Professional Documents
Culture Documents
Neumonía de La Comunidad
Uploaded by
Felipe CeaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Neumonía de La Comunidad
Uploaded by
Felipe CeaCopyright:
Available Formats
Felipe Martnez Lomakin
Programa de Especializacin en Medicina Interna
Neumona
Adquirida en la Comunidad
mircoles 17 de agosto de 11
Neumona
Introduccin
Conceptos Generales
Diagnstico frecuentemente accesible desde la clnica y la radiografa de trax.
- Distinciones en diagnstico diferencial ms difciles de obtener.
Microbiologa de difcil tipicacin
- Seleccin de terapia ms bien emprica segn caractersticas del enfermo y ora local.
Determinar el riesgo de cada episodio es crucial para un manejo apropiado.
- Escalas de riesgo validadas orientan al tratamiento ms adecuado.
Moran G, Talan D, Abrahamian F - Diagnosis and management of pneumonia in the emergency department
Infectious Disease Clinics of North America 2008 vol. 22 (1) pp. 53-72, vi
Lionel A Mandell, Richard G Wunderink, Antonio Anzueto,, et Al - Infectious Diseases Society of America/American Thoracic Society consensus
guidelines on the management of community-acquired pneumonia in adults
Clinical Infectious Diseases 2007 vol. 44 Suppl 2 pp. S27-72
Denicin
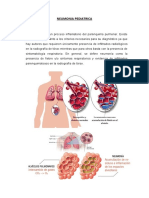
Inamacin del espacio alveolar con acumulacin de clulas inamatorias y
secreciones en el espacio del mismo que dicultan el intercambio gaseoso
mircoles 17 de agosto de 11
Neumona
Epidemiologa
Magnitud del Problema
Una enfermedad frecuente (y grave) a nivel mundial.
- Cuatro millones de casos por ao, un 25% hospitalizados, en Estados Unidos.
- Incidencia de 2 a 15 casos / 1000 habitantes con cambios por edad.
- Primera causa de muerte por enfermedad infecciosa en Chile y Estados Unidos.
Mortalidad variable segn sitio de cuidado.
- Ambulatorio: <1-3% de los pacientes.
- Hospitalizados en sala comn: 14%.
- Unidades de Cuidados Intensivos: 20 al 50%.
Carga importante para sistemas de salud: 8.4 billones de dlares anuales en Estados Unidos.
Moran G, Talan D, Abrahamian F - Diagnosis and management of pneumonia in the emergency department
Infectious Disease Clinics of North America 2008 vol. 22 (1) pp. 53-72, vi
Lionel A Mandell, Richard G Wunderink, Antonio Anzueto,, et Al - Infectious Diseases Society of America/American Thoracic Society consensus
guidelines on the management of community-acquired pneumonia in adults
Clinical Infectious Diseases 2007 vol. 44 Suppl 2 pp. S27-72
Lim WS, Bauddouin RC, George A, et Al. - BTS guidelines for the management of community acquired pneumonia in adults: update 2009
Thorax 2009 vol. 64 Suppl 3 pp. iii1-55
mircoles 17 de agosto de 11
Neumona
Epidemiologa
Jokinen C, Heiskanen L, Juvonen H, et al - Incidence of community- acquired pneumonia in the population of four municipalities in eastern Finland
American Journal of Epidemiology 1993; 137 - 977 - 988
Incidencia de Neumona
Seminar
2 www.thelancet.com Published online March 23, 2011 DOI:10.1016/S0140-6736(10)61459-6
of antibodies in paired serum samples. Introduction of
PCR has increased the ability to detect respiratory viruses,
including those that are di cult to culture. At least
26 viruses have now been associated with community-
acquired pneumonia (panel).
Despite technological advances, establishing the cause
of pneumonia remains challenging.
13
Specimens from
the lower-respiratory tract can be hard to obtain, and
distinguishing possible prolonged shedding or
colonisation from infection can be di cult. For diagnosis
of viral pneumonia, reliance on testing of nasopharyngeal
specimens presents its own challenges; detection of a
virus in the nasopharynx could represent coincidental
upper-respiratory infection or a pneumonia pathogen.
Measurement of background prevalence of asymptomatic
nasopharyngeal viral infection in a control group might
help to clarify the size of this diagnostic issue at a
population level, but this approach has been used only
rarely in aetiological studies. Furthermore, most research
has focused on patients admitted to hospital and,
therefore, ndings might not be representative of mild-
to-moderate disease.
Several dierent types of specimen from the upper and
lower airway have been used in aetiological studies of
community-acquired pneumonia, including: naso-
pharyngeal aspirates or washes; swabs from the
nasopharynx, nose, or throat; combined nasopharygeal
and throat swabs; expectorated and induced sputum;
tracheal aspirates; bronchoalveolar lavage; and lung
puncture.
14,15
Recovery of virus uctuates according to
specimen type, which probably accounts for some of the
variability of ndings between studies.
Most studies of the cause of viral pneumonia have
used upper-respiratory specimens to test for viruses. In
children, nasopharyngeal aspirates are generally deemed
the specimen of choice because both nasal and
nasopharyngeal mucus samples are gathered. Respira-
tory viruses have been noted in 95% of mucus samples
obtained by nasopharyngeal aspiration from children
with respiratory infection.
16
Obtaining an aspirate is,
however, unpleasant and requires a suction device.
Nasal swabs taken with a sterile cotton swab from a
depth of 23 cm have comparable sensitivity to
nasopharyngeal aspirates for culture of all major
respiratory viruses, except respiratory syncytial virus.
17
Flocked swabs with nylon bres in a perpendicular
fashion are now preferred by many clinicians because
they are convenient to use and have a similar sensitivity
to nasopharyngeal aspirates for detection by PCR of
respiratory viruses.
15,17,18
In adults, nasopharyngeal swabs
have a higher sensitivity than throat swabs, but they can
be less sensitive than nasopharyngeal washes.
14
Transnasal nasopharyngeal ocked swabs also have
high virus detection rates in adults.
19,20
Lower-respiratory specimens have obvious advantages
for establishing the cause of pneumonia because they
come from the site of infection. However, obtaining
reliable specimens that are not contaminated by ora
from the upper airway is di cult. Induced sputum
specimens have been used in paediatric pneumonia
studies, although assuring that the specimens are
representative of the lower-respiratory tract can be
challenging.
21
High-quality specimens can be obtained by
thoracic needle aspiration, but this technique has not
been adopted widely because of safety concerns, despite
a low complication rate.
22,23
In general, PCR-based methods are between two and
ve times more sensitive than conventional virus
diagnostic methods (culture, antigen detection, and
serological assays) for detection of respiratory viruses.
0 15 30 45 60 75
0
20
40
60
80
I
n
c
i
d
e
n
c
e
(
p
e
r
1
0
0
0
p
o
p
u
l
t
i
o
n
p
e
r
y
e
a
r
)
Age (years)
Figure : Age-specic incidence of community-acquired pneumonia
Error bars=95% CIs. Modied from reference 8 with permission of Oxford
University Press.
Panel: Viruses linked to community-acquired pneumonia
in children and adults
Respiratory syncytial virus
Rhinovirus
Inuenza A, B, and C viruses
Human metapneumovirus
Parainuenza viruses types 1, 2, 3, and 4
Human bocavirus*
Coronavirus types 229E, OC43, NL63, HKU1, SARS
Adenovirus
Enteroviruses
Varicella-zoster virus
Hantavirus
Parechoviruses
Epstein-Barr virus
Human herpesvirus 6 and 7
Herpes simplex virus
Mimivirus
Cytomegalovirus
Measles
*Mostly in children. Mostly in developing countries.
Olli Ruuskanen, Elina Lahti, Lance C Jennings, David R Murdoch - Viral Pneumonia
The Lancet 2011 vol. 22 (1) pp. 53-72, vi
12 / 1000 hab
Incidencia Promedio
mircoles 17 de agosto de 11
Neumona
Diagnstico
Moran G, Talan D, Abrahamian F - Diagnosis and management of pneumonia in the emergency department
Infectious Disease Clinics of North America 2008 vol. 22 (1) pp. 53-72, vi
Lionel A Mandell, Richard G Wunderink, Antonio Anzueto,, et Al - Infectious Diseases Society of America/American Thoracic Society consensus
guidelines on the management of community-acquired pneumonia in adults
Clinical Infectious Diseases 2007 vol. 44 Suppl 2 pp. S27-72
Pilares Bsicos
Ocasionalmente
Micro
biologa
Manifestaciones
Clnicas
Imgenes
Siempre?
M Nawal Lutyya, Eric Henley, Linda F Chang, Stephanie Wessel Reyburn- Diagnosis and Treatment of Community - Acquired Pneumonia
American Family Physician 2006 vol. 73 (3) pp. 442-50
mircoles 17 de agosto de 11
Neumona
Manifestaciones Clnicas
Generalidades
El pilar fundamental en el diagnstico de neumona.
- BTS: Basta diagnstico clnico en atencin primaria
- Otras sociedades indican que la radiografa es mandatoria para conrmacin (40% de acierto).
Manifestaciones asociadas incrementan probabilidad de neumona.
- Taquipnea > 25 respiraciones por minuto.
- Fiebre mayor a 38,5C.
- Dolor pleurtico o cambios en examen pulmonar.
No es posible diferenciar etiologas puramente con clnica.
Moran G, Talan D, Abrahamian F - Diagnosis and management of pneumonia in the emergency department
Infectious Disease Clinics of North America 2008 vol. 22 (1) pp. 53-72, vi
Lionel A Mandell, Richard G Wunderink, Antonio Anzueto,, et Al - Infectious Diseases Society of America/American Thoracic Society consensus
guidelines on the management of community-acquired pneumonia in adults
Clinical Infectious Diseases 2007 vol. 44 Suppl 2 pp. S27-72
Lim WS, Bauddouin RC, George A, et Al. - BTS guidelines for the management of community acquired pneumonia in adults: update 2009
Thorax 2009 vol. 64 Suppl 3 pp. iii1-55
mircoles 17 de agosto de 11
Neumona
Manifestaciones Clnicas
Metlay JP, Kapoor WN, Fine MJ - Does this patient have community-acquired pneumonia? Diagnosing pneumonia by history and physical examination
Journal of the American Medical Association 1997, 278:1440-1445
Sintomatologa ms frecuente
0%
22,5%
45%
67,5%
90%
90%
66%
50%
15%
Tos
Expectoracin
Disnea
Hemoptisis
Adulto
Asintomtico
Mayor
mircoles 17 de agosto de 11
Neumona
Imgenes
Lim WS, Bauddouin RC, George A, et Al. - BTS guidelines for the management of community acquired pneumonia in adults: update 2009
Thorax 2009 vol. 64 Suppl 3 pp. iii1-55
Generalidades
La mayora de las sociedades recomiendan uso de imgenes en neumona.
