Professional Documents
Culture Documents
Overview of The Hereditary Ataxias PDF
Uploaded by
dupuytrenOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Overview of The Hereditary Ataxias PDF
Uploaded by
dupuytrenCopyright:
Available Formats
Overview of the hereditary ataxias
1 sur 19
http://www.uptodate.com/contents/overview-of-the-hereditary-ataxias?to...
Official reprint from UpToDate
www.uptodate.com 2016 UpToDate
Overview of the hereditary ataxias
Authors
Puneet Opal, MD, PhD
Huda Y Zoghbi, MD
Section Editors
Marc C Patterson, MD, FRACP
Helen V Firth, DM, FRCP, DCH
Deputy Editor
John F Dashe, MD, PhD
All topics are updated as new evidence becomes available and our peer review process is complete.
Literature review current through: Dec 2015. | This topic last updated: Mar 09, 2015.
INTRODUCTION AND CLASSIFICATION The hereditary ataxias are a genetically heterogeneous group of diseases
that may be difficult to distinguish clinically because they are all characterized by motor incoordination resulting from
dysfunction of the cerebellum and its connections [1]. With the identification of the gene defects in many of these
disorders, the diagnosis now is made more often by genetic testing.
The hereditary ataxias have traditionally been divided into two main classes:
Ataxia caused by underlying inborn errors of metabolism; these disorders usually are inherited in an autosomal
recessive manner and typically present in childhood.
Progressive degenerative ataxias not due to inborn errors of metabolism. This group of disorders, which are more
common, are divided by their mode of inheritance into autosomal dominant, autosomal recessive, X-linked, and
mitochondrial forms.
The hereditary ataxias caused by inborn errors of metabolism and the episodic, X-linked, and mitochondrial ataxias are
discussed in this topic.
The National Ataxia Foundation (www.ataxia.org), the Friedreich Ataxia Research Alliance (www.curefa.org), and other
nonprofit organizations provide important information for patients and the larger public.
AUTOSOMAL DOMINANT ATAXIAS The most common autosomal dominant ataxias are the spinocerebellar
ataxias. Other causes include dentatorubral-pallidoluysian atrophy (DRPLA), which is common in Japan, and the ataxic
variant of the Gerstmann-Strussler-Scheinker syndrome, a prion disease. These disorders are briefly reviewed here,
and discussed in detail separately. (See "The spinocerebellar ataxias".)
More than 20 types of spinocerebellar ataxia (and the number probably will continue to grow) with characteristic clinical
and genetic abnormalities have been identified. Rather than representing an enzyme deficiency, some of these
disorders are caused by trinucleotide (or, in SCA10, pentanucleotide) repeat expansion within the disease-causing gene
(table 1).
The most common are CAG repeats in the coding region that encode for polyglutamine tracts in the protein products,
similar to that seen in Huntington disease. Expansion of CAG repeats is thought to produce a toxic "gain of function" (ie,
disease develops because the mutant form of the protein gains a new function, not because the protein loses its normal
function). The repeats show both somatic and germline instability. As a result, successive generations of affected
families experience anticipation, a phenomenon characterized by earlier onset and a progressively worse phenotype in
subsequent generations.
AUTOSOMAL RECESSIVE ATAXIAS The most common autosomal recessive ataxias are Friedreich ataxia and
ataxia-telangiectasia. These are discussed separately. (See "Friedreich ataxia" and "Ataxia-telangiectasia".)
Less frequent causes are xeroderma pigmentosum and Cockayne syndrome which, like ataxia-telangiectasia, are
caused by defects in DNA repair mechanisms. (See "Hereditary neuropathies associated with generalized disorders",
section on 'DNA repair disorders'.)
All of these disorders at some point have prominent non-neurologic manifestations, but Friedreich ataxia and ataxiatelangiectasia may be confused in the early stages of the disease. Diagnostic criteria have been proposed for ataxia-
06/01/2016 19:50
Overview of the hereditary ataxias
2 sur 19
http://www.uptodate.com/contents/overview-of-the-hereditary-ataxias?to...
telangiectasia (table 2), and the two disorders can be distinguished by genetic testing [2].
As already noted, ataxias due to underlying inborn errors of metabolism usually are inherited in an autosomal recessive
manner. (See 'Ataxias caused by inborn errors of metabolism' below.)
X-LINKED ATAXIAS X-linked progressive ataxias are a heterogeneous group of rare disorders. Some are pure
cerebellar syndromes [3,4], while others encompass additional neurologic abnormalities such as spasticity, deafness,
intellectual disability (mental retardation), or dementia [5-8]. The genetic loci remain unknown in most of these
disorders, with the exception of an early onset X-linked ataxia that is associated with deafness and loss of vision and
links to locus Xq21.2-q24 [7]. Although the X-linked diseases primarily are expressed in males, a small percentage of
females have some symptoms because of skewed inactivation of the X chromosome bearing the normal allele. Other
patients have ataxia combined with systemic abnormalities such as sideroblastic anemia and adrenal insufficiency.
X-linked sideroblastic anemia with ataxia X-linked sideroblastic anemia with ataxia is a recessive disorder
characterized by relatively mild anemia, unresponsiveness to pyridoxine, and nonprogressive cerebellar ataxia [9,10].
(See "Causes of congenital and acquired sideroblastic anemias".)
The molecular defect resides at Xq13 in the ABC7 transporter gene [11,12]. The role of the ABC7 protein, an
ATP-binding cassette transporter, in human erythroid cells is not yet defined. The yeast ortholog of the ABC7 protein is
involved in the generation of cytosolic iron-sulfur cluster-containing proteins [12]. How such a defect might lead to the
phenotype of X-linked sideroblastic anemia with ataxia remains to be determined.
Adrenoleukodystrophy Progressive ataxia and incoordination is an atypical presentation of adrenoleukodystrophy,
an X-linked recessive disorder characterized by progressive neurologic dysfunction and primary adrenal insufficiency.
This disorder is discussed in detail elsewhere. (See "Adrenoleukodystrophy", section on 'Other presentations'.)
MITOCHONDRIAL ATAXIAS Certain mitochondrial disorders can present with a progressive or intermittent ataxia.
Leigh syndrome Leigh syndrome (subacute necrotizing encephalomyelopathy) is an inherited neurodegenerative
disorder of infancy or childhood that is discussed in detail elsewhere. (See "Hereditary neuropathies associated with
generalized disorders", section on 'Leigh syndrome'.)
Summarized briefly, this disorder is characterized by developmental delay or psychomotor regression, signs of
brainstem dysfunction, ataxia, dystonia, external ophthalmoplegia, seizures, lactic acidosis, vomiting, and weakness.
Peripheral neuropathy with reduced nerve conduction velocity and demyelination also are frequent findings. The
prognosis is poor, with survival often being a matter of months after disease onset. Histologic examination reveals
bilateral, symmetric necrotizing lesions in the basal ganglia, thalamus, brainstem, and spinal cord. Magnetic resonance
imaging shows abnormal white matter signal in the putamen, basal ganglia, and brainstem with T2 images.
The Leigh syndrome phenotype appears to be related to altered mitochondrial metabolism. Alterations in the
mitochondrial respiratory chain complex I, pyruvate dehydrogenase complex (PDHC), or in mitochondrial DNA (mtDNA)
have been associated with autosomal, X-linked, or mtDNA mutations (maternally-inherited Leigh syndrome). A
deficiency in cytochrome c oxidase (COX), the fourth multisubunit complex of the respiratory chain, is a common finding
that is inherited as an autosomal recessive trait. Mutations in SURF1, a gene located on chromosome 9q34, have been
identified in many COX deficient patients with Leigh syndrome. (See "Hereditary neuropathies associated with
generalized disorders", section on 'Leigh syndrome'.)
Ataxia and myoclonus Ataxia and myoclonus can be produced by a variety of mitochondrial lesions. They include
large deletions and duplications characteristic of Kearns-Sayre syndrome and maternally-inherited point mutations in
mitochondrial genes encoding tRNA, the MELAS (mitochondrial myopathy, encephalopathy, lactic acidosis, and
stroke-like episodes) and MERRF (myoclonic epilepsy with ragged red fibers) syndromes [13-18]. In MELAS, for
example, the genetic defect alters amino acid incorporation into the subunits of the oxidative phosphorylation system
that are synthesized in the mitochondria, resulting in altered function [13]. In MERRF, on the other hand, an impairment
in mitochondrial calcium homeostasis occurs [17].
ATAXIAS CAUSED BY INBORN ERRORS OF METABOLISM Numerous hereditary ataxias appear to be caused by
06/01/2016 19:50
Overview of the hereditary ataxias
3 sur 19
http://www.uptodate.com/contents/overview-of-the-hereditary-ataxias?to...
inborn errors of metabolism. These ataxias tend to have recessive inheritance, as enzymatic activity of 50 percent in
heterozygotes is sufficient for most metabolic pathways to proceed.
