Professional Documents
Culture Documents
13 Oral Manifestations
Uploaded by
Arantza ArantzaCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
13 Oral Manifestations
Uploaded by
Arantza ArantzaCopyright:
Available Formats
HIV Curriculum for the Health Professional
Oral Manifestations of HIV Infection
Nicoleta Vaseliu, DDS, MS, OMFS
Harrison Kamiru, BDS, MS, DrPH
Mark Kabue, BDS, MS, MPH, DrPH
Objectives
1. Discuss the importance of oral and dental care
for patients with human immunodeficiency virus
(HIV) infection.
2. Review the classification of orofacial lesions
associated with HIV infection in adults and
children.
3. Describe the clinical presentation and
management of the most common oral
manifestations of HIV infection.
Key Points
1. Oral health care is an important part of HIV
primary care.
2. Oral manifestations are common clinical findings
in children and adults with HIV infection.
3. Early diagnosis and management of oral mani
festations is important to prevent complications
and improve quality of life.
Importance of Oral Manifesta
tions of HIV Infection
Since human immunodeficiency virus (HIV) infection
was first described in 1981, a variety of oral conditions
associated with HIV disease have been documented.
Studies have shown that 70%-90% of HIV-infected
individuals will develop at least one oral manifestation
during the course of the disease. A review of the dental
literature shows that HIV-associated orofacial lesions
have been considered
clinical indicators of HIV infection in otherwise
healthy, undiagnosed individuals;
early clinical features of HIV infection;
clinical markers for the classification and staging of
HIV disease; and
predictors of HIV disease progression.
In developed countries, HIV disease progression is
monitored by two key laboratory markers: CD4+ lympho
cyte count and HIV viral load. Unfortunately, these tests
are not readily available in many developing countries.
There, other important clinical findings guide clinicians
in the evaluation and treatment of HIV disease. Because
the oral cavity is easily accessible to clinical examination,
orofacial lesions associated with HIV infection may be
used as clinical markers of HIV disease progression.
The advent of highly active antiretroviral therapy
(HAART) in 1996 greatly reduced the mortality and
morbidity of HIV-infected patients who have access to
treatment. The incidence rates of many opportunistic
infections associated with HIV disease have decreased,
including that of HIV-associated orofacial lesions.
Evaluation of oral health status is an important part
of routine health care. A thorough oral examination is
important at every stage in the management of HIV
disease. It is also desirable to encourage collaboration
among general medical practitioners, infectiousdisease doctors, general and pediatric dentists, and oral
pathologists to provide the best care possible for HIVinfected patients.
Classification of Orofacial Lesions
Associated with HIV
There are two main classification systems of oral lesions
associated with HIV infection. The first is based on the
etiology of the oral lesions. According to this system,
orofacial lesions are classified as bacterial, viral, or fungal
infections or as neoplastic lesions or other conditions.
The second, more widely used, systemrecommended
by the EC Clearinghouse on Oral Problems Related to
HIV Infection and WHO Collaborating Centre on Oral
Manifestations of the Human Immunodeficiency Virus
classifies orofacial lesions into three groups according
to the degree of their association with HIV infection.
184
184
Oral Manifestations of HIV Infection
Tables 1 and 2 show this classification of orofacial
lesions associated with HIV/AIDS in adults and children,
respectively.
Clinical Presentation and
Management
Oral Candidiasis
Oral candidiasis is the most common orofacial manifes
tation of HIV infection. Its prevalence may depend on
study population, diagnostic criteria, study design, and
availability of antiretroviral therapy. Reported prevalence
rates have varied widely, to as high as 72% in children
and 94% in adults. Oral candidiasis is also a significant
predictor of HIV disease progression in both adults and
children. The median time of survival from its clinical
diagnosis to death is 3.4 years among HIV-infected
children. The main etiologic factor of oral candidiasis is
the fungus Candida albicans, although other species of
Candida may be involved.
Clinical appearance. Oral candidiasis is often observed
in one of the following four clinical forms: erythematous
(atrophic) candidiasis, pseudomembranous candidiasis,
hyperplastic candidiasis, and angular cheilitis.
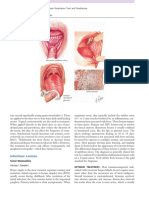
1. Erythematous (atrophic) candidiasis appears
clinically as multiple small or large patches, most
often localized on the tongue and/or palate
(Figure 1).
2. Pseudomembranous candidiasis (oral thrush)
is characterized by the presence of multiple
superficial, creamy white plaques that can be
easily wiped off, revealing an erythematous base
(Figure 2). They are usually located on the buccal
mucosa, oropharynx, and/or dorsal face of the
tongue.
3. Hyperplastic candidiasis lesions appear white and
hyperplastic and cannot be removed by scraping.
This form of oral candidiasis is rare in HIVinfected individuals.