- Modalidad ms recomendada es la radiografa de trax.
- Todo paciente con neumona que amerite hospitalizacin debe tenerla.
En general, signos son inespeccos.
- Neumona bacteriana: Broncograma areo.
- Neumona viral: Ndulos mal denidos, vidrio esmerilado peribronquial, consolidacin.
Alta variabilidad interobservador (! = 0.4)
La Tomografa computarizada tiene un rol en pacientes con radiografa negativa.
- No recomendada como modalidad de primera lnea.
Sat Sharma, Bruce Maycher, Gregg Eschun- Radiological imaging in pneumonia: recent innovations
Current Opinion in Pulmonary Medicine 2007 vol. 13 (3) pp. 159-69
T Franquet - Imaging of pneumonia: trends and algorithms
The European Respiratory Journal 2001 vol. 18 (1) pp. 196-208
mircoles 17 de agosto de 11
Neumona
Imgenes
T Franquet - Imaging of pneumonia: trends and algorithms
The European Respiratory Journal 2001 vol. 18 (1) pp. 196-208
The diagnosis of NP is difcult, and the criteria
used for surveillance have been based on clinical
ndings of fever, cough, and the development of
purulent sputum in combination with a new or
progressive inltrate on the chest radiograph. When
pneumonia arises in the hospitalized patient, aerobic
Gram negative bacilli, particularly Pseudomonas
aeruginosa and Enterobacter spp. and S. aureus, are
the major causative organisms [33]. Other common
causes of NP are H. Inuenza, pneumococcus,
aspiration with anaerobes, Legionella spp. and viruses
in certain hosts. Respiratory syncytial virus, inuenza
A and B, and parainuenza, are responsible forw70%
of nosocomial viral diseases [33]. The clinical and
radiographical clues to the aetiological diagnosis of
pneumonia are shown in table 1.
Immunosuppressed host pneumonia
Patients with impaired immune function are sus-
ceptible to infections by a wide range of organisms
[6, 7]. In the last several decades, AIDS epidemic,
advances in the treatment of cancer, organ transplan-
tation, and immunossuppressive therapy has resulted
in large numbers of patients who develop abnormal-
ities in their immune system [3436]. Pneumonia is a
major clinical problem for immunosuppressed pati-
ents and many of the bacteria causing CAP in the
healthy community are also responsible for pneumo-
nia in these risk patients. Mildy impaired host immu-
nity as it occurs in chronic debilitating illness, diabetes
mellitus, malnutrition, alcoholism, advanced age, pro-
longed corticosteroid administration and chronic obs-
tructive lung disease have also been regarded as
predisposing factors of pulmonary infections [37].
Acquired immune deciency syndrome
In AIDS patients, pulmonary complications may
result from a number of infectious and noninfectious
Fig. 5. Hospital-acquired pneumonia in an intensive care unit
patient. Portable anteroposterior supine chest radiography shows
bilateral lung consolidation. Protected bronchial brushes revealed
Gram positive cocci, gram positive rods, and Gram negative rods
on smear. Cultures grew Staphylococcus aureus and Pseudomonas
and Serratia organisms.
Table 1. Summary of clinical and radiographical clues to the aetiological diagnosis of pneumonia
Radiographical ndings Clinical circumstance Organism
Segmental consolidation Community-acquired S. pneumonia, M. pneumoniae
Lobar consolidation Community-acquired
Diabetes
S. pneumoniae (2/3 of community-acquired pneumonias)
K. pneumoniae
Gram negative bacilli
Rounded pneumonia Community-acquired
Alcoholic
S. pneumoniae
Bronchopneumonia Hospital-acquired P. aeruginosa, S. aureus, streptococci, Gram negative bacilli,
anaerobes, M. pneumoniae, aspiration, L. pneumophila
Interstitial pneumonia Community-acquired (winter) Virus, M. pneumoniae
Cavitation/necrosis Aspiration
COPD
S. aureus, Gram negative bacilli, anaerobes, actinomycosis,
M. Tuberculosis
Aspergillus
Multiple cavitary nodules Drug addict S. aureus
Pneumatoceles Postinuenza S. aureus
Empyema Complication of pneumonia S. pneumoniae
S. aureus
Gram negative bacilli
M. tuberculosis
Chest wall invasion Alcoholic Actinomycosis
M. tuberculosis
Fungi
Lymphadenopathy M. pneumoniae
M. tuberculosis
COPD: chronic obstructive pulmonary disease; S. pneumoniae: Streptococcus pneumoniae; S. aureus: Staphylococcus aureus;
M. tuberculosis: Mycobacterium tuberculosis; M. pneumoniae: Mycoplasma pneumoniae; K. pneumoniae: Klebsiella pneumoniae;
P. aeruginosa: Pseudomonas aeruginosa; L. pneumophila: Legionella pneumophila. Adapted from [34].
200 T. FRANQUET
Patrones Radiolgicos y Microorganismos
mircoles 17 de agosto de 11
Neumona
Imgenes
T Franquet - Imaging of pneumonia: trends and algorithms
The European Respiratory Journal 2001 vol. 18 (1) pp. 196-208
The diagnosis of NP is difcult, and the criteria
used for surveillance have been based on clinical
ndings of fever, cough, and the development of
purulent sputum in combination with a new or
progressive inltrate on the chest radiograph. When
pneumonia arises in the hospitalized patient, aerobic
Gram negative bacilli, particularly Pseudomonas
aeruginosa and Enterobacter spp. and S. aureus, are
the major causative organisms [33]. Other common
causes of NP are H. Inuenza, pneumococcus,
aspiration with anaerobes, Legionella spp. and viruses
in certain hosts. Respiratory syncytial virus, inuenza
A and B, and parainuenza, are responsible forw70%
of nosocomial viral diseases [33]. The clinical and
radiographical clues to the aetiological diagnosis of
pneumonia are shown in table 1.
Immunosuppressed host pneumonia
Patients with impaired immune function are sus-
ceptible to infections by a wide range of organisms
[6, 7]. In the last several decades, AIDS epidemic,
advances in the treatment of cancer, organ transplan-
tation, and immunossuppressive therapy has resulted
in large numbers of patients who develop abnormal-
ities in their immune system [3436]. Pneumonia is a
major clinical problem for immunosuppressed pati-
ents and many of the bacteria causing CAP in the
healthy community are also responsible for pneumo-
nia in these risk patients. Mildy impaired host immu-
nity as it occurs in chronic debilitating illness, diabetes
mellitus, malnutrition, alcoholism, advanced age, pro-
longed corticosteroid administration and chronic obs-
tructive lung disease have also been regarded as
predisposing factors of pulmonary infections [37].
Acquired immune deciency syndrome
In AIDS patients, pulmonary complications may
result from a number of infectious and noninfectious
Fig. 5. Hospital-acquired pneumonia in an intensive care unit
patient. Portable anteroposterior supine chest radiography shows
bilateral lung consolidation. Protected bronchial brushes revealed
Gram positive cocci, gram positive rods, and Gram negative rods
on smear. Cultures grew Staphylococcus aureus and Pseudomonas
and Serratia organisms.
Table 1. Summary of clinical and radiographical clues to the aetiological diagnosis of pneumonia
Radiographical ndings Clinical circumstance Organism
Segmental consolidation Community-acquired S. pneumonia, M. pneumoniae
Lobar consolidation Community-acquired
Diabetes
S. pneumoniae (2/3 of community-acquired pneumonias)
K. pneumoniae
Gram negative bacilli
Rounded pneumonia Community-acquired
Alcoholic
S. pneumoniae
Bronchopneumonia Hospital-acquired P. aeruginosa, S. aureus, streptococci, Gram negative bacilli,
anaerobes, M. pneumoniae, aspiration, L. pneumophila
Interstitial pneumonia Community-acquired (winter) Virus, M. pneumoniae
Cavitation/necrosis Aspiration
COPD
S. aureus, Gram negative bacilli, anaerobes, actinomycosis,
M. Tuberculosis
Aspergillus
Multiple cavitary nodules Drug addict S. aureus
Pneumatoceles Postinuenza S. aureus
Empyema Complication of pneumonia S. pneumoniae
S. aureus
Gram negative bacilli
M. tuberculosis
Chest wall invasion Alcoholic Actinomycosis
M. tuberculosis
Fungi
Lymphadenopathy M. pneumoniae
M. tuberculosis
COPD: chronic obstructive pulmonary disease; S. pneumoniae: Streptococcus pneumoniae; S. aureus: Staphylococcus aureus;
M. tuberculosis: Mycobacterium tuberculosis; M. pneumoniae: Mycoplasma pneumoniae; K. pneumoniae: Klebsiella pneumoniae;
P. aeruginosa: Pseudomonas aeruginosa; L. pneumophila: Legionella pneumophila. Adapted from [34].
200 T. FRANQUET
Patrones Radiolgicos y Microorganismos
No Recomendado
mircoles 17 de agosto de 11
Neumona
Etiologa
Daz A, Fuentes G, Couble B, Uribe R, et Al.- Etiologa de la neumona adquirida en la comunidad en adultos hospitalizados en Santiago, Chile:
implicancias para las guas clnicas
Revista Chilena de Enfermedades Respiratorias 2005, vol. 21 pp. 23-32
Microorganismos
Anucha Apisarnthanarak, Linda M Mundy - Etiology of community-acquired pneumonia
Clinics in Chest Medicine 2005 vol. 26 (1) pp. 47-55
Causa
!50%
Identificable
0%
7,5%
15%
22,5%
30%
21%
9,5% 7,5%
11%
5%
1%
14%
Neumococo
Mycoplasma
C. pneumoniae
H. inuenzae
M. catharralis
Legionella
Inuenza
mircoles 17 de agosto de 11
Neumona
Etiologa
Daz A, Fuentes G, Couble B, Uribe R, et Al.- Etiologa de la neumona adquirida en la comunidad en adultos hospitalizados en Santiago, Chile:
implicancias para las guas clnicas
Revista Chilena de Enfermedades Respiratorias 2005, vol. 21 pp. 23-32
Microorganismos
Anucha Apisarnthanarak, Linda M Mundy - Etiology of community-acquired pneumonia
Clinics in Chest Medicine 2005 vol. 26 (1) pp. 47-55
Causa
!50%
Identificable
0%
10%
20%
30%
40%
34%
22%
14% 11%
5%
3%
Neumococo
Parainuenza
Inuenza
H. inuenzae
M. pneumoniae
Legionella
mircoles 17 de agosto de 11
Neumona
Etiologa
Asociaciones
S. pneumoniae, H. inuenzae, K. pneumoniae, Anaerobios
S. aureus, Anaerobios, Bacilos Gram - Negativos
S. pneumoniae, Moraxella catarrhalis, H. inuenzae
Staphylococcus aureus
Pseudomonas aeruginosa, Gram negativos entricos, S. aureus
Pseudomonas aeruginosa
Anucha Apisarnthanarak, Linda M Mundy - Etiology of community-acquired pneumonia
Clinics in Chest Medicine 2005 vol. 26 (1) pp. 47-55
S. pneumoniae, H. inuenzae, S. aureus, Rodococcus equi
Alcohol
Aspiracin
EPOC
Drogas EV
Neutropenia
Bronquiectasias
VIH
mircoles 17 de agosto de 11
Neumona
Estudio Etiolgico
Estudio Recomendado
Lim WS, Bauddouin RC, George A, et Al. - BTS guidelines for the management of community acquired pneumonia in adults: update 2009
Thorax 2009 vol. 64 Suppl 3 pp. iii1-55
Hemocultivo
A todos?
