Professional Documents
Culture Documents
4NUR-8.1 Case 4 - Gynecologic Nursing (Written Report)
Uploaded by
lhedaven0 ratings0% found this document useful (0 votes)
194 views30 pagesThis document provides demographic and health history information for a 49-year-old female patient admitted with right lower quadrant pain and a diagnosis of metastatic ovarian cancer. It details her chief complaint, history of present illness over the past year, past medical history, family history, and physical assessment findings on admission. It also includes an anatomy and physiology section summarizing the key structures of the female reproductive system including the external genitalia, internal organs like the vagina and uterus, and their functions.
Original Description:
4NUR-8.1 Case 4 - Gynecologic Nursing (Written Report)
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document provides demographic and health history information for a 49-year-old female patient admitted with right lower quadrant pain and a diagnosis of metastatic ovarian cancer. It details her chief complaint, history of present illness over the past year, past medical history, family history, and physical assessment findings on admission. It also includes an anatomy and physiology section summarizing the key structures of the female reproductive system including the external genitalia, internal organs like the vagina and uterus, and their functions.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
194 views30 pages4NUR-8.1 Case 4 - Gynecologic Nursing (Written Report)
Uploaded by
lhedavenThis document provides demographic and health history information for a 49-year-old female patient admitted with right lower quadrant pain and a diagnosis of metastatic ovarian cancer. It details her chief complaint, history of present illness over the past year, past medical history, family history, and physical assessment findings on admission. It also includes an anatomy and physiology section summarizing the key structures of the female reproductive system including the external genitalia, internal organs like the vagina and uterus, and their functions.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 30
1 | P a g e
UNIVERSITY OF SANTO TOMAS
COLLEGE OF NURSING
COMPETENCY APPRAISAL - OB
CASE SCENARIO
WRITTEN REPORT
Gynecologic Disorder
Submitted by: IV-8 RLE 1
Pascual, Kimberly Mae M.
Paterno, Marielle Ina S.
Paulino, Katrina Sarah Mae P.
Paulino, Lianne Alyzza A.
Payuran, Joanna Lissa F.
Pazcoguin, John Micko A.
Pelonio, Jeannie Lou N.
Perez, Mark Lester M.
Pesigan, Kristoffer Louis P.
Pineda, Angelica Marie B.
Pitargue, Maria Inna B.
Pieda, Maria Angela Kristine S.
I. DEMOGRAPHIC DATA
Name: M.A
Age: 49 y/o
Gender: Female
II. HEALTH HISTORY
Chief Complaint: RLQ pain
Diagnosis: Metastatic Ovarian Cancer
History of Present Illness:
1 yr PTA Noted progressive weight loss
Irregularities in menstruation
Dysmenorrhea on the first 2 days of menses
Dysparunea
8 months PTA Noted progressive weight loss
Irregularities in menstruation
Dysmenorrhea
Dysparunea
(-) result in pregnancy test
5 months PTA Still with progressive abdominal enlargement
Weight loss and anorexia
Early satiety and bloatedness
Epigastric pain, nausea and vomiting
3 months PTA Still with amenorrhea
Palpable node in the LUQ of her breast
2 | P a g e
Consulted an internist -> advised mammography and breast
nodule biopsy
1 month PTA Pain on the RLQ
Progressive abdominal enlargement
Weight loss
Occasional febrile episode
Dyspnea
Prompted consult and subsequent admission
Past Medical History:
Hypertensive (8 yrs) maintained on Amlodipine 10 mg BID
Diabetic (2 yrs) on Metformin 500mg/tab TID
Family History:
(+) Family hx of colon cancer - uncle
Personal and Social History:
G3 P2 (1-1-1-2)
1
st
sexual contact: 16 y/o
Previous intake of OCP (8 yrs)
Smoker: 6-7 sticks (30 yrs)
III. PHYSICAL ASSESSMENT:
Physical Examination on Admission:
VS: BP 170/90, PR 113/min, RR 26, T 38.9, BMI 15
Conscious, coherent but restless
Pale palpebral conjunctiva, anicteric sclera
(+) nasal flaring with intercostal retraction
Lagging on the L hemi-diaphragm
Decrease tactile fremiti on the L
Decrease BS on the L
(+) 2x 1.3 mm nodular fixed mass on the L breast
AC 68 cmm
Bulging flanks with (+) fluid wave
(+) 4x 3.8 cm palpable mass on the RLQ area with direct and rebound tenderness
(+) grade 2 bipedal edema
NE is essentially normal
3 | P a g e
IV. ANATOMY AND PHYSIOLOGY:
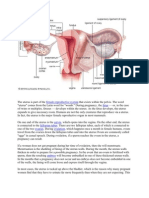
Female Reproductive System
The female reproductive organ consists of the external and internal organs and
the accessory organs of the breasts.
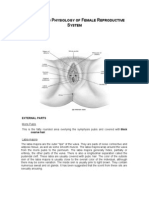
EXTERNAL GENITALS
- Also referred as the vulva includes the following:
Mons Pubis
Labia majora
Labia minora
Clitoris
Urethral meatus and the opening of the paraurethral (skenes) glands
Vaginal vestibule (vaginal orifice, vulvovaginal glands, hymen, and fossa
navicularis)
Perineal body
The urethral meatus and the perineal body are not true parts of the female
reproductive system, they are just considered because of their proximity and
relationship to the vulva
MONS PUBIS
Also known as Mons Veneris. It is a softly rounded mound of subcutaneous fatty
tissue beginning at the lowest portion of the anterior abdominal wall. The mons pubis is
covered with pubic hair. The mons pubis protects the pelvic bones, especially during
coitus.
LABIA MAJORA
The labia majora are the outer lips of the vulva, which are pads of fatty tissue that
wrap around the vulva from top to bottom around the mons veneris to the perineum. It is
usually covered with pubic hair, and contains numerous sweat and oil glands.
LABIA MINORA
The labia minora are the inner lips of the vulva, whose thin stretches of skin and
tissue reside directly inside of the labia majora. The labia minora provides added
protection to the vagina, urethra, and clitoris.
CLITORIS
The clitoris is a small light pink oval between the top of the labia minora and the
clitoral hood. It is a small body of smooth spongy tissue that is highly sensitive and
contains some 8,000 nerve endings and is the primary erogenous organ of women. It is
protected by the prepuce, or clitoral hood, a covering of tissue similar to the labia
minora. In addition, it secretes smegma, which along with other vulval secretions has a
unique odor that may be sexually stimulating to the male.
4 | P a g e
URETHRAL MEATUS and PARAURETHRAL GLANDS
The urethral meatus is located 1 to 2.5 cm beneath the clitoris in the midline of
the vestibule; it often appears as a puckered, slitlike opening. At times the meatus is
difficult to visualize because of the presence of the blind dimples, small mucosal folds,
or wide variations in location.
The paraurethral glands, or skenes glands, open into the porsterior wall of the
urethra close to its opening. Their secretions lubricate the vaginal opening, facilitating
sexual intercourse.
VAGINAL VESTIBULE
It is a part of the vulva between the labia minora into which the urethral
opening and the vaginal opening open. The vestibule contains the vaginal opening or
the introitus, which is the border between the external and internal glands.
The hymen is a thin, elastic collar or semicollar of tissue that surrounds the
vaginal opening. External to the hymen at the base of the vestibule are the two small
papular elevations containing the openings of the ducts of the vulvovaginal (Bartholins)
glands. These glands secrete a clear, thick, alkaline mucus that enhances the viability
and motility of the sperm deposited in the vaginal vestibule. These gland ducts can
harbor Neiserria gonorrhea and other bacteria, which can cause pus formation and
abscess in the Bartholins glands.
The vestibular area is innervated mainly by the perineal nerve from the sacral
plexus. The area is not sensitive to touch generally; however, the hymen contains
numerous free endings as receptors to pain.
PERINEAL BODY
The perineal body (or central tendon of perineum) is a pyramidal
fibromuscular mass in the middle line of the perineum at the junction between the
urogenital triangle and the anal triangle. It is found between the vagina and anus, the
perineal body is essential for the integrity of the pelvic floor, particularly in females. Its
rupture during delivery leads to widening of the gap between the anterior free borders of
levator ani muscle of both sides, thus predisposing the woman to prolapse of
the uterus, rectum, or even the urinary bladder.
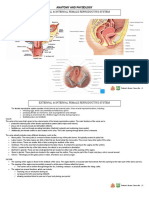
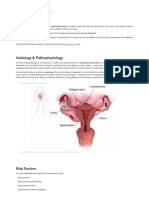
INTERNAL ORGANS
- The female internal reproductive organs include:
Vagina
Uterus
Fallopian tubes and ovaries
These are the target organs for estrogenic hormones and play a unique part in the
reproductive cycle
5 | P a g e
VAGINA
The vagina is an elastic muscular canal that extends from the cervix to
the vulva. The internal lining of the vagina consists of stratified squamous epithelium.