Table 1. Orofacial lesions associated with HIV/AIDS in adults
Lesions strongly associated with HIV infection
Candidiasis
Erythematous
Pseudomembranous
Hairy leukoplakia
Kaposis sarcoma
Lesions less commonly associated with HIV infection
Non-Hodgkins lymphoma
Periodontal disease
Linear gingival erythema
Necrotizing (ulcerative) gingivitis
Necrotizing (ulcerative) periodontitis
Bacterial infections
Mycobacterium avium-intracellulare
Mycobacterium tuberculosis
Melanotic hyperpigmentation
Necrotizing (ulcerative) stomatitis
Salivary gland disease
Dry mouth due to decreased salivary flow rate
Unilateral or bilateral swelling of the major
salivary glands
Thrombocytopenic purpura
Ulceration NOS (not otherwise specified)
Lesions seen in HIV infection
Viral infections
Herpes simplex virus
Human papillomavirus (wart-like lesions)
Condyloma acuminatum
Focal epithelial hyperplasia
Verruca vulgaris
Varicella zoster virus
Herpes zoster
Varicella
Fungal infection other than candidiasis
Cryptococcus neoformans
Geotrichum candidum
Histoplasma capsulatum
Mucoraceae (mucormycosis/ zygomycosis)
Aspergillus flavus
Recurrent aphthous stomatitis
Viral infections
Cytomegalovirus
Molluscum contagiosum
1
2
Bacterial infections
Actinomyces Israel
Escherichia coli
Klebsiella pneumoniae
Cat-scratch disease
Drug reactions (ulcerative, erythema multiforme,
lichenoid, toxic epidermolysis
Epithelioid (bacillary) angiomatosis
Neurologic disturbances
Facial palsy
Trigeminal neuralgia
185
HIV Curriculum for the Health Professional
Figure 1. Erythematous candidiasis in an HIV-infected child
Figure 2. Pseudomembranous candidiasis in an HIV-infected child
4. Angular cheilitis is characterized by the presence
of erythematous fissures at the corners of the
mouth. It is usually accompanied by another form
of intraoral candidiasis.
presence of OHL is a sign of severe immunosuppression.
OHL is a significant predictor of HIV disease progression
in adults. Although its etiology is not clear, OHL seems to
be caused by Epstein-Barr virus infection.
Treatment. Treatment with topical and systemic
antifungal agents is recommended (Table 3).
Clinical appearance. OHL presents as white, thick
patches that do not wipe away and that may exhibit
vertical corrugations with a hairlike appearance (Figure
3). The lesions usually start on the lateral margins
of the tongue and sometimes inside the cheeks and
lower lip. They may be unilateral or bilateral, and they
are asymptomatic. OHL is often associated with oral
candidiasis.
Oral Hairy Leukoplakia
Oral hairy leukoplakia (OHL) is more common among
HIV-infected adults than among HIV-infected children.
The reported prevalence of OHL in adults is about 20%25%, increasing as the CD4+ lymphocyte count decreases,
whereas in children the prevalence is about 2%-3%. The
Table 2. Orofacial lesions associated with pediatric HIV infection
Lesions commonly associated with pediatric HIV infection
Oral candidiasis
Pseudomembranous
Erythematous
Angular cheilitis
Herpes simplex virus infection
Linear gingival erythema
Parotid enlargement (swelling of the major salivary glands)
Recurrent aphthous ulcers
Minor
Major
Herpetiform
Lesions less commonly associated with pediatric HIV infection
Bacterial infections of oral tissues
Periodontal diseases
Necrotizing ulcerative gingivitis
Necrotizing ulcerative periodontitis
Necrotizing stomatitis
Xerostomia
Seborrheic dermatitis
Viral infections
Cytomegalovirus
Human papillomavirus
Molluscum contagiosum
Varicella zoster virus
Herpes zoster
Varicella
Lesions strongly associated with HIV infection but rare in children
Neoplasms
Kaposis sarcoma and non-Hodgkins lymphoma
Oral hairy leukoplakia
Tuberculosis-related ulcers
186
Oral Manifestations of HIV Infection
Figure 3. Oral Hairy Leukoplakia in an HIV-infected adult
Figure 4. Linear Gingival Erythema in an HIV-infected adult
Treatment. OHL usually does not require any treatment,
but in severe cases systemic antivirals are recommended
(Table 3). When OHL is associated with oral candidiasis,
therapeutic management of oral candidiasis is required.
erythema on the attached gingiva and oral
mucosa (Figure 4). The degree of erythema is
disproportionately intense compared with the
amount of plaque present on the teeth.
2. NUG is more common in adults than in
children. It is characterized by the presence of
ulceration, sloughing, and necrosis of one or
more interdental papillae, accompanied by pain,
bleeding, and fetid halitosis.
3. NUP is characterized by the extensive and rapid
loss of soft tissue and teeth.
4. Necrotizing stomatitis is thought to be a con
sequence of severe, untreated NUP. It is charac
terized by acute and painful ulceronecrotic
lesions on the oral mucosa that expose underlying
alveolar bone.
