Professional Documents
Culture Documents
Coccygectomy PDF
Uploaded by
Diaz RandanilOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Coccygectomy PDF
Uploaded by
Diaz RandanilCopyright:
Available Formats
National Medical Policy
Subject: Coccygectomy and Treatments for Coccydynia
Policy Number: NMP390
Effective Date*: November 2007
Updated: June 2014
This National Medical Policy is subject to the terms in the
IMPORTANT NOTICE
at the end of this document
For Medicaid Plans: Please refer to the appropriate Medicaid Manuals for coverage
guidelines prior to applying Health Net Medical Policies
The Centers for Medicare & Medicaid Services (CMS)
For Medicare Advantage members please refer to the following for coverage guidelines first:
Use Source Reference/Website Link
National Coverage Determination
(NCD)
National Coverage Manual Citation
Local Coverage Determination
(LCD)*
Article (Local)*
Other
X None Use Health Net Policy
Instructions
Medicare NCDs and National Coverage Manuals apply to ALL Medicare members in ALL
regions.
Medicare LCDs and Articles apply to members in specific regions. To access your specific
region, select the link provided under “Reference/Website” and follow the search
instructions. Enter the topic and your specific state to find the coverage determinations
for your region. *Note: Health Net must follow local coverage determinations (LCDs) of
Medicare Administration Contractors (MACs) located outside their service area when
those MACs have exclusive coverage of an item or service. (CMS Manual Chapter 4
Section 90.2)
If more than one source is checked, you need to access all sources as, on occasion, an
LCD or article contains additional coverage information than contained in the NCD or
National Coverage Manual.
Coccygectomy for Coccygodynia Jun 14
1
If there is no NCD, National Coverage Manual or region specific LCD/Article, follow the
Health Net Hierarchy of Medical Resources for guidance.
Current Policy Statement
Health Net, Inc. considers coccygectomy medically necessary for treatment of coccydynia
when all of the following are met:
1. Patient has severe, persistent pain in or around the coccyx which is poorly tolerated,
chronically disabling or, at times, functionally limiting; and
2. Direct pressure on the coccyx or movement of the coccyx on digital rectal examination
reproduces the pain; and
3. Patient has a history of any of the following:
Trauma to the coccyx (e.g., fracture or dislocation from a fall, sacrococcygeal
joint is forced out of alignment during childbirth, horseback riding, extensive bike
riding or rowing)
Patient has degenerative arthritis in the sacrococcygeal discs and/or
intercoccygeal discs
Patient has radiological instability of the coccyx as judged by intermittent
subluxation or hypermobility* seen on lateral dynamic radiographs when standing
and sitting
Patient has a small bony excrescence on the dorsal aspect of the tip of the
coccyx, i.e., a coccygeal spicule or spur which may harm the subcutaneous
tissues when sitting
Patient has a bone scan demonstrating an ongoing inflammatory process in or
around the coccyx
* Note: Flexion in the sacrococcygeal joint larger than 25-30 degrees represents
hypermobility and slipping larger than 25% represents luxation.
4. Pain has persisted despite at least an 8-month trial of maximal conservative therapy,
including all of the following:
Non-steroidal anti-inflammatory drugs (NSAIDs), e.g., ibuprofen, naproxen, COX-
2 inhibitors; and
Usage of a donut-shaped pillow or a gel cushion to help take pressure off the
coccyx when sitting on hard surfaces; and
Digital manipulation of the coccygeal ligaments with the rectal finger and/or
massages of the pelvic muscles (levator ani or piriformis); and
Physical therapy with ultrasound; and
Repeated local injections of steroid and an anesthetic in and around the coccyx;
and
Intradiscal injections under fluoroscopy in patients with luxation or hypermobility;
and
Note: Even though coccygectomy is the treatment of last resort for coccydynia, it is a
required treatment for sacrococcygeal teratoma and other germ cell tumors involving the
coccyx.
Treatment for Coccydynia
Coccygectomy for Coccygodynia Jun 14
2
Health Net, Inc. considers ganglion impar coccygeal injection medically necessary for
chronic coccydynia when other conservative measures (i.e. treatment with oral analgesics,
physical therapy, epidural steroid injections) have not alleviated the pain and the individual
is not a surgical candidate.
Codes Related To This Policy
NOTE:
The codes listed in this policy are for reference purposes only. Listing of a code in this policy
does not imply that the service described by this code is a covered or non-covered health
service. Coverage is determined by the benefit documents and medical necessity criteria.
This list of codes may not be all inclusive.
On October 1, 2015, the ICD-9 code sets used to report medical diagnoses and inpatient
procedures will be replaced by ICD-10 code sets. Health Net National Medical Policies will
now include the preliminary ICD-10 codes in preparation for this transition. Please note
that these may not be the final versions of the codes and that will not be accepted for billing
or payment purposes until the October 1, 2015 implementation date.
ICD-9 Codes
724.79 Coccydynia
ICD-10 Codes
M53.3 Sacrococcygeal disorders, not elsewhere classified
CPT Codes
27080 Coccygectomy, primary
HCPCS Codes
N/A
Scientific Rationale Update – November 2013
The ganglion impar (ganglion of Walther) is the terminal ganglion of the paravertebral
sympathetic nervous system; it is the only nonpaired sympathetic ganglion. The ganglion
impar is usually located anterior to the sacrococcygeal junction, the first intracoccygeal
junction, or the first coccygeal vertebra. One possible mechanism for persistent coccydynia
is excessive activity or sensitivity of the ganglion impar, thus creating sympathetically
maintained or chronic coccyx pain, known as coccydynia.
Since its original description in 1990, blockade of the ganglion impar has become a potential
minimally invasive intervention in the management of pelvic and perineal pain. Local
injection of an anesthetic is proposed to block the ganglion impar and thereby relieve
coccyx pain. In a published report by Foye et al. (2009), nerve blocks using local
anesthetics with a fast onset (eg, lidocaine) were shown to provide short-term relief.
However, after the local anesthetic block wears off, some of the coccyx pain may start to
return, but generally it returns at a lower severity than existed prior to the injection. Repeat
ganglion impar blocks have been shown to provide additional benefit, further lowering the
plateau level of pain. Thus, in patients without complete resolution, repeat injections are
often medically necessary and therefore more clinically helpful.
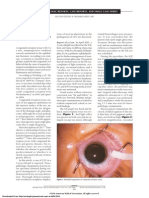
The more recent transsacrococcygeal approach to the ganglion impar involves inserting a
thin needle into the sacrococcygeal junction, from posterior to anterior. The
Coccygectomy for Coccygodynia Jun 14
3
transsacrococcygeal approach for ganglion impar sympathetic blockade uses a lateral
fluoroscopic view to visualize the sacrococcygeal junction. A small, 25-gauge spinal needle
is then inserted through the junction until the needle tip is just anterior to that articulation.
Radiographic contrast can be used to confirm that the needle placement is not intravascular,
not too far anterior and not too superficial. The ganglion impar block can be preceded by a
separate local anesthetic block of the coccygeal nerve, to anesthetize the posterior region
prior to the impar injection and to provide more complete relief of the coccydynia. Often, it
makes sense to combine these injections on the same injection date, so that both anterior
and posterior relief is obtained.
A case series reported good results from the administration of 20 ganglion impar blocks by
physical medicine and rehabilitation physicians at New Jersey Medical School to patients
who were suffering from persistent coccydynia despite treatment with oral medications,
cushions, and other conservative therapies. The results showed that each of the 20
injections provided significant relief in these patients. The percentage of relief obtained per
injection varied from 20-75%, with most patients reporting 50-75% relief obtained per
injection and with the relief generally lasting weeks to months or longer. For cases in which
patients had incomplete relief after a given injection, additional analgesic benefit was
obtained from subsequent injections. Thus, repeat injections were often helpful.
