Professional Documents
Culture Documents
Detection of Breathing Phases : Ivan Božić, Djordje Klisić, Andrej Savić
Uploaded by
Atika AudiniOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Detection of Breathing Phases : Ivan Božić, Djordje Klisić, Andrej Savić
Uploaded by
Atika AudiniCopyright:
Available Formats
SERBIAN JOURNAL OF ELECTRICAL ENGINEERING
Vol. 6, No. 3, December 2009, 389 - 398
UDK: 615.849:621.37]:616.24-008.4
Detection of Breathing Phases*
Ivan Boi1,a, Djordje Klisi1, Andrej Savi1
Abstract: The electrical stimulation systems, for the needs of artificial
ventilation are in the grater or lesser extent, in commercial use since 1970s.
Apart from development of new methods of stimulation and hardware solutions,
the key role in development of such systems is reliable detection of phases
during breathing. This paper gives the review of stimulation methods,
physiology of respiratory system and one of the possible solutions, proposed by
the authors.
Keywords: Functional electrical stimulation, Detection of breathing phases,
Artificial ventilation, Stimulation methods, Physiology of respiratory.
Introduction
Respiratory complications are the leading cause of illness and death in
patients with spinal cord injuries. In patients with spinal injuries in cervical
level, all four limbs are affected, resulting in tetraplegia with increased risk of
respiratory complications for nature of this injuries result also in partial or
complete paralysis of the breathing muscles. This can lead to reduction of flow
during cough, which affects the ability of cleaning the airways, leading to
increased probability of respiratory infections in patients with chronic
tetraplegia.
Physiology of Respiratory System
Because of its gas exchange function, respiratory system is one of the most
important physiological systems in human body. Gas exchange is considered
crucial for the elimination of unhealthy gases, which are produced by burning
the oxygen on the cellular level and enrichment of the blood with oxygen.
Energy for the gas exchange process is obtained by actions of two groups
of muscles, so-called inspiration and expiration muscles. Contraction of the
inspiration muscles leads to increase in tidal volume and decrease of the
pressure, so the air enters the lungs. Main muscle of inspiration is the
1
Department of Biomedical Engineering, School of Electrical Engineering, University of Belgrade, Bulevar
Kralja Aleksandra 73, 11120 Belgrade, Serbia; E-mail: aivbozic@yahoo.com
*Award for the best paper presented in Section Biomedicine, at Conference ETRAN 2009, June 15-19,
Vrnjaka Banja, Serbia.
389
I. Boi, Dj. Klisi, A. Savi
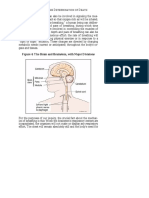
diaphragm, which provides the biggest changes in volume and pressure, of
thoracal part by its movement. When the complete breathing process is done
only by the movement of diaphragm, this kind of breathing is called quiet
breathing and it represents the normal gas exchange process, which happens
daily. Apart from diaphragm, inspiration muscles are also the external
intercostals and some neck and head muscles. Expiration muscles are mainly
inactive during quite breathing. This group of muscles is solely used during
intensive air discharges, for an example cough or sneezing. The main expiratory
muscles are abdominal muscles but the internal intercostals are also used during
expiration. Respiratory muscles are shown in Fig. 1.
Fig. 1 Respiratory muscles [10].
Neural Breathing Prothesis
For the artificial ventilation dependant patients, with injuries at C1-C2
levels, technique of phrenic nerve (which innervates the diaphragm) stimulation
is developed. This technique improves breathing function and gives patients
independence of mechanical ventilation, which automatically reduces the risk of
respiratory infections. However, this technique is often not applicable in
tetraplegic patients with injuries on levels just below C2, due to the minor
motor-neural damage of the phrenic nerve, which is innervated between third
and fourth cervical level.
390
Detection of Breathing Phases
In this case, stimulation of intercostals can be an alternative or additional
way of improvement of breathing process. Combined functions in inspiration
and expiration of the intercostals can be an obstacle in gaining satisfactory tidal
volumes by stimulating this group of muscles. In addition, both of these
methods are hard for implementation by transcutaneous techniques and require
implantable stimulation electrodes.
