Professional Documents
Culture Documents
M19-RAD Overview of Radiation Oncology Team5
Uploaded by
William PinzonOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
M19-RAD Overview of Radiation Oncology Team5
Uploaded by
William PinzonCopyright:
Available Formats
YL7
I.
II.
III.
IV.
V.
VI.
VII.
VIII.
IX.
X.
XI.
XII.
XIII.
XIV.
I.
II.
ONCOLOGY Module [RADIOLOGY]
8 February 2012
OVERVIEW OF RADATION ONCOLOGY
Dr. Chavez
Outline
Objectives
Cancer incidence
Historical perspective
The discipline of radiology
How does RT work?
Basic radiologic principles
Principles of fractionation
Aims of radiotherapy
When do we give RT?
Types of external beam radiation therapy
Brachytherapy
Process of care
The radiology oncology team
Common radiation side effects
Radiology
Therapeutic
Radiology
General Radiology
Interventional
Radiology
CT scan, UTZ, MRI,
Nuclear Medicine
OBJECTIVES
To understand the principles of radiation therapy
To understand the roles of radiation therapy in cancer
management
To be familiar with the differentiation approaches for dose
delivery
o External beam radiotherapy
o Brachytherapy
o Stereotactic radiation surgery
CANCER INCIDENCE
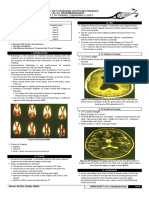
V. HOW DOES RT WORK?
Radiation
Propagation of energy from a radioactive source to another
medium
Ionizing radiation dislodged electrons from atoms
SEE APPENDIX
2nd leading cause of death
Exceeds all other diseases in terms of working life lost
Cancer incidence in 2011
o 10M new cases of cancer per year worldwide
o 1/2 of the cases in developing countries
Cancer incidence in 2015
o 15M cases per year worldwide
o 2/3 of the cases in developing countries
Radiation
DNA
Cellular
Transformation
Emil Grubbe (Jan 29, 1896) used x-rays to treat a 65 year old
female patient named Rosa Lee with recurrent breast
carcinoma
Naturally reactive radium applied where medicine was
deficient
Serious side effects regulated by strict rules and laws
Radiation effective tool for treating cancer for >100 years
More than 60% of cancer patients will receive radiation
therapy as part of their treatment
o > 1 million cancer patients are treated annually with
radiation
IV. THE DISCIPLINE OF RADIOLOGY
Radiation oncology is the clinical and scientific discipline devoted
to:
Treatment of patients with cancer (and other diseases) using
ionizing radiation (alone or in combination with other
modalities)
Investigation of the biologic and physical basis of radiation
therapy
Training of professionals in the field
Group 05
Radiation Oncology
Figure 1. Branches of radiology
III. HISTORICAL PERSPECTIVE
Diagnostic Radiology
Genetic
damage
Mitotic Cell
Death
Malignant
transformation
Cancer
DNA damage
Direct ionization (1%); Direct DNA target
o Single strand repair
o Double strand cell death
Indirect ionization (99%)
o Formation of hydroxy radicals
o Interaction of free radicals with DNA, causing cell death
Agoncillo | Barbon | Cantalejo | Carandang | Chua | Faria | Santos | Ubaldo
Page 1 of 5
OVERVIEW OF RADIATION ONCOLOGY
RADIOLOGY
VI. BASIC RADIOLOGIC PRINCIPLES
Fractionation dividing the total dose into small daily fractions
over several weeks
o Better tumor control than a single large fraction
Experiments performed in paris in the 1920s and 1930s
confirmed this principle
Moderately
sensitive
VII. PRINCIPLES OF FRACTIONATION
Repair
o RT causes lethal damage to tumor cells and sublethal
damage in normal tissues
o Fractionated doses allow normal tissues time to repair
Repopulation
o Regrowth of cells between fractions
o Increases the number of tumor cells to be destroyed ->
against treatment
o Increases the number of normal tissue cells following
irradiation -> in favor of treatment
Redistribution (=reassortment)
o Most sensitive: M and G2
o Most resistant: S phase
o If you give fractionated dose, S phase will move on to
more resistant phases
Less sensitive
Optic lens epithelium
Endothelium
Growing bone and cartilage
Fibroblast
Glial cells
Mammary gland epithelium
Lung epithelium
Renal epithelium
Hepatic epithelium
Pancreas epithelium
Thyroid epithelium
Mature erythrocyte
Muscle cell
Mature connective tissue
Mature bone and cartilage
Ganglion cell
IN SUMMARY
Fractionation spares normal tissue through repair and
repopulation
Fractionation increases damage to tumor cells through
redistribution and reoxygenation
Radionsensitivity: directly proportional to mitosis and inversely
proportional to differentiation
VIII. AIMS OF RADIOTHERAPY
Aim of Radiotherapy
To kill all viable cancer cells
To deliver as much dose as possible to the target while
minimizing the dose to surrounding healthy tissues
High quality of life and prolongation of survival
Competitive cost
Prior to RT:
What is the stage?