The metabolic pathways involved in these disorders typically have numerous functions. As a result, ataxia is just one
component of the clinical phenotype, which, taken as a whole, often points toward the underlying defect. The clinical
phenotype can be divided into two general groups: the intermittent ataxias that occur with exacerbations of the
underlying biochemical abnormal and the chronic progressive ataxias that are induced by specific enzyme deficiencies
(table 3). A review of the individual disorders is beyond the scope of this discussion.
Intermittent ataxias The most common causes of intermittent ataxias are the aminoacidurias resulting from
mutations in urea cycle enzymes, which lead to hyperammonemia and disorders of pyruvate and lactate metabolism
(table 3). Affected infants with all of these conditions typically display intellectual disability (mental retardation) and
developmental delay. Nevertheless, establishing the correct diagnosis is important because supportive measures differ.
Urea cycle enzyme deficiencies Neonates with urea cycle enzyme deficiencies typically present with acute
neurologic deterioration and hypotonia. Older children may have clumsiness, vomiting, and headaches. In addition,
seizures, involuntary movements, and ptosis can occur at the peaks of hyperammonemia, usually induced by stress or
ingestion of protein. Inheritance of urea cycle deficits is autosomal recessive, with the important exception of the
relatively common ornithine transcarbamylase deficiency, which is X-linked. However, some female carriers with OTC
convert less ammonia nitrogen to urea and are symptomatic [19-21]. (See "Urea cycle disorders: Clinical features and
diagnosis".)
Aminoacidurias Ataxia may be seen in children with aminoaciduria, such as intermittent branched-chain
ketoaciduria and isovaleric acidemia. This ataxic picture often is combined with seizures, episodic vomiting, and
lethargy, similar to that seen in children with urea cycle deficits. The urine usually has a characteristic odor.
Hartnup disease is a pathogenetically different cause of ataxia, resulting from a defect in renal and intestinal transport
of neutral amino acids rather than a metabolic defect. This disorder also is associated with niacin deficiency, often
leading to symptoms of pellagra (such as rash and confusion). Hartnup disease results from mutations in the SLC6A19
gene, which encodes for a sodium-dependent neutral amino acid transporter that is primarily expressed in the kidney
and intestine [22,23].
Disorders of pyruvate and lactate metabolism Pyruvate dehydrogenase (PDH) deficiency, a less common
cause of metabolic intermittent ataxia, is characterized by lactic acidosis, seizures, intellectual disability (mental
retardation), ataxia, and spasticity [24]. This condition typically is caused by a mutation in PDHA1, the gene for the E1
alpha subunit of the PDH enzyme complex (Xp22.2-p22.1) [25]. Other less common genetic defects associated with
PDH deficiency have been reported, including mutations in the E1 beta [26], E2 [27], and E3 [28] subunits, the E3
binding protein [29], and in the PDH phosphatase enzyme that regulates the PDH complex [30].
Biotin-responsive multiple carboxylase deficiency is an autosomal recessive ataxia, characterized by ketoacidosis,
dermatitis, seizures, myoclonus, and nystagmus [31]. The infantile form can be caused by a variety of mutations in the
holocarboxylase synthetase gene at locus 21q22 [31-33]. This enzyme catalyzes the fixation of biotin to inactive
apocarboxylases, producing four active carboxylases (including pyruvate carboxylase). In children with late onset
(usually juvenile) disease, the defect appears to lie in biotinidase, which catalyzes the removal of biotin from the
carboxylases, thereby generating biotin for reutilization [34,35]. The biotinidase gene is located on chromosome 3p25
[36].
Diagnosis Metabolic ataxias usually are diagnosed by screening biochemical tests when the neurologic
abnormalities are first noticed. Based on a positive family history, OTC deficiency and several of the hyperammonemias
can be diagnosed from blood samples taken in utero. Pyruvate dehydrogenase deficiency can, in addition, be
corroborated by a relatively simple biochemical assay on cultured fibroblasts. Despite the identification of individual
gene defects, genetic testing, at least at present, is impractical because of the numerous mutations in the relevant
genes.
Therapy Although the underlying defect usually cannot be corrected, many of the intermittent ataxias can be
06/01/2016 19:50
Overview of the hereditary ataxias
4 sur 19
http://www.uptodate.com/contents/overview-of-the-hereditary-ataxias?to...
indirectly treated:
Supportive therapy for the urea cycle disorders consists of hydration and dietary protein restriction. No treatment
exists for the underlying enzyme deficiency in these disorders except for liver transplantation or, perhaps in the
future, hepatocyte transplantation [37,38]. (See "Hepatocyte transplantation".)
Treatment of the aminoacidurias consists of a high-protein diet. In addition, children with Hartnup disease are
given niacin (nicotinamide) supplementation.
Among the disorders of pyruvate and lactate metabolism, pyruvate dehydrogenase deficiency can be treated with
a ketogenic diet [39] and dichloroacetate, which increases the activity of pyruvate dehydrogenase by stabilizing
the mutant subunit [40,41]. Both infantile [42,43] and late onset multiple carboxylase deficiency can be treated
with pharmacologic doses of biotin [35,44,45].
Possible gene therapies are still experimental [46].
Progressive ataxias Progressive ataxias induced by catalytic deficiency can be seen in a variety of diseases (table
3). These disorders typically present in later childhood or adolescence, unlike the intermittent ataxias. The probable
explanation for this difference is that cumulative damage must reach a threshold before the clinical signs appear.
Storage diseases predominate in this group and include Niemann-Pick disease type C, Wilson disease, metachromatic
leukodystrophy, the heterogeneous ceroid lipofuscinosis and hexosaminidase deficiencies (eg, Tay-Sachs disease,
Sandhoff disease), and adrenoleukodystrophy/adrenomyeloneuropathy (table 3). Some of these disorders are
discussed in detail elsewhere. (See "Hereditary neuropathies associated with generalized disorders" and "Overview of
Niemann-Pick disease" and "Wilson disease: Epidemiology and pathogenesis".)
The diagnosis of a particular storage disease is usually made from the clinical picture in conjunction with histopathologic
findings or biochemical tests. In adrenoleukodystrophy/adrenomyeloneuropathy, for example, the disease is suspected
from the X-linked inheritance and confirmed by elevated serum very long-chain fatty acid concentrations. (See 'X-linked
ataxias' above.)
In Niemann-Pick disease type C (NPC), the diagnosis may be suspected based upon the finding of vertical supranuclear
gaze palsy, which is virtually always present in patients with NPC and ataxia. Additional features include splenomegaly
and large, lipid-laden foam cells in bone marrow. In Wilson disease, important findings include hepatomegaly and
Kayser-Fleischer rings on slit lamp examination (picture 1). (See "Overview of Niemann-Pick disease" and
"Supranuclear disorders of gaze in children" and "Wilson disease: Epidemiology and pathogenesis".)
Treatable diseases No cure has been found for the ataxias induced by storage defects, but specific measures
can at least halt progression in a variety of disorders. Some examples are ataxia with vitamin E deficiency,
cerebrotendinous xanthomatosis, Refsum disease, and Wilson disease.
Ataxia with vitamin E deficiency Vitamin E deficiency from a variety of causes (eg, malabsorption) can lead
to ataxia [47,48]. Several hereditary ataxias also are associated with vitamin E deficiency. The neurologic injury in these
disorders may be related to low vitamin E content [49]. Ataxia with vitamin E deficiency (AVED) is an autosomal
recessive disease caused by mutations in the alpha tocopherol transfer protein gene on chromosome 8q13.1 [50-52]. It
can present as a slowly progressive ataxia syndrome with neuropathy that can resemble Friedreich ataxia. In addition,
some patients develop retinitis pigmentosa [53,54]. High doses of vitamin E typically lead to neurologic improvement,
although recovery may be slow and incomplete [55]. Heterozygotes are phenotypically normal but have serum vitamin E
concentrations 25 percent lower than normal [51].
Hypovitaminosis E results from fat malabsorption in patients with abetalipoproteinemia, an autosomal recessive
disorder also known as Bassen-Kornzweig disease. The disease is caused by mutations in the microsomal triglyceride
transfer protein gene [56]. Defective assembly and secretion of apolipoprotein B (apo B) and apo-B-containing
lipoproteins leads to impaired fat absorption, very low serum concentrations of cholesterol and very low-density
lipoprotein (VLDL) triglyceride, and absent serum beta lipoprotein. The neurologic manifestations include progressive
06/01/2016 19:50
Overview of the hereditary ataxias
5 sur 19
http://www.uptodate.com/contents/overview-of-the-hereditary-ataxias?to...
retinal degeneration (caused by coexisting vitamin A deficiency), peripheral neuropathy, and ataxia. Supplementation
with vitamin E and the other fat-soluble vitamins early in the clinical course may improve the neuropathy and retinopathy.