Foye et al. (2009) also published a new, slightly more direct approach to ganglion impar
injections. Specifically, they reported the option of passing the needle through the first
intracoccygeal joint instead of through the sacrococcygeal joint. An important benefit to this
approach over the transsacrococcygeal one is that the first intracoccygeal joint is often
easier to visualize, since it is not obstructed by the sacral or coccygeal cornua.
Foye et al. (2009) completed a study and presented information regarding performing nerve
blocks of the ganglion impar. These injections have been reported to relieve coccydynia, as
well as other malignant and nonmalignant pelvic pain syndromes. A variety of techniques
have been previously described for blocking this sympathetic nerve ganglion, which is
located in the retrorectal space just anterior to the upper coccygeal segments. Prior
techniques have included approaches through the anococcygeal ligament, through the
sacrococcygeal joint, and through intracoccygeal joint spaces. This article presents a new,
paracoccygeal approach whereby the needle is inserted alongside the coccyx and the needle
is guided through three discrete steps with a rotating or corkscrew trajectory. Compared
with some of the previously published techniques, this paracoccygeal corkscrew approach
has multiple potential benefits, including ease of fluoroscopic guidance using the lateral
view, ability to easily use a stylet for the spinal needle, and use of a shorter, thinner needle.
While no single technique works best for all patients and each technique has potential
advantages and disadvantages, this new technique adds to the available options.
Kozlowski et al. (2009) reviewed charts and computed tomography (CT)-scans of patients
who underwent block and neuroablation of the ganglion impar (Walther) between 2003 and
2007 were systematically reviewed with respect to adverse events and efficacy by rating
pain intensity. A total of 76 blocks were performed, 48 of them being diagnostic blocks and
28 neuroablations. Chemical destruction was performed with ethanol, if pain recurred
despite injection of local anesthetic. Interventional pain therapy was performed in 43
patients (age: 64.6+/-12.4 y, median 49.5 y, range: 36 to 86 y, male/female: 27/16)
presenting with perineal pain of unknown origin (n=15), carcinoma of the prostate (n=8),
colorectal carcinoma (n=7), postsurgery of thrombosis of perineal veins (n=3), postherpetic
neuralgia (n=4), malformation of the spinal cord (n=2), vaginal protrusion (n=2), failed
back surgery syndrome (n=1), and ablation of testis (n=1). CT-guided puncture was not
associated with any adverse events and resulted in a reduction of numeric rating scale
Coccygectomy for Coccygodynia Jun 14
4
values from 8.2+/-1.6 to 2.2+/-1.6 (P<0.0001, 95% confidence interval 0.5) immediately
at discharge and to 2.2+/-1.4 (P<0.0001, 95% confidence interval 0.4) at 4 months on
follow up. CT-guided block and neuroablation of the ganglion impar (Walther) results in a
significant reduction of pain scores and carries virtually no hazards.
Lin et al. (2010) Ganglion impar block is an uncommon procedure that has been performed
traditional with fluoroscopy. One approach is the trans-sacrococcygeal approach. Sometimes
this can be difficult because the sacrococcygeal joint (SCJ) cannot be readily seen on
anteroposterior (AP) and lateral fluoroscopy. This technical report describes the feasibility of
ultrasound in assisting ganglion impar blocks. METHODS: We performed ganglion impar
block using ultrasound as the primary imaging tool, with fluoroscopic confirmation in 15
patients. We used a linear array transducer (5-12 MHz) to obtain sonographic transverse
and longitudinal views at the sacral cornua; we identified the first cleft below the sacral
hiatus as the SCJ. Then we inserted a 23-gauge (7 cm in length) needle into the SCJ under
sonographic guidance. Then we confirmed proper needle depth by lateral fluoroscopy and
injection of contrast agent. In all 15 procedures, we accurately located and passed the
needle into the patients' SCJs under real time sonographic guidance. In cases where the
cleft cannot be readily seen on AP and lateral fluoroscopy, we have found ultrasound to be
of assistance. Ultrasound does not replace fluoroscopy, because lateral fluoroscopy is still
required to establish safe depth, and correct site of injection. However, ultrasound can be
helpful when fluoroscopy alone is insufficient.
Datir (2010) completed a study to evaluate the role of computed tomography (CT) in needle
placement for ganglion impar blocks, and to determine the efficacy of CT-guided ganglion
impar blocks in the management of coccydynia. The results of ganglion impar blockade in
eight patients with coccydynia secondary to trauma or unknown cause were reviewed. The
diagnosis of coccydynia was based on clinical history, location of pain, and response to
previous diagnostic and therapeutic procedures. The eight patients were treated with CT-
guided ganglion impar blocks to manage their coccyx pain after conservative procedures,
including oral medication and cushions, failed to provide relief. All patients were subjected
to ganglion impar blocks under a thin-section CT-guided technique for needle placement,
using a mixture of bupivacaine and triamcinolone. The patients were followed-up for a
period of 6-months. Eight patients were treated in this study with a total of 11 injections. A
technical success of 100% was achieved in all cases with accurate needle placement without
any complications and all the patients tolerated the procedure well. Out of eight, three
patients (37%) had complete relief of pain on the follow-up intervals up to 6 months. Three
out of eight patients (37%), had partial relief of symptoms and a second repeat injection
was given at the 3 month interval of the follow-up period. At the end of the 6-month follow-
up period, six out of eight patients (75%) experienced symptomatic relief (four complete
relief and two partial relief) without any additional resort to conventional pain management.
Twenty-five percent (two out of eight) did not have any symptomatic improvement. The
mean visual analogue score (VAS) pre-procedure was 8 (range 6-10) and had decreased to
2 (range 0-5) in six out of eight patients. CT can be used as an imaging method to identify
the ganglion and guide the needle in ganglion impar blockade. The advantages of CT-guided
injection over those performed under fluoroscopy may include accurate and confident
needle placement in the sacro-coccygeal region, ease of wide area coverage, lesser risk of
complications due to inadvertent injections into the major pelvic structures, and increased
likelihood of reaching the ganglion impar, especially in cases with anatomical variation in
the ganglion impar location. These factors may have implications in the overall success rate
of ganglion impar blockade.
Sáenz et al. (2011) completed a retrospective study of 23 patients who underwent
treatment for coccydynia and failed to respond to conservative management. They were
Coccygectomy for Coccygodynia Jun 14
5
treated by radiologically guided infiltration of the ganglion blockade impar and/or caudal
blockade with 1% lidocaine 60–80 mg triamcinolone. Of these 23 patients, 21 were
available for clinical review and completed a questionnaire giving their assessment of the
effect of the infiltration of the ganglion impar block and/or caudal block. Positive results
were obtained in 16 of the 21 patients with coccydynia due to trauma. In five patients the
results were moderate or poor, although none described worse pain after the operation.
They are no complications after the infiltration. Ganglion impar block and/or caudal block
offered satisfactory relief of pain in the majority of patients in this study regardless of the
cause of their symptoms, however, this was a very small retrospective study. (This was one
of the studies that the Physician Reviewer noted).