HIV-Associated Periodontal Disease
Periodontal (gum) disease is common among HIVinfected patients. It is characterized by bleeding gums,
bad breath, pain/discomfort, mobile teeth, and some
times sores. Its reported prevalence ranges widely,
between 0% and 50%. Left untreated, HIV-associated
periodontal disease may progress to life-threatening
infections, such as Ludwigs angina and noma (cancrum
oris).
Clinical appearance. Four forms of HIV-associated
periodontal disease have been described: linear
gingival erythema, necrotizing ulcerative gingivitis
(NUG), necrotizing ulcerative periodontitis (NUP), and
necrotizing stomatitis.
1. Linear gingival erythema is characterized by
the presence of a 2- to 3-mm red band along
the marginal gingiva, associated with diffuse
Treatment. Management and control of HIV-associated
periodontal disease begin with good daily oral hygiene.
In addition to brushing, flossing and use of mouthwash
solutions are effective ways to prevent and control
periodontal disease. Table 3 presents various therapeutic
options.
Figure 5. Recurrent Herpes Simplex in an HIV-infected child
Figure 6. Recurrent minor Aphthous Ulcers in an HIV-infected adult
187
HIV Curriculum for the Health Professional
Table 3. Therapeutic options for the most common HIV-associated oral manifestations23,34,35,36,37
Oral Lesion
Treatment for Adults
Treatment for Children
Comments
Oral
Topical
Topical
Candidiasis
Nystatin (Mycostatin) Nystatin suspension 200,000-
(Erythematous,
Oral gel: apply gel q8h 400,000 U/day divided in 4-6 doses,
Pseudomembranous, or q6h, for 10-14 days for 14 days
and Hyperplastic) Cream: Apply q12h, for Clotrimazole troches 10 mg q8h or
10-14 days q6h, for 4 weeks
Gentian violet 1% aqueous solution
Systemic painted in the affected areas q8h
Nystatin (Mycostatin) antifungal agents are administered
400,000-600,000 U q6h,
for 14 days
Systemic
Ketoconazole (Nizoral) Ketoconazole 3.5-6.6 mg/kg/day in
200-400 mg PO q.d. a single dose
Fluconazole (Diflucan) Fluconazole 6 mg/kg on day 1, then
50-100 mg PO q.d. 3 mg/kg qd, up to 2 weeks
Itraconazole (Sporanox) Itraconazole 100 mg PO, daily for
(Capsules or solution) children older than 3 years
200 mg PO qd for 7 days
Amphotericin B10 mg Prophylaxis
IVq6h, for 10 days
Clotrimazole 10 mg PO q8h or
q12h for long period
Prophylaxis
Nystatin 100,000-400,000 U PO
Fluconazole 100 mg q12h for long period
PO qwk, for long period Fluconazole 3-6 mg/kg PO daily or
weekly for long period
Different forms of oral candidiasis
may occur simultaneously.
Hyperplastic candidiasis requires
systemic treatment.
Ketoconazole may interact with
Lopinavir-Ritonavir (Kaletra) at
doses >200 mg/day.
Topical fluoride should be used if
for long periods to counteract high
sugar content of some antifungal
medications.
Amphotericin B may be used in
azole-resistant infections.
Amphotericin B may also be
available as a topical preparation.
Dentures should be removed when
medication is applied.
Angular
Topical
Topical
Cheilitis
Nystatin-triamcinolone Nystatin-triamcinolone (Mycolog II)
(Mycolog II) ointment ointment applied on the affected
applied on the affected areas after meals and at bedtime
areas after meals and
Clotrimazole 1% (Mycelex) cream
at bedtime
Miconazole 2% cream applied q12h
Clotrimazole 1% on the affected areas, for 1-2 weeks
(Mycelex) cream
Miconazole 2% cream
applied q12h on the
affected areas, for 1-2
weeks
Herpes Simplex
Systemic
Systemic
Virus (HSV)
Acyclovir (Zovirax)
Acyclovir 10 mg/kg PO q4h or q6h
Infection 800 mg PO q4h,
Acyclovir 10 mg/kg IV q8h
for 10 days
Foscarnet 24-40 mg/kg PO q8h, for
Foscarnet 24-40 mg/kg resistant herpetic lesions
PO q8h, for resistant
herpetic lesions
Linear Gingival
Local
Local
Erythema
Scaling and root planing Scaling and root planing
(LGE)
0.12% Chlorhexidine
0.12% Chlorhexidine gluconate
gluconate (Periogard, (Periogard, Peridex) 0.5 oz q12h
Peridex) 0.5 oz q12h rinse, for 30 sec. and spit
rinse, for 30 sec. and spit
Lesions tend to heal slowly
because of the repeated opening
of the mouth.
Ganciclovir, Valacyclovir and
Famciclovir are probably effective.
Foscarnet is the drug of choice for
Acyclovir-resistant cases.
Patients taking Acyclovir should
be instructed to drink plenty of
fluids.
Topical antiviral medications may
be used for labial and perioral
herpetic lesions.
Prophylaxis is recommended:
brushing, flossing, and use of
mouth rinses.
Antifungal agents may be useful in
the treatment of LGE.
