Professional Documents
Culture Documents
A New Standard For Malignant Pleural Mesothelioma
Uploaded by
Ari0 ratings0% found this document useful (0 votes)
12 views3 pagesmalignancy
Original Title
A New Standard for Malignant Pleural Mesothelioma
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentmalignancy
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
12 views3 pagesA New Standard For Malignant Pleural Mesothelioma
Uploaded by
Arimalignancy
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 3
Comment
assessed clinically relevant ecacy, for which they
selected small bowel obstruction as a suitable indicator.
By diagnosing small bowel obstruction at the time
of reoperation, they avoided some of the variability
associated with subjective surgical endpoints. Reduction
of postoperative complications after elective surgery is
undoubtedly of interest to patients, but the investigators
could have enhanced the clinical importance of their
results by including patient-reported outcome measures.
Such measures should routinely be built into future trials.
The double-blind trial has long been held as the
ideal platform for clinical evaluation and this blinding
is perhaps even more important for complex surgical
interventions that encompass multiple variables.
The ideal surgical trial would go a step further and be
triple blinded; the surgeon, patient, and outcome assessor
would all be masked to treatment assignment. Masking of
the patient and the assessor to the intervention is often
possible, but blinding the surgeon to the intervention is
not possible. For patient masking, the ethical dilemma of
future doctors knowing about the procedure performed
can be overcome through use of coding in the patients
notes, with unblinding through a central register. Surgical
trials should seek to stipulate blinded outcome assessors.
The study by Stenberg and colleagues will help
surgeons to make better decisions and to rene
their technique. Mesenteric defects should be closed
routinely after laparoscopic gastric bypass to reduce the
incidence of internal hernia and subsequent small bowel
obstruction. However, defect closure is associated with
increased short-term complications, which might be
related to a surgical learning curve.
This study has many strengths and a few imperfections.
There remains room for improvement in the design and
delivery of technique and technology trials during early
phase implementation and late phase evaluation. As a
multidisciplinary community, we should keep striving
for the perfect surgical trial because improvements will
accelerate standardised dissemination of new techniques
and increase trial participation, resulting in greater
benets for more patients.
*Aneel Bhangu, Dion Morton
Academic Department of Surgery, Queen Elizabeth Hospital,
Birmingham B15 2TH, UK
aneelbhangu@doctors.org.uk
We declare no competing interests.
1
2
4
5
6
McCulloch P, Altman DG, Campbell WB, et al. No surgical innovation without
evaluation: the IDEAL recommendations. Lancet 2009; 374: 110512.
Stenberg E, Szabo E, gren G, et al. Closure of mesenteric defects in
laparoscopic gastric bypass: a multicentre, randomised, parallel, open-label
trial. Lancet 2016; published online Feb 16. http://dx.doi.org/10.1016/
S0140-6736(15)01126-5.
Harrysson IJ, Cook J, Sirimanna P, Feldman LS, Darzi A, Aggarwal R.
Systematic review of learning curves for minimally invasive abdominal
surgery: a review of the methodology of data collection, depiction of
outcomes, and statistical analysis. Ann Surg 2014; 260: 3745.
Blencowe NS, Brown JM, Cook JA, et al. Interventions in randomised controlled
trials in surgery: issues to consider during trial design. Trials 2015; 16: 392.
Bhangu A, Kolias AG, Pinkney T, Hall NJ, Fitzgerald JE. Surgical research
collaboratives in the UK. Lancet 2013; 382: 109192.
Bhangu A, Ives N, Magill L. Feasibility study from a randomised controlled
trial of standard closure of stoma site versus biologic mesh reinforcement.
Colorectal Dis (in press).
Chapman S, Shelton B, Marutappu M, Bhangu A. Assessment quality of
novel implantable biotechnology in gastrointestinal surgery:
cross-sectional, observational study. Colorectal Dis 2015; 17 (suppl 2): 35.