Patients with tetraplegia, which have lesions on lower levels, are usually
capable of voluntary breathing, and are mostly independent of mechanical
ventilation. However, their breathing capacity is further reduced due to paralysis
of inspiratory and expiratory muscles. Paralysis also affects the abdominal
muscles, which are the main expiratory muscles, and their capacity to forcefully
expire is reduced.
It was shown that stimulation of abdominal muscles during expiration can
improve respiratory function. This technique can amplify coughing, for
contraction of respiratory muscles leads to increase of respiratory pressure,
which consequently leads to increase of expiration. Stimulation of abdominal
muscles is most often used in patients that have voluntary breathing ability,
although this technique is used also in patients who cannot breathe
spontaneously. One of the great advantages of this method is that the
stimulation is performed by surface electrodes placed on the skin.
The only stimulation method (of those previously described) that is
commercially available today is phrenic nerve stimulation method, while the
other two are still in testing phase.
Although all three methods have different stimulation techniques and
stimulation regions, they have one mutual flaw the asynchronous work of the
stimulator. Disadvantage of this kind of approach is mainly in constant
parameters of stimulation, not regarding the patients momentary needs i.e.
without following physiological parameters of breathing.
Detection of Breathing Phases
Reliable detection of phases during respiratory process, by using the simple
sensors, would provide enormous amount of possibilities in projecting future
systems for artificial ventilation. Under detecting phases during breathing, it is
mainly considered expiration and inspiration, or detection of their start, end and
duration and certain characterization of these processes. In addition, it would be
useful if certain sub-phases and current events during inspiration could be
isolated (such as moment of maximum flow during expiration). Any reliable
information on these sub-phases and events would be of great importance when
designing systems that would have the role of support and assistive breathing
systems. If they would show satisfactory reliability of sensory information in
391
I. Boi, Dj. Klisi, A. Savi
the detection and prediction of these stages, the results would have great
significance for the creation of advanced automated systems that would be able
to monitor the physiological process of breathing and synchronize their work
with spontaneous respiration.
This kind of information is required when creating algorithms for such
systems and greatly contributes to their reliability and accuracy. Another
important issue in this case would be the differentiation of phenomena such as
coughing or sneezing, which are also associated with the process of breathing,
but they should be well separated from normal inspiration and expiration.
Otherwise, it could cause the wrong action of the device, thereby undermine the
process of breathing, and cause discomfort. It is also important to detect the
patients speech, because the speech itself may be treated as a phase of
breathing. Relevant fact regarding speech is that in these moments there is no
breathing, so constant stimulation during the speech led only to inconvenience
of the patient. All of the above results in ideas and motivation for research and
further advances in this field for designing comfortable (as less tying for the
patient's daily activities and easy to use), non-invasive, clinically attainable and
commercially competitive device, with simple and easily applicable sensor
systems.
Different Methods of Detection of Phases during Breathing
Currently, phase detection of the breathing process is being done only
spirometer, the device for direct measurement of the flow. All systems that use
FES to improve breathing function, for validation of their results, or possibly
synchronous stimulation are using this device. This method has the advantage of
a direct measurement of airflow, which is actually the parameter of interest,
since with it we may differ phases of speech and cough [16]. However, the
disadvantage of this device is a mask that is placed on the face, so the patient is
unable to speak or eat during measurements; also, the dimensions of the device
are not small. Therefore, there is a need for developing new techniques that
would be more mobile and gave the patient greater comfort in everyday life.
Currently, the newest research in this field include the development of
systems for the detection, which would be realized by using measurements of
blood oxygen saturation using pulse oximetre and systems based on
electromyography (EMG), i.e. electrical activity of muscles. During the last
decades, surface EMG of respiratory muscles has been used in several research
and clinical studies, both in animals and in humans [17, 18]. Monitoring
activities of diaphragm and the intercostal muscular system is one of the most
direct methods for collecting information about the function of respiratory
muscles [19]. There are also developed algorithms to detect each cycle of
breathing in experimental animals [20].
392
Detection of Breathing Phases
System for Detection of Phases during Breathing
Given all the previously mentioned, we come to the conclusion that it is
necessary to develop a system that would be as simple as possible, mobile, and
which minimally interferes with the patient during normal daily activities:
eating, talking, etc.. One possible solution is a system (Fig 2.) of three sensors
that will be explained below.