Continued on next page
188
Oral Manifestations of HIV Infection
Table 3. Therapeutic options for the most common HIV-associated oral manifestations23,34,35,36,37 (continued)
Oral Lesion
Treatment for Adults Treatment for Children
Comments
Linear Gingival
Local
Local
Prophylaxis is recommended:
Erythema
Scaling and root planing Scaling and root planing brushing, flossing, and use of
(LGE)
0.12% Chlorhexidine
0.12% Chlorhexidine gluconate mouth rinses.
gluconate (Periogard, (Periogard, Peridex) 0.5 oz q12h
Antifungal agents may be useful in
Peridex) 0.5 oz q12h rinse, for 30 sec. and spit the treatment of LGE.
rinse, for 30 sec. and spit
Xerostomia
Topical
Topical
Good oral hygiene measures and
Chewing or sucking
Chewing or sucking sugarless candy diet control (control of sugar and
sugarless candy
Frequent sips of water sugary foods) are recommended
Frequent sips of water Commercial artificial saliva to prevent dental caries.
Commercial artificial substitutes
Mouth rinses with high alcohol
saliva substitutes
Topical fluoride products content should be avoided due to
Topical fluoride products drying effect.
Systemic
Pilocarpine (Salagen)
5 mg PO q8h before
meals; it may increase
to 7.5 mg PO q8h
Parotid
Systemic
Enlargement (of
Non-steroidal
major salivary anti-inflammatories
glands)
Analgesics
Antibiotics
Steroids
Systemic
Surgical removal of the parotid
Non-steroidal anti-inflammatories gland may be necessary for
Analgesics esthetic reasons.
Antibiotics
Steroids
Oral Hairy
Local
Local
Recurrence often occurs after the
Leukoplakia (OHL) Podophyllin resin
Podophyllin resin 25% 1-2 applica- treatment is discontinued.
25% 1-2 applications tions on the affected areas, at
OHL is rare in children.
on the affected areas, at 1 week apart Symptomatic and extensive lesions
1 week apart
Retinoic acid (Tretinoin) may require topical treatment.
Retinoic acid (Tretinoin) Surgical excision
OHL has been shown to disappear
Surgical excision in patients receiving zidovudine
(AZT).
Systemic
Acyclovir (Zovirax)
800 mg PO q4h or q6h,
for 14 days
Famciclovir 500 mg PO
q8h, for 5-10 days
Valacyclovir 1000 mg
PO q8h, for 5-10 days
Necrotizing
Local
Local
Prolonged use of chlorhexidine
Ulcerative
Debridement of
Debridement of affected areas may cause staining of teeth,
Gingivitis (NUG), affected areas
Irrigation with povidon-iodine tongue, and restorations; taste
Irrigation with povidon- (10% Betadine) alteration; and mucosal
Necrotizing iodine (10% Betadine) 0.12% chlorhexidine gluconate desquamation and irritation.
Ulcerative
0.12% chlorhexidine (Peridex, Periogard) mouth rinse
Metronidazole should not be
Periodontitis (NUP), gluconate (Peridex, q12h given to patients taking
Periogard) mouth rinse didanosine (ddI) or zalcitabine
Necrotizing q12h (ddC), because it may potentiate
Stomatitis (NS) peripheral neuropathy.
Continued on next page
189
HIV Curriculum for the Health Professional
Table 3. Therapeutic options for the most common HIV-associated oral manifestations23,34,35,36,37 (concluded)
Oral Lesion
Treatment for Adults
Treatment for Children
Comments
Necrotizing
Systemic
Systemic
(See chart on previous page)
Ulcerative
Metronidazole (Flagyl) Metronidazole (Flagyl) 15-35 mg/kg
Gingivitis (NUG), 250 mg PO q8h or PO q8h, for 7-10 days
500 mg q12h, for 7-10 days Clindamycin (Cleocin) 20-30 mg/kg
Necrotizing
Clindamycin (Cleocin) PO q6h, for 7 days
Ulcerative
150 mg PO q6h or
Amoxicillin clavulanate (Augmentin)
Periodontitis (NUP), 300 mg PO q8h, for 7 days 40 mg/kg PO q8h, for 7 days
Amoxicillin clavulanate
Necrotizing (Augmentin) 250 mg PO
Stomatitis (NS) q12h, for 7 days
Oral Ulcers
Topical
Topical
Major aphthous ulcers usually
(Recurrent
Triamcinolone in
Triamcinolone in Carboxymethyl- require systemic steroids.
Aphthous Ulcers) Carboxymethylcellulose cellulose 0.1% paste applied in a
Aphthous ulcers may be exacebated
0.1% paste thin layer q6h daily by stress.
Betamethasone
Betamethasone phosphate:
Iron, vitamin B12, and folate
phosphate: 0.5 mg tablet dissolved in 10 ml deficiencies should be ruled out.
0.5 mg tablet dissolved mouthwash and rinse q4h
Dexamethasone elixir should be
in 10 ml mouthwash spray on ulcer (1 spray = 100 g) used for multiple ulcers or ulcers
and rinse q4h up to 800 g not accessible for topical applica-
spray on ulcer (1 spray Fluocinonide (Lidex) 0.05% tion.