A new standard for malignant pleural mesothelioma
Published Online
December 21, 2015
http://dx.doi.org/10.1016/
S0140-6736(15)01311-2
See Articles page 1405
1352
Mesothelioma is an asbestos-related malignancy that
begins in the pleural lining of the lung, pericardium,
peritoneum, or testes. Early-stage pleural mesothelioma
can be resected, but almost always recurs. Many patients
are diagnosed at an advanced stage of disease, at which
point surgery has no role. Since 2003, the standard
treatment for unresectable disease has been combination
chemotherapy with cisplatin and pemetrexed.1 Despite
many attempts, until now, no regimen has further
improved survival. Although addiction to oncogenes
occurs in some cancers, most molecular alterations
in mesothelioma occur in tumour suppressors and
the corresponding drug target is unclear. Research is
underway to exploit some of the most common molecular
aberrations and dependencies in mesothelioma.24 For
example, the important role of vascular endothelial
growth factor (VEGF) signalling in mesothelioma has
been known for many years,5,6 but studies of single-drug
VEGF inhibitors were disappointing.710
In this context, the Intergroupe Francophone de
Cancrologie Thoracique began randomly allocating
448 patients with unresectable malignant pleural
mesothelioma to cisplatin and pemetrexed with or
without bevacizumab (an antibody against VEGF).
As reported by Grard Zalcman and colleagues11 in
The Lancet, the trials primary endpoint of overall
www.thelancet.com Vol 387 April 2, 2016
survival was improved in those who received cisplatin
and pemetrexed plus bevacizumab, at 188 months with
bevacizumab versus 161 months without (hazard ratio
077 [95% CI 062095]). Grade 34 adverse events
were more common in the bevacizumab group (158
[71%] of 222 patients) than in the non-bevacizumab
group (139 [62%] of 224 patients), and more patients
stopped rst-line treatment because of toxic eects in
the bevacizumab group (53 [243%] of 218 patients)
than in the non-bevacizumab group (13 [60%] of 217;
dierence 183% [117249]).
Early all-cause mortality was similar between
the groups: ve (28%) of 178 patients without
bevacizumab versus eight (49%) of 164 patients
with bevacizumab. Somewhat unexpectedly, fewer
patients in the bevacizumab group went on to receive
poststudy chemotherapy: 129 (620%) of 208 patients
in the bevacizumab group versus 152 (724%) of
210 patients in the non-bevacizumab group. Even with
the dierences in early discontinuation and poststudy
treatment favouring the group without bevacizumab,
overall survival was improved in the bevacizumab group.
Of note, while this trial was taking place, a randomised
phase 2 study12 of cisplatin and gemcitabine with or
without bevacizumab in unresectable mesothelioma
reported no signicant dierence in progression-free
survival and was underpowered for overall survival.
The results of Zalcman and colleagues trial11 warrant
routine use of bevacizumab in addition to cisplatin and
pemetrexed for unresectable mesothelioma. In patients
without contraindications to bevacizumab, addition of
bevacizumab to cisplatin and pemetrexed is appropriate,
with acknowledgment that toxic eects and treatment
discontinuation will be more common than without
bevacizumab. However, despite the impressive results
of this rigorously designed and executed phase 3
clinical trial, many questions remain. For patients who
cannot tolerate cisplatin, should bevacizumab be
added to carboplatin and pemetrexed? What about
those older than 75 years of age (who were excluded
from Zalcman and colleagues study)? Where does
pemetrexed maintenance t into this paradigm? In view
of the previous negative trial of bevacizumab added to
cisplatin and gemcitabine,12 are these results specic to
the combination of pemetrexed and bevacizumab?
Denitive answers to all of these questions will probably
never be obtained. Even if patients and resources were
www.thelancet.com Vol 387 April 2, 2016
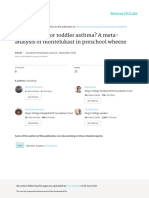
Du Cane Medical Imaging Ltd/Science Photo Library
Comment
Coloured CT scan showing pleural mesothelioma (dark red, lower right)
more abundant than at present, we must not spend
time and eort on questions of modest eect. Rather, we
need to refocus our eorts on opportunities not only to
shift the survival curve, but also to raise it, by aiming to
cure more patients.13 We should continue to forge ahead
with development and study of new drugs with strong
biological rationale and assess them in new clinical trial
designs that optimise the ability to rapidly advance care,
enrol patients, and answer valuable questions.