Sağır (2011) Ganglion impar blockade is not a routinely used anesthetic and analgesic
procedure in clinical practice. An elective intrarectal manuel treatment was planned for a
woman patient with coccyx dislocation due to falling down from a chair 5 days ago. Ganglion
impar block was performed with saccrococcygeal approach using 22 gauge spinal needle
along with fluoroscopy following routine monitorization. Blood pressure, heart rate,
peripheral oxygen saturation and visual analog scale (VAS) were recorded before and, after
block with three minute intervals. VAS value of the patient, 8 before the procedure,
decreased 50% 6 minutes after block. Intrarectal manuel treatment was applied to the
patient with VAS of 0 at 9th minute. Hemodynamic values were within normal limits during
and after the procedure and no motor block was observed. The patient with VAS of 0 at 2nd
and 6th hour after block was discharged. VAS of 0 was determined at 24th and 48th hour
by phone call. In conclusion, ganglion impar block provided adequate analgesia without
causing any complications during and after the intrarectal manuel treatment for the patient
with coccyx dislocation. However, the authors believe that further clinical studies are
required to establish the safety and efficiency of this technique for other procedures at
perianal region.
Johnston (2012) The ganglion impar is an unpaired sympathetic structure located at the
level of the sacrococcygeal joint. Blockade of this structure has been utilized to treat chronic
perineal pain. Methods to achieve this block often involve the use of fluoroscopy which is
associated with radiation exposure of staff involved in providing these procedures. We
report a combined loss of resistance injection technique in association with ultrasound
guidance to achieve the block. Ultrasound was used to identify the sacrococcygeal joint and
a needle was shown to enter this region. Loss of resistance was then used to demonstrate
that the needle tip lies in a presacral space. The implication being that any injectate would
be located in an adequate position. The potential exception would be a neurodestructive
procedure as radiographic control of needle tip in relation to the rectum should be
performed and recorded. However when aiming for a diagnostic or local anaesthetic based
treatment option we feel that this may become an accepted method.
Toshniwal (2007) In this study, the author analyzed the feasibility, safety, and efficacy of
ganglion impar block by transsacrococcygeal approach. In this prospective study, 16
consecutive patients who required ganglion impar block for CPP were followed for two
months. After informed and written consent, the ganglion impar was blocked under aseptic
precautions, using a transsacrococcygeal approach. The Visual Analogue Scale for pain
(VAS) at presentation time required for the pain to reduce by 50% to be considered
effective and VAS was recorded at different time points during 2-month follow-up, and time
required to perform the procedure, number of attempts, and any complications were also
noted. All the blocks were effective with a mean duration of 12+/-3 minutes for 50%
reduction in VAS. The mean duration required to perform the procedure in neurolytic block
patients was 7.8+/-2 minutes and 5.7+/-1 minutes in therapeutic block patients. There
were no adverse events. All the patients had significant pain relief during 2 month follow-up
Coccygectomy for Coccygodynia Jun 14
6
(p <0.05 compared to baseline). The mean VAS at 2 months was about 2. Statistical
analysis was done by using paired "t"/Wilcoxon signed rank test. A transsacrococcygeal
approach for a ganglion impar block is a technically feasible and safe technique. The author
recommends this technique for neurolysis or radiofrequency ablation of the ganglion impar
and for diagnostic blocks, especially when the diagnosis and further plan of management is
dependent on the response of the diagnostic block.
Per UpToDate (Fletcher et al. 2013) Some consultants inject coccygeal structures, guided by
fluoroscopy, with either local anesthetic or local anesthetic plus corticosteroids. Injections
may be directed at the sacrococcygeal junction, the caudal epidural space, or the ganglion
impar, a midline sympathetic ganglion located just anterior to the sacro-coccygeal junction.
Case reports describe positive results, although pain may be relieved for only a few weeks.
As far as the other Health Plans, Aetna considers Coccygeal ganglion (ganglion impar) block
for coccydynia, pelvic pain, and all other indications as investigational. I could not find any
other Health Plans that had specific policies on this treatment. Hayes, Medline, and NICE
had no information, and UpToDate had minimal information. There are NO specific Clinical
Trials.
Per UpToDate (2013) A minority of patients develop chronic coccydynia, as the patient
noted in the report that was sent. These patients are often referred to specialists in pain
management, or orthopedic surgeons. An algorithm for therapeutic decision-making and
treatment in persistent cases, from the point of view of a pain specialist, has been
published. Many treatments have been advocated but the evidence base for effectiveness is
weak. Patients with intractable symptoms should be referred to a specialist with experience
in managing coccydynia. In the absence of randomized trials of effectiveness, management
with a series of coccygeal injections containing local anesthetic or local anesthetic plus
glucocorticoid, is suggested (Grade 2C). An alternative option is levator ani
massage/stretching and sacrococcygeal joint mobilization. (A Grade 2C recommendation is
a very weak recommendation; other alternatives may be equally reasonable).
In summary, ganglion impar injections or blocks for coccydynia has been around since the
1990's, so this is not a new treatment. When all other treatments have not worked, this
may be something that could be used and approved as medically necessary on a case by
case basis. The studies also note that the nerve blocks using local anesthetics with a fast
onset (eg, lidocaine) were shown to provide short-term relief only. However, after the local
anesthetic block wears off, some of the coccyx pain may start to return, but generally it
returns at a lower severity than existed prior to the injection. Repeat ganglion impar blocks
have been shown to provide additional benefit, further lowering the plateau level of pain. In
patients without complete resolution, repeat injections are often medically necessary and
clinically helpful. Since this treatment is not new, the studies that I found, (i.e., primarily
small case reports, retrospective studies, reviews) are primarily related to various and new
approaches for this block, which the authors feel would be more beneficial regarding the
pain relief.
Scientific Rationale Update – October 2011
Kerr et al. (2011) completed a retrospective review of 62 successive coccygectomy
surgeries for coccygodynia, in 61 patients identified from the surgical database; they had
been treated between 1997 and 2009. The authors succeeded in contacting 26 patients for
follow-up (42.6%). A retrospective chart review was performed, and a telephone
questionnaire was administered to these patients. Data collected included cause, pre- and
postoperative visual analog scale, a graded outcome measure, and patient satisfaction. The
median follow-up time was 37 months (range 2-133 months). The clinical results among the
Coccygectomy for Coccygodynia Jun 14
7
26 patients with follow-up were as follows: 13 excellent, 9 good, 2 fair, and 2 poor. The
overall favorable (excellent and good) outcome after coccygectomy was 84.6%. There were
3 wound infections (11.5%). There were no rectal injuries. An overwhelming majority of
patients were satisfied with the procedure. The authors report the results of their clinical
case series, which to date is the largest in North America. The results closely concur with
previously published case series from Europe. Coccygectomy for chronic intractable
coccygodynia is simple and effective, with a low complication rate.
Scientific Rationale Update - February 2011
In general, prolonged conservative treatment is usually successful in treating coccydynia.
For those that have persistent coccygeal pain that does not respond to conservative
management, coccygectomy may be an option.
Karadimas et al (2010) performed a systematic review is to evaluate the results of
treatment of coccygectomy. Literature retrieval was performed excluding case reports and
tumor related case series, as well as articles published in other languages. In total 24
manuscripts were analyzed. Only 2 of them were prospective studies whereas 22 were
retrospective case series; five were classified as Level III studies and the remaining as Level
IV studies. In total, 671 patients with coccygodynia underwent coccygectomy following
failed conservative management. The sex ratio, male/female was 1:4.4. The most popular
etiology for coccygodynia was direct trauma in 270 patients. 504 of the patients reported an
excellent/good outcome following the procedure. There were 9 deep and 47 superficial
infections. Other complications included two hematomas, six delayed wound healings and
nine wound dehiscence. The overall complication rate was 11%. Patients with history of
spinal or rectal disorders, as well as idiopathic or with compensation issues, had less
predictable outcome than those with history of trauma or childbirth. The reviewer concluded
coccygectomy can provide pain relief to as high as 85% of the cases. The most common
reported complication was wound infection.