Cultivo Esputo
(Sin antibiticos)
Legionella
Antgeno Urinario
IFI viral /
PCR
Si disponible
Neumococo
Antgeno Urinario
Recomendacin General
Pacientes Hospitalizados o Muy Graves
mircoles 17 de agosto de 11
Neumona
Estudio Etiolgico
Samuel G Campbell, Thomas J Marrie, Rosemary Anstey, Garth et Al.- The contribution of blood cultures to the clinical management of adult patients
admitted to the hospital with community-acquired pneumonia: a prospective observational study
Chest 2003 vol. 123 (4) pp. 1142-50
Hemocultivo para Todos?
Una herramienta sugerida en la mayora de las guas clnicas en neumona.
- Considerar que un 25 a 30% de las neumonas son bacterimicas.
- Diabticos ms susceptibles a neumona bacterimica.
- Utilidad en identicar patgeno especco y orientar terapia antimicrobiana.
Controversias: Tasa de positividad en torno al 5%.
- La misma probabilidad de falso positivo.
- Cambios de conducta raros: 0.4 a 2%.
Recomendacin: Uso juicioso
- En general, pacientes gravemente enfermos o con neumonas imagenolgicamente graves.
Lionel A Mandell, Richard G Wunderink, Antonio Anzueto,, et Al - Infectious Diseases Society of America/American Thoracic Society consensus
guidelines on the management of community-acquired pneumonia in adults
Clinical Infectious Diseases 2007 vol. 44 Suppl 2 pp. S27-72
mircoles 17 de agosto de 11
Neumona
Estudio Etiolgico
Samuel G Campbell, Thomas J Marrie, Rosemary Anstey, Garth et Al.- The contribution of blood cultures to the clinical management of adult patients
admitted to the hospital with community-acquired pneumonia: a prospective observational study
Chest 2003 vol. 123 (4) pp. 1142-50
Lionel A Mandell, Richard G Wunderink, Antonio Anzueto,, et Al - Infectious Diseases Society of America/American Thoracic Society consensus
guidelines on the management of community-acquired pneumonia in adults
Clinical Infectious Diseases 2007 vol. 44 Suppl 2 pp. S27-72
S40 CID 2007:44 (Suppl 2) Mandell et al.
Table 5. Clinical indications for more extensive diagnostic testing.
Indication
Blood
culture
Sputum
culture
Legionella
UAT
Pneumococcal
UAT Other
Intensive care unit admission X X X X X
a
Failure of outpatient antibiotic therapy X X X
Cavitary inltrates X X X
b
Leukopenia X X
Active alcohol abuse X X X X
Chronic severe liver disease X X
Severe obstructive/structural lung disease X
Asplenia (anatomic or functional) X X
Recent travel (within past 2 weeks) X X
c
Positive Legionella UAT result X
d
NA
Positive pneumococcal UAT result X X NA
Pleural effusion X X X X X
e
NOTE. NA, not applicable; UAT, urinary antigen test.
a
Endotracheal aspirate if intubated, possibly bronchoscopy or nonbronchoscopic bronchoalveolar lavage.
b
Fungal and tuberculosis cultures.
c
See table 8 for details.
d
Special media for Legionella.
e
Thoracentesis and pleural uid cultures.
dividuals risk of death but may decrease cost, drug adverse
effects, and antibiotic resistance pressure.
Some etiologic diagnoses have important epidemiologic im-
plications, such as documentation of severe acute respiratory
syndrome (SARS), inuenza, legionnaires disease, or agents of
bioterrorism. Diagnostic testing for these infections may affect
not only the individual but also many other people. Although
pneumonia etiologies that should be reported to public health
ofcials vary by state, in general, most states health regulations
require reporting of legionnaires disease, SARS, psittacosis,
avian inuenza (H5N1), and possible agents of bioterrorism
(plague, tularemia, and anthrax). In addition, specic diag-
nostic testing and reporting are important for pneumonia cases
of any etiology thought to be part of a cluster or caused by
pathogens not endemic to the area.
There are also societal reasons for encouraging diagnostic
testing. The antibiotic recommendations in the present guide-
lines are based on culture results and sensitivity patterns from
patients with positive etiologic diagnoses [102]. Without the
accumulated information available from these culture results,
trends in antibiotic resistance are more difcult to track, and
empirical antibiotic recommendations are less likely to be
accurate.
The main downside of extensive diagnostic testing of all
patients with CAP is cost, which is driven by the poor quality
of most sputum microbiological samples and the low yield of
positive culture results in many groups of patients with CAP.
A clear need for improved diagnostic testing in CAP, most likely
using molecular methodology rather than culture, has been
recognized by the National Institutes of Health [103].
The cost-benet ratio is even worse when antibiotic therapy
is not streamlined when possible [104, 105] or when inappro-
priate escalation occurs [95]. In clinical practice, narrowing of
antibiotic therapy is, unfortunately, unusual, but the committee
strongly recommends this as best medical practice. The pos-
sibility of polymicrobial CAP and the potential benet of com-
bination therapy for bacteremic pneumococcal pneumonia
have complicated the decision to narrow antibiotic therapy.
Delays in starting antibiotic therapy that result from the need
to obtain specimens, complications of invasive diagnostic pro-
cedures, and unneeded antibiotic changes and additional testing
for false-positive tests are also important considerations.
The general recommendation of the committee is to strongly
encourage diagnostic testing whenever the result is likely to
change individual antibiotic management. For other patients
with CAP, the recommendations for diagnostic testing focus
on patients in whom the diagnostic yield is thought to be
greatest. These 2 priorities often overlap. Recommendations for
patients in whom routine diagnostic testing is indicated for the
above reasons are listed in table 5. Because of the emphasis on
clinical relevance, a variety of diagnostic tests that may be ac-
curate but the results of which are not available in a time
window to allow clinical decisions are neither recommended
nor discussed.
11. Routine diagnostic tests to identify an etiologic diagnosis
are optional for outpatients with CAP. (Moderate rec-
ommendation; level III evidence.)
Retrospective studies of outpatient CAP management usually
show that diagnostic tests to dene an etiologic pathogen are
infrequently performed, yet most patients do well with empir-
mircoles 17 de agosto de 11
Neumona
Riesgo en Neumona
Evaluacin
El pronstico de la neumona es diverso segn el sitio de cuidado.
- Caractersticas de pacientes con enfermedad ms o menos grave.
- Dene opciones para la mejor terapia antimicrobiana.
- Una de las preguntas ms importantes a responder es decidir el lugar de cuidado.
Caractersticas clnicas clsicas operacionalizadas en ndices.
- Mltiples ndices descritos: PSI, CURB-65, SCAP, CURXO80, SCAP, APACHE-II entre otros.
Pedro Pablo Espaa Yandiola, Alberto Capelastegui, Jos Quintana - Prospective comparison of severity scores for predicting clinically relevant outcomes
for patients hospitalized with community-acquired pneumonia
Chest 2009 vol. 135 (6) pp. 1572-9
Lionel A Mandell, Richard G Wunderink, Antonio Anzueto,, et Al - Infectious Diseases Society of America/American Thoracic Society consensus
guidelines on the management of community-acquired pneumonia in adults
Clinical Infectious Diseases 2007 vol. 44 Suppl 2 pp. S27-72
Criterio Clnico: Siempre!
Un puntaje de riesgo en una escala no es una Ley
mircoles 17 de agosto de 11
Neumona
Riesgo en Neumona
Marcos I Restrepo, Antonio Anzueto - Severe Community - Acquired Pneumonia
Infectious Disease Clinics of North America 2009 vol. 23 (3) pp. 503-20
Escalas de Riesgo
PS-CURXO80, SMART-COP, and the PIRO-CAP scores have been created for this
purpose. Espan a and colleagues
48
developed and validated a clinical prediction
rule to assess the diagnosis of severe CAP. This new prediction score was derived
from the variables associated with severe CAP that include: arterial pH less than
7.30, Systolic blood pressure less than 90 mmHg, Confusion (or altered mental status),
blood Urea nitrogen greater than 30 mg/dL, Respiratory rate greater than 30 breaths/
min, multilobar/bilateral lung infiltrates (by X-ray), Oxygen arterial pressure less than
54 mm Hg or ratio of arterial oxygen tension to fraction of inspired oxygen less than
250 mm Hg, and age 80 years or older. The evaluation of severe CAP is based on
the presence of one major criterion (PS) or two or more minor criteria (CURXO80).
The model showed an area under the curve of 0.92 to accurately predict severe
CAP.
48
Charles and colleagues
49
developed the SMART-COP to predict the need for inten-
sive respiratory and vasopressor support. The features statistically significantly asso-
ciated with receipt of intensive respiratory care or vasopressor support were low
Systolic blood pressure (1 point), Multilobar chest radiography involvement (1 point),
low Albumin level (1 point), high Respiratory rate (age-adjusted) (1 point), Tachycardia
(1 point), Confusion (1 point), poor Oxygenation (age-adjusted) (2 points), and lowarte-
rial pH(< 7.35) (2 points): SMART-COP. A SMART-COP score of 3 points or more iden-
tified 92% of patients who received intensive respiratory care or vasopressor support,
including 84% of patients who did not need immediate admission to the ICU. This tool
was validated externally in five different cohorts with consistent results and can assist
the clinician in assessing the need for intensive respiratory care or vasopressor
support and CAP severity.
Table 2
Pneumonia severity index score and CURB- 65 hospital admission risk class stratification scores.
Pneumonia Severity Index Score
a
CURB- 65
b
Risk
Class Points
Mortality
(%)
Recommended
Site of Care
Risk
Class
Mortality
(%)
Recommended
Site of Care
I
c
0.1 Outpatient 0 0.7 Outpatient
II <70 0.6 Outpatient 1 2.1 Outpatient
III 7190 2.8 Outpatient
or brief
inpatient
2 9.2 Inpatient
IV 91130 8.2 Inpatient 3 14.5 Inpatient
V >130 29.2 Inpatient 45 4057 Inpatient
(possible need
for ICU care)
a
Metlay and Fine
47
suggested a three-step process to decide the initial site of CAP treatment based
on: (1) assessment of preexisting conditions that compromise safety of home care, (2) calculation of
the pneumonia severity index score, and (3) clinical judgment
48
. Data fromFine MJ, Auble TE, Yealy
DM, et al. A prediction rule to identify low-risk patients with community-acquired pneumonia.