What is our goal?
Reoxygenation
o Hypoxic cells: 2-3x more resistant to radiation (-> oxygen is
required for the indirect effect to occur)
o Oxygen supply constant; hypoxic cells gradually obtain
much better vascularity and oxygenation
o Increase radiosensitivity
Radiosensitivity
o Law of Bergonie and Tribendau (1907)
o Radiosensitivity is highest in the tissues with highest
mitotic index and lowest in differentiated tissues
o MOST sensitive more immature, higher mitotic index,
less differentiated (i.e., spermatogonia)
o LESS sensitive low mitotic indices (i.e., mature
erythrocytes)
Most sensitive
Sensitive
Group 05
Lymphocyte
Immature hematopoietic cells
Intestinal epithelium
Spermatogonia
Ovarian follicle cells
Bladder epithelium
Esophagus epithelium
Gastric mucosa
Epidermal epithelium
Dose Should be Accurate
To target:
o 5% too low may result in clinically detectable reduction in
tumor control (eg. Head and neck cancer: 15%)
To normal tissues:
o 5% too high significant increase in normal tissue
complication probability = morbidity = unacceptable side
effects
Prerequisites to RT Stage!
History and PE
Diagnostic test results
o Laboratory
o Imaging
Histopathologic confirmation
Operative record
Chemotherapeutic record
Goals of Radiation Therapy
Curative
o Early stage disease
High dose to tumor
o Good tumor control
Agoncillo | Barbon | Cantalejo | Carandang | Chua | Farias | Santos | Ubaldo
Page 2 of 5
OVERVIEW OF RADIATION ONCOLOGY
Low dose to normal tissues
o Minimal complication
Palliative
Late stage disease
Adequate dose to region involved
o Maximum relief of symptoms
Alleviate pain
Restoration of luminal patency
Preservation of skeletal integrity
Organ function re-establishment
o Minimum complication
Prophylactic
o Prevention of possible metastases or recurrences
Total body irradiation
o Ablation of bone marrow in order to suppress the immune
system, eradicate leukemic cells, and clear space for
transplant cells during bone marrow transplantation
conditioning
IX. WHEN DO WE GIVE RT?
Radiotherapy types according to timing:
Adjuvant radiotherapy given after any kind of treatment
modality
o If given after surgery -> postoperative RT
Neoadjuvant radiotherapy given before any kind of
treatment modality
o If given before surgery -> preoperative RT
Radiochemotherapy (chemoradiotherapy) given concurrently
with chemotherapy
Pre-op RTx
To render the tumor operable
To make the operation less extensive
To decrease potential dissemination
Disadvantage
o Interfere with normal tissue healing
Post-op RTx
(+) surgical margins eradicate subclinical/microscopic disease
Inadequate surgery
o Total vs radical
(+) lymph nodes sterilize ln mets
Delivery of radiation therapy
The type of treatment used will depend on the location, size
and type of cancer
Radiation therapy can be delivered in 2 ways
o External beam radiotherapy or teletherapy
Applied to the body externally using a treatment
machine
o Brachytherapy
Brachy = Short distance
Also known as Endocurietherapy/sealed-source
radiotherapy
Performed by placing temporary or permanent
radiation sources into body
Cavities or directly into the tumor
Group 05
RADIOLOGY
X.