= 100 g) up to 800 g ointment q4h
Thalidomide is indicated only
Fluocinonide (Lidex)
Dexamethasone elixir (0.5 mg/5ml) when recurrences are severe
0.05% ointment applied rinse and expectorate and frequent.
on ulcer q4h
The treatment with Thalidomide
Dexamethasone elixir
Systemic should be monitored thoroughly
(0.5 mg/5ml) rinse and Prednisone 2 mg/kg q6h, for 5-7 due to its teratogenicity. Birth
expectorate days with gradual tapering control measures are required.
Systemic
Prednisone starting at
30-40 mg PO daily with
taper over 1 month for
severe disease resistant
to topical agents
Thalidomide 200 mg PO
daily
Oral Warts
Topical
Topical
The recurrence rate is high.
Podophyllin resin 25% Podophyllin resin 25% applications Concurrent therapeutic approaches
applications q6h for q6h for long period should be considered.
long period
Surgical excision
Surgical excision
Laser ablation
Laser ablation
Cryotherapy
Cryotherapy
Systemic
Cimetidine (Tagamet)
600 mg PO q6h, for long
period (months)
Interferon alfan3 SC/IM
3,000,000 U (1 ml) qwk,
for several weeks
Abbreviations used in Table 3: PO = per os (by mouth); IV = intravenous; qd = every day; qwk = every week; q2h = every two hours;
q4h = every four hours; q6h = every six hours; q8h = every 8 hours; q12h = every 12 hours.
190
Oral Manifestations of HIV Infection
Noma, also known as cancrum oris, is a gangrenous
condition that affects primarily children. Noma has been
reported mainly in developing countries in West Africa,
but cases have also been described in other parts of the
world. It is a multifactorial disease. The most important
risk factors are poverty, chronic malnutrition, poor
oral hygiene, and severe immunosuppression. Though
considered a preventable disease, noma has a case fatality
rate of 70%-90% if left untreated.
aphthous ulcers occur as a crop of many small lesions (1-2
mm) disseminated on the soft palate, tonsils, tongue,
and/or buccal mucosa.
Herpes Simplex Virus Infection
Parotid enlargement is commonly associated with HIV
infection in children (10%-30%) and less commonly in
adults. It occurs in the late course of HIV infection and is
associated with a slower rate of HIV disease progression.
The median time from its diagnosis to death has been
reported to be 5.4 years among HIV-infected children.
Lymphocytic infiltration of the salivary glands may be an
etiologic factor.
Herpes simplex virus (HSV) infection may be either
primary (herpetic gingivostomatitis) or secondary
(herpes labialis). The prevalence of oral HSV infection
varies between 10% and 35% in HIV-infected adults and
children. The presence of HSV infection for more than 1
month constitutes an AIDS-defining condition.
Clinical appearance. HSV infection appears as a crop
of vesicles usually localized on the keratinized mucosa
(hard palate, gingiva) and/or vermillion borders of the
lips and perioral skin (Figure 5). The vesicles rupture and
form irregular painful ulcers. They may interfere with
mastication and swallowing, resulting in decreased oral
intake and dehydration.
Treatment. Systemic therapy with antiviral agents is
recommended (Table 3). The treatment is more effective
if it is instituted in the prodromal stage of infection.
Recurrent Aphthous Ulcers
Recurrent aphthous ulcers (RAUs) occur in about 1%-7%
of HIV-infected patients. They are painful ulcers on the
nonkeratinized oral mucosa, such as labial and buccal
mucosa, soft palate, and ventral aspect of the tongue.
Severe recurrent aphthous lesions usually occur when
the CD4+ lymphocyte count is less than 100 cells/L. This
result may be suggestive of HIV disease progression. The
etiology of RAUs is not well known.
Clinical appearance. RAUs may present as minor, major,
or herpetiform aphthae. Minor aphthous ulcers are ulcers
less than 5 mm in diameter covered by pseudomembrane
and surrounded by an erythematous halo. They usually
heal spontaneously without scarring (Figure 6). Major
aphthous ulcers resemble minor aphthous ulcers, but
they are fewer and larger in diameter (1-3 cm), are more
painful, and may persist longer. Their presence interferes
with mastication, swallowing, and speaking. Healing
occurs over 2-6 weeks. Scarring is common. Herpetiform
Treatment. The first line of management of RAUs is pain
control and prevention of superinfection. Depending on
the severity of the ulcers, topical and/or systemic steroid
agents are recommended (Table 3).
Parotid Enlargement and Xerostomia
Clinical appearance. Parotid enlargement occurs as
unilateral or bilateral swelling of the parotid glands.
It is usually asymptomatic and may be accompanied
by decreased salivary flow (xerostomia or dry mouth).
Problems with dry mouth in HIV-infected patients
are often caused by medications that interfere with
salivary secretion, such as antihistamines, antianxiety
medications, antidepressants, and some antiretroviral
drugs (didanosine and zalcitabine).