N Engl J Med 1997;336:24350.
b
CURB-65
40,41
related to Confusion (altered mental status); serum blood Urea nitrogen > 19.6 mg/
dL; Respiratory rate > 30 breaths per minute; Blood pressure (BP) (systolic BP < 90 mm Hg or dia-
stolic BP < 60 mm Hg); and age R 65 years. Each criterion has a score of one, and the total score
is added by the presence of each of the five criteria. Two or more criteria suggest severe CAP
and admission to the hospital is recommended; a patient who has three or more criteria needs
an assessment for ICU (more likely to be in scores 4 or 5).
c
Risk class I: age < 50 years, no comorbidities, and absence of vital sign abnormalities.
Severe Community-Acquired Pneumonia 507
mircoles 17 de agosto de 11
Neumona
Riesgo en Neumona
Marcos I Restrepo, Antonio Anzueto - Severe Community - Acquired Pneumonia
Infectious Disease Clinics of North America 2009 vol. 23 (3) pp. 503-20
Unidad de Cuidados Intensivos
Cundo Llamar al Residente?
Rello and colleagues
50
developed the CAP-PIRO score based on the score sug-
gested for the risk for sepsis. This score evaluates variables related to the PIRO score
that include: Predisposition, Infection, Response, and Organ dysfunction. The CAP-
PIRO score intends to adjust for the complexity of the patients critically ill with CAP.
CAP-PIRO score evaluates the following variables: Predisposition: comorbidities
(COPD or immunocompromised) (1 point), age greater than 70 years (1 point); Infec-
tion: bacteremia (1 point), multilobar opacities (1 point); Response: shock (1 point),
severe hypoxemia (1 point); and Organ dysfunction: acute respiratory distress
syndrome (ARDS, 1 point), acute renal failure (1 point). Considering the observed
mortality from each PIRO score, the patients were stratified in four levels of risk: (a)
low, 0 to 2 points; (b) mild, 3 points; (c) high, 4 points; and (d) very high, 5 to 8 points.
This score was able to consistently predict the ICU mortality and health care use in
a cohort of 529 patients admitted to the ICU with CAP.
50
In conclusion, the last four severity criteria scores have in common the overlap in the
variables selected, and it is clear that the newconcept of severe CAP goes beyond the
lungs and looks for systemic organ dysfunction (Table 4). Future prospective valida-
tion studies are needed for these scores.
THERAPEUTIC STRATEGIES TOMANAGE SCAP PATIENTS
Traditionally the antimicrobial agents have been considered the cornerstone of
therapy against severe CAP; however, with the purpose of understanding severe
CAP as a systemic disease, there are other non-antimicrobial therapies that should
be considered in this group of patients. Therapeutic strategies for managing patients
who have severe CAP are summarized in Box 1.
Antimicrobial Therapies
Several professional organizations developed clinical practice guidelines with the
objective of standardized therapy for CAP following an evidence-based medicine
Table 3
AmericanThoracic Society modified criteria and 2007 Infectious Diseases Society of America/
AmericanThoracic Society criteria
ATS 2001
29
IDSA/ATS 2007
24
Major criteria
Need for mechanical ventilation
Requiring vasopressors (septic shock)
Need for mechanical ventilation
Septic shock with the need for vasopressors
Minor criteria
Respiratory rate R30 breaths/min
PaO
2
/FiO
2
ratio % 250
Bilateral or multilobar infiltrates
Respiratory rate R30 breaths/min
New-onset confusion/disorientation
Thrombocytopenia (platelets < 100,000
cells/mL)
PaO
2
/FIO
2
ratio %250
Uremia (BUN level > 20 mg/dL)
Hypothermia (core temperature < 36
C)
Bilateral or multilobar infiltrates
Leukopenia (WBC count <4000 cells/mL)
Hypotension requiring aggressive fluid
resuscitation
The presence of at least one major criterion or at least two minor criteria defines pneumonia case
severe enough to require ICU admission.
Abbreviations: BUN, blood urea nitrogen; FIO
2
, fraction of inspired oxygen; WBC, white blood cell.
Data from References.
24,29,42,43,45
Restrepo & Anzueto 508
mircoles 17 de agosto de 11
Neumona
Riesgo en Neumona
Y qu tan bien predicen las escalas?
cohort, the rate of these outcomes increased
steadily from low- to high-risk classes for the
SCAP score as well as for the PSI and CURB-65
(p 0.001). In the internal validation cohort,
there were no significant differences in outcomes
such as ICU admission and mechanical ventilation
for the PSI and CURB-65. This could be attrib-
uted to a lower proportion of these two outcomes
in the internal validation cohort.
All three scores predicted treatment failure with
low to moderate discrimination in the external vali-
dation cohort. It must be noted that the initial
severity of CAP is only one factor predicting treat-
ment failure. Other factors, such as the causal mi-
croorganism and treatment-related factors,
17
are not
part of the three prediction tools.
The SCAP score classified a significantly higher
proportion of patients as low risk in both cohorts
than the PSI and CURB-65, with lower rates of all
adverse outcomes. Another goal of the tool is its
negative predictive value. If the score is low, ICU
admission and others adverse outcomes are very
unlikely. In addition, patients identified as high risk by
the SCAP score had somewhat higher rates of ICU
admissions, need for mechanical ventilation, and severe
sepsis compared with the PSI and CURB-65. Thus,
Table 4Comparison of Different Outcome Measures of the CURB-65 Predictive Rule
CURB-65 Patients, No. ICU Admission
Mechanical
Ventilation Severe Sepsis
Treatment
Failure
Hospital
LOS, d*
Internal validation group
Total No. of patients 1,189 57 23 453 141
Low (01) 485 (40.8) 19 (3.9) 7 (1.4) 101 (22.9) 42 (8.7) 3.6
Intermediate (2) 404 (34) 19 (4.7) 9 (2.2) 146 (36.1) 56 (13.9) 4.5
High (35) 300 (25.2) 19 (6.3) 7 (2.3) 196 (65.3) 43 (14.3) 4.6
p Value 0.30 0.59 0.0001 0.018 0.0003
External validation group
Total No. of patients 671 57 22 249 73
Low (01) 297 (44.3) 14 (4.7) 5 (1.7) 59 (19.9) 29 (9.8) 8.6
Intermediate (2) 219 (32.6) 14 (6.4) 7 (3.2) 86 (39.3) 20 (9.1) 8.3
High (35) 155 (23.1) 29 (18.7) 10 (6.4) 104 (67.1) 24 (15.5) 11.4
p Value 0.0001 0.026 0.0001 0.11 0.0005
*Statistically significant differences (by ANOVA with Scheff test) in hospital LOS among the three CURB-65 classes were found between
low vs intermediate or high classes in the internal cohort, whereas in the external cohort they were found between high vs intermediate
or low classes.
Table 5Predictive Values of Scores for Adverse Outcomes in the External Validation Cohort*
Scores Sensitivity Specificity Odds Ratio 95% CI AUC
SCAP
ICU admission 80.7 68.4 9.05 4.5917.86 0.746
Severe sepsis 71.9 85.5 15.13 10.2722.29 0.79
Mechanical ventilation 86.4 65.9 12.26 3.5941.88 0.76
Treatment failure 54.8 66.6 2.41 1.483.94 0.61
PSI
ICU admission 70.2 56.6 3.07 1.705.54 0.63
Severe sepsis 73.8 70.9 6.88 4.839.79 0.72
Mechanical ventilation 81.8 55.6 5.63 1.8816.82 0.69
Treatment failure 58.9 56 1.82 1.112.98 0.57
CURB-65
ICU admission 75.4 46.1 2.63 1.414.90 0.61
Severe sepsis 76.3 56.4 4.16 2.945.91 0.66#
Mechanical ventilation 77.3 45 2.78 1.017.63 0.61#
Treatment failure 60.3 44.8 1.32 0.752.02 0.52
*The scores were dichotomized as low risk vs higher risk (SCAP score 2, CURB-65 2, and PSI IV). CI confidence interval.
Statistically significant difference (vs PSI and CURB-65).
Statistically significant difference (vs CURB-65).
Statistically significant difference (vs SCAP).
Statistically significant difference (vs SCAP and CURB-65).
No difference.
#Statistically significant difference (vs SCAP and PSI).
www.chestjournal.org CHEST / 135 / 6 / JUNE, 2009 1577
2009 American College of Chest Physicians
by guest on April 6, 2011 chestjournal.chestpubs.org Downloaded from
Pedro Pablo Espaa Yandiola, Alberto Capelastegui, Jos Quintana - Prospective comparison of severity scores for predicting clinically relevant outcomes
for patients hospitalized with community-acquired pneumonia
Chest 2009 vol. 135 (6) pp. 1572-9
K L Buising, K A Thursky, J F Black, L MacGregor, A, et Al - A prospective comparison of severity scores for identifying patients with severe community
acquired pneumonia: reconsidering what is meant by severe pneumonia
Thorax 2006 vol. 61 (5) pp. 419-24
mircoles 17 de agosto de 11
Neumona
Tratamiento
Pilares Teraputicos
Lim WS, Bauddouin RC, George A, et Al. - BTS guidelines for the management of community acquired pneumonia in adults: update 2009
Thorax 2009 vol. 64 Suppl 3 pp. iii1-55
Lionel A Mandell, Richard G Wunderink, Antonio Anzueto,, et Al - Infectious Diseases Society of America/American Thoracic Society consensus
guidelines on the management of community-acquired pneumonia in adults
Clinical Infectious Diseases 2007 vol. 44 Suppl 2 pp. S27-72
Antimicrobianos
Terapia guiada por riesgo y antecedentes epidemiolgicos
Medidas generales
Dejar de fumar, reposo, analgesia, tromboprofilaxis
Oxigenoterapia
Saturacin inferior al 94% asociada a peores resultados
Protena C Activada Recombinante
Incrementa o disminuye la mortalidad?
Esteroides?
Pacientes especialmente graves Se Benefician?
mircoles 17 de agosto de 11
Neumona
Antimicrobianos
Lim WS, Bauddouin RC, George A, et Al. - BTS guidelines for the management of community acquired pneumonia in adults: update 2009
Thorax 2009 vol. 64 Suppl 3 pp. iii1-55
Lionel A Mandell, Richard G Wunderink, Antonio Anzueto,, et Al - Infectious Diseases Society of America/American Thoracic Society consensus
guidelines on the management of community-acquired pneumonia in adults
Clinical Infectious Diseases 2007 vol. 44 Suppl 2 pp. S27-72
Antibiticos
Considerados la piedra angular del manejo de la neumona.