TYPES OF EXTERNAL BEAM RADIATION THERAPY
1. Conventional Radiation Therapy (CRT)
o Uses 2D imaging for simulation; single beam of RT
delivered to the patient from several directions
2. Three-dimensional Conformal Radiation Therapy (3D-CRT)
o Dose volume conforms closely to the target through the
use of 3D anatomical data from CT or MRI
Apply max dose to target while sparing normal
neighboring structures
3. Intensity modulated radiation therapy (IMRT)
o Sophisticated form of 3D-CRT
o Non-uniform beam intensities, beamlets, the intensity of
each beam can be adjusted individually
o Compared to 3D-CRT wherein energy is uniform, each
beamlet can be modified
4. Image-guided radiotherapy (IGRT)
o Integration of various radiological and functional imaging
techniques
o Main aims to reduce setup and internal margins, to
account for target volume changes during treatment
(tumor volume decrease, weight loss)
o Difference between IMRT: IGRT has a built-in imaging
modality! You can look at the exact tumor
configuration during treatment
5. Stereotactic Radiotherapy (SRT)
o It is important to immobilize the patient here because of
very high ablative doses; must target tumor precisely
o Delivered by several beams that are precisely focused on
3d localized target
o If given in one-five fractions in ablative doses -> sterotactic
radiosurgery (SRS)
o If given in more than five fraction -> SRT
o Indications for SRS/SRT
Boost/adjunctive therapy
o Residual tumors after surgery
o Augment conventional radiotherapy
Salvage therapy
o Inoperable benign or malignant tumors with
previous irradiation
Benign non-invasive tumors of the brain
o Pituitary adenoma
o Acoustic neuroma
Brain metastasis
Av malformation
6. Particle therapy
o Proton beam therapy
Uses protons rather than x-rays to treat cancer
Radiation dose at a certain depth within the body ->
spares nearby normal tissue
o Neutron beam therapy
Specialized form of radiation therapy used to treat
certain tumors that are very difficult to manage using
conventional radiation therapy
Neutrons have a greater biologic impact on the tumor
than a similar dose of conventional radiation therapy
*Available in a few locations in the US and Japan
Agoncillo | Barbon | Cantalejo | Carandang | Chua | Farias | Santos | Ubaldo
Page 3 of 5
OVERVIEW OF RADIATION ONCOLOGY
XI. BRACHYTHERAPY
Radioactive sources are implanted into the tumor or
surrounding tissue
o brachy is greek for short distance
Purpose is to deliver high doses of radiation to the desired
target whie minimizing the dose to surrounding normal tissue
Indications for Brachytherapy
Definitive treatment (prostate, gyne)
Boost/adjunctive therapy
o Augment conventional radiotherapy (prostate, gyne)
o Residual tumors after surgery (oral cavity, breast)
Salvage therapy
o Residual tumors after previous irradiation wit/out
chemotherapy (np, head and neck)
Palliation
Types of Brachytherapy
Intracavity implants
o Radioactive sources are placed near the tumor through the
body cavities (cervix, trachea, nasal cavity)
Interstitial implants
o Sources placed directly into the tissue (prostate, oral cavity,
breast)
Intraoperative implants
o Surface applicator is in direct contact with the surgical
tumor bed (soft tissue sarcoma)
Procedures often require anesthesia and brief
hospitalization
Radiation delivered to the site through specially
designed applicators or catheters
Dose Rate for Brachytherapy
Low dose rate (ldr): 0.4 to 2 gy/hr
o Radiation delivered over the course of 48 to 120 hours
Gynecologic, head and neck, and prostate cancers may
be treated with low dose rate brachytherapy
Medium dose rate: 2 to 12 gy/hr