Beneath this lining is a layer of smooth muscle, which may contract during sexual
intercourse and when giving birth. Beneath the muscle is a layer of connective
tissue called adventitia.
Although there is wide anatomical variation, the length of the unaroused vagina
of a woman of child-bearing age is approximately 6 to 7.5 cm (2.5 to 3 in) across the
anterior wall (front) and 9 cm (3.5 in) long across the posterior wall (rear). During sexual
arousal the vagina expands in both length and width. Its elasticity allows it to stretch
during sexual intercourse and during birth to offspring. The vagina connects the
superficial vulva to the cervix of the deep uterus.
The vagina has three functions:
To serve as the passage for sperm and for the fetus during birth
To provide passage for the menstrual products from the uterine endometrium to
the outside of the body
To protect against trauma from sexual intercourse and infection from pathogenic
organisms.
UTERUS
The uterus, or womb, is the main female internal reproductive organ. The inner
lining of the uterus is called the endometrium, which grows and changes during the
menstrual cycle to prepare to receive a fertilized egg. The layer sheds at the end of
every menstrual cycle if fertilization does not happen. The uterus is lined with powerful
muscles to push the child out during labor.
The uterus consists of a body and a cervix.The cervix protrudes into the vagina.
The uterus is held in position within the pelvis by condensations of endopelvic fascia,
which are called ligaments. These ligaments include the pubocervical, transverse.
cervical ligaments cardinal ligaments, and the uterosacral ligaments. It is covered by a
sheet-like fold of peritoneum, the broad ligament.
The uterus is essential in sexual response by directing blood flow to
the pelvis and to the external genitalia, including the ovaries, vagina, labia, and clitoris.
The reproductive function of the uterus is to accept a fertilized ovum which
passes through the utero-tubal junction from the fallopian tube. It implants into
the endometrium, and derives nourishment from blood vessels which develop
exclusively for this purpose. The fertilized ovum becomes an embryo, attaches to a wall
of the uterus, creates a placenta, and develops into a fetus (gestates) until childbirth.
Due to anatomical barriers such as the pelvis, the uterus is pushed partially into the
abdomen due to its expansion during pregnancy. Even during pregnancy the mass of a
human uterus amounts to only about a kilogram (2.2 pounds).
6 | P a g e
The nulliparous uterus resembles an inverted pear and consists of two main
parts: the body and the cervix. The body is twice as long as the cervix, whereas the
converse is true in the newborn. The body includes the fundus, which is the portion that
lies superior and anterior to the openings of the uterine tubes. The body is usually tilted
anteriorly onto the bladder which is separated from the uterus by the uterovesical
pouch. Superior and posterior, the body is separated from the rectum by the recto-
uterine pouch , which usually contains coils of ileum. Right and left margins are
anchored to the broad ligaments. The region between the body and cervix is referred to
as the isthmus: during pregnancy, it is known as the "lower uterine segment." The cavity
of the isthmus was formerly called the "internal os." The cervix extends inferiorward and
posteriorward and usually forms approximately a right angle with the vagina. As the
bladder fills, the uterus tends to become retroverted. The cervix may be considered in
two parts: (1) a supravaginal portion superior to the limits of the vagina and (2) a vaginal
portion, which projects into the cavity of the vagina. The cavity of the uterine body,
which is somewhat triangular in coronal perspective, is slit-like in sagittal section. The
canal of the cervix communicates with the vagina by the external os, which is bounded
by anterior and posterior lips. The entire uterine cavity can be demonstrated
radiographically by hysterosalpingography. The uterus can be palpated bimanually.
Dilatation (of the cervical canal) and curettage (scraping of the uterine lining) are
performed for diagnostic or therapeutic purposes.
The layers, from innermost to outermost, are as follows:
Endometrium
The lining of the uterine cavity is called the "endometrium". It consists of the
functional endometrium and the basal endometrium from which the former arises.
Damage to the basal endometrium results in adhesion formation and/or fibrosis
(Asherman's syndrome). In all placental mammals, including humans, the
endometrium builds a lining periodically which is shed or reabsorbed if
no pregnancy occurs. Shedding of the functional endometrial lining is responsible
for menstrual bleeding (known colloquially as a "period" in humans, with a cycle
of approximately 28 days, +/-7 days of flow and +/-21 days of progression)
throughout the fertile years of a female and for some time beyond. Depending on
the species and attributes of physical and psychological health, weight,
environmental factors of circadian rhythm, photoperiodism (the physiological
reaction of organisms to the length of day or night), the effect of menstrual cycles
to the reproductive function of the uterus is subject to hormone production, cell
regeneration and other biological activities. The menstrual cycles may vary from
a few days to six months, but can vary widely even in the same individual, often
stopping for several cycles before resuming. Marsupials and monotremes do not
have menstruation.
Myometrium
The uterus mostly consists of smooth muscle, known as "myometrium." The
innermost layer of myometrium is known as the junctional zone, which becomes
thickened in adenomyosis.
7 | P a g e
Parametrium
The loose connective tissue around the uterus.
Perimetrium
The peritoneum covering of the fundus and ventral and dorsal aspects of the
uterus.
THE CERVIX
The cervix is the opening to the uterus. It varies in diameter from 1 to 3
millimeters, depending upon the time in the menstrual cycle when the measurement is
taken. The cervix is sometimes plugged with cervical mucous to protect the cervix from
infection; during ovulation, this mucous becomes a thin fluid to permit the passage of
sperm.
The cervical mucus has three functions:
To lubricate the vaginal canal
To act as a bacteriostatic agent
To provide an alkaline environment to shelter deposited sperm from the acidic
vagina
At ovulation, cervical mucus is clearer, thinner, more profuse, and more alkaline than
at other times.
UTERINE LIGAMENTS
Broad Ligaments. From each side of the uterus, the pelvic peritoneum extends
laterally, downward, and backward. A double fold of pelvic peritoneum forms the
layers of the broad ligament, enclosing the uterus. These layers separate to
cover the floor and sides of the pelvis. The uterine tube is situated within the free
upper border of broad ligament. The part of the broad ligament lying immediately
below the uterine tube is termed the mesosalpinx. The ovary lies behind the
broad ligament.
Round Ligaments. These fibromuscular bands are attached to the uterus. Each
round ligament passes forward and laterally between the layers of the broad
ligament to enter the deep inguinal ring.
Uterosacral Ligaments. These are a posterior continuation of the peritoneal
tissue, which forms the cardinal ligaments. The ligaments pass posteriorly to the
sacrum on either side of the rectum.
Ovarian ligament is a rounded, cord-like thickening of the broad ligament,
located at its lower end, where it is attached to the uterus. It, along with the other
ovarian ligaments, attaches to the ovaries and help hold them in position. The
largest of these ligaments, formed by a fold of peritoneum, is called the broad
ligament. It is also attached to the uterine tubes and to the uterus. At its upper
end, the ovary is held by a small fold of peritoneum called the suspensory
ligament, which contains the ovarian blood vessels and nerves. At its lower end,
it is attached to the uterus by a rounded, cord-like thickening of the broad
8 | P a g e
ligament, called the ovarian ligament. The peritoneum is a two-layered
membrane that supports the abdominal organs, produces lubricating fluid that
allows the organs to flow smoothly over each other, and protects against
infection.
Cardinal Ligament. It is located at the base of the broad ligament of the uterus.
Importantly, it contains the uterine artery and uterine vein. There is a pair of
cardinal ligaments in the female human body.It attaches the cervix to the lateral
pelvic wall at the ischial spine, and is continuous externally with the fibrous tissue
that surrounds the pelvic blood vessels. It thus provides support to the uterus.
Infundibulopelvic Ligament. It suspends and supports the ovaries. Arising from
the outer third of the broad ligament, the infundibulopelvic ligament contains the
ovarian vessels and nerves.
FALLOPIAN TUBES
The fallopian tubes stretch from the uterus to the ovaries and measure about 8 to
10 cm (4 to 6 inches) in length. The ends of the fallopian tubes lying next to the ovaries
feather into ends called fimbria (Latin for "fringes" or "fingers"). Millions of tiny hair-like
cilia line the fimbria and interior of the fallopian tubes. The cilia beat in waves hundreds
of times a second catching the egg at ovulation and moving it through the tube to the
uterine cavity. Other cells in the tube's inner lining or endothelium nourish the egg and
lubricate it's path during its stay inside the fallopian tube. Once inside the fallopian tube,
the egg and sperm meet and the egg is fertilized. If an egg doesn't become fertilized
within 24 to 36 hours after ovulation, it will deteriorate and be removed by the body's
immune system like any other dead cell in the body.