(See "Neuroacanthocytosis", section on 'Abetalipoproteinemia'.)
A similar autosomal recessive ataxic syndrome with vitamin E deficiency occurs in patients with familial
hypobetalipoproteinemia in which a mutation in the apo B gene is present [57,58]. Interestingly, some mutations
produce no symptoms and are associated with normal serum vitamin E concentrations [58].
Cerebrotendinous xanthomatosis Cerebrotendinous xanthomatosis is a relatively rare autosomal recessive
cause of progressive ataxia. It is characterized by a block in bile acid synthesis caused by mutations in the
mitochondrial sterol 27-hydroxylase gene on chromosome 2q33. The clinical manifestations include ataxia, neuropathy,
cataracts, Achilles tendon xanthomas, and accelerated atherosclerosis. The diagnosis is suggested by elevated serum
cholestanol in the presence of normal serum cholesterol and can be confirmed by genetic testing. Cholestanol is
thought to be responsible for the neurologic toxicity. Treatment with chenodeoxycholic acid can markedly reduce both
serum and cerebrospinal fluid cholestanol and appears to halt progression of the disease. It should be started early
because improvement in established disease is uncommon. (See "Cerebrotendinous xanthomatosis".)
Refsum disease Refsum disease is another treatable progressive ataxia. It should be suspected when a
patient with autosomal recessive ataxia presents with the additional triad of ichthyosis, retinitis pigmentosa, and
neuropathy. Patients with classic Refsum disease are unable to degrade phytanic acid due to deficient activity of
phytanoyl-CoA hydroxylase (PhyH) caused by mutations in the PHYH gene. Strict reduction in dietary phytanic acid
intake may be associated with a significant improvement in both the peripheral neuropathy and ataxia. (See
"Peroxisomal disorders", section on 'Refsum disease'.)
Wilson disease The majority of patients with neurologic Wilson disease have symptoms that fall into one of
several categories: dysarthric, dystonic, tremulous, pseudosclerotic (tremor with or without dysarthria), or parkinsonian
(see "Wilson disease: Clinical manifestations, diagnosis, and natural history", section on 'Neurologic manifestations').
Initially, only one symptom may be present (often unilaterally), but as the disease progresses, complex combinations of
neurologic signs and symptoms may develop. Cerebellar ataxia is generally not the sole neurologic manifestation of
Wilson disease. The ataxia is typically not clinically relevant, and frank limb ataxia is uncommon.
Wilson disease is associated with tissue copper accumulation caused by mutations in the gene for ATP7B, a copper
transporting ATPase (see "Wilson disease: Epidemiology and pathogenesis"). Symptomatic patients are treated with a
chelating agent (penicillamine or trientine) until stable. Trientine may be preferred in patients with neurologic symptoms,
since it appears to be less likely to exacerbate them. (See "Wilson disease: Treatment and prognosis".)
EPISODIC ATAXIAS There are seven varieties of dominantly inherited episodic ataxias (EAs), called EA1 through
EA7. Of these, EA1 and EA2 account for the majority of reported cases [59]. The diagnosis of episodic ataxia is
typically made based upon the history and clinical features. Molecular genetic testing is clinically available for some of
these disorders [60]. Both EA1 and EA2 respond to treatment with acetazolamide (250 to 750 mg/day) [61-65], and
EA2 responds to dalfampridine as discussed below.
Episodic ataxia type 1 Patients with EA1 present with brief episodes of cerebellar dysfunction consisting of gait
unsteadiness, limb ataxia, dysarthria, titubation, nystagmus, or tremor lasting for only a few minutes [9,66,67]. These
spells, often accompanied by myokymia (rippling of muscles), can be induced by triggers that include physical activity
or exercise, stress, environmental temperature, startle, postural change, emotion, hunger, alcohol, intercurrent illness,
or caffeine [68]. Most affected individuals have normal or near normal neurologic function between attacks. However,
persistent cerebellar dysfunction and hearing impairment have been reported [66,67]. Disease onset is usually in
childhood or adolescence.
The genetic basis for EA1 is the presence of point mutations in a voltage-gated potassium channel gene, KCNA1,
located on chromosome 12p13 [69,70]. Molecular genetic testing for KCNA1 mutations is clinically available [71,72].
Typically, the only pathological correlate is minimal atrophy of the anterior cerebellar vermis.
06/01/2016 19:50
Overview of the hereditary ataxias
6 sur 19
http://www.uptodate.com/contents/overview-of-the-hereditary-ataxias?to...
Episodic ataxia type 2 Patients with EA2 have prolonged attacks of ataxia that can last from a few hours to a few
days [73]. Severe vertigo, nausea, and vomiting often are part of the attacks, and gaze-evoked, rebound, or downbeat
nystagmus may be evident not only during but also between attacks [63]. These episodes appear to produce
cumulative cerebellar injury, as patients often develop persistent cerebellar symptoms and cerebellar atrophy [74].
Thus, subtle cerebellar signs, such as nystagmus and mild clumsiness, and the longer duration of episodes suggest
EA2 rather than EA1. The manifestations and rate of progression are variable but usually relatively uniform within a
kindred [63]. As with EA1, disease onset is usually late childhood or adolescence.
EA2 is caused by mutations in the CACNA1A gene that encodes the alpha-1A subunit of a brain-specific P/Q-type
calcium channel [75-78] or, in one family, in the gene for the beta-4 subunit of this channel [79]. The alpha-1A subunit
mutation also can occur de novo [64]. Mutations in the P/Q calcium channel may cause episodic ataxia in EA2 by
reducing calcium dependent neurotransmitter release in cerebellar Purkinje cells [80]. Molecular genetic testing for
CACNA1A mutations is clinically available [81].
As noted above, acetazolamide is often effective for reducing the frequency of attacks. In addition, the potassium
channel blocker dalfampridine (4-aminopyridine) is beneficial, as shown in a randomized controlled trial of 10 patients
with EA, including 7 patients with CACNA1A mutations; dalfampridine (5 mg three times a day) was significantly more
effective for reducing attack frequency than placebo [82]. In an earlier pilot study, dalfampridine completely prevented
attacks of ataxia in two patients and markedly reduced attacks in one [83]. Two of these patients had previously
developed an increased frequency of attacks despite treatment with acetazolamide. The proposed mechanism of
dalfampridine is increased excitability of cerebellar Purkinje cells with subsequent increased release of the inhibitory
neurotransmitter gamma aminobutyric acid (GABA) [83]. No trials have compared dalfampridine with acetazolamide in
EA2.
Episodic ataxia types 3 to 7
Episodic ataxia type 3 Patients with EA3 (originally designated as EA4) have recurrent brief (minutes) attacks of
vestibular ataxia, vertigo, tinnitus, and interictal myokymia [65]. The age of onset is variable. The attacks appear
to be responsive to acetazolamide. Genome-wide screening suggests linkage to chromosome 1q42 [84].
Episodic ataxia type 4 Patients with EA4 (previously designated as EA3 and also known as periodic
vestibulocerebellar ataxia) have recurrent attacks of vertigo, diplopia, tinnitus and ataxia beginning in early
adulthood [65,85]. Ocular manifestations include defective smooth pursuit and gaze-evoked nystagmus [86].
Unlike the other EAs, this form appears to be unresponsive to acetazolamide.
Episodic ataxia type 5 EA5 has clinical features similar to those of EA2, with attacks lasting hours [87]. EA5 is
caused by a mutation in the CACNB4 gene on chromosome 2q22-23; the same mutation was identified in another
family with generalized epilepsy but no ataxia [79].
Episodic ataxia type 6 EA6 is caused by a heterozygous mutation in the SLC1A3 gene, a member of the solute
carrier family that encodes excitatory amino acid transporter 1 (EAAT1), and was identified in an adolescent
patient with episodic ataxia, seizures, migraine and alternating hemiplegia [88]. Another SLC1A3 mutation was
found in three family members who had episodic ataxia but no seizures, migraine, or alternating hemiplegia [89].
Episodic ataxia type 7 EA7 was identified in a single family and has clinical features similar to those of EA2, with
the exception that neurologic examination is normal between attacks [90]. Linkage analysis suggested
chromosome 19q13 as the gene locus.
Overlap with other paroxysmal neurologic disorders Mutations in genes encoding ion channels, ion pumps, and
glutamate transporters have been associated with EAs, familial hemiplegic migraine (FHM), seizures, and
spinocerebellar ataxia (SCA). The following observations have been made:
Different mutations in the CACNA1A gene encoding the alpha-1A subunit of the P/Q type calcium channel have
been identified in EA2, FHM type 1, and SCA type 6.
Some patients with EA2 have episodic hemiplegia that may be associated with migraine headaches [91].
06/01/2016 19:50
Overview of the hereditary ataxias
7 sur 19
http://www.uptodate.com/contents/overview-of-the-hereditary-ataxias?to...