High dose rate (hdr): >12 gy/hr usually in the region of 150
gy/hr
o High energy source delivers the dose in a matter of minutes
rather than days
Gynecologic, breast, oral cavity, and some prostate
implants may use high dose rate brachytherapy
XII. THE RADIATION ONCOLOGY TEAM
1. Radiation oncologist
The doctor who prescribed and oversees the radiation therapy
treatments
2. Medical radiation physicist
Ensures the treatment plans are properly tailored for each
patient, and is responsible for the calibration and accuracy of
treatment equipment
3. Dosimetrist
Works with the radiation oncologist and medical physicist to
calculate the proper dose of radiation given to the tumor
4. Radiation therapist
Administers daily radiation under the doctors prescription and
supervision
5. Radiation oncology nurse
Group 05
RADIOLOGY
Interacts with the patient and family at the time of
consultation, throught the treatment process and during
follow up care
All have different roles. Effective communication is essential for
optimized treatment outcome.
Factors to Consider
Aim: Palliation vs care
RTcenter: Equipment, experience, cost, geography
Tumor: Stage, histology, location, radiosensitivity, previous
treatments
Patient: Age, performance, morbidity, cosmesis, patient
preference
XIII. PROCESS OF CARE
1. Simulation
Immobilization: imaging, tumor localization, blocking making
provides a blueprint for treatment
o Most common immobilization device: Thermoplastic
mask for head and neck tumors
o Also assures daily reproducibility of treatment
2. Process of care: treatment planning
Sophisticated software is used to carefully derive an
appropriate treatment plan for each patient
Computerized algorithms enable the treatment plan to spare
as much healthy tissue as possible
3. Set-up and treatment
Port films are used to check if treated fields are exactly the
same as the planned ones
Regularly taken during the therapy when the patient is on the
treatment couch and compared with the simulation films
4. Regular check-ups
Progress of treatment
Identify and treat possible side effects
Side effects are limited to the area treated and usually resolve
2-6 weeks post-radiation
Unlike the systemic side effects from chemotherapy, radiation
therapy usually only impacts the area that received radiation
5. Quality assurance
QA includes all aspects of the therapy
A problem at any stage of this overall procedures affects all
functions
Control mechanisms should be standardized and continuously
monitored if they are to be successful
XIV. COMMON RADIATION SIDE EFFECTS
Breast swelling, skin irritation
Abdomen nausea, vomiting, diarrhea
Chest cough, shortness of breath, pneumonitis, esophagitis
Head and neck taste alterations, dry mouth, mucositis, skin
irritation, hoarseness
Brain hair fall/loss, scalp irritation
Pelvis diarrhea, cramping, urinary frequency, vaginal
irritation
Fatigue is often seen when large areas are irradiated
o Breast, abdomen, pelvis, whole brain
Agoncillo | Barbon | Cantalejo | Carandang | Chua | Farias | Santos | Ubaldo
Page 4 of 5
OVERVIEW OF RADIATION ONCOLOGY
RADIOLOGY
Is radiation therapy safe?
Radiation has been safely used for cancer treatments for more
than a century
Many advances have been made to ensure it remains safe and
effective
The treatment plan is constantly checked and updated to
ensure proper treatment is being given
Equipment is routinely examined to make sure it is only giving
the dose of radiation prescribed
Radiation can sometimes cause secondary cancers many years
later. This risk is usually offset by the need to cure the patient
today.
Patients who receive external radiation are not radioactive.