- Disminuyen estada hospitalaria, duracin de enfermedad y mortalidad.
- Siempre pensar en cubrir patgenos de alta mortalidad: Neumococo y Legionella.
Severidad del episodio determinar seleccin de terapia antimicrobiana.
- Determinacin apropiada del riesgo fundamental para evitar abuso.
- Factores clnicos y epidemiolgicos deben considerarse adems del riesgo.
Meta a inicio de antibiticos (BTS): 4 Horas desde la consulta.
Controles clnicos seriados permiten de-escalar terapia.
Marcos I Restrepo, Antonio Anzueto - Severe Community - Acquired Pneumonia
Infectious Disease Clinics of North America 2009 vol. 23 (3) pp. 503-20
mircoles 17 de agosto de 11
Neumona
Antimicrobianos
Lim WS, Bauddouin RC, George A, et Al. - BTS guidelines for the management of community acquired pneumonia in adults: update 2009
Thorax 2009 vol. 64 Suppl 3 pp. iii1-55
Lionel A Mandell, Richard G Wunderink, Antonio Anzueto,, et Al - Infectious Diseases Society of America/American Thoracic Society consensus
guidelines on the management of community-acquired pneumonia in adults
Clinical Infectious Diseases 2007 vol. 44 Suppl 2 pp. S27-72
Marcos I Restrepo, Antonio Anzueto - Severe Community - Acquired Pneumonia
Infectious Disease Clinics of North America 2009 vol. 23 (3) pp. 503-20
Terapia por Grupos
Amoxicilina (500mg - 1gr c/12h), Macrlido, Doxiciclina (100mg c/12 horas)
Grupo 1
Sano
mircoles 17 de agosto de 11
Neumona
Antimicrobianos
Lim WS, Bauddouin RC, George A, et Al. - BTS guidelines for the management of community acquired pneumonia in adults: update 2009
Thorax 2009 vol. 64 Suppl 3 pp. iii1-55
Lionel A Mandell, Richard G Wunderink, Antonio Anzueto,, et Al - Infectious Diseases Society of America/American Thoracic Society consensus
guidelines on the management of community-acquired pneumonia in adults
Clinical Infectious Diseases 2007 vol. 44 Suppl 2 pp. S27-72
Marcos I Restrepo, Antonio Anzueto - Severe Community - Acquired Pneumonia
Infectious Disease Clinics of North America 2009 vol. 23 (3) pp. 503-20
Terapia por Grupos
Amoxicilina (500mg - 1gr c/12h), Macrlido, Doxiciclina (100mg c/12 horas)
Amoxicilina (500mg - 1gr c/12h) y/o Macrlido, Quinolona respiratoria,
Doxiciclina (100mg c/12 horas)
Quinolona respiratoria, ! - Lactmico y Macrlido
Quinolona respiratoria y ! - Lactmico (Antipseudomnico)
Grupo 1
Sano
Grupo 2
Bajo Riesgo
Grupo 3
Hospitalizado
Grupo 4
Intensivo
mircoles 17 de agosto de 11
Neumona
Antimicrobianos
Lim WS, Bauddouin RC, George A, et Al. - BTS guidelines for the management of community acquired pneumonia in adults: update 2009
Thorax 2009 vol. 64 Suppl 3 pp. iii1-55
Terapia por Agentes
in those patients initially managed with amoxicillin alone.
Changing to doxycyline or a new fluoroquinolone such as
levofloxacin are alternatives.
In the patient with high severity pneumonia already receiving
a b-lactam/clarithromycin regimen, the addition of levofloxacin
should be considered. In addition, urgent referral to a respiratory
physician should be made for clinical assessment including the
possible need for bronchoscopic sampling.
Recommendations
c When a change in empirical antibiotic therapy is
considered necessary, a macrolide could be substituted
for or added to the treatment for those with low
severity pneumonia treated with amoxicillin mono-
therapy in the community or in hospital. [D]
c For those with moderate severity pneumonia in
hospital on combination therapy, changing to doxycy-
cline or a fluoroquinolone with effective pneumococcal
cover are alternative options. [D]
c Adding a fluoroquinolone is an option for those with
high severity pneumonia not responding to a b-lactam/
macrolide combination antibiotic regimen. [D]
8.18 Antibiotic stewardship and avoiding inappropriate antibiotic
prescribing for CAP
Inappropriate antibiotic prescribing is a driver for antibiotic
resistance and increases the likelihood of development of C
difficile infection. Given the frequency of admissions to hospital
for suspected CAP and the difficulty in identifying a causative
pathogen often leading to initial empirical broad-spectrum
antibiotic therapy, it is timely to offer guidance to limit
inappropriate prescribing in the context of the management of
patients with CAP.
Ensuring an accurate diagnosis of CAP is the most important
issue in relation to the avoidance of inappropriate antibiotic
prescribing. One study reported that 29% of hospitalised
Box 4 Features indicating response to initial empirical
parenteral therapy permitting consideration of oral
antibiotic substitution
c Resolution of fever for .24 h
c Pulse rate ,100 beats/min
c Resolution of tachypnoea
c Clinically hydrated and taking oral fluids
c Resolution of hypotension
c Absence of hypoxia
c Improving white cell count
c Non-bacteraemic infection
c No microbiological evidence of legionella, staphylococcal or
Gram-negative enteric bacilli infection
c No concerns over gastrointestinal absorption
Table 6 Recommended treatment of microbiologically documented pneumonia and aspiration pneumonia
(local specialist advice should also be sought*)
Pathogen Preferred Alternative
S pneumoniae Amoxicillin 500 mg 1.0 g{ tds orally or
benzylpenicillin 1.2 g qds IV
Clarithromycin 500 mg bd orally or cefuroxine 0.751.5 g
tds IV or cefotaxime 12 g tds IV or ceftriaxone 2 g od IV
M pneumoniae
C pneumoniae
Clarithromycin 500 mg bd orally or IV Doxycycline 200 mg loading dose then 100 mg od orally
or fluoroquinolone{ orally or IV
C psittaci
C burnetii
Doxycycline 200 mg loading dose then 100 mg od
orally
Clarithromycin 500 mg bd orally or 500 mg bd IV
Legionella spp Fluoroquinolone orally or IV{1 Clarithromycin 500 mg bd orally or IV (or, if necessary,
azithromycin in countries where this antibiotic is used for
managing pneumonia)
H influenzae Non-b-lactamase-producing: amoxicillin 500 mg tds
orally or IV
b-lactamase-producing: co-amoxiclav 625 mg tds
orally or 1.2 g tds IV
Cefuroxime 750 mg 1.5 g tds IV or cefotaxime 12 g tds
IV or ceftriaxone 2 g od IV or fluoroquinolone{ orally or IV
Gram-negative
enteric bacilli
Cefuroxime 1.5 g tds or cefotaxime 12 g tds IV or
ceftriaxone 12 g bd IV
Fluoroquinolone{ IV or imipenem 500 mg qds IV or
meropenem 0.51.0 g tds IV
P aeruginosa Ceftazidime 2 g tds IV plus gentamicin or tobramycin
(dose monitoring)
Ciprofloxacin 400 mg bd IV or piperacillin 4 g tds IV, plus
gentamicin or tobramycin (dose monitoring)
S aureus Non-MRSA: flucloxacillin 12 g qds IV rifampicin
600 mg od or bd orally/IV
MRSA: vancomycin 1 g bd IV (dose monitoring) or
linezolid 600 mg bd IV or teicoplanin 400 mg bd IV
rifampicin 600 mg od or bd orally/IV
Aspiration
pneumonia
Co-amoxiclav 1.2 g tds IV Seek local microbiology advice
bd, twice daily; IV, intravenous; od, once daily; tds, three times daily.
*Treatment can be modified once the results of sensitivity testing are available.
{A higher dose of 1.0 g tds is recommended for infections documented to be caused by less susceptible strains (minimum
inhibitory concentration .1.0 mg/l).
{Currently UK licensed and available suitable fluoroquinolones include ciprofloxacin, ofloxacin and levofloxacin. Moxifloxacin can
be used for patients who cannot be treated or have failed treatment with other antibacterials.
1Specifically for legionella pneumonia, the large majority of published experience regarding the efficacy of fluoroquinolones is only
with levofloxacin. For high severity or life-threatening legionella pneumonia, combination therapy including the preferred and an
alternative antibiotic can be considered for the first few days (see text for further details). Rifampicin is not recommended on its
own but could be considered as the second additional antibiotic.
BTS guidelines
iii40 Thorax 2009;64(Suppl III):iii1iii55. doi:10.1136/thx.2009.121434
mircoles 17 de agosto de 11
Neumona
Esteroides
Corticoides en Sepsis
Existen argumentos para plantear uso de esteroides en sepsis.
- Insuciencia suprarrenal relativa en torno a dos tercios de los pacientes.
- Sensibilizacin a vasopresores.
- Modulacin de respuesta inmune.
Estudios antiguos plantean mejores resultados clnicos con Hidrocortisona.
- Mortalidad 0 v/s 30% (46 pacientes).
- Acortara estada hospitalaria en 7 das.
Sin embargo, benecios no han sido conrmados.
- Estudio CORTICUS no demostr benecios en mortalidad ni estada en UCI.
- No recomendados de rutina segn Campaa Sobreviviendo a la Sepsis.
Marcos I Restrepo, Antonio Anzueto - Severe Community - Acquired Pneumonia
Infectious Disease Clinics of North America 2009 vol. 23 (3) pp. 503-20
Charles L Sprung, Djillali Annane, Didier Keh, et Al. - Hydrocortisone therapy for patients with septic shock
The New England Journal of Medicine 2008 vol. 358 (2) pp. 111-24
R Phillip Dellinger, et Al. - Surviving Sepsis Campaign: international guidelines for management of severe sepsis and septic shock: 2008
Intensive Care Medicine 2008 vol. 34 (1) pp. 17-60
mircoles 17 de agosto de 11
Neumona
Esteroides
Neumona
Correlacin directa entre citoquinas proinamatorias y gravedad (APACHE II)
- Efecto inmunomodulador de esteroides beneciara a pacientes con neumona.
- Relacin evaluada en dos ensayos aleatorizados con buenos resultados.
El ms estudiado es la Hidrocortisona (10mg/Kg)
- Rapidez de accin.
- Mecanismos mineralocorticoides predominantes
Los benecios clnicos no han sido conrmados.
- Revisin Cochrane reciente slo demostr disminucin en sintomatologa.
- Dos revisiones sistemticas de baja calidad no demuestran benecio alguno.