One way to iterate advances more rapidly than at
present is to break free from the construct of studying
a promising new drug, with cisplatin and pemetrexed,
versus cisplatin and pemetrexed. Use of new drugs
upfront, either alone or with other new drugs, could
allow identication of promising treatments with
accompanying biomarkers more quickly than at
present, and thereby translate ndings rapidly into
meaningful change for patients. While such work
continues, those patients with pleural mesothelioma
who are not candidates for clinical trials or who do not
have access to such opportunities, but who do not have
contraindications to bevacizumab, should be oered
three-drug treatment as a new standard of care.
Marjorie G Zauderer
Department of Medicine, Division of Solid Tumor Oncology,
Thoracic Oncology Service, Memorial Sloan Kettering Cancer Center
and Weill Cornell Medical College, New York, NY 10065, USA
zauderem@mskcc.org
I have received research funding from Verastem, Sellas Life Sciences, and
MedImmune.
1353
Comment
3
4
5
Vogelzang NJ, Rusthoven JJ, Symanowski J, et al. Phase III study of
pemetrexed in combination with cisplatin versus cisplatin alone in
patients with malignant pleural mesothelioma. J Clin Oncol 2003;
21: 263644.
Ladanyi M, Zauderer MG, Krug LM, et al. New strategies in pleural
mesothelioma: BAP1 and NF2 as novel targets for therapeutic
development and risk assessment. Clin Cancer Res 2012; 18: 448590.
Pastan I, Hassan R. Discovery of mesothelin and exploiting it as a target for
immunotherapy. Cancer Res 2014; 74: 290712.
Stahel RA, Weder W, Felley-Bosco E, et al. Searching for targets for the
systemic therapy of mesothelioma. Ann Oncol 2015; 26: 164960.
Ohta Y, Shridhar V, Bright RK, et al. VEGF and VEGF type C play an
important role in angiogenesis and lymphangiogenesis in human
malignant mesothelioma tumours. Br J Cancer 1999; 81: 5461.
Strizzi L, Catalano A, Vianale G, et al. Vascular endothelial growth factor is
an autocrine growth factor in human malignant mesothelioma.
J Pathol 2001; 193: 46875.
Buikhuisen WA, Burgers JA, Vincent AD, et al. Thalidomide versus active
supportive care for maintenance in patients with malignant mesothelioma
after rst-line chemotherapy (NVALT 5): an open-label, multicentre,
randomised phase 3 study. Lancet Oncol 2013; 14: 54351.
10
11
12
13
Dubey S, Janne PA, Krug L, et al. A phase II study of sorafenib in malignant
mesothelioma: results of Cancer and Leukemia Group B 30307.
J Thorac Oncol 2010; 5: 165561.
Jahan T, Gu L, Kratzke R, et al. Vatalanib in malignant mesothelioma:
a phase II trial by the Cancer and Leukemia Group B (CALGB 30107).
Lung Cancer 2012; 76: 39396.
Nowak AK, Millward MJ, Creaney J, et al. A phase II study of intermittent
sunitinib malate as second-line therapy in progressive malignant pleural
mesothelioma. J Thorac Oncol 2012; 7: 144956.
Zalcman G, Mazieres J, Margery J, et al, on behalf of the French Cooperative
Thoracic Intergroup (IFCT). Bevacizumab for newly diagnosed pleural
mesothelioma in the Mesothelioma Avastin Cisplatin Pemetrexed Study
(MAPS): a randomised, controlled, open-label, phase 3 trial. Lancet 2015;
published online Dec 21. http://dx.doi.org/10.1016/S0140-6736(15)01238-6.
Kindler HL, Karrison TG, Gandara DR, et al. Multicenter, double-blind,
placebo-controlled, randomized phase II trial of gemcitabine/cisplatin plus
bevacizumab or placebo in patients with malignant mesothelioma.
J Clin Oncol 2012; 30: 250915.
Hellmann MD, Kris MG, Rudin CM. Medians and milestones in describing
the path to cancer cures: telling tails. JAMA Oncol 2015; published online
Nov 19. DOI:10.1001/jamaoncol.2015.4345.