Segments of the fallopian tube
The fallopian tube is not just a passive pipe or a conduit, but an active organ with its
separate locations performing separate functions. Starting from the ovarian end
(fimbria) and proceeding toward the uterus, these are the:
Fimbrial segment - faces the ovary
Infundibular segment - funnel shaped segment behind the fimbria
Ampullary segment - wide middle segment
Isthmic segment - narrow muscular segment near the uterus
Interstitial segment - passes through the uterine muscle into the uterine cavity
Role of the fallopian tubes in fertilization and implantation
A muscular ligament called the fimbria ovarica joins the fimbrial end of the tube
and the ovary. At the time of ovulation, the fimbria ovarica contracts to pull the fimbrial
end of the tube even closer to the ovary. The beating cilia cells of the fimbria capture
the egg and draw it into the fallopian tube. Muscular contractions of the tube and the
cilia of its inner lining move the egg and sperm toward the uterus. The interstitial
segment of the tube acts like a muscle sphincter and prevents the egg from being
9 | P a g e
released into the uterus until it is ready for implantation. During its week-long journey
through the fallopian tube, a fertilized egg is nourished by cells lining the tubal lumen
while the egg divides many times. When the outer membrane of the egg breaks apart,
allowing the embryo to "hatch", it is able to implant itself into the uterine lining or
endometrium. Implantation usually occurs about 1 week after ovulation.
OVARIES
The ovaries are 2 small glands located on either side of a woman's uterus. They
are part of the female reproductive system that are responsible for the storing and
releasing of the eggs (ova), which can develop into a fetus if fertilized by a male's
sperm. Approximately once a month, about 2 weeks before a woman's next period
ovulation occurs when an egg is released from one of her ovaries The ovaries also
produce female sex hormones, estrogen and progesterone, which help control the
menstrual cycle, breast development, and other functions.
FEMALE HORMONES
a. Estrogen
increases myometrial contractility in both the uterus and fallopian tubes
increases uterine sensitivity to oxytocin
inhibits FSH production
b. Progesterone
stimulates LH production
secreted by the corpus luteum
found in greatest amounts in the secretory phase of the menstrual cycle
decreases uterine motility and contractility caused by estrogens preparing the
uterus for implantation after the ovum is fertilized
hormone of pregnancy
vaginal epithelium proliferates and the cervix secretes thick, viscous
mucus
prepares the breast for lactation
c. Prostaglandin
oxygenated fatty acids produced by the cells of the endometrium
also classified as hormones
2 primary types
PGE- relaxes smooth muscles; potent vasodilator
PGF- increases contractility of muscles and arteries; potent
vasoconstrictor
OVARIAN CYCLE
a. Follicular phase (days 1 - 14)
Hypothalamus secretes gonadotropin releasing hormone(GnRH)
GnRH stimulate anterior pituitary gland to secrete FSH/LH
10 | P a g e
FSH is primarily responsible for the maturation of the ovarian follicle
b. Luteal phase (days 15 - 28 in a 28 day cycle)
Release of ovum
LH: corpus luteum develops from ruptured follicle
secretion of progesterone increases
fertilized ovum able to implant into endometrium secretion of human chorionic
gonadotropin (hCG)
absence of fertilization corpus luteum degenerates
MENSTRUAL CYCLE
Menstruation is cyclic uterine bleeding in response to cyclic hormonal changes.
Menstruation occurs when the ovum is not fertilized and begins about 14 days after
ovulation in a 28-day cycle. The menstrual discharge referred to as menses is
composed of blood mixed with fluid, cervical and vaginal secretions, bacteria, mucus,
leukocytes, and other cellular debris. The menstrual discharge is dark red and has a
distinctive odor.
Menstrual parameters vary greatly among individual. Emotional and physical
factors such as illness, excessive fatigue, stress or anxiety, and vigorous exercise
programs can alter the cycle interval. The duration of menses is from 2-8 days, with the
blood loss averaging 30 ml. The uterine (menstrual) cycle has four phases.
1. Menstrual phase
Menstruation occurs during this phase. Also, in this phase, some endometrial
areas are shed, while others remain. Some of the remaining tips of endometrial glands
begin to regenerate. The endometrium is in a resting state after menstruation. Estrogen
levels are low, and the endometrium is 1 to 2 mm deep. During this part of the cycle, the
cervical mucosa is scanty viscous, and opaque.
2. Proliferative phase
This phase begins when the endometrial glands enlarge, becoming twisted and
longer in response to increasing amounts of estrogen. The blood vessels become
prominent and dilated, and the endometrium increases in thickness six to eightfold. This
gradual process reaches its peak just before ovulation. The cervical mucosa becomes
thin, clear, watery, and more alkaline, making the mucosa more favorable to
spermatozoa. As ovulation nears, the cervical mucosa shows increased elasticity, called
spinnbarkeit. At ovulation, the mucus will stretch more than 5 cm. The cervical mucosa
pH increases from below 7.0 to 7.5 at the time of ovulation. On microscopic
examination, the mucosa shows a characteristic ferning pattern. This fern pattern is
useful in assessing ovulation time.
3. Secretory phase
The secretory phase follows ovulation. The endometrium, under estrogenic
influence, undergoes slight cellular growth. Progesterone, however, causes such
marked swelling and growth that the epithelium is warped into folds. The amount of
11 | P a g e
tissue glycogen increases. The glandular epithelial cells begin to fill with cellular debris,
become twisted, and dilate. The glands secrete small quantities of endometrial fluid in
preparation for a fertilized ovum. The vascularity of the entire uterus increases greatly,
providing a nourishing bed for implantation. If implantation occurs, the endometrium,
under the influence of progesterone, continues to develop and become even thicker.
4. Ischemic phase
If fertilization does not occur, the ischemic phase begins. The corpus luteum
begins to degenerate, and as a result both estrogen and progesterone levels fall. Areas
of necrosis appear under the epithelial lining. Extensive vascular changes also occur.
Small blood vessels rupture, and the spiral arteries constrict and retract, causing a
deficiency of blood in the endometrium, which becomes pale. This ischemic phase is
characterized by the escape of blood into the stromal cells of the uterus. The menstrual
flow begins, thus beginning the menstrual cycle again. After menstruation, the basal
layer remains, so that the tips of the glands can regenerate the new functional
endometrial layer.
V. GYNECOLOGIC DISORDERS:
A. Menstrual Dysfunctions:
1. Amenorrhea absence of menstruation anytime between puberty and
menopause (not a disease but a symptom)
a. Primary failure of menstruation to appear initially at puberty
b. Secondary cessation of menstruation after menarche
Physiologic normal absence before puberty, during pregnancy, lactation and
menopause
Cryptomenorrhea or Pseudomenorrhea menstruation occurs but does not
appear externally because of obstruction in the lower genital organs
Pathological due to some pathologic diseases of the reproductive system
2. Oligomenorrhea reduction in frequency of menstruation or prolongation of
interval abnormally, usually from 38 days to 3 months
3. Polymenorrhea interval is shortened or more frequent occurrence of menses,
usually every 20 days
4. Hypomenorrhea scanty menstrual flow without relation to frequency
5. Hypermenorrhea / menorrhagia excessive menstrual flow
6. Metrorrhagia bleeding or spotting without obvious relation to the menstrual
cycle; also known as intermenstrual bleeding
7. Dysmenorrhea painful menstruation with spastic, crampy, and congestive pains
a. Primary or Intrinsic onset of pain early in menstrual life with inherent or
congenital causes
12 | P a g e
b. Secondary or Acquired (Extrinsic) onset of pain several years after menarche
Membranous Dysmenorrhea caused by the removal of the endometrium as
one piece instead of breaking off or sloughing off; also known as endometrial
cast
Causes:
a. Psychogenic unstable nervous system or psychic trauma especially when
it occurs during the menstrual period; lack of knowledge about significance
and normality of menstrual functions
b. Constitutional results from disease condition such as anemia, overwork
or fatigue
c. Obstructive or Anatomical caused by cervical lesions, stenosis or acute
anteflexion of the uterus
d. Endocrine Factors increased estrogen which is a normal stimulant of
uterine contractility
Treatment:
a. Endocrine Therapy
1. use of estrogen inadequate dosage in early part of the cycle to convert
ovulatory cycle to unovulatory
- inhibition of ovulation brings about relief in pain
2. use of progesterone to suppress ovulation, the drug is given during the
first 25 days of the cycle
b. Pre-sacral Neurectomy - surgical removal of the presacral plexus the
group of nerves that conducts the pain signal from the uterus to the brain.
c. Treatment during attacks:
1. local use of heat
2. analgesics
3. antispasmodics
d. Psychotherapy
Possible causes of menstrual dysfunctions
a. Neurogenic organic lesions or idiopathic hypothalamic dysfunction
b. Pituitary insufficiency of hormones, tumors, or congenital defect
c. Psychogenic minor or major psychosis
d. Chronic illness
e. Metabolic diseases of the pancreas, thryroid, and adrenals
f. Nutritional disturbances like malnutrition
g. Ovarian tumors or congenital defects
h. Congenital causes like imperforate hymen, absence of vaginal septum
(gynatresis)
i. Traumatic stenosis of vagina or cervix due to trauma
General Methods of Treatment
- each patient must be treated according to etiologic factor:
a. Steroid Therapy designed to trigger pituitary functions
13 | P a g e
b. Gonadotropic Therapy designed to replace pituitary hormones
c. Clomiphene Therapy stimulate pituitary activity through the hypothalamus
d. Hypothalamic Hormone Stimulation directly stimulates synthesis and
release fo pituitary and gonadotropins (still under research)
e. Good Nutrition
B. Dysfunctional Uterine Bleeding (DUB)
- abnormal bleeding form the uterus associated with tumor and inflammations. It is apt
to occur at the extremes of menstrual life.