Marcos I Restrepo, Antonio Anzueto - Severe Community - Acquired Pneumonia
Infectious Disease Clinics of North America 2009 vol. 23 (3) pp. 503-20
Sean K Gorman, Richard S Slavik, Judith Marin - Corticosteroid treatment of severe community-acquired pneumonia
Annals of Pharmacotherapy 2007 vol. 41 (7) pp. 1233-7
Jorge I F Salluh, Pedro Pvoa, Mrcio Soares, Hugo C et Al. - The role of corticosteroids in severe community-acquired pneumonia: a systematic review
Critical Care 2008 vol. 12 (3) pp. R76
mircoles 17 de agosto de 11
Neumona
Criterios de Respuesta
Cuando Todo Anda bien!
Elementos para pensar en dar de alta al enfermo
Lim WS, Bauddouin RC, George A, et Al. - BTS guidelines for the management of community acquired pneumonia in adults: update 2009
Thorax 2009 vol. 64 Suppl 3 pp. iii1-55
in those patients initially managed with amoxicillin alone.
Changing to doxycyline or a new fluoroquinolone such as
levofloxacin are alternatives.
In the patient with high severity pneumonia already receiving
a b-lactam/clarithromycin regimen, the addition of levofloxacin
should be considered. In addition, urgent referral to a respiratory
physician should be made for clinical assessment including the
possible need for bronchoscopic sampling.
Recommendations
c When a change in empirical antibiotic therapy is
considered necessary, a macrolide could be substituted
for or added to the treatment for those with low
severity pneumonia treated with amoxicillin mono-
therapy in the community or in hospital. [D]
c For those with moderate severity pneumonia in
hospital on combination therapy, changing to doxycy-
cline or a fluoroquinolone with effective pneumococcal
cover are alternative options. [D]
c Adding a fluoroquinolone is an option for those with
high severity pneumonia not responding to a b-lactam/
macrolide combination antibiotic regimen. [D]
8.18 Antibiotic stewardship and avoiding inappropriate antibiotic
prescribing for CAP
Inappropriate antibiotic prescribing is a driver for antibiotic
resistance and increases the likelihood of development of C
difficile infection. Given the frequency of admissions to hospital
for suspected CAP and the difficulty in identifying a causative
pathogen often leading to initial empirical broad-spectrum
antibiotic therapy, it is timely to offer guidance to limit
inappropriate prescribing in the context of the management of
patients with CAP.
Ensuring an accurate diagnosis of CAP is the most important
issue in relation to the avoidance of inappropriate antibiotic
prescribing. One study reported that 29% of hospitalised
Box 4 Features indicating response to initial empirical
parenteral therapy permitting consideration of oral
antibiotic substitution
c Resolution of fever for .24 h
c Pulse rate ,100 beats/min
c Resolution of tachypnoea
c Clinically hydrated and taking oral fluids
c Resolution of hypotension
c Absence of hypoxia
c Improving white cell count
c Non-bacteraemic infection
c No microbiological evidence of legionella, staphylococcal or
Gram-negative enteric bacilli infection
c No concerns over gastrointestinal absorption
Table 6 Recommended treatment of microbiologically documented pneumonia and aspiration pneumonia
(local specialist advice should also be sought*)
Pathogen Preferred Alternative
S pneumoniae Amoxicillin 500 mg 1.0 g{ tds orally or
benzylpenicillin 1.2 g qds IV
Clarithromycin 500 mg bd orally or cefuroxine 0.751.5 g
tds IV or cefotaxime 12 g tds IV or ceftriaxone 2 g od IV
M pneumoniae
C pneumoniae
Clarithromycin 500 mg bd orally or IV Doxycycline 200 mg loading dose then 100 mg od orally
or fluoroquinolone{ orally or IV
C psittaci
C burnetii
Doxycycline 200 mg loading dose then 100 mg od
orally
Clarithromycin 500 mg bd orally or 500 mg bd IV
Legionella spp Fluoroquinolone orally or IV{1 Clarithromycin 500 mg bd orally or IV (or, if necessary,
azithromycin in countries where this antibiotic is used for
managing pneumonia)
H influenzae Non-b-lactamase-producing: amoxicillin 500 mg tds
orally or IV
b-lactamase-producing: co-amoxiclav 625 mg tds
orally or 1.2 g tds IV
Cefuroxime 750 mg 1.5 g tds IV or cefotaxime 12 g tds
IV or ceftriaxone 2 g od IV or fluoroquinolone{ orally or IV
Gram-negative
enteric bacilli
Cefuroxime 1.5 g tds or cefotaxime 12 g tds IV or
ceftriaxone 12 g bd IV
Fluoroquinolone{ IV or imipenem 500 mg qds IV or
meropenem 0.51.0 g tds IV
P aeruginosa Ceftazidime 2 g tds IV plus gentamicin or tobramycin
(dose monitoring)
Ciprofloxacin 400 mg bd IV or piperacillin 4 g tds IV, plus
gentamicin or tobramycin (dose monitoring)
S aureus Non-MRSA: flucloxacillin 12 g qds IV rifampicin
600 mg od or bd orally/IV
MRSA: vancomycin 1 g bd IV (dose monitoring) or
linezolid 600 mg bd IV or teicoplanin 400 mg bd IV
rifampicin 600 mg od or bd orally/IV
Aspiration
pneumonia
Co-amoxiclav 1.2 g tds IV Seek local microbiology advice
bd, twice daily; IV, intravenous; od, once daily; tds, three times daily.
*Treatment can be modified once the results of sensitivity testing are available.
{A higher dose of 1.0 g tds is recommended for infections documented to be caused by less susceptible strains (minimum
inhibitory concentration .1.0 mg/l).
{Currently UK licensed and available suitable fluoroquinolones include ciprofloxacin, ofloxacin and levofloxacin. Moxifloxacin can
be used for patients who cannot be treated or have failed treatment with other antibacterials.
1Specifically for legionella pneumonia, the large majority of published experience regarding the efficacy of fluoroquinolones is only
with levofloxacin. For high severity or life-threatening legionella pneumonia, combination therapy including the preferred and an
alternative antibiotic can be considered for the first few days (see text for further details). Rifampicin is not recommended on its
own but could be considered as the second additional antibiotic.
BTS guidelines
iii40 Thorax 2009;64(Suppl III):iii1iii55. doi:10.1136/thx.2009.121434
mircoles 17 de agosto de 11
Neumona
Criterios de Respuesta
Cuando Todo Anda bien!
Elementos para pensar en dar de alta al enfermo
Lim WS, Bauddouin RC, George A, et Al. - BTS guidelines for the management of community acquired pneumonia in adults: update 2009
Thorax 2009 vol. 64 Suppl 3 pp. iii1-55
in those patients initially managed with amoxicillin alone.
Changing to doxycyline or a new fluoroquinolone such as
levofloxacin are alternatives.
In the patient with high severity pneumonia already receiving
a b-lactam/clarithromycin regimen, the addition of levofloxacin
should be considered. In addition, urgent referral to a respiratory
physician should be made for clinical assessment including the
possible need for bronchoscopic sampling.
Recommendations
c When a change in empirical antibiotic therapy is
considered necessary, a macrolide could be substituted
for or added to the treatment for those with low
severity pneumonia treated with amoxicillin mono-
therapy in the community or in hospital. [D]
c For those with moderate severity pneumonia in
hospital on combination therapy, changing to doxycy-
cline or a fluoroquinolone with effective pneumococcal
cover are alternative options. [D]
c Adding a fluoroquinolone is an option for those with
high severity pneumonia not responding to a b-lactam/
macrolide combination antibiotic regimen. [D]
8.18 Antibiotic stewardship and avoiding inappropriate antibiotic
prescribing for CAP
Inappropriate antibiotic prescribing is a driver for antibiotic
resistance and increases the likelihood of development of C
difficile infection. Given the frequency of admissions to hospital
for suspected CAP and the difficulty in identifying a causative
pathogen often leading to initial empirical broad-spectrum
antibiotic therapy, it is timely to offer guidance to limit
inappropriate prescribing in the context of the management of
patients with CAP.
Ensuring an accurate diagnosis of CAP is the most important
issue in relation to the avoidance of inappropriate antibiotic
prescribing. One study reported that 29% of hospitalised
Box 4 Features indicating response to initial empirical
parenteral therapy permitting consideration of oral
antibiotic substitution
c Resolution of fever for .24 h
c Pulse rate ,100 beats/min
c Resolution of tachypnoea
c Clinically hydrated and taking oral fluids
c Resolution of hypotension
c Absence of hypoxia
c Improving white cell count
c Non-bacteraemic infection
c No microbiological evidence of legionella, staphylococcal or
Gram-negative enteric bacilli infection
c No concerns over gastrointestinal absorption
Table 6 Recommended treatment of microbiologically documented pneumonia and aspiration pneumonia
(local specialist advice should also be sought*)
Pathogen Preferred Alternative
S pneumoniae Amoxicillin 500 mg 1.0 g{ tds orally or
benzylpenicillin 1.2 g qds IV
Clarithromycin 500 mg bd orally or cefuroxine 0.751.5 g
tds IV or cefotaxime 12 g tds IV or ceftriaxone 2 g od IV
M pneumoniae
C pneumoniae
Clarithromycin 500 mg bd orally or IV Doxycycline 200 mg loading dose then 100 mg od orally
or fluoroquinolone{ orally or IV
C psittaci
C burnetii
Doxycycline 200 mg loading dose then 100 mg od
orally
Clarithromycin 500 mg bd orally or 500 mg bd IV
Legionella spp Fluoroquinolone orally or IV{1 Clarithromycin 500 mg bd orally or IV (or, if necessary,
azithromycin in countries where this antibiotic is used for
managing pneumonia)
H influenzae Non-b-lactamase-producing: amoxicillin 500 mg tds
orally or IV
b-lactamase-producing: co-amoxiclav 625 mg tds
orally or 1.2 g tds IV
Cefuroxime 750 mg 1.5 g tds IV or cefotaxime 12 g tds
IV or ceftriaxone 2 g od IV or fluoroquinolone{ orally or IV
Gram-negative
enteric bacilli
Cefuroxime 1.5 g tds or cefotaxime 12 g tds IV or
ceftriaxone 12 g bd IV
Fluoroquinolone{ IV or imipenem 500 mg qds IV or
meropenem 0.51.0 g tds IV
P aeruginosa Ceftazidime 2 g tds IV plus gentamicin or tobramycin
(dose monitoring)
Ciprofloxacin 400 mg bd IV or piperacillin 4 g tds IV, plus
gentamicin or tobramycin (dose monitoring)
S aureus Non-MRSA: flucloxacillin 12 g qds IV rifampicin
600 mg od or bd orally/IV
MRSA: vancomycin 1 g bd IV (dose monitoring) or
linezolid 600 mg bd IV or teicoplanin 400 mg bd IV
rifampicin 600 mg od or bd orally/IV
Aspiration
pneumonia
Co-amoxiclav 1.2 g tds IV Seek local microbiology advice
bd, twice daily; IV, intravenous; od, once daily; tds, three times daily.