Co-occurrence of FHM with childhood epilepsy and cerebellar ataxia in a single family with a CACNA1A mutation
has been reported [92].
As mentioned above in the discussion of EA6, a heterozygous mutation in the SLC1A3 gene was identified in a
single adolescent patient with episodic ataxia, seizures, migraine, and alternating hemiplegia [88]
EA, FHM, and SCA are often associated with cerebellar atrophy.
Disturbances of neuronal excitability may be the underlying mechanism causing these different clinical manifestations.
(See "Hemiplegic migraine", section on 'Familial hemiplegic migraine' and "The spinocerebellar ataxias".)
OTHER DISORDERS WITH ATAXIA AND MYOCLONUS
Unverricht-Lundborg disease Unverricht-Lundborg disease (ULD) is one form of progressive myoclonus epilepsy
(PME) that is characterized by myoclonic seizures and progressive ataxia. ULD is discussed separately. (See
"Hyperkinetic movement disorders in children", section on 'Unverricht-Lundborg disease'.)
Sialidosis Sialidosis (neuraminidase deficiency, mucolipidosis type I) is an autosomal recessive disorder
characterized by a defect in the sialidase (neuraminidase) gene on chromosome 6p21.3 [93]. Two main clinical variants
of sialidosis have been described:
Sialidosis type I is characterized by late onset with myoclonus and bilateral macular cherry-red spots.
Sialidosis type II is characterized by infantile onset with skeletal dysplasia, intellectual disability (mental
retardation), and hepatosplenomegaly.
SUMMARY
The hereditary ataxias are a genetically heterogeneous group of diseases that are characterized by motor
incoordination resulting from dysfunction of the cerebellum and its connections. The hereditary ataxias have
traditionally been divided into those caused by underlying inborn errors of metabolism (generally autosomal
recessive) and progressive ataxias not due to inborn errors of metabolism. (See 'Introduction and classification'
above.)
The most common autosomal dominant ataxias are the spinocerebellar ataxias (table 1). Other causes include
dentatorubral-pallidoluysian atrophy and the ataxic variant of the Gerstmann-Strussler-Scheinker syndrome. (See
'Autosomal dominant ataxias' above and "The spinocerebellar ataxias".)
The most common autosomal recessive ataxias are Friedreich ataxia and ataxia-telangiectasia. Less frequent
causes are xeroderma pigmentosum and Cockayne syndrome which, like ataxia-telangiectasia, are caused by
defects in DNA repair mechanisms. (See 'Autosomal recessive ataxias' above.)
X-linked progressive ataxias are a heterogeneous group of rare disorders. Some are pure cerebellar syndromes,
while others encompass additional neurologic abnormalities such as spasticity, deafness, intellectual disability
(mental retardation), or dementia. (See 'X-linked ataxias' above.)
Certain mitochondrial disorders can present with a progressive or intermittent ataxia (See 'Mitochondrial ataxias'
above.).
Numerous hereditary ataxias appear to be caused by inborn errors of metabolism. These ataxias tend to have
recessive inheritance, as enzymatic activity of 50 percent in heterozygotes is sufficient for most metabolic
pathways to proceed (see 'Ataxias caused by inborn errors of metabolism' above):
The most common causes of intermittent ataxias are the aminoacidurias resulting from mutations in urea
cycle enzymes, which lead to hyperammonemia, and disorders of pyruvate and lactate metabolism (table 3)
(see 'Intermittent ataxias' above).
Progressive ataxias induced by catalytic deficiency can be seen in a variety of diseases. Storage diseases
predominate in this group and include Niemann-Pick disease type C, Wilson disease, metachromatic
06/01/2016 19:50
Overview of the hereditary ataxias
8 sur 19
http://www.uptodate.com/contents/overview-of-the-hereditary-ataxias?to...
leukodystrophy, the heterogeneous ceroid lipofuscinosis and hexosaminidase deficiencies, and
adrenoleukodystrophy/adrenomyeloneuropathy (table 3) (see 'Progressive ataxias' above).
There are seven varieties of dominantly inherited episodic ataxias (EAs), called EA1 through EA7. Of these, EA1
and EA2 account for the majority of reported cases. The diagnosis of episodic ataxia is typically made based
upon the history and clinical features. Molecular genetic testing is clinically available for some of these disorders.
Both EA1 and EA2 respond to treatment with acetazolamide (250 to 750 mg/day). (See 'Episodic ataxias' above.)
Use of UpToDate is subject to the Subscription and License Agreement.
REFERENCES
1. Brusse E, Maat-Kievit JA, van Swieten JC. Diagnosis and management of early- and late-onset cerebellar ataxia.
Clin Genet 2007; 71:12.
2. Fogel BL, Perlman S. Clinical features and molecular genetics of autosomal recessive cerebellar ataxias. Lancet
Neurol 2007; 6:245.
3. Lutz R, Bodensteiner J, Schaefer B, Gay C. X-linked olivopontocerebellar atrophy. Clin Genet 1989; 35:417.
4. Spira PJ, McLeod JG, Evans WA. A spinocerebellar degeneration with X-linked inheritance. Brain 1979; 102:27.
5. Apak S, Yksel M, Ozmen M, et al. Heterogeneity of X-linked recessive (spino)cerebellar ataxia with or without
spastic diplegia. Am J Med Genet 1989; 34:155.
6. Arts WF, Loonen MC, Sengers RC, Slooff JL. X-linked ataxia, weakness, deafness, and loss of vision in early
childhood with a fatal course. Ann Neurol 1993; 33:535.
7. Kremer H, Hamel BC, van den Helm B, et al. Localization of the gene (or genes) for a syndrome with X-linked
mental retardation, ataxia, weakness, hearing impairment, loss of vision and a fatal course in early childhood.
Hum Genet 1996; 98:513.
8. Farlow MR, DeMyer W, Dlouhy SR, Hodes ME. X-linked recessive inheritance of ataxia and adult-onset
dementia: clinical features and preliminary linkage analysis. Neurology 1987; 37:602.
9. Eunson LH, Rea R, Zuberi SM, et al. Clinical, genetic, and expression studies of mutations in the potassium
channel gene KCNA1 reveal new phenotypic variability. Ann Neurol 2000; 48:647.
10. Pagon RA, Bird TD, Detter JC, Pierce I. Hereditary sideroblastic anaemia and ataxia: an X linked recessive
disorder. J Med Genet 1985; 22:267.
11. Allikmets R, Raskind WH, Hutchinson A, et al. Mutation of a putative mitochondrial iron transporter gene (ABC7)
in X-linked sideroblastic anemia and ataxia (XLSA/A). Hum Mol Genet 1999; 8:743.
12. Bekri S, Kispal G, Lange H, et al. Human ABC7 transporter: gene structure and mutation causing X-linked
sideroblastic anemia with ataxia with disruption of cytosolic iron-sulfur protein maturation. Blood 2000; 96:3256.
13. Flierl A, Reichmann H, Seibel P. Pathophysiology of the MELAS 3243 transition mutation. J Biol Chem 1997;
272:27189.
14. Chomyn A, Enriquez JA, Micol V, et al. The mitochondrial myopathy, encephalopathy, lactic acidosis, and
stroke-like episode syndrome-associated human mitochondrial tRNALeu(UUR) mutation causes aminoacylation
deficiency and concomitant reduced association of mRNA with ribosomes. J Biol Chem 2000; 275:19198.
15. Brner GV, Zeviani M, Tiranti V, et al. Decreased aminoacylation of mutant tRNAs in MELAS but not in MERRF
patients. Hum Mol Genet 2000; 9:467.
16. Chomyn A. The myoclonic epilepsy and ragged-red fiber mutation provides new insights into human mitochondrial
function and genetics. Am J Hum Genet 1998; 62:745.
17. Brini M, Pinton P, King MP, et al. A calcium signaling defect in the pathogenesis of a mitochondrial DNA inherited
oxidative phosphorylation deficiency. Nat Med 1999; 5:951.
18. Mancuso M, Filosto M, Mootha VK, et al. A novel mitochondrial tRNAPhe mutation causes MERRF syndrome.
Neurology 2004; 62:2119.
19. Batshaw ML, Msall M, Beaudet AL, Trojak J. Risk of serious illness in heterozygotes for ornithine
transcarbamylase deficiency. J Pediatr 1986; 108:236.
20. Yudkoff M, Daikhin Y, Nissim I, et al. In vivo nitrogen metabolism in ornithine transcarbamylase deficiency. J Clin
06/01/2016 19:50
Overview of the hereditary ataxias
9 sur 19
http://www.uptodate.com/contents/overview-of-the-hereditary-ataxias?to...
Invest 1996; 98:2167.
21. Gaspari R, Arcangeli A, Mensi S, et al. Late-onset presentation of ornithine transcarbamylase deficiency in a
young woman with hyperammonemic coma. Ann Emerg Med 2003; 41:104.