- major cause is increase in the endometrial lining of the uterus (endometrial
hyperplasia)
C. Unovulatory Bleeding
- follicle develops but instead of maturation becomes cystic and then degenerates
D. Abnormal Menstruation
Precacious appearance of menarche early in childhood; usually under 9 years of
age. There is a question whether they can be really called as menstruation.
VI. USUAL GYNECOLOGIC PROCEDURES:
A. Schillers test
a preliminary test for cancer of the uterine cervix in which the cervix is painted
with an aqueous solution of iodine and potassium iodide and which shows up
healthy tissue by staining it brown and possibly cancerous tissue as white or
yellow due to its failure to take up the stain because of a deficiency of glycogen
in the cells
B. Papanicolau test
a method or a test based on it for the early detection of cancer especially of the
uterine cervix that involves staining exfoliated cells by a special technique which
differentiates diseased tissue
subjects:
women 20 years above
sexually active women: done regularly
preparations:
no sexual activity in the preceding 24 hours
no lubricant use
no vaginal tablets for 2-3 nights before
no perennial douche before the exam
procedure:
aspirate or swab vaginal secretions from the posterior fornix and make a
smear on the glass with light rolling motion. Do not let smear become dry,
immerse immediately in a fixing solution of ethanol 95%.
Results:
has 90-95% accuracy for cervical Ca
14 | P a g e
70-75% accuracy for severe dysplasia
80% accuracy for endometrial Ca
Classification:
Class 1 absence of atypical or abnormal cells
Class 2 atypical cytology but no evidence of malignancy
Class 3 cytology suggestive but not conclusive of malignancy
Class 4 cytology strongly suggest Ca
Class 5 cytology is conclusive of Ca
C. Culdoscopy
Visualization of the internal reproductive organs by inserting a tubular lighted
instrument (culdoscope) through an incision made in the posterior fornix of the
vagina into the cul-de-sac of Douglas
Preparation: Knee-chest
Home-care instructions
o No douches and sexual activity for 1 week
o Watch out for complications like infection, hemorrhage, and air embolism
o Incision should heal rapidly
D. Laparoscopy
Abdomen is insufflated with CO2 and a trocar is introduced through the lower
portion of the umbilicus. A laparoscope is inserted and pelvic organs are
visualized. This is a diagnostic aid to determine ectopic pregnancy, inflammatory
disease and ovarian neoplasms
E. Hystero-Salpingogram
X-ray study of the uterus and the fallopian tubes after the injection of a contrast
medium through the cervix via a cannula (indigo-carmine dye)
Purposes:
Study problems of sterility
Evaluate tubal patency
Determine the presence of uterine pathology
Position: Lithotomy
Result: If tubes are patent the dye can be visualized passing out the fimbriated
end of the fallopian tubes
F. Rubins test
Determine tubal patency, CO2 is passed through the cervix into the uterus and
tubes. If patent, gas will pass through the fimbriated ends of the fallopian tubes
into the peritoneal cavity and will give a sensation of fullness and spasmodic
shoulder pains due to severe irritation from the gas
G. Sim-Hunners test
Post-coital exam
A specimen of seminal fluid from posterior-fornix and cervical canal is aspirated
2-4 hours after coitus
15 | P a g e
Purposes
Test for compatibility of sperms with cervical mucus
Determine husbands ability to deposit normal motile sperms in sufficient
amount
H. Semen analysis
Examination of the semen for number and motility
I. Ultrasound
Simple, safe, and inexpensive procedure which causes or uses soundwaves of a
transducer and scan oscilloscope
Purpose: to determine tumor or cysts or retroperitoneal masses
Limitations
technical difficulty in fat or obese patients
could be altered by gas interference
J. Computerized Tomography
Instead of just a single X-ray source and film, there is an x-ray source moving
around the patient with special detectors opposite the x-ray source. The
computer translates the x-ray film taken on the patient and projects it into the
screen.
VII. DIFFERENTIAL DIAGNOSES:
Other disease conditions that may present with the signs and symptoms manifested
by the client in the case scenario given include:
*N.B: signs or symptoms in bold are those that are manifested by client in the scenario given
Acute appendicitis
Appendicitis is a condition characterized by inflammation of the appendix. Signs
and symptoms of appendicitis include presence of right lower quadrant pain,
and occasional febrile episodes.
Pelvic Inflammatory Disease
Pelvic inflammatory disease (PID) is an infectious and inflammatory disorder of
the upper female reproductive tract, including the uterus, fallopian tubes, and
adjacent pelvic structures. PID is initiated by infection that ascends from the
vagina and cervix. The most common presenting complaint is lower abdominal
pain.
Ovarian Torsion
Ovarian torsion (adnexal torsion) is an infrequent but significant cause of
acute lower abdominal pain in women. This condition is usually associated with
reduced venous return from the ovary as a result of stromal edema, internal
hemorrhage, hyperstimulation, or a mass. The ovary and fallopian tube are
16 | P a g e
typically involved. Other signs presented by patient indicative of diagnosis stated
include fever, nausea, and vomiting.
Endometriosis
Endometriosis is defined as the presence of normal endometrial mucosa (glands
and stroma) abnormally implanted in locations other than the uterine cavity. This
tissue, possessing the same steroid receptors as normal endometrium, is
capable of responding to the normal cyclic hormonal milieu. Microscopic internal
bleeding, with the subsequent inflammatory response, neovascularization, and
fibrosis formation, is responsible for the clinical consequences of this disease.
Symptoms include dysmenorrhea, heavy or irregular bleeding, pelvic pain,
lower abdominal pain, back pain, dyspareunia, dyschezia (pain on defecation),
bloatedness, nausea, and vomiting.
Ascites
Ascites describes the condition of pathologic fluid collection within the abdominal
cavity. As more fluid accumulates, increased abdominal girth and size are
commonly seen. Abdominal pain, discomfort, and bloating are also frequently
seen as ascites becomes larger. Shortness of breath or dyspnea can also
happen with large ascites due to increased pressure on the diaphragm and the
migration of the fluid across the diaphragm causing pleural effusions (fluid
around the lungs). Other signs include bulging flanks with (+) fluid wave.
Disease conditions that predisposes client to develop ascites include
hypertension.
Diverticular disease
Diverticula are small mucosal herniations protruding through the intestinal layers
and the smooth muscle along the natural openings created by the vasa recta or
nutrient vessels in the wall of the colon. These herniations create small pouches
lined solely by mucosa. Diverticulitis is defined as an inflammation of one or more
diverticula. In simple diverticulitis, localized abdominal tenderness in the area
of the affected diverticula and fever are common findings. Right lower quadrant
tenderness, mimicking acute appendicitis, can occur in right-sided diverticulitis.
In complicated diverticulitis with abscess formation, a tender palpable mass
may be felt on physical examination. Peritonitis due to free perforation results in
generalized tenderness with rebound and guarding on abdominal
examination. The abdomen may be distended and tympanic to percussion.
Bowel sounds can be diminished or absent.
Inflammatory Bowel Disease
Inflammatory bowel disease (IBD) is an idiopathic disease, probably involving an
immune reaction of the body to its own intestinal tract. The 2 major types of IBD
are ulcerative colitis (UC) and Crohn disease (CD). As the name suggests,
ulcerative colitis is limited to the colon. Crohn disease can involve any segment
of the gastrointestinal (GI) tract from the mouth to the anus. Fever, tachycardia,
dehydration, and toxicity may occur in patients with IBD. Signs of localized
17 | P a g e
peritonitis may also occur, although abdominal tenderness is common. Patients
with Crohn disease may develop a mass in the right lower quadrant. Common
presenting signs of complications include occult blood loss and low-grade fever,
weight loss, and anemia.
Large Bowel or Small Bowel Obstruction
A bowel obstruction happens when either the small or large intestine is partly or
completely blocked. The blockage prevents food, fluids, and gas from moving
through the intestines in the normal way. The blockage may cause severe pain
that comes and goes. Obstruction to the bowels is commonly manifested by
abdominal tenderness, abdominal distention, vomiting, and bloatedness.