Fig. 2 Block scheme.
In order to keep the mouth of the patient free (without the mask, for
everyday use), it is impossible to apply direct measurement of the flow, so other
physiological breathing properties, which can characterize phases of breathing,
must be analyzed. Therefore three sensors are selected, where each has a task to
detect a possible phase of the breathing. For this purpose we selected pressure
sensor, thermistor - temperature sensor and microphone. Temperature sensor is
used to detect breathing, using the fact that the inhaled air is cooler than the air
exhaled. Scheme of the circuit in which thermistor is used is given in Fig. 3.
Pressure sensor is used as an indirect flow meter, that pressure and fluid
flow are related in Bernoullis equation (1):
p+
v 2
+ gh = const. ,
2
(1)
with
p Pressure;
- Fluid density; g - Gravitational acceleration;
v - Velocity of fluid; h - Distance.
In pressure measurements detection of cough or sneezing is determined by
the appearance of sudden changes of pressure, and therefore the flow, which is
typical for these situations [16]. Circuit scheme of pressure sensor, provided in
Fig. 4.
393
I. Boi, Dj. Klisi, A. Savi
Fig. 3 Circuit with thermistors.
Fig. 4 Circuits scheme with pressure meter.
394
Detection of Breathing Phases
As patient does not wear facemask, it means that it is necessary to also
detect moments of talking and block the stimulation at these moments.
Detection of speech is particularly demanding problem, because the noise
during measurement is large and comes from many different sources. Part of the
noise is the breathing itself, which may be in audible domain of the spectrum, or
any sound that does not derive from the patient, as well as cases of coughing
and sneezing. Therefore, it is necessary to make high-quality microphone
placement near the patient's mouth, and to apply quality filtration of the signal
with proper band selection before further use. Particular attention should be paid
to the fact that occurrence of signal on the microphone, does not necessarily
point to the existence of speech, so results of the pressure measurements should
be considered first to determine that there has been no occurrence of coughing.
Circuit scheme with the microphone is given in Fig. 5.
Fig. 5 Circuit with microphone.
Results
Results obtained using the described hardware is shown in Fig. 6.
Recordings were made on the healthy subject with the ability of spontaneous
breathing
Signals shown in Fig. 6 are signals recorded during breathing using a
pressure sensor, thermistors and microphone. In the picture are also presented
the moments in which the subject speaks (thick black line on the x-axis) and the
moments in which the subject coughs (thick gray line on x-axis). The rest of the
recorded sequence is normal breathing. Figure shows that the thermistor and
pressure signals are in phase during breathing, due to the fact that the
395
I. Boi, Dj. Klisi, A. Savi
temperature and pressure increase with expiration and decrease during
inspiration. During the speech, as expected, there is no breathing, and cough
occurs after the sudden change in pressure. Based on all parameters, there is a
very easy way to make the difference between each phase of breathing, which is
also shown.
Fig. 6 Results recorded from all three sensors during breathing.
Fig. 7 The differences in pressure during coughing.
396
Detection of Breathing Phases
Fig. 7 presents only signals from the thermistors and pressure sensor in
order to see more clearly the changes of pressure at the time of cough initiation
(fields marked with black spot on top of the figure). The signal from the
thermistors is represented in blue and pressure with green line.
Conclusion
In the case of spinal cord injury leading to the loss of respiratory function it
is extremely important to ensure normal functioning of the breathing process.
Studies have shown that life after injury lasts to three times longer than in the
case when the breathing process isnt supported. Currently, the main part of the
research in the area of developing systems for the stimulation of the respiratory
muscles is related to the detection and recognition of phases during breathing.
The results show that the complete detection of breathing can be done using
simple sensors, easy to use and small in size and weight. System of this kind
would be minimally intrusive and would allow easier patient adjustment.
Quality of detection is very good, errors are rare, and new solutions in the
implementation could further increase the reliability and applicability of such a
system. With well-selected pressure threshold, the system can, without any
problems detect coughing and sneezing. Errors may occur (although rarely)
during the speech and immediately after coughing, but they are short and
quickly corrected (not a single case in which missed more than one pulse in the
series noticed). Probably the most important characteristics of this system is that
it does not include measurements on the patients mouth, which allows normal
speech, food and water intake that would significantly improve the life quality
of its eventual users.