*Treatment can be modified once the results of sensitivity testing are available.
{A higher dose of 1.0 g tds is recommended for infections documented to be caused by less susceptible strains (minimum
inhibitory concentration .1.0 mg/l).
{Currently UK licensed and available suitable fluoroquinolones include ciprofloxacin, ofloxacin and levofloxacin. Moxifloxacin can
be used for patients who cannot be treated or have failed treatment with other antibacterials.
1Specifically for legionella pneumonia, the large majority of published experience regarding the efficacy of fluoroquinolones is only
with levofloxacin. For high severity or life-threatening legionella pneumonia, combination therapy including the preferred and an
alternative antibiotic can be considered for the first few days (see text for further details). Rifampicin is not recommended on its
own but could be considered as the second additional antibiotic.
BTS guidelines
iii40 Thorax 2009;64(Suppl III):iii1iii55. doi:10.1136/thx.2009.121434
20%
No cumple al Alta
46%
Muerto o Reingreso
11%
Muerto o Reingreso
mircoles 17 de agosto de 11
Neumona
Criterios de Respuesta
Lim WS, Bauddouin RC, George A, et Al. - BTS guidelines for the management of community acquired pneumonia in adults: update 2009
Thorax 2009 vol. 64 Suppl 3 pp. iii1-55
Y si todo sale mal?
(Cinco preguntas para no caer en pnico)
Diagnstico correcto?
TEP, Edema pulmonar, cncer broncognico, COP, Cuerpo extrao, ancianos, bronquiectasia
Patgeno correcto?
Atpicos no cubiertos o resistencia primaria al antimicrobiano
Defensas del paciente suficientes?
Bronquiectasias, aspiracin, obstruccin bronquial, SIDA, Mieloma, Hipogammaglobulinemia
Complicacin de Neumona?
Derrame pleural, empiema, absceso, SDRA, Sepsis severa, flebitis, infeccin a distancia
Expectativas realistas?
Recordar que ancianos tienen respuesta ms lenta
mircoles 17 de agosto de 11
Neumona
Prevencin
Conceptos Generales
Suprimir el tabaquismo es una medida fundamental para todo paciente.
- Factor de riesgo independiente de presentar neumona.
- Efecto directamente proporcional al nmero de paquetes/ao reducidos.
Neumococo es un objetivo importante de inmunizacin.
- Indicada en todo adulto mayor (>65 aos) y en pacientes de riesgo (2 a 64 aos).
- Neumo23 disminuye incidencia de episodios bacterimicos.
- Aplicable durante la convalecencia.
Lim WS, Bauddouin RC, George A, et Al. - BTS guidelines for the management of community acquired pneumonia in adults: update 2009
Thorax 2009 vol. 64 Suppl 3 pp. iii1-55
Lionel A Mandell, Richard G Wunderink, Antonio Anzueto,, et Al - Infectious Diseases Society of America/American Thoracic Society consensus
guidelines on the management of community-acquired pneumonia in adults
Clinical Infectious Diseases 2007 vol. 44 Suppl 2 pp. S27-72
Lisa A Jackson, Kathleen M Neuzil, Onchee Yu, et Al. - Effectiveness of pneumococcal polysaccharide vaccine in older adults
The New England Journal of Medicine 2003 vol. 348 (18) pp. 1747-55
mircoles 17 de agosto de 11
Neumona
Prevencin
T Jefferson, D Rivetti, A Rivetti, M Rudin, C Di Pietrantonj, V Demicheli - Efcacy and effectiveness of inuenza vaccines in elderly people: a systematic review
The Lancet 2005 vol. 366 (9492) pp. 1165-74
Inuenza
Articles
death from inuenza and pneumonia (26%), and prevent
admission for inuenza and pneumonia and for all
respiratory diseases (29%). Similarly, before adjustment,
inactivated inuenza and concomitant PPV in
individuals living in the community did not prevent
hospital admission for inuenza and pneumonia,
whereas after adjustment it did.
40,65,66
We identied ve randomised controlled trials
published over four decades and including just over
5000 observations. Given their heterogeneous nature by
vaccines tested (monovalent, trivalent, live, or inactivated
aerosol vaccines), setting, follow-up, and outcome
denition, no rm conclusions can be drawn from this
body of evidence. Two trials had adequate randomisation
and allocation concealment,
19,45
and one trial had
adequate measures to prevent attrition bias.
72
The results
of the most recent trial
19
are difcult to interpret because
of the presence of selection bias. Based on the results of a
meta-analysis of the two trials, inactivated vaccines were
more effective than placebo against inuenza-like disease
1170 www.thelancet.com Vol 366 October 1, 2005
0001 001
Favours treatment Favours control
01 1 10 100 1000
Subcategory and study
Outbreak and vaccine matching circulating strains
Feery, 1976
33
Horman, 1986
48
Saah 2, 1986
73
Fyson 1, 1983
41
Fyson 2, 1983
41
Goodman, 1982
44
Patriarca 1, 1985
67
Strassburg, 1986
76
Cartter 1, 1990
24
Cartter 2, 1990
24
Cartter 3, 1990
24
Meiklejohn 1, 1987
55
Taylor, 1992
78
Morens, 1995
57
Monto, 2001
56
Murayarna, 1999
59
Subtotal
Treatment
(n/N)
3/154
5/100
3/244
4/321
3/53
0/36
6/548
4/65
2/95
0/30
3/332
1/36
0/45
6/36
60/1728
0/60
100/3884
1/63
194 123 (0131158)
098 (024397)
033 (009122)
056 (015206)
1543 (08129346)
012 (001202)
025 (010060)
039 (010159)
242 (0124946)
060 (0031434)
057 (010337)
018 (002158)
038 (002920)
077 (050120)
038 (002909)
058 (041083)
141 (0102060)
462
512
519
115
125
943
455
110
100
299
202
099
138
2158
099
6530
419
330
237
608
125
448
1418
10000 046 (033063)
173
211
713
018 (003095)
018 (002133)
030 (009097)
060 (015249)
030 (014067)
007 (000115)
086 (008938)
022 (003187)
027 (009187)
014 (003063)
414
388
118
1338
3/59
8/214
5/224
0/118
9/84
21/470
3/19
0/46
1/55
2/126
3/19
1/52
0/3
28/623
1/68
86/2243
RR (95% Cl) Weight
(%)
Control
(n/N)
Test for heterogeneity:
2
=1562, p=041, I
2
=40%
Test for overall effect: Z=302, p=0003
Outbreak and matching absent or unknown
Ruden, 1974
71
Saah 1, 1986
73
Arroyo, 1984
21
Coles, 1992
27
Subtotal
Test for heterogeneity:
2
=492, p=018, I
2
=390%
Test for overall effect: Z=192, p=005
No outbreak and vaccine matching circulating strains
Patriarca 2, 1985
67
Carniniti, 1994
23
Deguchi, 2001
35
Subtotal
Test for heterogeneity:
2
=120, p=055, I
2
=0%
Test for overall effect: Z=220, p=003
No outbreak and matching absent or unknown
Howells 1, 1975
50
Howells 2, 1975
50
Howells 3, 1975
50
Saah 3, 1986
73
Subtotal
Test for heterogeneity:
2
=244, p=049, I
2
=0%
Test for overall effect: Z=293, p=0003
Total
Total events: 121 (treatment), 180 (Control)
Test for heterogeneity:
2
=2931, p=030, I
2
=113%
Test for overall effect: Z=479, p00001
121/16 357 180/15 822
7/665
1/134 15/356
3/123 22/267
0/183 11/287
3/225
2/339 4/119
2/169 1/73
1/10 739 5/11 723
5/226
53/1136
5/11 247 10/11 915
9/561
2/204
2/219
13/192
12/234
2/26 6/94
3/112 0/12
31/528
018 (004079)
115 (025538)
081 (0041474)
034 (011102)
Figure 3: Inuenza vaccines compared with no vaccination for prevention of deaths caused by inuenza or pneumonia in residents of long-term care facilities
by level of viral circulation and quality of vaccine matching
Numbers after names of authors indicate different datasets.
Reduccin
54%
Riesgo
relativo
mircoles 17 de agosto de 11
Neumona
Prevencin
T Jefferson, D Rivetti, A Rivetti, M Rudin, C Di Pietrantonj, V Demicheli - Efcacy and effectiveness of inuenza vaccines in elderly people: a systematic review
The Lancet 2005 vol. 366 (9492) pp. 1165-74
Inuenza
Articles
death from inuenza and pneumonia (26%), and prevent
admission for inuenza and pneumonia and for all
respiratory diseases (29%). Similarly, before adjustment,
inactivated inuenza and concomitant PPV in
individuals living in the community did not prevent
hospital admission for inuenza and pneumonia,
whereas after adjustment it did.
40,65,66
We identied ve randomised controlled trials
published over four decades and including just over
5000 observations. Given their heterogeneous nature by
vaccines tested (monovalent, trivalent, live, or inactivated
aerosol vaccines), setting, follow-up, and outcome
denition, no rm conclusions can be drawn from this
body of evidence. Two trials had adequate randomisation
and allocation concealment,
19,45
and one trial had
adequate measures to prevent attrition bias.