Healthcare workers only need to take special precaution when
treating patients receiving some types of brachytherapy
XV. SUMMARY
Radiotherapy is a well established modality for the treatment
of numerous malignancies
o Most common: head and neck, breast, lung, prostate,
cervix, endometrial, colorectal
Treatment is safe, quick and painless with tolerable short term
side effects.
o Morbidity localized to area irradiated
Radiated oncologists are specialists trained to treat cancer with
a variety of forms of radiation
o External beams, brachytherapy, stereotactic
XVI. APPENDIX
Breakdown of Ionizing Radiation
Ionizing
radiation
Electromangetic
X -ays
Group 05
Gamma rays
Particulate
Alpha particles
Electron
particles
Agoncillo | Barbon | Cantalejo | Carandang | Chua | Farias | Santos | Ubaldo
Neutron proton
Messon heavy
ions
Page 5 of 5
You might also like
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- (RADIO 250) LEC 03 Genitourinary and KUB ImagingDocument7 pages(RADIO 250) LEC 03 Genitourinary and KUB ImagingWilliam PinzonNo ratings yet
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- (RADIO 250) LEC 09 NeuroradiologyDocument3 pages(RADIO 250) LEC 09 NeuroradiologyWilliam PinzonNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- (RADIO 250) LEC 06 Chest RadiologyDocument10 pages(RADIO 250) LEC 06 Chest Radiologyjmhinos4833No ratings yet
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- (RADIO 250) LEC 01 Introduction To Radiology + Radioprotection PDFDocument4 pages(RADIO 250) LEC 01 Introduction To Radiology + Radioprotection PDFjmhinos4833No ratings yet
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- (RADIO 250) LEC 08 Introduction To Interventional RadiologyDocument4 pages(RADIO 250) LEC 08 Introduction To Interventional RadiologyWilliam PinzonNo ratings yet
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- (RADIO 250) LEC 10 Radiation OncologyDocument3 pages(RADIO 250) LEC 10 Radiation OncologyWilliam PinzonNo ratings yet
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- (RADIO 250) LEC 12 Abdominal RadiologyDocument8 pages(RADIO 250) LEC 12 Abdominal RadiologyWilliam PinzonNo ratings yet
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- (RADIO 250) LEC 07 Musculoskeletal RadiologyDocument11 pages(RADIO 250) LEC 07 Musculoskeletal RadiologyWilliam PinzonNo ratings yet
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- Radio Onco Tranx - 1Document8 pagesRadio Onco Tranx - 1William PinzonNo ratings yet
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- (RADIO 250) LEC 11 Nuclear MedicineDocument7 pages(RADIO 250) LEC 11 Nuclear MedicineWilliam Pinzon100% (1)
- MCQs in Plastic SurgeryDocument308 pagesMCQs in Plastic SurgeryVitowanu-Adesanya Blessing100% (5)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- ACLS 2013 Pocket Brain Book 5thDocument85 pagesACLS 2013 Pocket Brain Book 5thWilliam PinzonNo ratings yet
- Clinical Oncology - Previous Examination Papers 2011Document12 pagesClinical Oncology - Previous Examination Papers 2011wipi112No ratings yet
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- Chan 2016Document8 pagesChan 2016Samuel MonsalveNo ratings yet
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- SBRT Vs SurgeryDocument7 pagesSBRT Vs SurgerySandra SkaržinskaitėNo ratings yet
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Prushield Ebrochure English PDFDocument20 pagesPrushield Ebrochure English PDFIts My PlaceNo ratings yet
- Protocol Rtog 1119 1Document18 pagesProtocol Rtog 1119 1api-540888060No ratings yet
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Linear Accelerator Acceptance Testing and CommissioningDocument17 pagesLinear Accelerator Acceptance Testing and CommissioningSaamyNo ratings yet