Further development of the system includes integration, minimization and
preparation of mask which will carry sensors without obstruction of the mouth,
and testing of the system on real patients.
Acknowledgment
The authors would like to thank Dr. D.B. Popovi, Chairman and Professor,
Department of Biomedical Engineering, Faculty of Electrical Engineering,
University of Belgrade, Belgrade, Serbia, and BMIT group for suggestions and
help in editing the final version of the manuscript.
10 References
[1]
[2]
D.D. Cardenas, J.M. Hoffman, S. Kirshblum, W.O. McKinley: Etiology and Incidence of
Rehospitalization after Traumatic Spinal Cord Injury: A Multicenter Analysis, Archives of
Physical Medicine and Rehabilitation, Vol. 85, No. 11, Nov. 2004, pp. 1757 1763.
W.O. McKinley, A.B. Jackson, D.D. Cardenas, M.J. DeVivo: Long-term Medical
Complications after Traumatic Spinal Cord Injury: A Regional Model System Analysis,
Archives of Physical Medicine and Rehabilitation, Vol. 80, No. 11, Nov. 1999, pp. 1402 1410.
397
I. Boi, Dj. Klisi, A. Savi
[3]
[4]
[5]
[6]
[7]
[8]
[9]
[10]
[11]
[12]
[13]
[14]
[15]
[16]
[17]
[18]
[19]
[20]
M.J. DeVivo, J.S. Krause, D.P. Lammertse: Recent Trends in Mortality and Causes of Death
among Persons with Spinal Cord Injury, Archives of Physical Medicine and Rehabilitation,
Vol. 80, No. 11, Nov. 1999, pp. 1411 1419.
A.Y. Wang, R.J. Jaeger, G.M. Yarkony, R.M. Turba: Cough in Spinal Cord Injured Patients:
The Relationship between Motor Level and Peak Expiratory Flow, Spinal Cord, Vol. 35,
No. 5, May 1997, pp. 299 302.
D.M. Mitrovic: Osnovi fiziologije, Paral, Belgrade, 2002.
G.H. Creasey, J. Elefteriades, A.F. DiMarco, P. Talonen, M. Bijak, W. Girsch, C. Kantor:
Electrical Stimulation to Restore Respiration, Journal of Rehabilitation Research and
Development, Vol. 33, No. 2, Apr. 1996, pp. 123 132.
A.F. DiMarco: Neural Protheses in the Respiratory System, Journal of Rehabilitation
Research and Development, Vol. 38, No. 6, Nov.-Dec. 2001, pp. 601 607.
A.F. DiMarco: Restoration of Respiratory Muscle Function following Spinal Cord Injury:
Review of Electrical and Magnetic Stimulation Techniques, Respiratory Physiology and
Neurobiology, Vol. 147, No. 2-3, July 2005, pp. 273 287.
A.F. DiMarco, Y. Takaoka, K.E. Kowalski: Combined Intercostal and Diaphragm Pacing to
Provide Artificial Ventilation in Patients with Tetraplegia, Archives of Physical Medicine
and Rehabilitation, Vol. 86, No. 6, Jun 2005, pp. 1200 1207.
http://www.concept2.co.uk/training/breathing.php
S.H. Linder: Functional Electrical Stimulation to Enhance Cough in Quadriplegia, Chest,
Vol. 103, No. 1, Jan. 1993, pp. 166 169.
R.J. Jaeger, R.M. Turba, G. Yarkony, E.J. Roth: Cough in Spinal Cord Injured Patients:
Comparison of Three Methods to Produce Cough, Archives of Physical Medicine and
Rehabilitation, Vol. 74, No. 12, Dec. 1993, pp. 1358 1361.
W.E. Langbein, C. Maloney, F. Kandare, U. Stanic, B. Nemchausky, R.J. Jaeger: Pulmonary
Function Testing in Spinal Cord Injury: Effects of Abdominal Muscle Stimulation, Journal
of Rehabilitation Research and Development, Vol. 38, No. 5, Sept.-Oct. 2001, pp. 591 597.
A.F. DiMarco, J.R. Romaniuk, K.E. Kowalski, G.S. Supinski: Efficacy of Combined
Inspiratory Intercostal and Expiratory Muscle Pacing to Maintain Artificial Ventilation,
American Journal of Respiratory and Critical Care Medicine, Vol. 156, No. 1, July 1997,
pp. 122 126.