In a retrospective study, Trollegaard et al (2011) reported results of 41 patients who
underwent total coccygectomy for coccydynia after failure to respond to six months of
conservative management. Of these, 40 patients were available for clinical review and 39
completed a questionnaire giving their evaluation of the effect of the operation. Excellent or
good results were obtained in 33 of the 41 patients, comprising 18 of the 21 patients with
coccydynia due to trauma, five of the eight patients with symptoms following childbirth and
ten of 12 idiopathic onset. In eight patients the results were moderate or poor, although
none described worse pain after the operation. The only post-operative complication was
superficial wound infection which occurred in five patients and which settled fully with
antibiotic treatment. One patient required re-operation for excision of the distal cornua of
the sacrum. The reviewer concluded total coccygectomy offered satisfactory relief of pain in
the majority of patients regardless of the cause of their symptoms.
Scientific Rationale - Initial
The coccyx, colloquially referred to as the tailbone because it is considered to be a vestigial
remnant of a tail in animals, is the final segment of the human vertebral column, and
consists of four fused coccygeal vertebrae inferior to the sacrum. It is attached to the
sacrum in a fibrocartilaginous joint, which permits limited movement between them. Most
anatomy books wrongly state that the coccyx is normally fused into one rigid segment by
adulthood in most people. In fact, several well-designed X-ray studies (Postacchini [1983];
Kim [1999]) have shown that it is more common for it to be in 3-5 individual bony
segments. Only about 5% of the population have a coccyx in one piece, separate from the
sacrum, as described in anatomy books. This error in anatomy teaching can lead doctors to
Coccygectomy for Coccygodynia Jun 14
8
diagnose a 'fractured coccyx' when they see a coccyx in several segments on x-ray. These
studies also showed that two thirds of people have a coccyx that curves down and slightly
forward, and one third have a coccyx that points straight forward. The spinal cord does not
extend into the coccyx. The coccyx is attached by ligaments to the base of the sacrum,
which is the part of the spine that forms the back of the pelvis. The coccyx provides an
attachment for nine muscles, such as the gluteus maximus, and as something of a shock
absorber when the person sits down. The muscle that is necessary for defecation attaches
to the coccyx.
Coccydynia is a medical term meaning pain in the coccyx or tailbone area, usually brought
on by sitting. Coccydynia is also known as coccygodynia, coccygeal pain, coccyx pain,
coccaglia or, in layperson's terms, buttache. A number of different conditions can cause pain
in the general area of the coccyx, but not all involve the coccyx and the muscles attached to
it. The first task of diagnosis is to determine whether the pain is related to the coccyx.
Physical examination, high resolution x-rays and MRI scans can rule out various causes
unrelated to the coccyx. Although there may be no definitive cause for coccydynia, trauma
from falling or being bumped, repetitive action (horseback riding, extensive bike riding or
rowing), or childbirth can cause tailbone pain. Tailbone pain and lower back pain can mimic
coccydynia in sciatica, infection, pilonidal cysts, and fractured bone. The symptoms and
examination findings of localized tenderness upon direct palpation of the coccyx and/or by
rectal exam is typically all the physician needs to diagnose coccydynia. A simple test to
confirm the diagnosis involves an injection of local anesthetic into the area. If the pain
relates to the coccyx, this should produce immediate relief. Demonstration of radiological
instability of the coccyx as judged by intermittent subluxation or hypermobility seen on
lateral dynamic radiographs when standing and sitting is often seen. If there is any question
about the diagnosis, a CT scan or MRI can be ordered to rule out infection or tumor as a
cause of pain. Rarely, coccydynia is due to the undiagnosed presence of a sacrococcygeal
teratoma or other tumor in the vicinity of the coccyx. In these cases, appropriate treatment
usually involves surgery and/or chemotherapy.
In general, prolonged conservative treatment is usually successful in treating this condition.
The key to treatment is to allow enough time for the symptoms to respond to therapy,
usually more than 12 months. Conservative management should begin with the use of a
nonsteroidal anti-inflammatory drug (NSAID) to reduce inflammation and analgesics to
reduce pain. Initially, this is coupled with a donut-shaped pillow or a gel cushion to decrease
coccygeal pressure and local irritation while sitting. Many physicians also advise the patient
to use hot sitz-type baths to further soothe the irritated coccygeal soft tissues. If this
therapy fails, usually after a minimum of 2 months, most authors consider injection of
corticosteroid and analgesic combination. Local nerve blocks also can be beneficial,
especially when fluoroscopic guidance is used. For patients with recurrent or persistently
troublesome tailbone pain, a therapeutic injection can provide quick, thorough, and
sometimes lasting relief; for some patients, the injection completely resolves the symptoms.
Wray et al (1963) found that 60% of patients responded to local injections of anesthetics
and corticosteroids. The same study showed that 85% responded to this regimen when
combined with digital manipulation of the coccygeal ligaments and the muscles of the pelvic
floor. If traditional injection therapies fail, a neurolytic technique in which lidocaine is
injected at the junction of the sacrum and coccyx just in front of the junction can be tried.
This is directed at the fourth and fifth sacral nerves and the coccygeal nerve. If this provides
good pain relief, then a radiofrequency thermocoagulation probe can be inserted at the
same site and used to ablate these nerves. In 2006, Foye et al published that sometimes
even just a single local nerve block injection at the ganglion impar can give 100% relief of
coccydynia when performed under fluoroscopic guidance.
Coccygectomy for Coccygodynia Jun 14
9
For those few people who have persistent pain that is not alleviated or well-controlled with
conservative treatment, coccygectomy becomes an option in the form of a partial or
complete surgical removal of the coccyx. Although many surgeons are reluctant to perform
this surgery due to its proximity to the anus and the risk of rectal perforation and infection,
it is, however, a relatively simple operation in the hands of those surgeons who are familiar
with the anatomy. The best indications of being a good candidate appear to be an unstable
coccyx on lateral dynamic radiographs or a spur on the coccyx. A one to two-inch incision is
made right over the top of the coccyx, which is located directly under the skin and
subcutaneous fat tissue. There are no muscles to dissect away. The periosteum is then
dissected away from the bone starting on the back and carried around to the front. Staying
in this plane of tissue is very safe, and allows the coccyx to be dissected free and then
separated from the sacrum. The coccyx is then removed and can be sent to pathology if
there is any question as to whether or not it contains a tumor. To preserve normal
defecation, coccygectomy normally is accompanied by re-attachment of the two levator ani
muscles. The operation takes about thirty minutes to perform and can be done on an
outpatient basis. Recently, a limited coccygectomy has been proposed that involves only the
resection of the mobile or hypermobile segment of the coccyx. This has been identified by
fluoroscopic evaluation and local anesthetic injection prior to any surgery being attempted.
The most trying part of the operation is that it may take anywhere from three months to a
year after the surgery before the patient may begin to experience any relief from their
symptoms. The main risk with the surgery includes severe infection, if the surgical plane of
dissection strays from the subperiosteal region around the coccyx causing the rectal vault to
be violated.
Overall, there is only a number of small to modest-sized case series that have seemed to
indicate that a significant amount of properly selected patients may receive significant rates
of symptomatic relief after coccygectomy, but that postoperative complications (especially
infection) are common. The authors of these reports have generally indicated that surgery
was performed in only a small percentage of the patients presenting with coccydynia,
stating that prolonged conservative treatment (from 6 to 12 months) is more often than not
successful in treating coccydynia in the vast majority of patients (80%) prior to considering
surgery. They report that those who do not respond to a thorough course of nonsurgical
treatment and demonstrate radiological instability of the coccyx have a good a chance of
cure (90%) with coccygectomy. In those patients whose coccydynia had been preceded by
trauma, superior surgical results have been reported in the medical literature.