Benign tumors of the uterus
a. Endometrial polyps
Endometrial polyps are small, soft growths on the lining of the uterus
(endometrium) which are also known as uterine polyps. These endometrial
polyps can irritate the surrounding tissues causing spotting or vaginal bleeding.
Endometrial polyps can occur alone or in groups. Most occurrences of
endometrial polyps are benign in nature.
The exact cause for the occurrences of endometrial polyps is still unknown
but polyps are said to form when there is an overgrowth of tissue in the uterine
lining. Growth of endometrial polyps also appears to be affected by hormone
levels and grow in response to circulating estrogen.
Endometrial polyps often cause no symptoms but if symptoms do occur,
one of the most common is bleeding. This includes irregular menstrual bleeding,
bleeding between menstrual periods, excessive heavy menstrual periods, vaginal
bleeding after menopause and infertility.
Endometrial polyps usually occur in women ages 40-50 years old. Risk
factors for endometrial polyps include obesity, high blood pressure, history of
cervical polyps and also women taking hormone replacement therapy.
b. Myomata or fibroids
Myomata or fibroids are benign swellings in the muscle of the womb that
occur in women of all ages and races. It is the most common benign tumor of the
uterus which is estimated to be found in 20% of women over 35 years of age.
Frequent spoken as fibroids which can be either single or multiple, microscopic
or big with weight as high as 410 lbs. It is a dense well-encapsulated nodule
composed chiefly of unstriped muscle and fibroid connective tissue.
18 | P a g e
A common cause for myomata is hormonal changes (estrogen). Myomas
do not develop before the body begins producing estrogen. Myomas tend to grow
very quickly during pregnancy when the body is producing extra estrogen. Once
menopause has begun, myomas generally stop growing and can begin to shrink
due to the loss of estrogen. A predisposing factor for myomata is nulligravidity.
Symptoms includes palpable mass in the lower abdomen or abdominal
enlargement, bleeding, pain which can be assumes as dysmenorrheal or
sensation of weight and bearing down and pressure effects manifested as
frequency in urination or dysuria and constipation.
Types of Myomata or fibroids according to placement:
a) Submucous myoma
- develops beneath the endometrium
- either pedunculated (attached to a pedicle) or wandering submucous
(goes from one site to another)
b) Interstitial or intramural myoma
- situated in the muscular wall with no close proximity to either the mucosa
or the serosa
c) Subserous or subperitoneal
- growth out between the folds of the broad ligament which may impede
on the ureter and iliac vessels
d) Intraligementary
- implants on the pelvic ligaments
e) Cervical
- rare and obstructs the cervix
Secondary changes:
a. Hyaline degeneration most common secondary change which involves
the broad areas of the tumor causing liquification when the tumor
outgrows the blood supply
b. Cystic degeneration enlargement of the lymphatics
c. Calcification occurs when there is circulatory disturbances which
converts the mass into a hard, stony mass
d. Infection and suppuration commonly occurs in the submucous myoma
which is prone to thinning and ulceration of the underlying mucosa giving
access to organisms from the uterine canal that can cause infection
e. Necrosis due to impairment of the blood circulation
f. Fatty degeneration rare but may occur with hyaline degeneration
g. Sarcomatous degeneration rare to occur
19 | P a g e
h. Acute torsion of the pedicle with acute disruption of the blood supply
resulting to gangrenous changes in the myoma.
VIII. PATHOPHYSIOLOGY
20 | P a g e
21 | P a g e
IX. MEDICATIONS
Amlodipine anti-hypertensive, Ca channel blocker
Metformin for type 2 DM, oral anti-hyperglycemic
X. LABORATORY PROCEDURES
*done to the patient
MAMMOGRAPHY
specific type of imaging low dose x-ray system examine the breast
mammogram exam itself
early detection and diagnosis
Recent advances:
DIGITAL MAMMOGRAPHY
Also called full-field digital mammography (FFDM)
solid-state detectors that convert x-rays into electrical signals
similar to digital cameras
seen on a computer screen or printed on special film similar to
conventional mammograms
patients POV same as conventional
COMPUTER-AIDED DETECTION
digitized mammographic image that can be obtained from either a
conventional film mammogram or a digitally acquired mammogram
computer software then searches for abnormal areas of density,
mass, or calcification that may indicate the presence of cancer
highlighted parts
BREAST TOMOSYNTHESIS
3-D breast imaging
x-ray tube and imaging plate move during the exposure
creates a series of thin slices through the breast that allow for
improved detection of cancer and fewer patients recalled for
additional imaging
BREAST NODULE BIOPSY
removes a sample of breast tissue seen under microscope to know if (+) breast
cancer cancer cells
usually done to check a lump found during a breast examination or a suspicious
area found on a mammogram, ultrasound, or magnetic resonance imaging (MRI)
Types:
FINE-NEEDLE ASPIRATION BIOPSY - a thin needle is inserted into a
lump and removes a sample of cells or fluid
CORE NEEDLE BIOPSY - a needle with a special tip is inserted and
removes a sample of breast tissue about the size of a grain of rice
22 | P a g e
VACUUM-ASSISTED CORE BIOPSY - done with a probe that uses a
gentle vacuum to remove a small sample of breast tissue
- The single small cut doesn't require stitches and leaves a very small
scar.
OPEN (SURGICAL) BIOPSY - a small cut is done in the skin and breast
tissue to remove part or all of a lump
- This may be done as a first step to check a lump or if a needle biopsy
doesn't provide enough information
If needed, may use ultrasound or MRI to guide the biopsy needle
May use a computer to locate the exact spot for the biopsy sample from
mammograms that have been taken from two angles (stereotactic needle biopsy)
A fine wire, clip, or marker also may be used to mark the site
Only reliable way to see if cancer cells are present
Check! If the patient:
Is taking any medicines.
Is allergic to any medicines, including anesthetics.
Is allergic to latex.
Has any bleeding problems or is taking blood thinners, such as warfarin
(Coumadin) or clopidogrel (Plavix).
Is or might be pregnant.
XI. MEDICAL AND SURGICAL MANAGEMENT
In general, the course of treatment is determined by the stage of the cancer.
Stages range from I to IV based on the cancer's specific characteristics, such as
whether it has spread beyond the ovaries.
A. CHEMOTHERAPEUTIC DRUGS
Carboplatin: An anticancer drug ("antineoplastic" or "cytotoxic")
chemotherapy drug. Carboplatin is classified as an "alkylating agent."
Indication:
- Carboplatin is used to treat ovarian cancer.
- Carboplatin is also used for other types of cancer, including lung, head
and neck, endometrial, esophageal, bladder, breast, and cervical;
central nervous system or germ cell tumors; osteogenic sarcoma; and
as preparation for a stem cell or bone marrow transplant.
Side effects:
- Low blood counts (nadir)
- n/v
- taste changes
- hair loss
- weakness
- blood test abnormalities
23 | P a g e
Docetaxel: An anti-cancer ("antineoplastic" or "cytotoxic") chemotherapy
drug. This medication is classified as a "plant alkaloid," a "taxane" and an
"antimicrotubule agent."
Indication:
- Approved in treatment of breast cancer, non-small cell lung cancer,
advanced stomach cancer, head and neck cancer and metastatic
prostate cancer.
- Also being investigated to treat small cell lung, ovarian, bladder, and
pancreatic cancers, soft tissue sarcoma and melanoma.
Side effects
- Low white blood cell count. (This can increase your risk for infection)
- Low red blood cell count (anemia)Fluid retention with weight gain,
swelling of the ankles or abdominal area.
- Peripheral neuropathy (numbness in your fingers and toes) may occur
with repeated doses. This should be reported to your healthcare
provider.
- Nausea
- Diarrhea
- Mouth sores
- Hair loss
- Fatigue and weakness
- Infection
- Nail changes (Color changes to your fingernails or toenails may occur
while taking docetaxel. In extreme, but rare, cases nails may fall off.
After you have finished docetaxel treatments, your nails will generally
grow back) (see skin problems).
B. SURGICAL MANAGEMENT
Surgery is the main treatment for ovarian cancer. It is used to treat all stages of
ovarian cancer. For earlier stage ovarian cancer, it may be the only treatment.
Surgery involves:
1. Removal of both ovaries and fallopian tubes (bilateral salpingo-oophorectomy)
2. Partial or complete removal of the omentum, the fatty layer that covers and pads
organs in the abdomen
3. Oophorectomy, a surgical procedure to remove one or both ovaries. The ovaries
contain eggs and produce hormones that control your menstrual cycle.
Oophorectomy can be done alone, but it is often done as part of a larger surgery
to remove the uterus (hysterectomy) in women who have undergone
menopause. Oophorectomy is also commonly combined with surgery to remove
the nearby fallopian tubes (salpingectomy), since they share a common blood
supply with the ovaries. When combined, the procedure is called salpingo-
oophorectomy.