F. Kandare, G. Exner, J. Jeraj, A. Aliverti, R. Dellaca, U. Stanic, A. Pedotti, R. Jaeger:
Breathing Induced by Abdominal Muscle Stimulation in Individuals without Spontaneous
Ventilation, Neuromodulation, Vol. 5, No. 3, July 2002, pp. 180 185.
H. Gollee, K.J. Hunt, M.H. Fraser, A.N. McLean: Abdominal Stimulation for Respiratory
Support in Tetraplegia: A Tutorial Review, Journal of Automatic Control, Vol. 18, No. 2,
2008, pp. 85 92.
C. Campbell, M.B. Weinger, M. Quinn: Alterations in Diaphragm EMG Activity During
Opiate-induced Respiratory Depression, Respiration Physiology, Vol. 100, No. 2, May
1995,pp. 107 117.
C. Gaultier: Respiratory Muscle Function in Infants, European Respiratory Journal, Vol. 8,
1995, pp. 150 153.
E.J. Maarsingh, L.A. Van Eykern, A.B. Sprikkelman, M.O. Hoekstra, W.M.C. van
Aalderen: Respiratory Muscle Activity Measured with a Noninvasive EMG Technique:
Technical Aspects and Reproducibility, Journal of Applied Physiology, Vol. 88, No. 6, June
2000, pp. 1955 1961.
D.E. Dow, C. Mantillia, W.Z. Zhan, G.C. Sieck: EMG-based Detection of Inspiration in the
Rat Diaphragm Muscle, EMBS 06 , Aug.-Sept. 2006, pp. 1204 1207.
398
You might also like
- Satipatthana VipassanaDocument50 pagesSatipatthana VipassanapeperetruNo ratings yet
- DR Breath by Carl StoughDocument128 pagesDR Breath by Carl StoughAlonso RodriguezNo ratings yet
- Yi Chin ChingDocument2 pagesYi Chin Chingredmantis3No ratings yet
- Tsa Lung 1: Upward-Moving Wind Practice Instructions The Formal PracticeDocument2 pagesTsa Lung 1: Upward-Moving Wind Practice Instructions The Formal PracticeChris ChristodoulidisNo ratings yet
- SuctioningDocument58 pagesSuctioningAyusa PradhanNo ratings yet
- Buteyko Small ManualDocument27 pagesButeyko Small ManualStephen Murray100% (4)
- Textbooks of Pulmonary RehabilitationDocument383 pagesTextbooks of Pulmonary RehabilitationMaghiar Ioana67% (3)
- (2013) Respiratory Diseases of The HorseDocument238 pages(2013) Respiratory Diseases of The Horsekaren montoyaNo ratings yet
- Checklist For Steam Inhalation Using A Nelson'S Inhaler: S.No Content Demo Return Demo Practice 1 Practice 2 PurposeDocument5 pagesChecklist For Steam Inhalation Using A Nelson'S Inhaler: S.No Content Demo Return Demo Practice 1 Practice 2 PurposeNeelofur Ibran Ali50% (2)
- Neonatal Ventilation, First StepDocument101 pagesNeonatal Ventilation, First StepJimena JuarezNo ratings yet
- NCM 109 Resource UnitDocument51 pagesNCM 109 Resource UnitDaryl Adrian RecaidoNo ratings yet
- Nursing Care Plan - Impaired Gas ExchangeDocument3 pagesNursing Care Plan - Impaired Gas ExchangeYum C86% (65)
- 2015 Dens PCM Guide EnglishDocument142 pages2015 Dens PCM Guide EnglishParallaxster100% (5)
- Smart Pulmonary Function Analyser Project ProposalDocument7 pagesSmart Pulmonary Function Analyser Project Proposalيحيى البشيتيNo ratings yet
- Viren PC BasedDocument21 pagesViren PC BasedAman SainiNo ratings yet
- Research Proposal: MPT (Cardio Respiratory Disorders)Document14 pagesResearch Proposal: MPT (Cardio Respiratory Disorders)permanaNo ratings yet
- Diagnostic SpirometerDocument3 pagesDiagnostic SpirometerseventhsensegroupNo ratings yet
- Is My Patient's Respiratory Drive (Too) High?: What'S New in Intensive CareDocument4 pagesIs My Patient's Respiratory Drive (Too) High?: What'S New in Intensive CareBiancaPancuNo ratings yet