Treatment. Treatment is required only in severe
cases and may consist of systemic analgesics, antiinflammatories, antibiotics, and/or steroids (Table 3).
Human Papillomavirus Infection (Oral Warts)
The incidence of oral warts due to human papillomavirus
infection has increased dramatically since the era of
HAART. The lesions are more prevalent in adults (1%-4%
of cases) than in children.
Clinical appearance. Oral warts may appear cauliflowerlike, spiked, or raised with a flat surface. They are
asymptomatic. The most common location is the
labial and buccal mucosa. The most common clinical
presentation is multifocal flat lesions resembling focal
epithelial hyperplasia (Hecks disease).
Treatment. Treatment may be required for patients with
multiple lesions. Topical and systemic agents and various
surgical approaches are available (Table 3).
191
HIV Curriculum for the Health Professional
General Management
Considerations
To prevent the need for expensive dental services, it
is imperative to treat the oral manifestations of HIV
infection at all levels of care. Personal oral hygiene
practices, such as tooth brushing and use of interdental
cleaning aids, are the most effective ways of maintaining
good oral health.
At the primary level of oral care, prevention of oral
diseases takes priority. Prevention involves improving
oral hygiene awareness through health education at the
individual and community levels. Oral health education
messages should be made visible in all community
forums. Home-based care providers should undergo
training in basic oral hygiene practices so that they
can impart these to patients under their care. Use of
simple materials such as warm salty mouth rinse or
commercial mouthwash (chlorhexidine) can improve
basic oral hygiene cost-effectively. Patients whose manual
dexterity is intact should be taught appropriate brushing
techniques. Other adjuvant oral hygiene methods, such as
flossing and use of interdental toothbrushes, will depend
on the availability and affordability of supplies.
The secondary level of oral care involves visits to clinical
care facilities. Depending on local resources, the health
cadre available at this level may range from nursing
staff at a health center to primary care physicians. In
some countries, health centers may have no oral health
personnel or may offer only relief of pain with analgesics
and extractions. Health care workers at this level should
be trained to recognize suspicious lesions that may be
oral manifestations of HIV infection, and they should
know when and where to refer patients to a higher level
of oral care.
At the tertiary level of oral care, a dentist should be
available to make definitive diagnoses of oral lesions and
provide professional oral services such as prophylaxis,
restorations, biopsies, and the prescription of appropriate
medication.
Acknowledgment
We thank Professor Sudeshi Naidoo, Department of
Community Dentistry, Faculty of Dentistry and WHO
Collaborating Centre, University of the Western Cape,
South Africa, for providing the pictures of oral lesions
used in this chapter.
References
1. Arendorf TM, Bredekamp B, Cloete CAC, et al. Oral
manifestations of HIV infection in 600 South African
patients. J. Oral Pathol. Med. 1998;27:176-179.
2. Winfert M, Grimes RM, Lynch DP. Oral
manifestations of HIV infection. Ann. Intern. Med.
1996;125:485-496.
3. Kamiru HN, Naidoo S. Oral HIV lesions and oral
health behaviour of HIV positive patients attending
Queen Elizabeth II Hospital, Maseru, Lesotho. SADJ
2002;57:479-482.
4. Patton LL, Phelan JA, Ramos-Gomez FJ, et al.
Prevalence and classification of HIV-associated oral
lesions. Oral Dis. 2002;8(Suppl 2):98-109.
5. Chapple ILC, Rout PJ, Basu MK. Gingival Kaposis
sarcoma: the first indication of HIV infection. Dent.
Update 1992;19:296-301.
6. Klein RS, Harris CA, Small CB, et al. Oral candidiasis
in high-risk patients as the initial manifestations of
the acquired immunodeficiency syndrome. N. Engl. J.
Med. 1984;311:354-358.
7. Centers for Disease Control and Prevention. 1993
revised classification system for HIV infection and
expanded surveillance case definition for AIDS
among adolescents and adults. MMWR Recomm. Rep.
1993;41(RR-17):1-19.
8. Ramos-Gomez FJ, Petru A, Hilton JF. Oral
manifestations and dental status in paediatric HIV
infection. Int. J. Paediatr. Dent. 2000;10:3-11.
9. Magalhaes GM, Bueno DF, Serra E. Oral
manifestations of HIV positive children. J. Clin.
Pediatr. Dent. 2001;25:103-106.
10. Nicolatou O, Theodoridou M, Mostrou G. Oral
lesions in children with perinatally acquired
immunodeficiency virus infection. J. Oral Pathol.
Med. 1999;28:49-53.
11. Begg MD, Lamster IB, Panageas KS. A prospective
study of oral lesions and their predictive value for
progression of HIV disease. Oral Dis. 1997;3:176183.
12. Chapple ILC, Hamburger J. The significance of oral
health in HIV disease. Sex Transm. Inf. 2000;76:236243.
13. Katz MH, Mastrucci T, Leggott PJ, et al. Prognostic
significance of oral lesions in children with
perinatally acquired human immunodeficiency virus
infection. Am. J. Dis. Child. 1993;147:45-48.