Large-scale screening for somatic mutations in lung cancer
Published Online
January 14, 2016
http://dx.doi.org/10.1016/
S0140-6736(15)01125-3
See Articles page 1415
1354
Lung cancer is the leading cause of cancer-related death
worldwide. More than 85% of cases are classied as nonsmall-cell lung cancer (NSCLC), with predicted 5-year
survival of 16%. However, technological advances in
the past decade, including the introduction of nextgeneration sequencing, have allowed for identication
of several genetic mutations.1 These mutations are
considered to be actionable oncogenic drivers (ie,
treatable with specic drugs) since they cause specic
subclasses of NSCLC, and therefore can be targeted with
selective inhibitors. One example is NSCLC harbouring
mutations in the epidermal growth factor receptor (EGFR)
gene, mainly associated with lung adenocarcinoma. In
view of these advances, chemotherapy can no longer be
regarded as the standard treatment for all patients, but
rather the default treatment for those without oncogenic
driver mutations.2 In an unprecedented endeavour
reported in The Lancet, the French National Cancer
Institute (INCa), together with the French Cooperative
Thoracic Intergroup (IFCT), have reported on a 1-year
nationwide programme assessing testing for EGFR,
HER2 (also known as ERBB2), KRAS, BRAF, and PIK3CA
mutations, as well as ALK rearrangements in NSCLC,
with the aim of selecting genotype-directed therapy and
studying associations with survival.3 This work, by Fabrice
Barlesi and colleagues, builds on earlier studies which
established actionable oncogenic mutations in NSCLC.
EGFR mutations were identied in 17% of 2105 patient
samples screened in a Spanish Lung Cancer Group central
laboratory from 129 institutions in Spain. In this study,
overall survival for 217 patients who received erlotinib (a
tyrosine kinase inhibitor) was 27 months.4 EGFR inhibition
leads to the collapse of downstream signalling pathways
such as mitogen-activated protein kinase (MAPK) and
AKT protein kinase (gure). Other actionable oncogenic
mutations have been reported in lung adenocarcinoma,
including HER2, MET, and RIT1, and fusion oncogenes
involving ALK, ROS1, NRG1, NTRK1, and RET. Screening
should also be performed for KRAS and BRAF mutations
before selecting treatment1,58 (gure). In squamous-cell
carcinoma and small-cell lung carcinomas, several novel
driver mutations are being investigated as potentially
actionable targets: amplication of FGFR1, PIK3CA,9 and
the sequence of the entire 32 kb coding region of DDR2.5,10
DDR2 mutations can be detected at a frequency of 3% in
both adenocarcinoma and squamous-cell carcinoma.11
On the basis of this knowledge, new initiatives for
treatment of lung squamous-cell carcinoma are in
progress, such as the Lung Cancer Master Protocol (LungMAP), a unique publicprivate partnership in the USA,
including the US Food and Drug Administration.12 The
Network Genomic Medicine (NGM) in Cologne, Germany,
was the rst group to describe distribution of genotypes
and survival with targeted therapy compared with
chemotherapy in distinct genotypes.10 Since then, the
NGM has made great progress, implementing genotyping
by next-generation sequencing as well as other initiatives
in implementing genomic-driven treatment trials, such
www.thelancet.com Vol 387 April 2, 2016
You might also like
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (890)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Maternity and Pediatric Nursing 3rd EditionDocument347 pagesMaternity and Pediatric Nursing 3rd EditionTaylor Talley80% (15)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Absorption and Fluoresence Spectra of Methyl Salicylate in The Vapor PhaseDocument7 pagesAbsorption and Fluoresence Spectra of Methyl Salicylate in The Vapor PhaseAriNo ratings yet