22. Kleta R, Romeo E, Ristic Z, et al. Mutations in SLC6A19, encoding B0AT1, cause Hartnup disorder. Nat Genet
2004; 36:999.
23. Seow HF, Brer S, Brer A, et al. Hartnup disorder is caused by mutations in the gene encoding the neutral
amino acid transporter SLC6A19. Nat Genet 2004; 36:1003.
24. Robinson BH, MacMillan H, Petrova-Benedict R, Sherwood WG. Variable clinical presentation in patients with
defective E1 component of pyruvate dehydrogenase complex. J Pediatr 1987; 111:525.
25. Dahl HH, Brown GK, Brown RM, et al. Mutations and polymorphisms in the pyruvate dehydrogenase E1 alpha
gene. Hum Mutat 1992; 1:97.
26. Brown RM, Head RA, Boubriak II, et al. Mutations in the gene for the E1beta subunit: a novel cause of pyruvate
dehydrogenase deficiency. Hum Genet 2004; 115:123.
27. Head RA, Brown RM, Zolkipli Z, et al. Clinical and genetic spectrum of pyruvate dehydrogenase deficiency:
dihydrolipoamide acetyltransferase (E2) deficiency. Ann Neurol 2005; 58:234.
28. Hong YS, Korman SH, Lee J, et al. Identification of a common mutation (Gly194Cys) in both Arab Moslem and
Ashkenazi Jewish patients with dihydrolipoamide dehydrogenase (E3) deficiency: possible beneficial effect of
vitamin therapy. J Inherit Metab Dis 2003; 26:816.
29. Brown RM, Head RA, Brown GK. Pyruvate dehydrogenase E3 binding protein deficiency. Hum Genet 2002;
110:187.
30. Maj MC, MacKay N, Levandovskiy V, et al. Pyruvate dehydrogenase phosphatase deficiency: identification of the
first mutation in two brothers and restoration of activity by protein complementation. J Clin Endocrinol Metab
2005; 90:4101.
31. Aoki Y, Li X, Sakamoto O, et al. Identification and characterization of mutations in patients with holocarboxylase
synthetase deficiency. Hum Genet 1999; 104:143.
32. Suzuki Y, Aoki Y, Ishida Y, et al. Isolation and characterization of mutations in the human holocarboxylase
synthetase cDNA. Nat Genet 1994; 8:122.
33. Dupuis L, Leon-Del-Rio A, Leclerc D, et al. Clustering of mutations in the biotin-binding region of holocarboxylase
synthetase in biotin-responsive multiple carboxylase deficiency. Hum Mol Genet 1996; 5:1011.
34. Wolf B, Grier RE, Allen RJ, et al. Biotinidase deficiency: the enzymatic defect in late-onset multiple carboxylase
deficiency. Clin Chim Acta 1983; 131:273.
35. Wolf B, Heard GS, Weissbecker KA, et al. Biotinidase deficiency: initial clinical features and rapid diagnosis. Ann
Neurol 1985; 18:614.
36. Pomponio RJ, Reynolds TR, Cole H, et al. Mutational hotspot in the human biotinidase gene causes profound
biotinidase deficiency. Nat Genet 1995; 11:96.
37. Todo S, Starzl TE, Tzakis A, et al. Orthotopic liver transplantation for urea cycle enzyme deficiency. Hepatology
1992; 15:419.
38. Busuttil AA, Goss JA, Seu P, et al. The role of orthotopic liver transplantation in the treatment of ornithine
transcarbamylase deficiency. Liver Transpl Surg 1998; 4:350.
39. Wexler ID, Hemalatha SG, McConnell J, et al. Outcome of pyruvate dehydrogenase deficiency treated with
ketogenic diets. Studies in patients with identical mutations. Neurology 1997; 49:1655.
40. McCormick K, Viscardi RM, Robinson B, Heininger J. Partial pyruvate decarboxylase deficiency with profound
lactic acidosis and hyperammonemia: responses to dichloroacetate and benzoate. Am J Med Genet 1985;
22:291.
41. Morten KJ, Beattie P, Brown GK, Matthews PM. Dichloroacetate stabilizes the mutant E1alpha subunit in
pyruvate dehydrogenase deficiency. Neurology 1999; 53:612.
42. Suormala T, Fowler B, Duran M, et al. Five patients with a biotin-responsive defect in holocarboxylase formation:
evaluation of responsiveness to biotin therapy in vivo and comparative biochemical studies in vitro. Pediatr Res
1997; 41:666.
43. Sakamoto O, Suzuki Y, Li X, et al. Relationship between kinetic properties of mutant enzyme and biochemical and
clinical responsiveness to biotin in holocarboxylase synthetase deficiency. Pediatr Res 1999; 46:671.
06/01/2016 19:50
Overview of the hereditary ataxias
10 sur 19
http://www.uptodate.com/contents/overview-of-the-hereditary-ataxias?to...
44. Wastell HJ, Bartlett K, Dale G, Shein A. Biotinidase deficiency: a survey of 10 cases. Arch Dis Child 1988;
63:1244.
45. Lott IT, Lottenberg S, Nyhan WL, Buchsbaum MJ. Cerebral metabolic change after treatment in biotinidase
deficiency. J Inherit Metab Dis 1993; 16:399.
46. Ginn SL, Cunningham SC, Zheng M, et al. In vivo assessment of mutations in OTC for dominant-negative effects
following rAAV2/8-mediated gene delivery to the mouse liver. Gene Ther 2009; 16:820.
47. Sokol RJ, Guggenheim MA, Iannaccone ST, et al. Improved neurologic function after long-term correction of
vitamin E deficiency in children with chronic cholestasis. N Engl J Med 1985; 313:1580.
48. Satya-Murti S, Howard L, Krohel G, Wolf B. The spectrum of neurologic disorder from vitamin E deficiency.
Neurology 1986; 36:917.
49. Traber MG, Sokol RJ, Ringel SP, et al. Lack of tocopherol in peripheral nerves of vitamin E-deficient patients with
peripheral neuropathy. N Engl J Med 1987; 317:262.
50. Ouahchi K, Arita M, Kayden H, et al. Ataxia with isolated vitamin E deficiency is caused by mutations in the alphatocopherol transfer protein. Nat Genet 1995; 9:141.
51. Gotoda T, Arita M, Arai H, et al. Adult-onset spinocerebellar dysfunction caused by a mutation in the gene for the
alpha-tocopherol-transfer protein. N Engl J Med 1995; 333:1313.
52. Kono N, Ohto U, Hiramatsu T, et al. Impaired -TTP-PIPs interaction underlies familial vitamin E deficiency.
Science 2013; 340:1106.
53. Yokota T, Shiojiri T, Gotoda T, et al. Friedreich-like ataxia with retinitis pigmentosa caused by the His101Gln
mutation of the alpha-tocopherol transfer protein gene. Ann Neurol 1997; 41:826.
54. Mariotti C, Gellera C, Rimoldi M, et al. Ataxia with isolated vitamin E deficiency: neurological phenotype, clinical
follow-up and novel mutations in TTPA gene in Italian families. Neurol Sci 2004; 25:130.
55. Schuelke M, Mayatepek E, Inter M, et al. Treatment of ataxia in isolated vitamin E deficiency caused by alphatocopherol transfer protein deficiency. J Pediatr 1999; 134:240.
56. Sharp D, Blinderman L, Combs KA, et al. Cloning and gene defects in microsomal triglyceride transfer protein
associated with abetalipoproteinaemia. Nature 1993; 365:65.
57. Young SG, Hubl ST, Smith RS, et al. Familial hypobetalipoproteinemia caused by a mutation in the apolipoprotein
B gene that results in a truncated species of apolipoprotein B (B-31). A unique mutation that helps to define the
portion of the apolipoprotein B molecule required for the formation of buoyant, triglyceride-rich lipoproteins. J Clin
Invest 1990; 85:933.
58. Young SG, Bihain B, Flynn LM, et al. Asymptomatic homozygous hypobetalipoproteinemia associated with
apolipoprotein B45.2. Hum Mol Genet 1994; 3:741.
59. Jen JC, Graves TD, Hess EJ, et al. Primary episodic ataxias: diagnosis, pathogenesis and treatment. Brain
2007; 130:2484.
60. Bird TD. Hereditary ataxia overview. In: GeneReviews [Internet]. www.ncbi.nlm.nih.gov/bookshelf
/br.fcgi?book=gene&part=ataxias (Accessed on September 29, 2011).
61. Jen J. Familial Episodic Ataxias and Related Ion Channel Disorders. Curr Treat Options Neurol 2000; 2:429.
62. Zasorin NL, Baloh RW, Myers LB. Acetazolamide-responsive episodic ataxia syndrome. Neurology 1983;
33:1212.
63. Baloh RW, Yue Q, Furman JM, Nelson SF. Familial episodic ataxia: clinical heterogeneity in four families linked to
chromosome 19p. Ann Neurol 1997; 41:8.