- Chapter 07 Treatment PlanningDocument232 pagesChapter 07 Treatment PlanningAhmed Ridwan OladotunNo ratings yet
- 2014CVss NovDocument17 pages2014CVss Novshankar sivaNo ratings yet
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Design & Delivery of Automated Winston-Lutz Test For Isocentric &Document66 pagesDesign & Delivery of Automated Winston-Lutz Test For Isocentric &Harpreet sainiNo ratings yet
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- Understanding The Role of Global Operations in The Modern MarketplaceDocument6 pagesUnderstanding The Role of Global Operations in The Modern Marketplacealizasajid50No ratings yet
- 2013 Radiation Oncology Accessories CatalogDocument112 pages2013 Radiation Oncology Accessories CatalogJelicaMilutinovicNo ratings yet
- The Role of Hypofractionated Radiotherapy in ProstDocument10 pagesThe Role of Hypofractionated Radiotherapy in ProstАнастасия АнохинаNo ratings yet
- Chapter 07 Treatment PlanningDocument232 pagesChapter 07 Treatment PlanningsamNo ratings yet
- 2020-Thesis-Calculation LET and RBE FLUKA and EclipseDocument95 pages2020-Thesis-Calculation LET and RBE FLUKA and Eclipsebo zhaoNo ratings yet
- Handbook of Evidence Based Stereotactic Radiosurgery and StereotacticDocument303 pagesHandbook of Evidence Based Stereotactic Radiosurgery and Stereotacticyves2022sahaNo ratings yet
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- Radiology: Tadio Physics & Nuclear MedicimDocument33 pagesRadiology: Tadio Physics & Nuclear Medicimsk100% (1)
- Characteristics and Limitations of A Secondary Dose Check Software For VMAT Plan CalculationDocument8 pagesCharacteristics and Limitations of A Secondary Dose Check Software For VMAT Plan Calculationkaren CarrilloNo ratings yet
- Moderate and Extreme HypofractionationDocument32 pagesModerate and Extreme HypofractionationsamuelfsjNo ratings yet
- Ebook Schmidek and Sweet Operative Neurosurgical Techniques 7Th Edition Volume 1 PDF Full Chapter PDFDocument67 pagesEbook Schmidek and Sweet Operative Neurosurgical Techniques 7Th Edition Volume 1 PDF Full Chapter PDFwilliam.balasco829100% (20)
- Non-Invasive Ablation of Cardiac ArrhythmiaDocument2 pagesNon-Invasive Ablation of Cardiac ArrhythmiaPatrick Maguire100% (1)
- AVM Pediatric LilleDocument9 pagesAVM Pediatric LilleZdravko HeinrichNo ratings yet
- Interview Assignment - Writing in Biological SciencesDocument5 pagesInterview Assignment - Writing in Biological Sciencesapi-708250948No ratings yet
- Basics of Radiation Therapy: Ryan K. Funk,, Abigail L. Stockham,, Nadia N. Issa LaackDocument22 pagesBasics of Radiation Therapy: Ryan K. Funk,, Abigail L. Stockham,, Nadia N. Issa LaackAlejo RLNo ratings yet
- NUCLEAR 101 Topic 07 BookletDocument34 pagesNUCLEAR 101 Topic 07 BookletMichelle ArispeNo ratings yet
- 1 5114380527033385003Document10 pages1 5114380527033385003Joao LuisNo ratings yet
- 01 Materi 1Document98 pages01 Materi 1levina almiraNo ratings yet
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Does Proton Therapy HaveDocument14 pagesDoes Proton Therapy HaveRaul Matute MartinNo ratings yet
- NRG SBRT Physics Nov2016Document19 pagesNRG SBRT Physics Nov2016arifpharmjuNo ratings yet
- World Journal of Surgical OncologyDocument6 pagesWorld Journal of Surgical OncologyMusthafa Afif WardhanaNo ratings yet
- Chordoma of The Corpus Callosum: Case Report: Literature SearchDocument7 pagesChordoma of The Corpus Callosum: Case Report: Literature SearchAleksandar DimovskiNo ratings yet
- Safety Is No AccidentDocument57 pagesSafety Is No AccidentPrathameshNo ratings yet