192
Oral Manifestations of HIV Infection
14. Barasch A, Safford MM, Catalanotto FA, et al. Oral
soft tissue manifestations in HIV-positive vs. HIVnegative children from an inner city population:
a two-year observational study. Pediatr. Dent.
2000;22:215-220.
15. Schmidt-Westhausen AM, Priepke F, Bergmann FJ, et
al. Decline in the rate of oral opportunistic infections
following introduction of highly active antiretroviral
therapy. J. Oral Pathol. Med. 2000;29:336-341.
16. Darbyshire J. Therapeutic interventions in HIV
infectiona critical review. Trop. Med. Int. Health
2000;5:A26-A31.
17. Scully C, Diz Dios P. Orofacial effects of antiretroviral
therapies. Oral Dis. 2001;7:205-210.
18. Royce RA, Luckman RS, Fusaro RE, et al. The natural
history of HIV-1 infection: staging classifications of
disease. AIDS 1991;5:355-364.
19. EC Clearinghouse on Oral Problems Related to HIV
Infection and WHO Collaborating Centre on Oral
Manifestations of the Human Immunodeficiency
Virus. An update of the classification and diagnostic
criteria of oral lesions in HIV infection. J. Oral Pathol.
Med. 1991;20:97-100.
20. EC Clearinghouse on Oral Problems Related to HIV
Infection and WHO Collaborating Centre on Oral
Manifestations of the Human Immunodeficiency
Virus. Classification and diagnostic criteria for
oral lesions in HIV infection. J. Oral Pathol. Med.
1993;22:289-291.
21. Ramos-Gomez FJ, Flaitz CM, Catapano P, et al.;
Collaborative Workgroup on Oral Manifestations
of Pediatric HIV Infection, Oral AIDS Center,
University of California, San Francisco, San
Francisco, California. Classification, diagnostic
criteria, and treatment recommendations for
orofacial manifestations in HIV-infected pediatric
patients. J. Clin. Pediatr. Dent. 1999;23:85-96.
22. Kline MW. Oral manifestations of pediatric human
immunodeficiency HIV infection: a review of the
literature. Pediatrics 1996;97:380-388.
23. Kline MW. Cutaneous and oral manifestations of
pediatric HIV infection. In Pizzo PA & Wilfert CM
(Eds.): Pediatric AIDS: The Challenge of HIV Infection in
Infants, Children, and Adolescents. 3rd ed. Baltimore:
Williams & Wilkins, 1998.
193
24. Flaitz CM, Hicks MJ. Oral manifestations in
pediatric HIV infection. In: Shearer WT & Hanson
CI (Eds.): Medical Management of AIDS in Children.
Philadelphia: Saunders, 2003.
25. Schiodt M, Pindborg JJ. AIDS and the oral cavity:
epidemiology and oral manifestations of HIV
infection: a review. Int. J. Oral Maxillofac. Surg.
1987;16:1-14.
26. Ramos-Gomez FJ, Hilton JF, Canchola AJ, et
al. Risk factors for HIV-related orofacial softtissue manifestations in children. J. Pediatr. Dent.
1996;18:121-126.
27. Walling DM. Oral hairy leukoplakia: an Epstein-Barr
virus-associated disease of patients with HIV. Res.
Initiat. Treat Action 2000;6:10-15.
28. Lifson AR, Hilton JF, Westenhouse JL, et al. Time
from seroconversion to oral candidiasis or hairy
leukoplakia among homosexual and bisexual
men enrolled in three prospective cohorts. AIDS
1994;8:73-79.
29. Berthold P. Noma: a forgotten disease. Dent. Clin. N.
Am. 2003;47:559-574.
30. Enwonwu CO, Falkler WA, Idigbe EO, et al. Noma
(cancrum oris): questions and answers. Oral Dis.
1999;5:144-149.
31. Schiodt M. Less common oral lesions associated with
HIV infection: prevalence and classification. Oral Dis.
1997;3:S208-S213.
32. Clark PC, Flaitz CM, Nichols CM, et al. Oral human
papillomavirus infection in HIV: clinicopathologic
correlations. J. Dent. Res. 1998;77:250A.
33. Brothell DJ, Jutai DK, Hawkins RJ. An update of
mechanical oral hygiene practices: evidence-based
recommendations for disease prevention. J. Can.
Dent. Assoc. 1998;46:295-306.
34. Gage TW, Picket FA. Mosbys Dental Drug Reference.
6th ed. St. Louis: Mosby, 2003.
35. Naidoo S, Chikte U. HIV/AIDSthe evolving
pandemic and its impact on oral health in subSaharan Africa. SADJ 1999;54:661-630.