- Lung Function Assessment by ImpulseDocument12 pagesLung Function Assessment by Impulsethiago gibsonNo ratings yet
- Assignment 05: What Is It?Document3 pagesAssignment 05: What Is It?NIKAH PAULINE ALCANTARANo ratings yet
- PFT measures lung function through spirometry, diffusion testsDocument4 pagesPFT measures lung function through spirometry, diffusion testspragna novaNo ratings yet
- Using An Ambulatory Stress Monitoring Device To Identify Relaxation Due To Untrained Deep BreathingDocument4 pagesUsing An Ambulatory Stress Monitoring Device To Identify Relaxation Due To Untrained Deep BreathingGuillermo923No ratings yet
- Pakistan DyspneaDocument7 pagesPakistan DyspneaNelson LoboNo ratings yet
- Personal Lung FunctionDocument10 pagesPersonal Lung FunctionSandeepNo ratings yet
- The Effect of Pursed - Lip Breathing Exercise Vs Diaphragmatic Breathing in Stabilizing The Vitals After 6-MWT Among Overweight Individuals-IJRASETDocument12 pagesThe Effect of Pursed - Lip Breathing Exercise Vs Diaphragmatic Breathing in Stabilizing The Vitals After 6-MWT Among Overweight Individuals-IJRASETIJRASETPublicationsNo ratings yet
- Arduino Uno Based Obstructive Sleep Apnea Detection Using Respiratory SignalDocument5 pagesArduino Uno Based Obstructive Sleep Apnea Detection Using Respiratory SignalbengheniaNo ratings yet
- BronchiectasisDocument7 pagesBronchiectasisNelson LoboNo ratings yet
- Chest: Impact of Expiratory Muscle Strength Training On Voluntary Cough and Swallow Function in Parkinson DiseaseDocument8 pagesChest: Impact of Expiratory Muscle Strength Training On Voluntary Cough and Swallow Function in Parkinson DiseaseAna Marta AnastácioNo ratings yet
- Bertoni 2019Document10 pagesBertoni 2019MISSAEL ESPINOZANo ratings yet
- Asynchrony Consequences and ManagementDocument17 pagesAsynchrony Consequences and ManagementLexNo ratings yet
- Asynchrony Consequences and ManagementDocument17 pagesAsynchrony Consequences and ManagementAna MariaNo ratings yet
- Review of Experiment Biology JournalDocument7 pagesReview of Experiment Biology JournalBeth BloomwoodNo ratings yet
- Efficacy of Balloon Blowing Exercise on PEFR in Young Adult SmokersDocument5 pagesEfficacy of Balloon Blowing Exercise on PEFR in Young Adult Smokerselieser toding mendilaNo ratings yet
- Ejercicio DiafragmaticoDocument3 pagesEjercicio DiafragmaticoN onlyNo ratings yet
- Mechanical Ventilation Dyssynchrony Types and ManagementDocument17 pagesMechanical Ventilation Dyssynchrony Types and ManagementjuanNo ratings yet
- Ventilator System ServoDocument54 pagesVentilator System ServoRoshield RandasanNo ratings yet
- EMSTDocument10 pagesEMSTPilar Aguilera LópezNo ratings yet
- Manually Assisted Cough Improves Lung Function After Spinal Cord InjuryDocument6 pagesManually Assisted Cough Improves Lung Function After Spinal Cord InjuryIskandar PakayaNo ratings yet
- Gráficas Ventilación MecánicaDocument17 pagesGráficas Ventilación MecánicaLulú PérezNo ratings yet
- Jurnal PENA Vol.33 No.1 Edisi Maret 2019Document7 pagesJurnal PENA Vol.33 No.1 Edisi Maret 2019LailatulQomariyahNo ratings yet
- A Review of The Ultrasound Assessment of Diaphragmatic Function in Clinical PracticeDocument9 pagesA Review of The Ultrasound Assessment of Diaphragmatic Function in Clinical PracticeSilvanaNo ratings yet
