhan Diet Pada Pasien Gagal Ginjal Kronik Yang Menjalani HemodialisisDocument10 pagesHubungan Dukungan Keluarga Dengan Kepatuhan Diet Pada Pasien Gagal Ginjal Kronik Yang Menjalani Hemodialisisemilda adhamiNo ratings yet
- Castle Connolly Graduate Board Review SeriesDocument31 pagesCastle Connolly Graduate Board Review SeriesCCGMPNo ratings yet
- Blood Test Reference GuideDocument3 pagesBlood Test Reference GuideHNo ratings yet
- Edward Hammond, Andrew McIndoe, Mark Blunt, JohnDocument249 pagesEdward Hammond, Andrew McIndoe, Mark Blunt, JohnNOMOREHATEOKNo ratings yet
- Ch18 Lecture PPT ADocument70 pagesCh18 Lecture PPT AMiky rose De Guzman100% (1)
- Clinical Microscopy Guide to Urine and Body Fluid AnalysisDocument32 pagesClinical Microscopy Guide to Urine and Body Fluid AnalysispikachuNo ratings yet
- Anemia in Heart Failure: A Review of Pathophysiology, Treatment Challenges and UnknownsDocument13 pagesAnemia in Heart Failure: A Review of Pathophysiology, Treatment Challenges and UnknownsHedya Nadhrati SururaNo ratings yet
- 3rd FluidsDocument11 pages3rd FluidsFelix BalanNo ratings yet
- Surgical Ward ExamDocument8 pagesSurgical Ward ExamJaysellePuguonTabijeNo ratings yet
- JAMB Biology Past Questions and AnswersDocument53 pagesJAMB Biology Past Questions and AnswersOma AttamahNo ratings yet
- BED 4107 Gerontology Lecture Notes MARCH 2020Document40 pagesBED 4107 Gerontology Lecture Notes MARCH 2020SHARON KIHORONo ratings yet
- Case Presentation On Urinary Tract InfectionDocument56 pagesCase Presentation On Urinary Tract InfectionJohn Alvin Yoro92% (24)
- Anatomy of The Excretory SystemDocument6 pagesAnatomy of The Excretory SystemCherry Grace Articulo DabuconNo ratings yet
- PPIs and Kidney DiseaseDocument6 pagesPPIs and Kidney DiseaseSonia jolandaNo ratings yet
- Bscnursing QP BlueprintDocument33 pagesBscnursing QP Blueprintshankarmeti2004No ratings yet
- The Definition of Acute Kidney Injury and Its Use in PracticeDocument12 pagesThe Definition of Acute Kidney Injury and Its Use in PracticeErwin SiahaanNo ratings yet
- Chicken Anatomy & PhysiologyDocument26 pagesChicken Anatomy & PhysiologySanjeev ChaudharyNo ratings yet
- Electrolytes and Acid Base Common Fluid and Enlectrolyte DisordersDocument9 pagesElectrolytes and Acid Base Common Fluid and Enlectrolyte Disordersninta karinaNo ratings yet
- Organ Sistem UrinariaDocument43 pagesOrgan Sistem UrinariaAndrey DwiNo ratings yet
- Therapeutic Plasma Exchange (TPE) : Colm Magee, MD, MPH, MRCPIDocument23 pagesTherapeutic Plasma Exchange (TPE) : Colm Magee, MD, MPH, MRCPIsigitNo ratings yet
- Endotoxins: Myoglobin, Hemoglobin Exotoxin: Drugs Ethylene Glycol Contrast Medium Snakebite Nephropathy InfectionDocument34 pagesEndotoxins: Myoglobin, Hemoglobin Exotoxin: Drugs Ethylene Glycol Contrast Medium Snakebite Nephropathy InfectionpeekhakhaNo ratings yet
- Renal Pathology Lectures - PPT SeriesDocument267 pagesRenal Pathology Lectures - PPT SeriesMarc Imhotep Cray, M.D.100% (12)
- Anatomi GinjalDocument9 pagesAnatomi GinjalMinda IANo ratings yet
- Renal Function Tests: Understanding BUN, Creatinine, and ClearanceDocument26 pagesRenal Function Tests: Understanding BUN, Creatinine, and ClearanceHarshini MakkenaNo ratings yet
- Detailed Test Planner: NEET-XII (Passed)Document37 pagesDetailed Test Planner: NEET-XII (Passed)aryanNo ratings yet