You might also like
- 10-1055-s-0034-1389562 Fracturas de Orbita PDFDocument11 pages10-1055-s-0034-1389562 Fracturas de Orbita PDFArantza ArantzaNo ratings yet
- 10-1055-s-0034-1389562 Fracturas de Orbita PDFDocument11 pages10-1055-s-0034-1389562 Fracturas de Orbita PDFArantza ArantzaNo ratings yet
- 10-1055-s-0034-1389562 Fracturas de Orbita PDFDocument11 pages10-1055-s-0034-1389562 Fracturas de Orbita PDFArantza ArantzaNo ratings yet
- VasoconstrictoresDocument8 pagesVasoconstrictoresItzel SageyNo ratings yet
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (894)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Nursing Care Plan for Mental Retardation and SchizophreniaDocument20 pagesNursing Care Plan for Mental Retardation and SchizophreniaSARITA SHARMANo ratings yet
- 2016Document45 pages2016jimmyNo ratings yet
- Jurnal Herpes PDFDocument9 pagesJurnal Herpes PDFIstianah EsNo ratings yet
- Protocol For Symptoms HomeopathyDocument17 pagesProtocol For Symptoms HomeopathyUmer Shahzad ANSERNo ratings yet
- Inflammation and Repair: 1 Elsevier Items and Derived Items © 2009 by Saunders, An Imprint of Elsevier IncDocument145 pagesInflammation and Repair: 1 Elsevier Items and Derived Items © 2009 by Saunders, An Imprint of Elsevier IncaqeelNo ratings yet
- 3 - 500 MCQs PDFDocument140 pages3 - 500 MCQs PDFmusman1947100% (1)
- Classification System For Oral Submucous FibrosisDocument6 pagesClassification System For Oral Submucous FibrosisMohamed FaizalNo ratings yet
- Behcet's DiseaseDocument21 pagesBehcet's DiseaseFazal DalalNo ratings yet
- MFD Part 2 - Oral Medicine Qs & AnswersDocument26 pagesMFD Part 2 - Oral Medicine Qs & Answerskarimelmestekawy89No ratings yet
- Drug Induced StomatitisDocument4 pagesDrug Induced StomatitisRamadhani P SalichaNo ratings yet
- Tongue DisordersDocument31 pagesTongue DisordersMaphoto Xola0% (1)
- Non-Odontogenic Tumors of The JawsDocument5 pagesNon-Odontogenic Tumors of The JawsSaman SadeghiNo ratings yet
- Muhaidat PREVALENCE OF ORAL ULCERATION AMONG JORDANIAN PEOPLEDocument8 pagesMuhaidat PREVALENCE OF ORAL ULCERATION AMONG JORDANIAN PEOPLEPutri FifiNo ratings yet
- Netter 39 S Internal Medicine 2nd Edition Pages 65, 68Document2 pagesNetter 39 S Internal Medicine 2nd Edition Pages 65, 68Burca EduardNo ratings yet
- ADC Part 1 - TG Keynotes II v1.0 PDFDocument17 pagesADC Part 1 - TG Keynotes II v1.0 PDFDrSaif Ullah KhanNo ratings yet
- Jurnal 1Document8 pagesJurnal 1Renita Mandalinta SitepuNo ratings yet
- Cancer Nursing Care PlansDocument26 pagesCancer Nursing Care PlansMildred AlidonNo ratings yet
- Mouth UlcersDocument2 pagesMouth Ulcerspadmaja84No ratings yet
- Nonspecific Genital UlcersDocument16 pagesNonspecific Genital UlcersThảo NguyễnNo ratings yet
- Ayapana Tech ReportDocument16 pagesAyapana Tech ReportnurarNo ratings yet
- Ped Exam MacqsDocument99 pagesPed Exam MacqsIvailo FartalevNo ratings yet
- Management of Erythema Multiforme Secondary To Herpes Simplex by Systemic Acyclovir and Topical Corticosteroid A Case Report 45 49 PDFDocument5 pagesManagement of Erythema Multiforme Secondary To Herpes Simplex by Systemic Acyclovir and Topical Corticosteroid A Case Report 45 49 PDFindrayaniNo ratings yet
- Oral Lesions and HomoeopathyDocument27 pagesOral Lesions and HomoeopathyDr. Rajneesh Kumar Sharma MD HomNo ratings yet
- Gingival and PeriodontalDocument57 pagesGingival and PeriodontalPhanQuangHuyNo ratings yet
- Aim4aiims - In: The EarDocument39 pagesAim4aiims - In: The EardorjeesengeNo ratings yet
- Mucoadhesive System - PPT - Vijay BhaskarDocument60 pagesMucoadhesive System - PPT - Vijay Bhaskarboddarambabu100% (2)
- Nursing Management of Oral HygieneDocument40 pagesNursing Management of Oral HygieneGrace Shabrina HapsariNo ratings yet
- Acute Gingival Infection Lecture - pdf-1251132185Document68 pagesAcute Gingival Infection Lecture - pdf-1251132185irajput 001No ratings yet
- AUS - Boardreviewer (Test Your Knowledge)Document177 pagesAUS - Boardreviewer (Test Your Knowledge)Yusra FaisalNo ratings yet
- Ulcer Sinus Fistul ADocument47 pagesUlcer Sinus Fistul AAnil BasnetNo ratings yet