64. Yue Q, Jen JC, Thwe MM, et al. De novo mutation in CACNA1A caused acetazolamide-responsive episodic
ataxia. Am J Med Genet 1998; 77:298.
65. Steckley JL, Ebers GC, Cader MZ, McLachlan RS. An autosomal dominant disorder with episodic ataxia, vertigo,
and tinnitus. Neurology 2001; 57:1499.
66. Tomlinson SE, Rajakulendran S, Tan SV, et al. Clinical, genetic, neurophysiological and functional study of new
mutations in episodic ataxia type 1. J Neurol Neurosurg Psychiatry 2013; 84:1107.
67. Graves TD, Cha YH, Hahn AF, et al. Episodic ataxia type 1: clinical characterization, quality of life and genotypephenotype correlation. Brain 2014; 137:1009.
68. Gancher ST, Nutt JG. Autosomal dominant episodic ataxia: a heterogeneous syndrome. Mov Disord 1986; 1:239.
06/01/2016 19:50
Overview of the hereditary ataxias
11 sur 19
http://www.uptodate.com/contents/overview-of-the-hereditary-ataxias?to...
69. Browne DL, Gancher ST, Nutt JG, et al. Episodic ataxia/myokymia syndrome is associated with point mutations
in the human potassium channel gene, KCNA1. Nat Genet 1994; 8:136.
70. Scheffer H, Brunt ER, Mol GJ, et al. Three novel KCNA1 mutations in episodic ataxia type I families. Hum Genet
1998; 102:464.
71. Pessia M, Hanna MG. Episodic ataxia type 1. In: GeneReviews [Internet]. www.ncbi.nlm.nih.gov/bookshelf
/br.fcgi?book=gene&part=ea1 (Accessed on September 29, 2011).
72. Tacik P, Guthrie KJ, Strongosky AJ, et al. Whole-exome sequencing as a diagnostic tool in a family with episodic
ataxia type 1. Mayo Clin Proc 2015; 90:366.
73. Jen J, Kim GW, Baloh RW. Clinical spectrum of episodic ataxia type 2. Neurology 2004; 62:17.
74. Denier C, Ducros A, Vahedi K, et al. High prevalence of CACNA1A truncations and broader clinical spectrum in
episodic ataxia type 2. Neurology 1999; 52:1816.
75. Ophoff RA, Terwindt GM, Vergouwe MN, et al. Familial hemiplegic migraine and episodic ataxia type-2 are
caused by mutations in the Ca2+ channel gene CACNL1A4. Cell 1996; 87:543.
76. Spacey SD, Hildebrand ME, Materek LA, et al. Functional implications of a novel EA2 mutation in the P/Q-type
calcium channel. Ann Neurol 2004; 56:213.
77. Wan J, Carr JR, Baloh RW, Jen JC. Nonconsensus intronic mutations cause episodic ataxia. Ann Neurol 2005;
57:131.
78. Riant F, Mourtada R, Saugier-Veber P, Tournier-Lasserve E. Large CACNA1A deletion in a family with episodic
ataxia type 2. Arch Neurol 2008; 65:817.
79. Escayg A, De Waard M, Lee DD, et al. Coding and noncoding variation of the human calcium-channel beta4subunit gene CACNB4 in patients with idiopathic generalized epilepsy and episodic ataxia. Am J Hum Genet
2000; 66:1531.
80. Kullmann DM. The neuronal channelopathies. Brain 2002; 125:1177.
81. Spacey S. Episodic ataxia type 2. In: GeneReviews [Internet]. www.ncbi.nlm.nih.gov/bookshelf
/br.fcgi?book=gene&part=ea2 (Accessed on September 29, 2011).
82. Strupp M, Kalla R, Claassen J, et al. A randomized trial of 4-aminopyridine in EA2 and related familial episodic
ataxias. Neurology 2011; 77:269.
83. Strupp M, Kalla R, Dichgans M, et al. Treatment of episodic ataxia type 2 with the potassium channel blocker
4-aminopyridine. Neurology 2004; 62:1623.
84. Cader MZ, Steckley JL, Dyment DA, et al. A genome-wide screen and linkage mapping for a large pedigree with
episodic ataxia. Neurology 2005; 65:156.
85. FARMER TW, MUSTIAN VM. Vestibulocerebellar ataxia. A newly defined hereditary syndrome with periodic
manifestations. Arch Neurol 1963; 8:471.
86. Damji KF, Allingham RR, Pollock SC, et al. Periodic vestibulocerebellar ataxia, an autosomal dominant ataxia with
defective smooth pursuit, is genetically distinct from other autosomal dominant ataxias. Arch Neurol 1996;
53:338.
87. Herrmann A, Braathen GJ, Russell MB. [Episodic ataxias]. Tidsskr Nor Laegeforen 2005; 125:2005.
88. Jen JC, Wan J, Palos TP, et al. Mutation in the glutamate transporter EAAT1 causes episodic ataxia, hemiplegia,
and seizures. Neurology 2005; 65:529.
89. de Vries B, Mamsa H, Stam AH, et al. Episodic ataxia associated with EAAT1 mutation C186S affecting
glutamate reuptake. Arch Neurol 2009; 66:97.
90. Kerber KA, Jen JC, Lee H, et al. A new episodic ataxia syndrome with linkage to chromosome 19q13. Arch
Neurol 2007; 64:749.
91. Jen J, Yue Q, Nelson SF, et al. A novel nonsense mutation in CACNA1A causes episodic ataxia and hemiplegia.
Neurology 1999; 53:34.
92. Kors EE, Melberg A, Vanmolkot KR, et al. Childhood epilepsy, familial hemiplegic migraine, cerebellar ataxia, and
a new CACNA1A mutation. Neurology 2004; 63:1136.
93. Pshezhetsky AV, Richard C, Michaud L, et al. Cloning, expression and chromosomal mapping of human lysosomal
sialidase and characterization of mutations in sialidosis. Nat Genet 1997; 15:316.
06/01/2016 19:50
Overview of the hereditary ataxias
12 sur 19
http://www.uptodate.com/contents/overview-of-the-hereditary-ataxias?to...
Topic 6234 Version 16.0
06/01/2016 19:50
Overview of the hereditary ataxias
13 sur 19
http://www.uptodate.com/contents/overview-of-the-hereditary-ataxias?to...
GRAPHICS
Characteristics of the autosomal dominant spinocerebellar ataxias
Disorder
Distinguishing features
Gene locus and protein
SCA1
Pyramidal signs, peripheral neuropathy
ATXN1
CAG repeat, ataxin-1
SCA2
Slow saccades; less often myoclonus,
areflexia
ATXN2
CAG repeat, ataxin-2
SCA3 (MJD)
Slow saccades, persistent stare,
extrapyramidal signs, peripheral
neuropathy
ATXN3
CAG repeat, ataxin-3
(MJD1)
SCA4
Sensory neuropathy
16q22.1
SCA5
Early onset but slow progression
SPTBN2
Beta III spectrin
SCA6
May have very late onset, mild, may lack
family history, nystagmus
CACNA1A
CAG repeat, alpha 1A P/Q
calcium channel subunit
SCA7
Macular degeneration
ATXN7
CAG repeat, ataxin-7
SCA8
Mild disease
ATXN8
CTG*CAG repeat
ATXN8OS
SCA9
Not assigned
SCA10
Generalized or complex partial seizures
ATXN10
ATTCT repeat, ataxin-10
SCA11
Mild disease
TTBK2
Tau tubulin kinase-2
SCA12
Tremor, dementia
PPP2R2B
CAG repeat in 5' region,
protein phosphatase 2A
SCA13
Mental retardation
KCNC3
Voltage gated potassium
channel KCNC3
SCA14
Intermittent myoclonus with early onset
disease
PRKCG
Protein kinase C gamma
SCA15/16
Slowly progressive
ITPR1
Inositol 1,4,5-triphosphate
receptor 1
SCA17
Gait ataxia, dementia
TBP
CAG repeats, TATA binding
protein
SCA18
Pyramidal signs, weakness, sensory
axonal neuropathy
7q22-q32
SCA19/22
Predominantly cerebellar syndrome,
sometimes with cognitive impairment or
myoclonus
KCND3 gene
SCA20
Palatal tremor and dysphonia
11q12
SCA21
Mild to severe cognitive impairment
TMEM240
Transmembrane protein
240
SCA23
Distal sensory deficits
PDYN
Prodynorphin
SCA24
Recessive inheritance; redesignated as
SCAR4
1p36
Voltage-gated potassium
channel Kv4.3
06/01/2016 19:50
Overview of the hereditary ataxias
14 sur 19
http://www.uptodate.com/contents/overview-of-the-hereditary-ataxias?to...