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- 803 Service ManualDocument196 pages803 Service Manualвася рогов100% (1)
- ISA CCST Task List Reference GuideDocument13 pagesISA CCST Task List Reference GuideNaseer HydenNo ratings yet
- Essential Oils in The Treatment of Respiratory Tract Diseases Highlighting Their Role in Bacterial Infections and Their Anti-Inflammatory Action: A ReviewDocument11 pagesEssential Oils in The Treatment of Respiratory Tract Diseases Highlighting Their Role in Bacterial Infections and Their Anti-Inflammatory Action: A ReviewAri100% (2)
- Case Study - BronchopneumoniaDocument45 pagesCase Study - Bronchopneumoniazeverino castillo91% (33)
- Before The Honourable Supreme Court of India: Memorandum On Behalf of PetitonersDocument31 pagesBefore The Honourable Supreme Court of India: Memorandum On Behalf of Petitonerspalkin50% (2)
- Concept of Health and IllnessDocument24 pagesConcept of Health and IllnessHydra Olivar - Pantilgan100% (1)
- DodompemperidoneDocument8 pagesDodompemperidonetiwNo ratings yet
- Clinical Effectiveness and Safety of Montelukast in AsthmaDocument12 pagesClinical Effectiveness and Safety of Montelukast in AsthmaAriNo ratings yet
- Depression in Amyotrophic Lateral SclerosisDocument8 pagesDepression in Amyotrophic Lateral SclerosisAriNo ratings yet
- Inhaled Salbutamol Plus Ipratropium in Moderate and Severe AsthmaDocument6 pagesInhaled Salbutamol Plus Ipratropium in Moderate and Severe AsthmaAriNo ratings yet
- New Efficacy of LTRAs (Montelukast Sodium)Document3 pagesNew Efficacy of LTRAs (Montelukast Sodium)AriNo ratings yet
- Meta-Analysis of The Efficacy of A Single Dose of Phenylephrine 10mg Compared With Placebo in Adults With Acute Nasal Congestion Due To The Common ColdDocument14 pagesMeta-Analysis of The Efficacy of A Single Dose of Phenylephrine 10mg Compared With Placebo in Adults With Acute Nasal Congestion Due To The Common ColdAriNo ratings yet
- Daftar Isi PulmoDocument5 pagesDaftar Isi PulmoAriNo ratings yet
- Chronic Diarrhea Diagnosis and ManagementDocument15 pagesChronic Diarrhea Diagnosis and ManagementNicolas BustamanteNo ratings yet
- Sensitization Predicts Asthma Development Among Wheezing Toddlers in Secondary HealthcareDocument8 pagesSensitization Predicts Asthma Development Among Wheezing Toddlers in Secondary HealthcareAriNo ratings yet
- Safety and Efficacy of Phenylephrine Nasal Drops in BronchiolitisDocument5 pagesSafety and Efficacy of Phenylephrine Nasal Drops in BronchiolitisAriNo ratings yet
- Anemia: Dr. Saranya VinothDocument45 pagesAnemia: Dr. Saranya Vinothareeb khanNo ratings yet
- Design Development and Evaluation of Oral Thin Films of Montelukast SodiumDocument14 pagesDesign Development and Evaluation of Oral Thin Films of Montelukast SodiumAriNo ratings yet
- JpedsDocument7 pagesJpedsAriNo ratings yet
- Anemia Anak 2: Dr. BerthaDocument35 pagesAnemia Anak 2: Dr. BerthaAriNo ratings yet
- Intermittent Montelukast in Children Aged 10 Months To 5 Years With WheezeDocument8 pagesIntermittent Montelukast in Children Aged 10 Months To 5 Years With WheezeAriNo ratings yet
- Montelukast For Toddler AsthmaDocument8 pagesMontelukast For Toddler AsthmaAriNo ratings yet
- Are One or Two Dangerous? Methyl Salicylate ExposureDocument7 pagesAre One or Two Dangerous? Methyl Salicylate ExposureAriNo ratings yet
- Evaluation of Step-Down Therapy From An Inhaled Steroid To Montelukast in Childhood AsthmaDocument7 pagesEvaluation of Step-Down Therapy From An Inhaled Steroid To Montelukast in Childhood AsthmaAriNo ratings yet
- Camphor: Risks and Benefits of A Widely Used Natural ProductDocument6 pagesCamphor: Risks and Benefits of A Widely Used Natural ProductAriNo ratings yet
- Cold and Flu: Conventional Vs Botanical & Nutritional Therapy PDFDocument14 pagesCold and Flu: Conventional Vs Botanical & Nutritional Therapy PDFAriNo ratings yet