24 | P a g e
4. Examination, biopsy, or removal of the lymph nodes and other tissues in the
pelvis and abdomen
Following surgery, women with higher-stage tumors may receive chemotherapy.
It is used to treat any remaining disease and can also be used if there is recurrent
cancer. Chemotherapy is a drug treatment that uses powerful chemicals to kill fast-
growing cells in the body. Though chemotherapy is an effective way to treat many
types of cancer, chemotherapy treatment also carries a risk of side effects. Some
chemotherapy side effects are mild and treatable, while others can cause serious
complications.
After surgery and chemotherapy, patients should have:
1. A physical exam (including pelvic exam) every 2 - 4 months for the first 2
years, followed by every 6 months for 3 years, and then annually
2. A CA-125 blood test at each visit if the level was initially high
3. A computed tomography (CT) scan of the chest, abdomen, and pelvic area
and a chest x-ray.
25 | P a g e
XII. NURSING CARE PLANS:
Assessement Nursing
Diagnosis
Scientific
Rationale
Objectives Planning Scientific Rationale Evaluation
With
abdominal
enlargement
With dyspnea
Bloatedness
Nasal flaring
with
intercostals
retraction
RR: 26 bpm
Lagging on the
left hemi-
diaphragm
Decrease
tactile fremiti
on the left
Decreased
breath sounds
on left lung
field
AC: 68 cm
(+) fluid wave
Ineffective
breathing
pattern related
to compression
of diaphragm
secondary to
peritoneal fluid
accumulation
Ineffective
breathing
pattern
happens when
the inspiration
and/or
expiration does
not provide
adequate
ventilation.
The increasing
amount of fluid
in the peritoneal
cavity presses
the diaphragm
limiting lung
expansion
therefore
leading to
ineffective
breathing
pattern.
By the end of 4
hours of nursing
intervention, the
patient should be
able to:
demonstrate
proper deep
breathing
exercises
show an
improvement in
her respiratory
pattern as
evidenced by
the absence of
signs and
symptoms of
hypoxia
verbalize
awareness of
causative factors
Independent:
1. Encourage
adequate rest
periods
between
activities
2. Elevate HOB
and/or have
client sit up in a
chair, as
appropriate
3. Encourage
slower/ deeper
respirations
such as the use
of the pursed-lip
technique
4. Maintain a calm
attitude when
dealing with
client
5. Advise to avoid
overeating or
gas-forming
foods
1. To limit fatigue and
decrease oxygen
demand.
2. To promote
physiological/
psychological ease
of maximal
inspiration
3. To promote
optimum lung
expansion and
effective
respiration.
4. Limits anxiety level
and decrease
oxygen demand.
5. May cause
abdominal
distention
At the end of 4
hours of nursing
intervention, the
patient was able to:
Establish a
normal /
effective
respiratory
pattern as
evidenced by
the absence of
sign and
symptoms of
hypoxia
Demonstrated
proper
breathing
pattern
Verbalized
awareness of
causative
factors
26 | P a g e
6. Stress
importance of
good posture
and effective
use of
accessory
muscles
7. Discuss the
possible cause
of difficulty
breathing
Dependent:
8. Hook to oxygen
as ordered
9. Monitor oxygen
saturation with
pulse oximeter
as indicated.
10. Medicate with
analgesics as
appropriate
6. To maximize
respiratory effort
7. Decreases anxiety
level
8. To provide proper
oxygenation.
9. To verify
maintenance/
improvement in O2
saturation
10. To promote
deeper
respiration and
decrease oxygen
demand.
27 | P a g e
Assessment Diagnosis Scientific Rationale Objective Intervention Rationale Evaluation
Grade 2
bipedal edema
(+) venous
congestion
BP = 170 / 90
PP = 80
MAP = 117
PR = 113
HPN for 8
years
DM for 2 years
Ineffective tissue
perfusion related
to decreased
blood oxygen
supply
secondary to
increased
peripheral
vascular
resistance
In order to ensure
maximal organ
functioning, adequate
blood supply is
necessary. In patients
with hypertension,
there is increased
peripheral vascular
resistance due to
vasoconstriction. This
is further worsened by
diabetes mellitus
wherein blood
becomes viscous thus
requiring a greater
effort for the heart to
pump blood and
deliver systemic
supply. When there is
ineffective tissue
perfusion, the body
tries to compensate
by increasing blood
pressure and MAP,
and widening the
pulse pressure.
Short-term
After 5 hours of
nursing interventions,
the patient will be
able to:
Manifest a
decrease in the
severity of edema
Show signs of
improved perfusion
as seen by a
decrease in BP,
MAP, and PP
Long-term
After the 2 weeks of
nursing intervention,
the patient will be
able to:
Demonstrate
adequate
perfusion, as
evidenced by
stable vital signs,
palpable pulses,
good capillary refill,
usual mentation,
and individually
adequate urinary
output.
1. Elevate legs but
maintain semi-
high fowlers
position
2. Apply warm
compress to
extremity with
edema
3. Turn client and
encourage
frequent AROM
exercises.
4. Assist with and
instruct in foot
and leg
exercises and
ambulate as
soon as able.
5. Note erythema,
swelling of
extremity, or
reports of
sudden chest
pain with
dyspnea
1. Helps lessen
edema and
direct
circulation to
vital organs
2. Doing this
results to
vasodilation
that will help
lessen edema
3. Prevents stasis
of secretions
and respiratory
complications
4. Movement
enhances
circulation and
prevents stasis
complications.
5. May be
indicative of
development of
thrombophlebiti
s and
pulmonary
embolus
Short-term
After 2 hours of
nursing interventions,
the patient was able
to:
Manifest a
decrease in the
severity of edema
Show signs of
improved perfusion
as seen by a
decrease in BP,
MAP, and PP
Long-term
After the 2 weeks of
nursing intervention,
the patient was be
able to:
Demonstrate
adequate
perfusion, as
evidenced by
stable vital signs,
palpable pulses,
good capillary refill,
usual mentation,
and adequate
urinary output.
28 | P a g e
Be free of edema
and signs of
thrombus
formation.
6. Educate the
client regarding
underlying
disease
processes that
may have
contributed to
her problem
6. Promotes better
understanding
of disease
condition and
helps client
accept
implications of
disease
Be free of edema
and signs of
thrombus
formation.
29 | P a g e
Assessment Diagnosis Scientific
Rationale
Objective Intervention Rationale Evaluation
(+) progressive
weight loss
Irregularities in
menstruation
Abdominal
enlargement
Anorexia
Early satiety
Bloatedness
Epigastric pain
Nausea
Vomiting
Progressive
abdominal
enlargement
Pain RLQ
BMI = 15
Bulging planks
(+) fluid wave
AC = 68cm
Imbalanced
Nutrition:
Less than
body
requirement
s related to
poor food
intake
secondary to
disease
process
Abdominal
enlargement
causes
compression
of the GI
tract which
yields to
early satiety,
bloatedness,
and
epigastric
pain. This
often leads
to loss of
appetite
causing
poor food
intake.
Furthermore
, nausea
and
vomiting,
especially if
it happens in
increased
frequencies,
can lead to
further
depletion of
nutrients.
Short-term
After the shift, the
patient will:
Understand
health teachings
given regarding
diet
Able to eat
properly with
accordance to
diet prescribed by
the dietician
Verbalize
commitment to
achieving dietary
goals
Long-term
After the 4 weeks of
nursing intervention,
the patient will be
able to:
Meet Caloric
Requirements
Demonstrate
progressive weight
1. Emphasize
importance of well-
balanced, nutritious
intake. Provide
information
regarding individual
nutritional needs
2. Discuss eating
habits, including
food preferences,
intolerances, or
aversions
3. Note age, body
build, strength,
activity/rest level,
and other factors
that may affect food
intake
4. Promote adequate
and timely fluid
intake
5. Weigh regularly at
the same time with
the same clothing
6. Encourage small
frequent feeding if
unable to tolerate
large amount of
1. To make client
realize importance
of maintaining a
well-balanced diet
to ensure optimal
health
2. To appeal to
clients likes or
dislikes
3. To help in
determining
nutritional needs
4. To reduce
possibility of early
satiety
5. To monitor
effectiveness of
dieting plan
6. Prevents stomach
upset and
distention which
makes food more
Short-term
After the shift the
patient was able to:
Verbalize
understanding
regarding health
teachings given
concerning her diet
Eat properly with
accordance to diet
prescribed by the
dietician
Verbalize lifestyle
changes to regain
appropriate weight
Verbalize
commitment to
achieving dietary
goals
Long-term
After the 4 weeks of
nursing intervention,
the patient was be
able to:
Meet Caloric
30 | P a g e
gain
Continuously follow
health teachings
given regarding diet
Demonstrate BMI
>15 or in normal
range (18-24.9)
food in a single
meal
7. Encouraged intake
of high-calorie and
high-protein foods
8. Limit fiber.
9. Prevent or
minimize
unpleasant odors
and sights
10. Develop
consistent, realistic
weight goal with
client
11. Consult dietician
for long term
needs
tolerable.