Wray et al (1985) reported in the British Journal of Bone and Joint Surgery that they had a
90% success rate for the procedure in 20 patients. Maigne et al (2000) established that
patients with luxation or hypermobility were better responders to a local intradiscal
corticosteroid injection than patients with normal coccyges. About two months after the
injection, 50% of the patients with luxation or hypermobility were improved or healed,
whereas only 27% of the patients with normal coccyges improved. In case of relapse, a
second injection may be performed. If the result is better after this second injection (a
longer relief), the prognosis is good. If the relief is shorter, injections do not appear to be
the right treatment. Usually, spicules (spurs) do very well after one or two injections.
Maigne et al (2000) also attempted to define criteria for selection of patients for
coccygectomy. They chose to prospectively study 37 patients with chronic pain secondary to
coccygeal instability unrelieved by conservative treatment and who were not involved in
litigation. Patients were followed up for a minimum of two years after coccygectomy, with
independent assessment at two years. There were 23 excellent, 11 good and three poor
results. The mean time to definitive improvement was four to eight months. Their
conclusion was that coccygectomy gave good results in this group of patients.
Coccygectomy for Coccygodynia Jun 14
10
Wood (2004) retrospectively reviewed his experience with coccygectomy and compared it
with injections for the relief of coccygodynia in 51 consecutive patients to determine rates of
success, patient satisfaction and complications. All of the patients complained of pain while
sitting and had localized pain to external and internal palpation of the coccyx on physical
examination. Nonoperative treatment (medications, cushions, manual therapy) had failed to
relieve the patients' symptoms. All patients were seen in follow-up for physical examination
and completed a questionnaire by an independent examiner. Follow-up of the patients was
26 months (range 12-59 months). Follow-up data were available on 45 of the 51 enrolled.
The patients were divided as follows: 20 patients were treated with total coccygectomy and
25 patients were treated with injection therapy. Of those treated operatively, 18 patients
(90%) felt improved and were satisfied with the procedure. Two patients felt their
symptoms to be unchanged and were dissatisfied. Postoperative complications included
seven wound problems: four superficial infections and three patients with persistent
drainage. All resolved with local wound care and oral antibiotics. No further surgery was
necessary. There were no bowel injuries and no reports of rectal sphincter problems. Of
those treated with injections, 5 of the 25 (20%) felt improvement and were satisfied.
Sixteen (64%) were not improved, and four (16%) felt worse. Five (20%) eventually were
treated with coccygectomy, four with eventual satisfactory relief in symptoms. They
concluded that, despite the potential for wound problems, coccygectomy for relief of
coccygodynia can be a safe and effective treatment option with a high patient satisfaction
rate. Fogel (2004) came to the same conclusion that coccygectomy usually is successful in
carefully selected patients, with the best results in those with radiographically demonstrated
abnormalities of coccygeal mobility.
Doursounian et al (2005) reported their experience of 61 patients with instability-related
coccygodynia to validate an objective criterion for patient selection: radiological instability of
the coccyx (intermittent luxation or hypermobility of the coccyx). All patients were
unrelieved by conservative treatment, and not involved in litigation. Twenty-seven patients
had hypermobility of the coccyx and 33 subluxation. In all cases, the unstable portion was
removed through a limited incision directly over the coccyx. The outcome was assessed
using a detailed questionnaire. Follow-up was between 12 months and more than 30
months. The outcome was rated excellent or good in 53 patients, fair in one, and poor in
seven. There were nine patients with infection requiring reoperation. The average time to
definitive improvement was 4 to 8 months, which is fairly long, but in line with other
authors' reports. They proposed that such a long interval of time could be explained by a
'phantom limb syndrome' with coccygectomy being an amputation. When improvement is
slow to appear, they prescribed Elavil (amiltriptyline) that seemed to alleviate the constant
pain.
Sehirlioglu (2007) retrospectively analyzed 74 patients who were surgically managed for
traumatic coccygodynia after a failure of conservative treatment and performed a critical
review of the results obtained in comparison to the literature. The mean follow up was 4.1
years (range, 2-8 years). The mean age of patients on the date of surgery was 43.4 years
(range, 16-65 years). The average duration of pain prior to surgery was 7 months (range, 3
months to one year). They discovered that all but three patients had either good or
excellent results after surgery. Three patients reported postoperative pain lasting 3-6
months. All three had good results after re-operation of a proximal segment without
excision. Five postoperative complications, four superficial and one deep infection were
observed. In patient’s wit, conservative therapy-resistant, posttraumatic coccygodynia, they
surmised that coccygectomy is a feasible management option. They recommend total or
partial coccygectomy confined to the removal of the mobile bony element using a
longitudinal incision in carefully selected and well-informed patients.
Coccygectomy for Coccygodynia Jun 14
11
To summarize, coccydynia has been a somewhat neglected topic and coccygectomy remains
a controversial subject in the medical literature. Some authors have reported good results;
however, selection criteria are ill-defined. Others advise against this procedure. Pyper
(1957) stated “there is no constant factor in the history, no reliable physical sign, and no
specific radiographic change that can be regarded as a definite pointer in advising
operation”. Although most papers report retrospective analyses of particular treatments or
offer anecdotal comments on a handful of cases, one can come to the conclusion that the
outcome of coccygectomy is largely dependent on pre-operative patient selection and
remains a treatment of last resort, reserved for the small percentage of patients who fail to
obtain adequate relief via nonsurgical treatments. A logical, step-wise approach is to almost
always provide the full spectrum of modern pain management interventions prior to
considering surgery.
Review History
November 2007 Medical Advisory Council initial approval
February 2011 Update – no revisions
October 2011 Update - no revisions
October 2012 Update – no revisions
October 2013 Update – no revisions
November 2013 Update – Added ganglion impar coccygeal injection
medically necessary for chronic coccydynia when other
conservative measures (i.e. treatment with oral analgesics,
physical therapy, epidural steroid injections) have not
alleviated the pain and the individual is not a surgical
candidate. Title of policy changed to ‘Coccygectomy and
Treatments for Coccydynia’. Codes updated.
June 2014 Update – no revisions. Codes updated.
References – Update June 2014
1. Kim HS, Yang SH, Park HJ, et al. Glomus tumor as a cause of coccydynia. Skeletal
Radiol. 2013 Oct;42(10):1471-3. doi: 10.1007/s00256-013-1654-z. Epub 2013 Jun 4.
References – Update November 2013
1. Buttaci CJ, Foye PM, Stitik TP, et al. Coccydynia successfully treated with ganglion
impar blocks: a case series. Am J Phys Med Rehabil. Mar 2005;84(3):218.
2. Datir A. CT-guided injection for ganglion impar blockade: a radiological approach to the
management of coccydynia. Clin Radiol. 01-JAN-2010; 65(1): 21-5.
3. Fletcher RH. Coccydynia (coccygodynia). UpToDate. July 11, 2013.
4. Foye et al. Coccyx Pain Treatment & Management. Medscape. January 23, 2012.
5. Foye PM. Paracoccygeal corkscrew approach to ganglion impar injections for tailbone
pain. Pain Pract. 01-JUL-2009; 9(4): 317-21.
6. Foye PM. Ganglion impar injection techniques for coccydynia (coccyx pain) and pelvic
pain. Anesthesiology. May 2007;106(5):1062-3.