SCA25
Sensory neuropathy, facial tics,
gastrointestinal symptoms
2p21-p13
SCA26
Pure cerebellar ataxia
EEF2
Eukaryotic translation
elongation factor 2
SCA27
Cognitive impairment
FGF14
Fibroblast growth factor 14
SCA28
Ophthalmoparesis and ptosis
AFG3L2
Catalytic subunit of the
mitochondrial AAA
protease
SCA29
Early onset, nonprogressive ataxia; may
be an allelic variant of SCA15
3p26
SCA30
Slowly progressive, relatively pure ataxia
4q34.3-q35.1
SCA31
Decreased muscle tone
BEAN
SCA32
Cognitive impairment, affected males with
azoospermia and testicular atrophy
7q32-q33
SCA33
Not assigned
SCA34
Skin lesions consisting of papulosquamous
erythematous ichthyosiform plaques
ELOVL4
ELOVL fatty acid elongase
4
SCA35
Late onset, slowly progressive gait and
limb ataxia
TGM6
Transglutaminase 6
SCA36
Late onset, truncal ataxia, dysarthria,
variable motor neuron disease and
sensorineural hearing loss
NOP56
GGCCTG repeat
SCA37
Late onset, falls, dysarthria, clumsiness,
abnormal vertical eye movements
1p32
SCA38
Slowly progressive pure cerebellar
phenotype
ELOVL5
ELOVL fatty acid elongase
5
SCA39
Not assigned
SCA40
Hyperreflexia and spasticity
CCDC88
Coiled-coil domaincontaining 88C
DRPLA
Chorea, seizures, myoclonus, dementia
ATN1
CAG repeat, atrophin-1
(TGGAA)n repeat
DRPLA: dentatorubral pallidoluysian atrophy; MJD: Machado-Joseph disease; SCA: spinocerebellar ataxia.
Data from: Online Mendelian Inheritance in Man and Neuromuscular Disease Center, Washington University.
Graphic 74269 Version 11.0
06/01/2016 19:50
Overview of the hereditary ataxias
15 sur 19
http://www.uptodate.com/contents/overview-of-the-hereditary-ataxias?to...
Diagnostic criteria for ataxia-telangiectasia
Definitive diagnosis*
Male or female patient with either increased radiation-induced chromosomal breakage in cultured cells
or progressive cerebellar ataxia and who has disabling mutations on both alleles of ATM.
Probable diagnosis*
Male or female patient with progressive cerebellar ataxia and three of the following four findings:
1. Ocular or facial telangiectasia.
2. Serum IgA at least 2 SD below normal for age.
3. Alpha fetoprotein at least 2 SD above normal for age.
4. Increased radiation-induced chromosomal breakage in cultured cells.
Possible diagnosis*
Male or female patient with progressive cerebellar ataxia and at least one of the following four
findings:
1. Ocular or facial telangiectasia.
2. Serum IgA at least 2 SD below normal for age.
3. Alpha fetoprotein more than 2 SD above normal for age.
4. Increased chromosomal breakage after exposure to irradiation.
* Patients with a definitive or probable diagnosis are assumed to have a greater than 98 and 85 percent
probability, respectively, that in 20 years they will still have the same diagnosis. Patients with a possible
diagnosis are those that have some but not all of the characteristic clinical or laboratory findings of a
particular disorder.
From Conley, ME, Notarangelo, LD, Etzioni, A. Clin Immunol 1999; 93:190.
Graphic 57053 Version 2.0
06/01/2016 19:50
Overview of the hereditary ataxias
16 sur 19
http://www.uptodate.com/contents/overview-of-the-hereditary-ataxias?to...
Major causes of hereditary ataxias due to known enzymatic defects
Disorder
Gene locus and protein
Intermittent ataxias
Hyperammonemias and aminoacidurias
Ornithine transcarbamylase deficiency
Xp21.1
Ornithine transcarbamylase
Citrullinemia
9q34
Arginosuccinate synthetase
Arginase deficiency
6q23
Arginase
Argininosuccinic aciduria
7cen-q11
Arginosuccinate lyase
Hyperornithemia-hyperammonemiahomocitrullinuria syndrome
13q14
Mitochondrial ornithine
transporter
Hartnup disease
5p15.33
Neutral amino acid transporter
Isovaleric acidemia
15q14
Isovaleric acid CoA
dehydrogenase
Pyruvate dehydrogenase complex
Xp22.2 (most
common)
E1-alpha subunit (most common)
Multiple carboxylase deficiency
21q22
Holocarboxylase synthetase
Tay-Sachs disease
15q23-q24
Alpha subunit of hexosaminidase
A
Sandhoff disease
15q13
Beta subunit of hexosaminidase A
and B
Niemann-Pick type A and B
11p15.4-p15.1
Acid sphingomyelinase
Niemann-Pick type C
18q11-q12
NPC1
14q24.3
NPC2
Metachromatic leukodystrophy
22q13
Arylsulfatase A
Adrenomyeloneuropathy
Xq28
Adrenoleukodystrophy protein
Abetalipoproteinemia
4q22
Microsomal triglyceride transfer
protein
Hypobetalipoproteinemia
2p24
Apolipoprotein B
Cerebrotendinous xanthomatosis
2q33
Mitochondrial sterol
27-hydroxylase
Ataxia with vitamin E deficiency
8q13
Alpha-tocopherol transfer protein
Lesch-Nyhan syndrome
Xq26
Hypoxanthine-guanine
phosphoribosyl- transferase
Wilson disease
13q14
ATP7B (copper transporting
ATPase)
Ceroid lipofuscinosis
Several variants
Multiple gene products
Refsum disease
10pter
Phytanoyl CoA hydroxylase
Disorders of pyruvate and lactate metabolism
Progressive ataxias
06/01/2016 19:50
Overview of the hereditary ataxias
17 sur 19
X-linked ataxia, ichthyosis, and
tapetoretinal dystrophy
http://www.uptodate.com/contents/overview-of-the-hereditary-ataxias?to...
Xpter-p22
Arylsulfatase C
Graphic 56126 Version 4.0
06/01/2016 19:50
Overview of the hereditary ataxias
18 sur 19
http://www.uptodate.com/contents/overview-of-the-hereditary-ataxias?to...
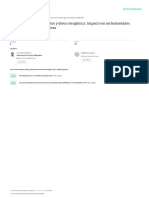
Kayser-Fleischer ring
Kayser-Fleischer ring (arrow) in a patient with advanced
neuropsychiatric Wilson disease. The dense brown copper deposits
encircle the iris. It is rare to see Kayser-Fleischer rings without the aid
of a slit lamp examination because Wilson disease is usually recognized
at an earlier stage when the rings are not as prominent.
Courtesy of Marshall M Kaplan, MD.
Graphic 65925 Version 2.0
06/01/2016 19:50
Overview of the hereditary ataxias
19 sur 19
http://www.uptodate.com/contents/overview-of-the-hereditary-ataxias?to...
Disclosures
Disclosures: Puneet Opal, MD, PhD Nothing to disclose. Huda Y Zoghbi, MD Nothing to disclose. Marc C Patterson, MD, FRACP
Grant/Research/Clinical Trial Support: Actelion [Lysosomal diseases (Miglustat)]. Consultant/Advisory Boards: Amicus; Agios; Cydan;
Genzyme; Orphazyme; Shire HGT [Lysosomal diseases (Arimoclomol, cyclodextrin, glucocerebrosidase)]; Stem Cells, Inc; Vtesse [Lysosomal
diseases (Human embryonic stem cells)]. Helen V Firth, DM, FRCP, DCH Nothing to disclose. John F Dashe, MD, PhD Nothing to disclose.
Contributor disclosures are reviewed for conflicts of interest by the editorial group. When found, these are addressed by vetting through a
multi-level review process, and through requirements for references to be provided to support the content. Appropriately referenced content is
required of all authors and must conform to UpToDate standards of evidence.