- Thesis Topics in Respiratory MedicineDocument5 pagesThesis Topics in Respiratory Medicinecyndiruppelspringfield100% (2)
- Neurovent Research & Neurally Adjusted Ventilatory Assist (Nava)Document27 pagesNeurovent Research & Neurally Adjusted Ventilatory Assist (Nava)peterNo ratings yet
- Effects of Respiratory Muscle Therapy On Obstructive Sleep Apnea: A Systematic Review and Meta-AnalysisDocument17 pagesEffects of Respiratory Muscle Therapy On Obstructive Sleep Apnea: A Systematic Review and Meta-AnalysisDavid SoaresNo ratings yet
- New JEEEM Itemplate2021 MAS DIO BaruDocument19 pagesNew JEEEM Itemplate2021 MAS DIO BaruAyu NissaNo ratings yet
- Understanding the Clinical Presentation and Pathophysiology of Total Brain FailureDocument5 pagesUnderstanding the Clinical Presentation and Pathophysiology of Total Brain FailureEmmaNo ratings yet
- FinalversionofC3018 PDFDocument21 pagesFinalversionofC3018 PDFEdgar FarfánNo ratings yet
- FinalversionofC3018 PDFDocument21 pagesFinalversionofC3018 PDFEdgar FarfánNo ratings yet
- HospitalisasiDocument13 pagesHospitalisasiViviNo ratings yet
- Chiropractic Treatment FOR: AsthmaDocument5 pagesChiropractic Treatment FOR: AsthmaAdriana HuescaNo ratings yet
- Design and Implementation of A Noncontact Sleep Monitoring System Using Infrared Cameras and Motion SensorDocument9 pagesDesign and Implementation of A Noncontact Sleep Monitoring System Using Infrared Cameras and Motion SensorugurAyvazNo ratings yet
- Bioethic - Intro 8Document5 pagesBioethic - Intro 8EmmaNo ratings yet
- Jurnal Musculoskeletal System 2Document14 pagesJurnal Musculoskeletal System 2miraNo ratings yet
- Physiotherapy in IcuDocument23 pagesPhysiotherapy in Icuradhika thapaNo ratings yet
- Asthma Enose IOT ReportDocument55 pagesAsthma Enose IOT ReportASHVIK JNo ratings yet
- Introduction to Mechanical VentilationDocument4 pagesIntroduction to Mechanical VentilationvgmanjunathNo ratings yet
- Indian Journal of Nursing SciencesDocument5 pagesIndian Journal of Nursing Sciencesmadhu.BNo ratings yet
- Clinical Guidelines PDFDocument19 pagesClinical Guidelines PDFEmilio AcostaNo ratings yet
- Wireless Smartphone Diagnosis of Pulmonary IllnessesDocument20 pagesWireless Smartphone Diagnosis of Pulmonary IllnessesMay Shuen PoonNo ratings yet
- TripodDocument4 pagesTripodlauraNo ratings yet
- Tee Slide 2Document10 pagesTee Slide 2OpeyemiNo ratings yet
- Slow Deep Pursed-Lips Breathing Exercise On Vital Lung Capacity in Post-Extubation Patients in The Intensive Care UnitDocument10 pagesSlow Deep Pursed-Lips Breathing Exercise On Vital Lung Capacity in Post-Extubation Patients in The Intensive Care Unitanggi rahmawatiNo ratings yet
- 6 - WolfeDocument25 pages6 - WolfeEzeBorjesNo ratings yet
- Emphysema Facts: Causes, Symptoms, Diagnosis and TreatmentDocument27 pagesEmphysema Facts: Causes, Symptoms, Diagnosis and TreatmentDiana Laura LeiNo ratings yet
- 2014 1 4 1 VetkasovDocument8 pages2014 1 4 1 VetkasovDianaSantosNo ratings yet
- Copd Response of The Respiratory Muscles To Rehabilitation inDocument7 pagesCopd Response of The Respiratory Muscles To Rehabilitation inoanceaNo ratings yet
- Effects of A Balloon-Blowing Exercise On Lung Function of SmokersDocument4 pagesEffects of A Balloon-Blowing Exercise On Lung Function of SmokersMónica ReisNo ratings yet