- Bmri2014 606021Document11 pagesBmri2014 606021AriNo ratings yet
- 1 s2.0 S2221169115001033 Main PDFDocument11 pages1 s2.0 S2221169115001033 Main PDFxiuhtlaltzinNo ratings yet
- AromaSciCh07 2Document18 pagesAromaSciCh07 2Ánh Nguyễn ThịNo ratings yet
- Pharmacologic Agents For Chronic DiarrheaDocument7 pagesPharmacologic Agents For Chronic DiarrheaAriNo ratings yet
- Cholestyramine Therapy For Intractable DiarrheaDocument6 pagesCholestyramine Therapy For Intractable DiarrheaAriNo ratings yet
- Use of Oral Gentamicin, Metronidazole, and Cholestyramine in The Treatment of Severe Persistent Diarrhea in InfantsDocument7 pagesUse of Oral Gentamicin, Metronidazole, and Cholestyramine in The Treatment of Severe Persistent Diarrhea in InfantsAriNo ratings yet
- A Comparative Trial of Cholestyramine and Loperamide For Acute Diarrhoea in Infants Treated As OutpatientsDocument114 pagesA Comparative Trial of Cholestyramine and Loperamide For Acute Diarrhoea in Infants Treated As OutpatientsAriNo ratings yet
- Multiple Bank Accounts Registration FormDocument2 pagesMultiple Bank Accounts Registration FormAjith JainNo ratings yet
- wk4 Stdconferencereflection ElmoreajaDocument4 pageswk4 Stdconferencereflection Elmoreajaapi-316378224No ratings yet
- Idioma Extranjero I R5Document4 pagesIdioma Extranjero I R5EDWARD ASAEL SANTIAGO BENITEZNo ratings yet
- Chapter 2 ManojDocument4 pagesChapter 2 ManojBro FistoNo ratings yet
- Badhabits 2022Document53 pagesBadhabits 2022Sajad KhaldounNo ratings yet
- Final Final PosterDocument1 pageFinal Final Posterapi-486056653No ratings yet
- Dasar Genetik GandumDocument282 pagesDasar Genetik GandumAlekkyNo ratings yet
- Report On Baby Food Industry in BangladeshDocument5 pagesReport On Baby Food Industry in BangladeshIffatur RahmanNo ratings yet
- English Dept Guidebook: Grammar & Exercises for Level 4Document57 pagesEnglish Dept Guidebook: Grammar & Exercises for Level 4KIngLyonLuis100% (1)
- Practical Laser Diodes GuideDocument4 pagesPractical Laser Diodes GuideM Xubair Yousaf XaiNo ratings yet
- The Evolution of FungiDocument15 pagesThe Evolution of Fungi2010eon2010No ratings yet
- HVDCProjectsListingMarch2012 ExistingDocument2 pagesHVDCProjectsListingMarch2012 ExistingHARLEY SANDERSNo ratings yet
- Installation and Operating Instructions DPV and DPLHS PumpsDocument36 pagesInstallation and Operating Instructions DPV and DPLHS PumpsSergeyNo ratings yet
- Effective Determinantsof Consumer Buying Decisionon OTCDocument13 pagesEffective Determinantsof Consumer Buying Decisionon OTCThinh PhamNo ratings yet
- MBBS Final Part-I (Winter Session) Time Table (Jan 2023)Document1 pageMBBS Final Part-I (Winter Session) Time Table (Jan 2023)crystal mindNo ratings yet
- B Cell Cytokine SDocument11 pagesB Cell Cytokine Smthorn1348No ratings yet
- CEP Lesson Plan Form: Colorado State University College of Health and Human Sciences Page 1Document13 pagesCEP Lesson Plan Form: Colorado State University College of Health and Human Sciences Page 1Apple AterradoNo ratings yet
- Clarifying Questions on the CPRDocument20 pagesClarifying Questions on the CPRmingulNo ratings yet
- Jose Irizarry ResumeDocument2 pagesJose Irizarry ResumeAnastasia GloverNo ratings yet
- Using Casts For ImmobilizationDocument17 pagesUsing Casts For Immobilizationmpmayer2No ratings yet
- SKY BUILDER SILICON CITY QuotationDocument10 pagesSKY BUILDER SILICON CITY QuotationVikram SolankiNo ratings yet
- Dermato Venerology ScienceDocument11 pagesDermato Venerology ScienceAQis AQishNo ratings yet
- 2 - Electrical Energy Audit PDFDocument10 pages2 - Electrical Energy Audit PDFPrachi BhaveNo ratings yet
- LENZE E84AVxCx - 8400 StateLine-HighLine-TopLine 0.25-45kW - v9-0 - ENDocument291 pagesLENZE E84AVxCx - 8400 StateLine-HighLine-TopLine 0.25-45kW - v9-0 - ENClaudioNo ratings yet