7. Foye PM. New approaches to ganglion impar blocks via coccygeal joints. Reg Anesth
Pain Med. May-Jun 2007;32(3):269.
8. Johnston PJ. Blockade of the ganglion impar (walther), using ultrasound and a loss of
resistance technique. Prague Med Rep - 01-JAN-2012; 113(1): 53-7.
9. Kabbara AI. Transsacrococcygeal ganglion impar block for postherpetic neuralgia.
Anesthesiology. Jul 2005;103(1):211-2. 15.
Coccygectomy for Coccygodynia Jun 14
12
10. A. Kozlowski K. CT-guided blocks and neuroablation of the ganglion impar (Walther) in
perineal pain: anatomy, technique, safety, and efficacy. Clin J Pain. 01-SEP-2009;
25(7): 570-6.
11. Kuthuru M, Kabbara AI, Oldenburg P, et al. Coccygeal pain relief after
transsacrococcygeal block of the ganglion Impar under fluoroscopy: a case report. Arch
Phys Med Rehabil. Sep 2003;84(9):E24.
12. Lin CS. Ultrasound-guided ganglion impar block: a technical report. Pain Med. 01-MAR-
2010; 11(3): 390-4.
13. Reig E, Abejón D, Del Pozo C, et al. Thermocoagulation of the ganglion impar or
ganglion of walther: description of a modified approach. Preliminary results in chronic,
nononcological pain. Pain Pract. Jun 2005;5(2):103-10.
14. Sağır O. Application of ganglion impar block in patient with coccyx dislocation].
Agri. 01-JUL-2011; 23(3): 129-33.
15. Sáenz MC, Cerrillo JAI, Colomo CV, et al. Infiltration of impar and caudal ganglia in the
management of traumatic coccydynia refractory to conventional analgesic treatment.
Vol. 55. Núm. 05. September 2011 - October 2011.
16. Scott-Warren JT. Ganglion impar blockade: a review. Curr Pain Headache Rep - 01-JAN-
2013; 17(1): 306.
17. Toshniwal GR. Transsacrococcygeal approach to ganglion impar block for management
of chronic perineal pain: a prospective observational study. Pain Physician - 01-SEP-
2007; 10(5): 661-6.
18. Williams BS. Superior Hypogastric Plexus, Ganglion Impar Blocks, and Neurolysis.
Comprehensive Treatment of Chronic pain by Medical, Interventional, and Integrative
Approaches. 2013. pp 435-440.
References – Update October 2013
1. Aggarwal A, Kumar S, Kumar D. Factors influencing the evaluation and management
outcomes of coccygodynia: a literature review. J Back Musculoskelet Rehabil. 2013 Jan
1;26(2):105-15.
References – Update October 2012
1. Atim A, Ergin A, Bilgiç S, et al. Pulsed radiofrequency in the treatment of coccygodynia.
Agri. Jan 2011;23(1):1-6.
2. Foye PM. Coccyx Pain Treatment & Management. Medscape. January 23, 2012.
References – Update October 2011
1. Fletcher RH. Coccygectomy for Coccygodynia. UpToDate. May 13, 2010, Updated March
23, 2012.
2. Kerr EE. Coccygectomy for chronic refractory coccygodynia: clinical case series and
literature review. J Neurosurg Spine. 01-MAY-2011; 14(5): 654-63.
3. Aarby NS. Coccygectomy can be a treatment option in chronic coccygodynia]. Laeger
U. 14-FEB-2011; 173(7): 495-500.
References – Update February 2011
1. Bilgic S, Kurklu M, Yurttaş Y, et al. Coccygectomy with or without periosteal resection.
Int Orthop. 2010 Apr;34(4):537-41.
2. Lyons M. Coccygodynia: Treatment. eMedicine. Oct 2009. Available at:
http://emedicine.medscape.com/article/1264763-treatment
3. Karadimas EJ, Trypsiannis G, Giannoudis PV. Surgical treatment of coccygodynia: an
analytic review of the literature. Eur Spine J. 2010 Nov 3, Eur Spine J 2011; 20:698.
4. Patijn J, Janssen M, Hayek S, et al. Coccygodynia. Pain Pract. 2010 Nov-
Dec;10(6):554-9
Coccygectomy for Coccygodynia Jun 14
13
5. Trollegaard AM, Aarby NS, Hellberg S. Coccygectomy: an effective treatment option for
chronic coccydynia: retrospective results in 41 consecutive patients. J Bone Joint Surg
Br. 2010 Feb;92(2):242-5.
References - Initial
1. Foye PM. Ganglion impar injection techniques for coccydynia (coccyx pain) and pelvic
pain. Anesthesiology. May 2007;106(5):1062-3.
2. Foye PM. New approaches to ganglion impar blocks via coccygeal joints. Reg Anesth
Pain Med. May-Jun 2007;32(3):269. .
3. Foye PM. Reasons to delay or avoid coccygectomy for coccyx pain. Injury. 2007 Sep 18.
4. Cebesoy O, Guclu B, Kose KC, et al. Coccygectomy for coccygodynia: Do we really have
to wait? Injury. 2007 Apr 3.
5. Sehirlioglu A. Coccygectomy in the surgical treatment of traumatic coccygodynia. Injury
2007;38(2):182-7.
6. Foye PM. Coccydynia (coccyx pain) caused by chordoma. Int Orthop. Jun
2007;31(3):427.
7. Mouhsine E, Garofalo R, Chevalley F, et al. Posttraumatic coccygeal instability. Spine J.
2006 Sep-Oct;6(5):544-9.
8. Balain B, Eisenstein SM, Alo GO, et al. Coccygectomy for coccydynia: case series and
review of literature. Spine. 2006 Jun 1;31(13):E414-20.
9. Foye PM, Buttaci CJ, Stitik TP, et al. Successful injection for coccyx pain. Am J Phys Med
Rehabil. Sep 2006;85(9):783-4.
10. Maigne JY, Chatellier G, Faou ML, et al. The treatment of chronic coccydynia with
intrarectal manipulation: a randomized controlled study. Spine. Aug 15
2006;31(18):E621-7.
11. Medical papers relevant to coccydynia. Available at:
http://www.coccyx.org/medabs/index.htm
12. Pennekamp PH, Kraft CN, Stütz A, et al. Coccygectomy for coccygodynia: does
pathogenesis matter?. J Trauma. Dec 2005;59(6):1414-9. .
13. Buttaci CJ, Foye PM, Stitik TP, et al. Coccydynia successfully treated with ganglion
impar blocks: a case series. Am J Phys Med Rehabil. Mar 2005;84(3):218.
14. Kabbara AI. Transsacrococcygeal ganglion impar block for postherpetic neuralgia.
Anesthesiology. Jul 2005;103(1):211-2. .
15. Reig E, Abejón D, Del Pozo C, et al. Thermocoagulation of the ganglion impar or
ganglion of walther: description of a modified approach. Preliminary results in chronic,
nononcological pain. Pain Pract. Jun 2005;5(2):103-10. .
16. Fogel GR. Coccygodynia: evaluation and management. J Am Acad Orthop Surg
2004;12(1): 49-54
17. Doursounian L, Maigne JY, Faure F, Chatellier G. Coccygectomy for instability of the
coccyx. Int Orthop. 2004 Jun;28(3):176-9.
18. Wood KB, Mehbod AA. Operative treatment for coccygodynia. J Spinal Disord Tech. Dec
2004;17(6):511-5. .
19. Hodges SD, Eck JC, Humphreys SC. A treatment and outcomes analysis of patients with
coccydynia. Spine J. Mar-Apr 2004;4(2):138-40. .