7. To ensure that
nutritional needs
are met
8. May lead to early
satiety
9. May have
negative effect on
appetite and
eating
10. To develop a
good, consistent
progression of
weight gain
11. To assess long-
term needs
Requirements
Demonstrate
progressive weight
gain
BMI = 16.5
You might also like
- Hijama (Cupping) Treatment Points PDFDocument18 pagesHijama (Cupping) Treatment Points PDFMohammed Afsar90% (49)
- Anatomy and Physiology of Female Reproductive SystemDocument12 pagesAnatomy and Physiology of Female Reproductive SystemSyed Isamil100% (1)
- Female Reproductive SystemDocument75 pagesFemale Reproductive SystemProf Lina Ramli67% (3)
- GynaDocument22 pagesGynaIGA ABRAHAMNo ratings yet
- Anatomy and Physiology of Reproductive SystemDocument93 pagesAnatomy and Physiology of Reproductive SystemMelizza Fajardo BañanoNo ratings yet
- BIOLOGYDocument6 pagesBIOLOGYCLANSIE BUXTON CHIKUMBENo ratings yet
- Anatomy and Physiology Reproductive SystemDocument91 pagesAnatomy and Physiology Reproductive SystemApril BenaventeNo ratings yet
- REWIEW OF FEMALE REPRODUCTIVE SYSTEM NewDocument49 pagesREWIEW OF FEMALE REPRODUCTIVE SYSTEM NewnamitaNo ratings yet
- Anatomy and PhysiologyDocument8 pagesAnatomy and PhysiologyAironne ManguilimotanNo ratings yet
- Anatomy and Physiology of Female Reproductive System: External Generative OrgansDocument28 pagesAnatomy and Physiology of Female Reproductive System: External Generative OrgansAlmira Gamao100% (1)
- Female RSsystem 2Document90 pagesFemale RSsystem 2icliftonguytonNo ratings yet
- Anatomy and Physiology of Female Reproductive SystemDocument67 pagesAnatomy and Physiology of Female Reproductive Systemannu panchalNo ratings yet
- Anatomy and PhysiologyDocument5 pagesAnatomy and Physiologychinchin ramosNo ratings yet
- Female Reproductive System (Yuni)Document36 pagesFemale Reproductive System (Yuni)Ayi Abdul BasithNo ratings yet
- Maternal & Child Nursing ANATOMY & PHYSIOLOGY SECTION 1Document102 pagesMaternal & Child Nursing ANATOMY & PHYSIOLOGY SECTION 1emma rose lutella100% (1)
- Presented By, P.Jeyanthi, M.SC (N) I Year Apollo CONDocument67 pagesPresented By, P.Jeyanthi, M.SC (N) I Year Apollo CONPaul AndersonNo ratings yet
- Female RSystemDocument71 pagesFemale RSystemicliftonguytonNo ratings yet
- Final Module in M101Document56 pagesFinal Module in M101J. TSNo ratings yet
- Final Module in M101 1Document54 pagesFinal Module in M101 1J. TSNo ratings yet
- Presentation On: Female Reproductive SystemDocument54 pagesPresentation On: Female Reproductive SystemLetsShop BbsrNo ratings yet
- Anatomy of The Female ReproductionDocument108 pagesAnatomy of The Female ReproductionDaisy HamdaliNo ratings yet
- Unit XDocument18 pagesUnit XPreeti ChouhanNo ratings yet
- Anatomy and Physiology of Female Reproductive SystemDocument42 pagesAnatomy and Physiology of Female Reproductive SystemLiangkiuwiliuNo ratings yet
- Anatomy of Female Reproductive SystemDocument14 pagesAnatomy of Female Reproductive SystemkukadiyaNo ratings yet
- Anatomy and Physiology of Female Reproductive SystemDocument6 pagesAnatomy and Physiology of Female Reproductive SystemFarlyn Real MoralesNo ratings yet
- Anatomy and PhysiologyDocument7 pagesAnatomy and PhysiologyKristine Alejandro100% (1)
- Reproductive SystemDocument43 pagesReproductive SystemDoc Zay VillafuerteNo ratings yet
- Female Reproductive System PDFDocument48 pagesFemale Reproductive System PDFTeppy the GreatNo ratings yet
- Obs-Gyn Final 2019Document169 pagesObs-Gyn Final 2019koalakid55No ratings yet
- Anatomy and Physiology - EctopicDocument4 pagesAnatomy and Physiology - EctopicReyzelinNo ratings yet
- Operative Review TAHBSODocument22 pagesOperative Review TAHBSOGinger Enireht HTaibNo ratings yet
- A Case Study About Cervical PolypsDocument8 pagesA Case Study About Cervical PolypsJisel-Apple BulanNo ratings yet
- Anatomy and PhysiologyDocument8 pagesAnatomy and PhysiologyG3-PORTILLA John MartNo ratings yet
- Female Genital Tract and The Pelvic BonesDocument37 pagesFemale Genital Tract and The Pelvic Bonesعبد الله الحربيNo ratings yet
- PT Physiology of PuerperiumDocument14 pagesPT Physiology of PuerperiumPragati BholeNo ratings yet
- Minor Discomfort and Complications of Puerperium (1) - Converted654Document57 pagesMinor Discomfort and Complications of Puerperium (1) - Converted654Pragati BholeNo ratings yet
- Female Reproductive AnatomyDocument34 pagesFemale Reproductive AnatomyAswin Dwi PrayudiNo ratings yet
- Screenshot 2022-03-28 at 10.17.47 PMDocument127 pagesScreenshot 2022-03-28 at 10.17.47 PMqdvvqvxn7gNo ratings yet
- Ana & PhysioDocument3 pagesAna & PhysioarzeManzanoNo ratings yet
- Female ReproductiveDocument55 pagesFemale ReproductiveDenise RegalaNo ratings yet
- Anatomy and Physiology CompleteDocument9 pagesAnatomy and Physiology CompleteJohn BretanaNo ratings yet
- Anatomy Physiology of Female Reproductive SystemDocument96 pagesAnatomy Physiology of Female Reproductive SystemRabin BasnetNo ratings yet
- Anatomy & Physiology of Female Reproductive System Lecturer .Mahabad.M.koyiDocument36 pagesAnatomy & Physiology of Female Reproductive System Lecturer .Mahabad.M.koyiKarwan DilmanyNo ratings yet
- A and P of FRSDocument13 pagesA and P of FRSAjay DNo ratings yet
- Pandapatan Paler AnaPhyDocument3 pagesPandapatan Paler AnaPhyShara Lailanie A. AzisNo ratings yet
- Anatomy and Physiology Reproductive System: ComponentsDocument7 pagesAnatomy and Physiology Reproductive System: ComponentsMark Nel Nuñez100% (1)
- Female Reproductive System Anatomy and PhysiologyDocument5 pagesFemale Reproductive System Anatomy and PhysiologyIkea Balhon100% (3)
- 2 Anatomy and PhysiologyDocument11 pages2 Anatomy and PhysiologyAYO NELSONNo ratings yet
- Introduction To Women HealthDocument47 pagesIntroduction To Women HealthDarren LimNo ratings yet
- C CCCCC CCCC C C CC C C C C C CCCCCCCCCCCC CCC CC CCCCCCCCCCC CCCC!CC"CCC C C CCCCC CCCCCCCC CC C CCCCCC#CCCCC CC C CCCCC CCCCC C C C CC CCCC#C C CCCCCC C $CCCCC C %C C&C 'CCCDocument4 pagesC CCCCC CCCC C C CC C C C C C CCCCCCCCCCCC CCC CC CCCCCCCCCCC CCCC!CC"CCC C C CCCCC CCCCCCCC CC C CCCCCC#CCCCC CC C CCCCC CCCCC C C C CC CCCC#C C CCCCCC C $CCCCC C %C C&C 'CCCJona Phie Domingo MonteroNo ratings yet
- Female Reproductive SystemDocument7 pagesFemale Reproductive SystemjonaNo ratings yet
- Anatomy Lec 22 (FGOs)Document49 pagesAnatomy Lec 22 (FGOs)Humraz100% (1)
- Uterus AnatomyDocument7 pagesUterus AnatomyJoseph RadislaoNo ratings yet
- Mayo MaDocument23 pagesMayo Madextroid12No ratings yet
- Assessment and Health PromotionDocument24 pagesAssessment and Health PromotionGladys YaresNo ratings yet
- X. Anatomy & Physiology Cervix: VaginaDocument8 pagesX. Anatomy & Physiology Cervix: VaginaNicaMariannePañaNo ratings yet