Conflict of interest policy
06/01/2016 19:50
You might also like
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (890)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- 40 Easy and Natural Essential Oil Recipes Detox Your Home, Cooking, and Personal Care Routine - Caitlin WeeksDocument105 pages40 Easy and Natural Essential Oil Recipes Detox Your Home, Cooking, and Personal Care Routine - Caitlin WeeksVincentius Milten100% (1)
- 50 Foods To Avoid To Lose Weigh - Malik Johnson PDFDocument391 pages50 Foods To Avoid To Lose Weigh - Malik Johnson PDFtotherethymNo ratings yet
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Dietetic Internship - Mini Case Study PowerpointDocument21 pagesDietetic Internship - Mini Case Study Powerpointapi-535934790No ratings yet
- OIC Standards HalalDocument34 pagesOIC Standards HalalfarizzulNo ratings yet
- TF TestsDocument72 pagesTF Testsluismsgoncalves86% (14)
- Ok sa Deped Program Accomplishment ReportDocument6 pagesOk sa Deped Program Accomplishment Reportkristine arnaizNo ratings yet
- Lentivirus Production ProtocolDocument11 pagesLentivirus Production ProtocoldupuytrenNo ratings yet
- Eview: Alternative Polyadenylation: A Twist On mRNA 3 End FormationDocument9 pagesEview: Alternative Polyadenylation: A Twist On mRNA 3 End FormationdupuytrenNo ratings yet
- Adenovirus Production ProtocolDocument13 pagesAdenovirus Production ProtocoldupuytrenNo ratings yet
- Genome-Wide Alternative Polyadenylation in Animals: Insights From High-Throughput TechnologiesDocument10 pagesGenome-Wide Alternative Polyadenylation in Animals: Insights From High-Throughput TechnologiesdupuytrenNo ratings yet
- Fluorescence and Fluorescence ApplicationsDocument13 pagesFluorescence and Fluorescence ApplicationsPaulraj Mosae SelvakumarNo ratings yet
- Simplicon Rna Reprogramming - PrinterviewDocument5 pagesSimplicon Rna Reprogramming - PrinterviewdupuytrenNo ratings yet
- Non-Genetic Inheritance Via The Male Germline in Mammals: ReviewDocument7 pagesNon-Genetic Inheritance Via The Male Germline in Mammals: ReviewdupuytrenNo ratings yet
- Heat Inactivation ProtocolDocument1 pageHeat Inactivation ProtocoldupuytrenNo ratings yet
- Direct Comparison of Dna Versus Mrna On The Efficiency of Induced Pluripotent Stem Cells Generation From Human Primary FibroblastsDocument7 pagesDirect Comparison of Dna Versus Mrna On The Efficiency of Induced Pluripotent Stem Cells Generation From Human Primary FibroblastsdupuytrenNo ratings yet
- Microtubules in SynapseDocument6 pagesMicrotubules in SynapsedupuytrenNo ratings yet
- Dynamics of Epigenetic Phenomena: Intergenerational and Intragenerational Phenotype Washout'Document8 pagesDynamics of Epigenetic Phenomena: Intergenerational and Intragenerational Phenotype Washout'dupuytrenNo ratings yet
- An Integrative Framework For Understanding The Mechanisms and Multigenerational Consequences of Transgenerational PlasticityDocument22 pagesAn Integrative Framework For Understanding The Mechanisms and Multigenerational Consequences of Transgenerational PlasticitydupuytrenNo ratings yet
- Adhesion Signalling Complexes: PrimerDocument5 pagesAdhesion Signalling Complexes: PrimerdupuytrenNo ratings yet
- 5550 FullDocument8 pages5550 FulldupuytrenNo ratings yet
- Uncovering Cell Biology in The Third DimensionDocument5 pagesUncovering Cell Biology in The Third DimensiondupuytrenNo ratings yet
- Stemcells 2006-0409Document9 pagesStemcells 2006-0409dupuytrenNo ratings yet
- Commercialization of Organoids: ForumDocument4 pagesCommercialization of Organoids: ForumdupuytrenNo ratings yet
- Focal Adhesions in Osteoneogenesis: Special Issue Paper 1441Document13 pagesFocal Adhesions in Osteoneogenesis: Special Issue Paper 1441dupuytrenNo ratings yet
- Echinocandins ReviewDocument11 pagesEchinocandins ReviewdupuytrenNo ratings yet
- Perspectives: Applying CRISPR-Cas9 Tools To Identify and Characterize Transcriptional EnhancersDocument8 pagesPerspectives: Applying CRISPR-Cas9 Tools To Identify and Characterize Transcriptional EnhancersdupuytrenNo ratings yet
- Studying Hallmarks of Cancer - AbcamDocument11 pagesStudying Hallmarks of Cancer - AbcamdupuytrenNo ratings yet
- Pioneer Transcription Factors in Cell Fate ControlDocument5 pagesPioneer Transcription Factors in Cell Fate ControldupuytrenNo ratings yet
- Cellular Viability - Calcein / Propidium Iodide: We've Performed This Assay On The Following Cell TypesDocument1 pageCellular Viability - Calcein / Propidium Iodide: We've Performed This Assay On The Following Cell TypesdupuytrenNo ratings yet
- New Drugs 2017Document2 pagesNew Drugs 2017dupuytrenNo ratings yet
- Plan the retrosynthesis of target moleculesDocument3 pagesPlan the retrosynthesis of target moleculesJaya KumarNo ratings yet
- 8927 FullDocument5 pages8927 FulldupuytrenNo ratings yet
- Treatment of Antineutrophil Cytoplasmic Antibodyassociated VasculitisDocument8 pagesTreatment of Antineutrophil Cytoplasmic Antibodyassociated VasculitisdupuytrenNo ratings yet
- Preliminary MatterDocument26 pagesPreliminary MatterdupuytrenNo ratings yet
- Neuroview: How To Be A Graduate AdviseeDocument3 pagesNeuroview: How To Be A Graduate AdviseedupuytrenNo ratings yet
- Cold Spring Harb Protoc-2011-Matheu-pdb - Prot5565Document6 pagesCold Spring Harb Protoc-2011-Matheu-pdb - Prot5565dupuytrenNo ratings yet
- Manish Synopsis1 EditDocument13 pagesManish Synopsis1 EditManish kumar gurjarNo ratings yet
- Favoured Food Prophet Part3Document1 pageFavoured Food Prophet Part3Fahad ParuvanathNo ratings yet
- IntroductionDocument4 pagesIntroductionCeyah Nurr0% (1)
- Nutrition LectureDocument2 pagesNutrition LectureIrwan M. IskoberNo ratings yet
- Stroke - Nutrition Guide For CliniciansDocument1 pageStroke - Nutrition Guide For CliniciansAjo SultanNo ratings yet
- Feeds Feeding of Dairy AnimalsDocument174 pagesFeeds Feeding of Dairy AnimalsKiran KumarNo ratings yet
- Digestibility Determination in Fish Using Chromic Oxide Marking and Analysis of Contents From Different Segments of The Gastrointestinal TractDocument8 pagesDigestibility Determination in Fish Using Chromic Oxide Marking and Analysis of Contents From Different Segments of The Gastrointestinal TractRafael Hamakawa ViannaNo ratings yet
- Karbohidrat: Dyke Gita Wirasisya, S.Farm., M.SC., Apt Program Studi Farmasi, Fakultas Kedokteran, Universitas MataramDocument37 pagesKarbohidrat: Dyke Gita Wirasisya, S.Farm., M.SC., Apt Program Studi Farmasi, Fakultas Kedokteran, Universitas Matarambrahmani ptrNo ratings yet
- Hhs Lower Body Lesson Plan Leg DayDocument3 pagesHhs Lower Body Lesson Plan Leg Dayapi-481363865No ratings yet
- Food Energy - WikipediaDocument28 pagesFood Energy - WikipediaviraNo ratings yet
- Lemon Grass DistillateDocument9 pagesLemon Grass DistillateJoe Joseph100% (1)
- Risk Factors of Diabetes in RawalpindiDocument29 pagesRisk Factors of Diabetes in RawalpindiFarrukh Ali BaigNo ratings yet
- Micro Niches You Can Work On - Sheet1Document1 pageMicro Niches You Can Work On - Sheet1zuneraNo ratings yet
- Bioequivalence Study of Two Formulations of Bisoprolol Fumarate Film-Coated Tablets in Healthy SubjectsDocument8 pagesBioequivalence Study of Two Formulations of Bisoprolol Fumarate Film-Coated Tablets in Healthy SubjectsSafira DewiNo ratings yet
- Underutilised Greens in KarnatakaDocument3 pagesUnderutilised Greens in KarnatakashalNo ratings yet
- Complete guide blood testsDocument7 pagesComplete guide blood testsVickram JainNo ratings yet
- Dietabajaencarbohidratos Moreno Capponi 2020Document11 pagesDietabajaencarbohidratos Moreno Capponi 2020PerlaNo ratings yet
- Global Update Food Security MonitoringDocument13 pagesGlobal Update Food Security MonitoringNasrul SetiawanNo ratings yet
- Andrew SaulDocument3 pagesAndrew Saultito19593No ratings yet
- How Do We Take Care of Our Endocrine SystemDocument7 pagesHow Do We Take Care of Our Endocrine SystemAndrei CunananNo ratings yet
- I. Objectives: Grade Level Quarter Semester Region Learning Area Teaching Date Teachers Department HeadDocument3 pagesI. Objectives: Grade Level Quarter Semester Region Learning Area Teaching Date Teachers Department HeadNico Gil GonzalesNo ratings yet
- Nutrition Lesson Plan-1Document5 pagesNutrition Lesson Plan-1api-357196634No ratings yet
- Niki Credit SeminarDocument32 pagesNiki Credit SeminarJasmin OotyNo ratings yet
- Revised Syllabus of Everyday Science PDFDocument6 pagesRevised Syllabus of Everyday Science PDFAadilIftikhar67% (3)