20. Kuthuru M, Kabbara AI, Oldenburg P, et al. Coccygeal pain relief after
transsacrococcygeal block of the ganglion Impar under fluoroscopy: a case report. Arch
Phys Med Rehabil. Sep 2003;84(9):E24.
21. Maigne JY, Lagauche D, Doursounian L. Instability of the coccyx in coccydynia. J Bone
Joint Surg Br. 2000 Sep;82(7):1038-41.
22. Maigne JY, Doursounian L, Chatellier G: Causes and mechanisms of common
coccydynia: role of body mass index and coccygeal trauma. Spine 2000 Dec 1; 25(23):
3072-9.
Coccygectomy for Coccygodynia Jun 14
14
23. Kim NH; Suk KS: Clinical and radiological differences between traumatic and idiopathic
coccygodynia. Yonsei Med J, 1999 Jun;40:3, 215-20.
24. Valen B, Bringedal K: Coccygectomy for coccygodynia. Tidsskr Nor Laegeforen 1999 Apr
20; 119(10): 1429-30.
25. Alo GO, Eisenstein SM, Darby A. The sacro-coccygeal joint in coccydynia. J Bone Joint
Surg Br. 1998;80-B(2S):196.
26. Maigne JY: Treatment Strategies for Coccydynia. 1998; Available at:
http://www.coccyx.org.
27. Maigne JY, Tamalet B. Standardized radiologic protocol for the study of common
coccygodynia and characteristics of the lesions observed in the sitting position. Clinical
elements differentiating luxation, hypermobility, and normal mobility. Spine. Nov 15
1996;21(22):2588-93.
28. Maigne JY, Guedj S, Straus C: Idiopathic coccygodynia. Lateral roentgenograms in the
sitting position and coccygeal discography. Spine 1994 Apr 15; 19(8): 930-4.
29. Maigne JY, Guedj S, Fautrel B. Coccygodynia: value of dynamic lateral x-ray films in
sitting position. Rev Rhum Mal Osteoartic. Nov 30 1992;59(11):728-31. .
30. Wray CC, Easom S, Hoskinson J. Coccydynia. Aetiology and treatment. J Bone Joint
Surg Br. Mar 1991;73(2):335-8.
31. Plancarte R, Amescua C, Patt RB, et al. Presacral blockade of the ganglion of Walther
(ganglion Impar). Anesthesiology. 1990;73(3a):A751.
32. Traycoff RB, Crayton H, Dodson R: Sacrococcygeal pain syndromes: diagnosis and
treatment. Orthopedics 1989 Oct; 12(10): 1373-7.
33. Postacchini F, Massobrio M: Idiopathic coccygodynia. Analysis of fifty-one operative
cases and a radiographic study of the normal coccyx. J Bone Joint Surg Am 1983 Oct;
65(8): 1116-24.
Important Notice
General Purpose.
Health Net's National Medical Policies (the "Policies") are developed to assist Health Net in administering plan
benefits and determining whether a particular procedure, drug, service or supply is medically necessary. The
Policies are based upon a review of the available clinical information including clinical outcome studies in the peer-
reviewed published medical literature, regulatory status of the drug or device, evidence-based guidelines of
governmental bodies, and evidence-based guidelines and positions of select national health professional
organizations. Coverage determinations are made on a case-by-case basis and are subject to all of the terms,
conditions, limitations, and exclusions of the member's contract, including medical necessity requirements. Health
Net may use the Policies to determine whether under the facts and circumstances of a particular case, the
proposed procedure, drug, service or supply is medically necessary. The conclusion that a procedure, drug, service
or supply is medically necessary does not constitute coverage. The member's contract defines which procedure,
drug, service or supply is covered, excluded, limited, or subject to dollar caps. The policy provides for clearly
written, reasonable and current criteria that have been approved by Health Net’s National Medical Advisory Council
(MAC). The clinical criteria and medical policies provide guidelines for determining the medical necessity criteria for
specific procedures, equipment, and services. In order to be eligible, all services must be medically necessary and
otherwise defined in the member's benefits contract as described this " Important Notice" disclaimer. In all cases,
final benefit determinations are based on the applicable contract language. To the extent there are any conflicts
between medical policy guidelines and applicable contract language, the contract language prevails. Medical policy
is not intended to override the policy that defines the member’s benefits, nor is it intended to dictate to providers
how to practice medicine.
Policy Effective Date and Defined Terms.
The date of posting is not the effective date of the Policy. The Policy is effective as of the date determined by
Health Net. All policies are subject to applicable legal and regulatory mandates and requirements for prior
notification. If there is a discrepancy between the policy effective date and legal mandates and regulatory
requirements, the requirements of law and regulation shall govern. * In some states, prior notice or posting on the
website is required before a policy is deemed effective. For information regarding the effective dates of Policies,
contact your provider representative. The Policies do not include definitions. All terms are defined by Health Net.
For information regarding the definitions of terms used in the Policies, contact your provider representative.
Policy Amendment without Notice.
Coccygectomy for Coccygodynia Jun 14
15
Health Net reserves the right to amend the Policies without notice to providers or Members. In some states, prior
notice or website posting is required before an amendment is deemed effective.
No Medical Advice.
The Policies do not constitute medical advice. Health Net does not provide or recommend treatment to members.
Members should consult with their treating physician in connection with diagnosis and treatment decisions.
No Authorization or Guarantee of Coverage.
The Policies do not constitute authorization or guarantee of coverage of particular procedure, drug, service or
supply. Members and providers should refer to the Member contract to determine if exclusions, limitations, and
dollar caps apply to a particular procedure, drug, service or supply.
Policy Limitation: Member’s Contract Controls Coverage Determinations.
The determination of coverage for a particular procedure, drug, service or supply is not based upon the Policies,
but rather is subject to the facts of the individual clinical case, terms and conditions of the member’s contract, and
requirements of applicable laws and regulations. The contract language contains specific terms and conditions,
including pre-existing conditions, limitations, exclusions, benefit maximums, eligibility, and other relevant terms
and conditions of coverage. In the event the Member’s contract (also known as the benefit contract, coverage
document, or evidence of coverage) conflicts with the Policies, the Member’s contract shall govern. Coverage
decisions are the result of the terms and conditions of the Member’s benefit contract. The Policies do not replace or
amend the Member’s contract. If there is a discrepancy between the Policies and the Member’s contract, the
Member’s contract shall govern.
Policy Limitation: Legal and Regulatory Mandates and Requirements
The determinations of coverage for a particular procedure, drug, service or supply is subject to applicable legal and
regulatory mandates and requirements. If there is a discrepancy between the Policies and legal mandates and
regulatory requirements, the requirements of law and regulation shall govern.
Policy Limitations: Medicare and Medicaid
Policies specifically developed to assist Health Net in administering Medicare or Medicaid plan benefits and
determining coverage for a particular procedure, drug, service or supply for Medicare or Medicaid members shall
not be construed to apply to any other Health Net plans and members. The Policies shall not be interpreted to limit
the benefits afforded Medicare and Medicaid members by law and regulation.