- Mag 2003 PDFDocument32 pagesMag 2003 PDFAtika AudiniNo ratings yet
- Introduct Ioni Ni NT Ro: Menu Planning and Sample MenusDocument11 pagesIntroduct Ioni Ni NT Ro: Menu Planning and Sample MenusAtika AudiniNo ratings yet
- Global Initiative For Chronic Obstructive L Ung D Isease: OR ReproduceDocument0 pagesGlobal Initiative For Chronic Obstructive L Ung D Isease: OR ReproducePorfirio Astudillo CastroNo ratings yet
- Prna 2009 - 5 PDFDocument132 pagesPrna 2009 - 5 PDFAtika AudiniNo ratings yet
- American Lung PDFDocument6 pagesAmerican Lung PDFAtika AudiniNo ratings yet
- 2 PDFDocument10 pages2 PDFAtika AudiniNo ratings yet
- Prna 2009 - 5 PDFDocument132 pagesPrna 2009 - 5 PDFAtika AudiniNo ratings yet
- Print Nomer 4Document10 pagesPrint Nomer 4Atika AudiniNo ratings yet
- IBM MakalahDocument4 pagesIBM MakalahAtika AudiniNo ratings yet
- 3.5 Mundane Food and DrinkDocument16 pages3.5 Mundane Food and DrinkJames LewisNo ratings yet
- Newer Modes of Mechanical Ventilation - Diapo PDFDocument11 pagesNewer Modes of Mechanical Ventilation - Diapo PDFStefany MedinaNo ratings yet
- Sindh Rescue 1122 Test Sample PapersDocument12 pagesSindh Rescue 1122 Test Sample PapersMAANJONY100% (1)
- Breathing and Exchange of GasesDocument3 pagesBreathing and Exchange of GasesMaahika MitraNo ratings yet
- 1 Radiant Health For BeginnersDocument28 pages1 Radiant Health For BeginnersAnonymous fO8xe7rMyA100% (1)
- Errors in VO2 TestingDocument16 pagesErrors in VO2 Testingcrisanto valdezNo ratings yet
- Pranayamas and Their Neurophysiological EffectsDocument10 pagesPranayamas and Their Neurophysiological EffectsPuneeth RaghavendraNo ratings yet
- Simulated Exam RationalesDocument20 pagesSimulated Exam Rationalesrhymes2u100% (3)
- Mechanisms of Gas Exchange Impairment in IPFDocument7 pagesMechanisms of Gas Exchange Impairment in IPFertyucbNo ratings yet
- Artificial RespirationDocument32 pagesArtificial RespirationJonathan cagasan100% (1)
- Electric Shock Dangers and First AidDocument6 pagesElectric Shock Dangers and First AidMilos VirijevicNo ratings yet
- Mindray Medical brochure overviewDocument2 pagesMindray Medical brochure overviewVernica AndreiNo ratings yet
- Task NCPDocument12 pagesTask NCPferdy ilhamNo ratings yet
- Oxygen and carbon dioxide transport mechanismsDocument9 pagesOxygen and carbon dioxide transport mechanismspuchio100% (1)
- SyndromeDocument6 pagesSyndromeVillegas Valentín José AlbertoNo ratings yet
- Oxygenation: An Essential Process for LifeDocument14 pagesOxygenation: An Essential Process for LifeVinzii DrtNo ratings yet
- Circulatory, Respiratory and Excretory Systems TestDocument6 pagesCirculatory, Respiratory and Excretory Systems TestJunior SencionNo ratings yet
- Y3 Science - Learner - Book - Answers - PDF - Moon - ShadowDocument20 pagesY3 Science - Learner - Book - Answers - PDF - Moon - Shadow21ke21i846No ratings yet
- Msds-Alkyd PrimerDocument5 pagesMsds-Alkyd Primerrian wijayaNo ratings yet
- Specimen QP - Paper 1 OCR (A) Biology As-LevelDocument23 pagesSpecimen QP - Paper 1 OCR (A) Biology As-LevelNatsaisheNo ratings yet
- Chapter 22 Upper Respiratory DisorderDocument171 pagesChapter 22 Upper Respiratory DisorderAnnette Aquino GuevarraNo ratings yet
- Nursing Practice 1 QuestionDocument12 pagesNursing Practice 1 QuestiongranfrancoNo ratings yet