- Anatomy and Physiology of Reproduction: Female Reproduction Male ReproductionDocument15 pagesAnatomy and Physiology of Reproduction: Female Reproduction Male ReproductionMhiahLine TolentinoNo ratings yet
- ANATOMY OF FEMALE InternalDocument49 pagesANATOMY OF FEMALE InternalJohaifha CompaniaNo ratings yet
- Health & Health PromotionDocument110 pagesHealth & Health Promotionlhedaven100% (1)
- Temperature DataDocument5 pagesTemperature DatalhedavenNo ratings yet
- Temperature DataDocument5 pagesTemperature DatalhedavenNo ratings yet
- Metal Extraction DataDocument6 pagesMetal Extraction DatalhedavenNo ratings yet
- PSI ED Machines Loading Set-UpDocument15 pagesPSI ED Machines Loading Set-UplhedavenNo ratings yet
- ED7 Frame Discoloration (Pre & Post ED) - Set2-11 03 2016Document18 pagesED7 Frame Discoloration (Pre & Post ED) - Set2-11 03 2016lhedavenNo ratings yet
- MDF PDFDocument2 pagesMDF PDFghailNo ratings yet
- Company SmoothmovesDocument2 pagesCompany SmoothmoveslhedavenNo ratings yet
- Q4151228 - 1 - EC Metal Fab&Rework PDFDocument1 pageQ4151228 - 1 - EC Metal Fab&Rework PDFlhedavenNo ratings yet
- Q4151228 - 1 - EC Metal Fab&Rework PDFDocument1 pageQ4151228 - 1 - EC Metal Fab&Rework PDFlhedavenNo ratings yet
- Christmas Street Party - LetterDocument2 pagesChristmas Street Party - LetterlhedavenNo ratings yet
- Nilo CV 2012Document9 pagesNilo CV 2012lhedavenNo ratings yet
- Smart and Globe PasswordDocument1 pageSmart and Globe PasswordlhedavenNo ratings yet
- Q4151228 - 1 - EC Metal Fab&ReworkDocument1 pageQ4151228 - 1 - EC Metal Fab&ReworklhedavenNo ratings yet
- Member's Data Form (MDF, Hqp-pff-039, V04.1)Document5 pagesMember's Data Form (MDF, Hqp-pff-039, V04.1)Ron Villanueva0% (1)
- Quotation: 1775 D Purok 5 Brgy. Sto. Tomas Binan Laguna Tel No: (049) 250-6033 Email AddDocument1 pageQuotation: 1775 D Purok 5 Brgy. Sto. Tomas Binan Laguna Tel No: (049) 250-6033 Email AddlhedavenNo ratings yet
- Qualification of Forming Tool 12.31.15Document1 pageQualification of Forming Tool 12.31.15lhedavenNo ratings yet
- 'Love of My Life''Document5 pages'Love of My Life''lhedavenNo ratings yet
- Teaching Demonstration RubricDocument3 pagesTeaching Demonstration Rubriclhedaven100% (1)
- A3397a (30ld Pdip) Strip Measurement 2Document1 pageA3397a (30ld Pdip) Strip Measurement 2lhedavenNo ratings yet
- The Problem and Its BackgroundDocument68 pagesThe Problem and Its BackgroundlhedavenNo ratings yet
- April 4, 2016: Jamester J Carlo D.V. Dela Cruz 2014677392, BS TOURISMDocument1 pageApril 4, 2016: Jamester J Carlo D.V. Dela Cruz 2014677392, BS TOURISMlhedavenNo ratings yet
- Practicum Visit FormDocument2 pagesPracticum Visit FormlhedavenNo ratings yet
- AlfieDocument1 pageAlfielhedavenNo ratings yet
- Thesis For Accreditation Page 10 and 11 OnlyDocument61 pagesThesis For Accreditation Page 10 and 11 Onlylhedaven0% (1)
- 2016 RN DetTestPlan EducatorDocument67 pages2016 RN DetTestPlan EducatorshambruceNo ratings yet
- Engineer BatuigasDocument1 pageEngineer BatuigaslhedavenNo ratings yet
- Bushong Review Q 25 28Document10 pagesBushong Review Q 25 28lhedavenNo ratings yet
- Professional Regulation CommissionDocument2 pagesProfessional Regulation CommissionlhedavenNo ratings yet
- Lunacy in The 19th Century PDFDocument10 pagesLunacy in The 19th Century PDFLuo JunyangNo ratings yet
- Pretest and PosttestDocument3 pagesPretest and PosttestMarissa FontanilNo ratings yet
- 09 Touch of His GarmentDocument32 pages09 Touch of His GarmentOrlando BalagotNo ratings yet
- AUB Classification - FIGODocument8 pagesAUB Classification - FIGOjeansabalosNo ratings yet
- Acupuncture For Primary Dysmenorrhea A Randomized Controlled TrialDocument3 pagesAcupuncture For Primary Dysmenorrhea A Randomized Controlled TrialAnnis RohmawatiNo ratings yet
- Endometriosis: DR OMBAKU Kingsley Sama DR SakinatouDocument99 pagesEndometriosis: DR OMBAKU Kingsley Sama DR SakinatouOmbaku KingsleyNo ratings yet
- Fitri Hana Sukma - UASDocument10 pagesFitri Hana Sukma - UASfitri hanaNo ratings yet
- Day 14 NCM 109 FE AdolescentDocument57 pagesDay 14 NCM 109 FE AdolescentSheena Patricia ArasulaNo ratings yet
- Acceptance, Awareness and Management of Menstruation:: A Challenge For Safeguarding Rights of Girl ChildDocument25 pagesAcceptance, Awareness and Management of Menstruation:: A Challenge For Safeguarding Rights of Girl ChildrohitNo ratings yet
- History Taking and Physical Examination in GynaecologyDocument41 pagesHistory Taking and Physical Examination in GynaecologygimNo ratings yet
- Endometriosis - Clinical Features - Diangosis - TeachMeObGynDocument3 pagesEndometriosis - Clinical Features - Diangosis - TeachMeObGynLiridon SopajNo ratings yet
- 101-Article Text-772-1-10-20180918Document7 pages101-Article Text-772-1-10-20180918Sinta Widyawati IINo ratings yet
- Maria Garcia Dolphin Pose (Ardha Pincha Mayurasana) & Plough Pose (Halasana) Spring 2016 M 2:30-4:00Document5 pagesMaria Garcia Dolphin Pose (Ardha Pincha Mayurasana) & Plough Pose (Halasana) Spring 2016 M 2:30-4:00api-301722320No ratings yet
- Family Study: Shefali Rawat BATCH 2017 Serial No.114Document24 pagesFamily Study: Shefali Rawat BATCH 2017 Serial No.114Shefali RawatNo ratings yet
- 1 JGK 2023Document12 pages1 JGK 2023Agus KarismaNo ratings yet
- The Ritual Ablutions For WomenDocument24 pagesThe Ritual Ablutions For WomenShahid.Khan1982No ratings yet
- ZoloftDocument26 pagesZoloftgofastjayNo ratings yet
- Abnomal Uterine Bleeding in Premenopausal Women AAFPDocument9 pagesAbnomal Uterine Bleeding in Premenopausal Women AAFPAliNasrallahNo ratings yet
- Abnormal Uterine BleedingDocument13 pagesAbnormal Uterine BleedingratnacantikNo ratings yet
- Akhdari English SaidyDocument17 pagesAkhdari English SaidyOltrasNo ratings yet
- Xi-Cleft Points TheoryDocument6 pagesXi-Cleft Points TheoryKarthikeyan Nanjappan100% (2)
- Comprehensive Medical Assisting Administrative and Clinical Competencies 6th Edition Lindh Test BankDocument36 pagesComprehensive Medical Assisting Administrative and Clinical Competencies 6th Edition Lindh Test Bankabetterguerillal4o2100% (28)
- Maternal Child Nursing ExaminationDocument14 pagesMaternal Child Nursing Examinationjames_manuel11187084100% (1)
- Gynecology GY Emtyaz Quiz JordanDocument40 pagesGynecology GY Emtyaz Quiz JordanVicviclookThekingNo ratings yet
- Soal Usulan UnHas Juli 2019Document25 pagesSoal Usulan UnHas Juli 2019Ibnu SinaNo ratings yet
- Sex, by Henry Stanton 1Document56 pagesSex, by Henry Stanton 1luckyreads67% (3)
- Why Do You Have Hemorrhagic Ovarian Cyst?Document1 pageWhy Do You Have Hemorrhagic Ovarian Cyst?ovariancyst1hemoNo ratings yet
- Kasus Ujian PhantomDocument4 pagesKasus Ujian PhantomMishael Octaviany JirehNo ratings yet
- Bullets For Nursing Basic Concepts Part 15Document61 pagesBullets For Nursing Basic Concepts Part 15oh_chamieNo ratings yet