Coccygectomy for Coccygodynia Jun 14
16
You might also like
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (890)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Electrical Stimulation: Prepared By: Floriza P. de LeonDocument49 pagesElectrical Stimulation: Prepared By: Floriza P. de LeonFloriza de Leon75% (4)
- Health and Safety Manual FINALDocument61 pagesHealth and Safety Manual FINALbmarsh10100% (2)
- PILATES FOR LIFE Taster PDFDocument20 pagesPILATES FOR LIFE Taster PDFEma GhinterNo ratings yet
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Types of Skin LesionsDocument5 pagesTypes of Skin LesionsZielledee100% (2)
- IG2 68J S.J Steel PVT LTD 1 - 084932Document16 pagesIG2 68J S.J Steel PVT LTD 1 - 084932Muhammad Farooq Malik100% (1)
- Wound Care and Wound DressingDocument46 pagesWound Care and Wound DressingAj Macoto50% (2)
- Thoracolumbar Spine Trauma Classification and ManagementDocument29 pagesThoracolumbar Spine Trauma Classification and ManagementFernaldi Anggadha100% (1)
- Virchow's Triad and Thrombosis PathogenesisDocument18 pagesVirchow's Triad and Thrombosis PathogenesisEslam Almassri100% (1)
- Electrical Burn PathophysiologyDocument1 pageElectrical Burn PathophysiologydanicaNo ratings yet
- Assisting in Application of CastDocument9 pagesAssisting in Application of CastJames PanesNo ratings yet
- Continuum Spinal Cord AnatomyDocument25 pagesContinuum Spinal Cord AnatomyslojnotakNo ratings yet
- Installation Manual 1VDD005976 GB - Rev December 2015Document41 pagesInstallation Manual 1VDD005976 GB - Rev December 2015maruf048100% (1)
- Taylor v. MeralcoDocument2 pagesTaylor v. MeralcoKim ManaloNo ratings yet
- An Overview of Coccyx Pain: Causes and Treatment OptionsDocument4 pagesAn Overview of Coccyx Pain: Causes and Treatment OptionsJose Luis Pimentel RosarioNo ratings yet
- Coccygectomy Relieves Stubborn CoccydyniaDocument4 pagesCoccygectomy Relieves Stubborn CoccydyniaDiaz RandanilNo ratings yet
- Surgical technique of coccygectomy: review of 28 studiesDocument7 pagesSurgical technique of coccygectomy: review of 28 studiesDiaz RandanilNo ratings yet
- Coccyx 3 RXDocument6 pagesCoccyx 3 RXRudolfGerNo ratings yet
- Cover JR THT CikaDocument1 pageCover JR THT CikanobumblebeeNo ratings yet
- EpididymoDocument1 pageEpididymoDiaz RandanilNo ratings yet
- Characteristics GroupaasDocument8 pagesCharacteristics GroupaasDiaz RandanilNo ratings yet
- Cover JR THT CikaDocument1 pageCover JR THT CikanobumblebeeNo ratings yet
- Original Article Safety of Dexamethasone in PemphigusDocument5 pagesOriginal Article Safety of Dexamethasone in PemphigusTara WandhitaNo ratings yet
- Daftar PustakaDocument3 pagesDaftar PustakaDiaz RandanilNo ratings yet
- Epididymitis Is The Most Common Cause of Intrascrotal InflammationDocument6 pagesEpididymitis Is The Most Common Cause of Intrascrotal InflammationDiaz RandanilNo ratings yet
- Epididymitis Is The Most Common Cause of Intrascrotal InflammationDocument6 pagesEpididymitis Is The Most Common Cause of Intrascrotal InflammationDiaz RandanilNo ratings yet
- Original Article Safety of Dexamethasone in PemphigusDocument5 pagesOriginal Article Safety of Dexamethasone in PemphigusTara WandhitaNo ratings yet
- EpididymoDocument1 pageEpididymoDiaz RandanilNo ratings yet
- EpididymoDocument1 pageEpididymoDiaz RandanilNo ratings yet
- Characteristics GroupaasDocument8 pagesCharacteristics GroupaasDiaz RandanilNo ratings yet
- Specific FractureDocument19 pagesSpecific FractureDiaz RandanilNo ratings yet
- Lateral RhinotomyDocument11 pagesLateral RhinotomyDiaz RandanilNo ratings yet
- Clin Infect Dis. 2012 1426 8xfrdDocument3 pagesClin Infect Dis. 2012 1426 8xfrdDiaz RandanilNo ratings yet
- Medial Ectropion Repair of Lower Eyelids With A Cicatricial ComponentDocument3 pagesMedial Ectropion Repair of Lower Eyelids With A Cicatricial ComponentDiaz RandanilNo ratings yet
- Congenital: Ectropion AND DistichiasisDocument38 pagesCongenital: Ectropion AND DistichiasisDiaz RandanilNo ratings yet
- Postpartum Hemorrhage 12-01Document50 pagesPostpartum Hemorrhage 12-01pkmmanaluNo ratings yet
- Open FractureDocument20 pagesOpen FractureDiaz RandanilNo ratings yet
- 11.ok-Lap. Kas. Dr. IqbalaDocument2 pages11.ok-Lap. Kas. Dr. IqbalaDiaz RandanilNo ratings yet
- Clinicopathologic Reports, Case Reports, and Small Case SeriesDocument3 pagesClinicopathologic Reports, Case Reports, and Small Case SeriesDiaz RandanilNo ratings yet
- Entropion and Ectropion Repair: BackgroundDocument10 pagesEntropion and Ectropion Repair: BackgroundDiaz RandanilNo ratings yet
- Background: FrequencyDocument2 pagesBackground: FrequencyDiaz RandanilNo ratings yet
- Radiologi Bone TumourDocument56 pagesRadiologi Bone TumourAwang WibisonoNo ratings yet
- Bone Tumor Diagnosis and Treatment Yarsi University 2008Document17 pagesBone Tumor Diagnosis and Treatment Yarsi University 2008Diaz RandanilNo ratings yet
- Chicken Wing DissectionDocument4 pagesChicken Wing DissectionGeorge HarrisonNo ratings yet
- Physiological Principles of SotaiDocument13 pagesPhysiological Principles of SotaiBuyu IkkanNo ratings yet
- Dokumen PDF 12Document86 pagesDokumen PDF 12Cindy AnggrainiNo ratings yet
- KTJ ComparisonDocument1 pageKTJ Comparisoninfo_ktjNo ratings yet
- MSK practice quiz model answersDocument3 pagesMSK practice quiz model answersJenniferChenNo ratings yet
- PainDocument3 pagesPainAdie't Crisnandaezc Sieep PuoolNo ratings yet
- 2 4 37Document4 pages2 4 37Rizky Ananda PutriNo ratings yet
- Elevated Intracranial PressureDocument53 pagesElevated Intracranial PressureHandre PutraNo ratings yet
- Balan SysDocument84 pagesBalan SysVeronica Montiel TerronNo ratings yet
- Blood Supply of Head and NeckDocument29 pagesBlood Supply of Head and NeckBM mugalNo ratings yet
- Hamstring Muscle Injuries - OrthoInfo - AAOSDocument8 pagesHamstring Muscle Injuries - OrthoInfo - AAOSAndy Delos ReyesNo ratings yet
- HO Ortho NotesDocument13 pagesHO Ortho NotesAhmad Syahmi YZNo ratings yet
- Extortion: A Stargate SG-1 Fanfiction Short StoryDocument26 pagesExtortion: A Stargate SG-1 Fanfiction Short StoryAKarswyllNo ratings yet
- The Differences Between Modifiers 51 and 59Document5 pagesThe Differences Between Modifiers 51 and 59Randy MarmerNo ratings yet
- Mobile Foam Unit Technical SpecsDocument2 pagesMobile Foam Unit Technical SpecskennymagallanesNo ratings yet
- Manual Quebradora Rock LabsDocument73 pagesManual Quebradora Rock LabsquintanacalzadillasjaimeNo ratings yet
- Health Week 4 - 3rd QuarterDocument5 pagesHealth Week 4 - 3rd QuarterNoemelyn VecinaNo ratings yet