72
The results
of the most recent trial
19
are difcult to interpret because
of the presence of selection bias. Based on the results of a
meta-analysis of the two trials, inactivated vaccines were
more effective than placebo against inuenza-like disease
1170 www.thelancet.com Vol 366 October 1, 2005
0001 001
Favours treatment Favours control
01 1 10 100 1000
Subcategory and study
Outbreak and vaccine matching circulating strains
Feery, 1976
33
Horman, 1986
48
Saah 2, 1986
73
Fyson 1, 1983
41
Fyson 2, 1983
41
Goodman, 1982
44
Patriarca 1, 1985
67
Strassburg, 1986
76
Cartter 1, 1990
24
Cartter 2, 1990
24
Cartter 3, 1990
24
Meiklejohn 1, 1987
55
Taylor, 1992
78
Morens, 1995
57
Monto, 2001
56
Murayarna, 1999
59
Subtotal
Treatment
(n/N)
3/154
5/100
3/244
4/321
3/53
0/36
6/548
4/65
2/95
0/30
3/332
1/36
0/45
6/36
60/1728
0/60
100/3884
1/63
194 123 (0131158)
098 (024397)
033 (009122)
056 (015206)
1543 (08129346)
012 (001202)
025 (010060)
039 (010159)
242 (0124946)
060 (0031434)
057 (010337)
018 (002158)
038 (002920)
077 (050120)
038 (002909)
058 (041083)
141 (0102060)
462
512
519
115
125
943
455
110
100
299
202
099
138
2158
099
6530
419
330
237
608
125
448
1418
10000 046 (033063)
173
211
713
018 (003095)
018 (002133)
030 (009097)
060 (015249)
030 (014067)
007 (000115)
086 (008938)
022 (003187)
027 (009187)
014 (003063)
414
388
118
1338
3/59
8/214
5/224
0/118
9/84
21/470
3/19
0/46
1/55
2/126
3/19
1/52
0/3
28/623
1/68
86/2243
RR (95% Cl) Weight
(%)
Control
(n/N)
Test for heterogeneity:
2
=1562, p=041, I
2
=40%
Test for overall effect: Z=302, p=0003
Outbreak and matching absent or unknown
Ruden, 1974
71
Saah 1, 1986
73
Arroyo, 1984
21
Coles, 1992
27
Subtotal
Test for heterogeneity:
2
=492, p=018, I
2
=390%
Test for overall effect: Z=192, p=005
No outbreak and vaccine matching circulating strains
Patriarca 2, 1985
67
Carniniti, 1994
23
Deguchi, 2001
35
Subtotal
Test for heterogeneity:
2
=120, p=055, I
2
=0%
Test for overall effect: Z=220, p=003
No outbreak and matching absent or unknown
Howells 1, 1975
50
Howells 2, 1975
50
Howells 3, 1975
50
Saah 3, 1986
73
Subtotal
Test for heterogeneity:
2
=244, p=049, I
2
=0%
Test for overall effect: Z=293, p=0003
Total
Total events: 121 (treatment), 180 (Control)
Test for heterogeneity:
2
=2931, p=030, I
2
=113%
Test for overall effect: Z=479, p00001
121/16 357 180/15 822
7/665
1/134 15/356
3/123 22/267
0/183 11/287
3/225
2/339 4/119
2/169 1/73
1/10 739 5/11 723
5/226
53/1136
5/11 247 10/11 915
9/561
2/204
2/219
13/192
12/234
2/26 6/94
3/112 0/12
31/528
018 (004079)
115 (025538)
081 (0041474)
034 (011102)
Figure 3: Inuenza vaccines compared with no vaccination for prevention of deaths caused by inuenza or pneumonia in residents of long-term care facilities
by level of viral circulation and quality of vaccine matching
Numbers after names of authors indicate different datasets.
Nmero
163
a vacunar
mircoles 17 de agosto de 11
La neumona de la comunidad es una enfermedad frecuente y que puede ser
fatal en una minora de los casos
El manejo es guiado por la valoracin del riesgo de cada episodio y
antecedentes epidemiolgicos
Cuando no hay criterios de mejora debe pensarse en un diagnstico
alternativo o en una complicacin como primeras posibilidades
Inmunizaciones para neumococo e inuenza son recomendables al alta en
pacientes de riesgo
Neumona
Sntesis
mircoles 17 de agosto de 11
Felipe Martnez Lomakin
Programa de Especializacin en Medicina Interna
Neumona
Adquirida en la Comunidad
mircoles 17 de agosto de 11
You might also like
- Neumonía Extrahospitalaria (Adquirida en La Comunidad)Document40 pagesNeumonía Extrahospitalaria (Adquirida en La Comunidad)Alex B'DzNo ratings yet
- La pandemia del covid-19. Efectos sobre la saludFrom EverandLa pandemia del covid-19. Efectos sobre la saludRating: 5 out of 5 stars5/5 (1)
- ¿Tiene Este Niño NeumoníaDocument23 pages¿Tiene Este Niño NeumoníaEduardo GarciaNo ratings yet
- Vacuna contra el Virus del Papiloma Humano: La única vacuna cuestionada incluso por gran parte de la comunidad médicaFrom EverandVacuna contra el Virus del Papiloma Humano: La única vacuna cuestionada incluso por gran parte de la comunidad médicaNo ratings yet
- Neumonia PediatriaDocument11 pagesNeumonia Pediatriafernanda grendyNo ratings yet
- Panel Viral RespiratorioDocument2 pagesPanel Viral RespiratorioJesús BautistaNo ratings yet
- Enfrentando el COVID-19 con los beneficios del cannabis medicinalFrom EverandEnfrentando el COVID-19 con los beneficios del cannabis medicinalNo ratings yet
- Consenso Irab 2015 SapDocument24 pagesConsenso Irab 2015 SapRenzo FormiaNo ratings yet
- Neumonía Adquirida en La ComunidadDocument42 pagesNeumonía Adquirida en La ComunidadKatherine LazoNo ratings yet
- Joya Cervera Raul EdgardoDocument33 pagesJoya Cervera Raul EdgardoFreyyyyBmNo ratings yet
- Neumonia y Bronconeumonia Ped.Document16 pagesNeumonia y Bronconeumonia Ped.flores.fridasofia306No ratings yet
- pt164d PDFDocument6 pagespt164d PDFSarita GomezNo ratings yet
- Proyecto de InvestigaciónDocument31 pagesProyecto de Investigaciónsanchez erikaNo ratings yet
- Diagnostico Diferencial de Cuadros Respiratorios en Contexto AmbulatorioDocument36 pagesDiagnostico Diferencial de Cuadros Respiratorios en Contexto Ambulatorioeve.parada01No ratings yet
- Neumonias en Pediatria Consenso SVNCT 2005Document25 pagesNeumonias en Pediatria Consenso SVNCT 2005thefirstbrain_1No ratings yet
- Estudio de Caso - NeumoníaDocument24 pagesEstudio de Caso - NeumoníaBoni LimaNo ratings yet
- Precop NeumoniaDocument12 pagesPrecop Neumoniajohnsam93No ratings yet
- Guía de Manejo de NeumoníaDocument16 pagesGuía de Manejo de NeumoníaLinea Educativa Health & Life IPSNo ratings yet
- Neumonia ExtrahospitalariaDocument7 pagesNeumonia ExtrahospitalariaBenjamin PeregrinaNo ratings yet
- IAAS Hospital Mártires del 9 de Abril 2014-2017Document11 pagesIAAS Hospital Mártires del 9 de Abril 2014-2017Angel Navas NaranjoNo ratings yet
- Tuberculosis pleural: frecuencia, manifestaciones clínicas y métodos diagnósticosDocument6 pagesTuberculosis pleural: frecuencia, manifestaciones clínicas y métodos diagnósticosMariann BarahonaNo ratings yet
- Bacterol 2023Document10 pagesBacterol 2023yuly aleman cadenaNo ratings yet
- Revision Nac PediatriaDocument16 pagesRevision Nac PediatriaGeovanny IbaNo ratings yet
- NeumoniaDocument171 pagesNeumoniapepinillod13100% (1)
- Neumonía: definición, clasificación y tratamientoDocument54 pagesNeumonía: definición, clasificación y tratamientoRocío Hernández BustosNo ratings yet
- interciencia+medica_Vol13_N3_2Document9 pagesinterciencia+medica_Vol13_N3_2figohec203No ratings yet
- Mi Cop La SPM ADocument9 pagesMi Cop La SPM AGiovanni Ismael Reyes PérezNo ratings yet
- Neumo 1Document12 pagesNeumo 1NeriNo ratings yet
- Dx. de NeumoniaDocument9 pagesDx. de NeumoniaJohnny FernandezNo ratings yet
- Intro Ducci OnDocument21 pagesIntro Ducci OnAna guely santivañez mitmaNo ratings yet
- Neumonia en Pediatria PDFDocument6 pagesNeumonia en Pediatria PDFBoris Elio Canahuire VictorioNo ratings yet
- Articulo Infección Respiratoria en Paciente Oncológico - Rev Investigaciones AndinaDocument10 pagesArticulo Infección Respiratoria en Paciente Oncológico - Rev Investigaciones AndinaBlanca Ros Masry Mendoza PinzónNo ratings yet
- Agentes Etiológicos de La Neumonía Adquirida en La Comunidad NAC...Document11 pagesAgentes Etiológicos de La Neumonía Adquirida en La Comunidad NAC...Andres MahechaNo ratings yet
- Virus RespiratoriosDocument5 pagesVirus RespiratoriosRosario ParesNo ratings yet
- Caso Pediatrico Mario Calderon MontesDocument24 pagesCaso Pediatrico Mario Calderon Montesmario calderonNo ratings yet
- Neumonia Adquirida en La ComunidadDocument18 pagesNeumonia Adquirida en La ComunidadCris Isa LSNo ratings yet
- Factores de Riesgo Asociados A NeumoniaDocument7 pagesFactores de Riesgo Asociados A NeumoniaJonathan Huanacuni RamosNo ratings yet
- Universitas Médica 0041-9095: IssnDocument11 pagesUniversitas Médica 0041-9095: IssnlorenzNo ratings yet
- Clase 15 Neumonia Adquirida en La ComunidadDocument42 pagesClase 15 Neumonia Adquirida en La ComunidadClever SalazarNo ratings yet
- Neumonía Adquirida en La Comunidad PDFDocument18 pagesNeumonía Adquirida en La Comunidad PDFLinda MedinaNo ratings yet
- NeumoníaDocument45 pagesNeumoníaChristina Garcia100% (2)
- Nac - GVR 2020 10 17Document31 pagesNac - GVR 2020 10 17Jesus RodriguezNo ratings yet
- Resumen NeumoníaDocument12 pagesResumen NeumoníaAngello PereiraNo ratings yet
- Infecciones Por Mycoplasma Pneumoniae ChinaDocument4 pagesInfecciones Por Mycoplasma Pneumoniae Chinavovaco7476No ratings yet
- Enfermedades NosocomialesDocument26 pagesEnfermedades NosocomialesJavier Rosas RioseguraNo ratings yet
- 583-Texto Del Artículo-6041-1-10-20220718Document12 pages583-Texto Del Artículo-6041-1-10-20220718Karel ZertucheNo ratings yet
- PuryDocument5 pagesPuryagustina brandiNo ratings yet
- NEUMONIADocument10 pagesNEUMONIAShantal PierceNo ratings yet
- Utilidad de La Escala de Predicción DiagnósticaDocument7 pagesUtilidad de La Escala de Predicción DiagnósticaRosa ArrascueNo ratings yet
- Práctica de Infección de Vías AéreasDocument4 pagesPráctica de Infección de Vías AéreasVictor PrimoNo ratings yet
- Etiología y Diagnóstico de La Neumonía Adquirida en La Comunidad y Sus Formas ComplicadasDocument18 pagesEtiología y Diagnóstico de La Neumonía Adquirida en La Comunidad y Sus Formas ComplicadasJuan Carlos GutiérrezNo ratings yet
- 1620 110 4059 1 10 20220418Document6 pages1620 110 4059 1 10 20220418Taehyung KimNo ratings yet
- TBC Vih Sida Patron Radiologico 2017Document11 pagesTBC Vih Sida Patron Radiologico 2017Orion AtenasNo ratings yet
- VirusDocument6 pagesVirusNikkole VelascoNo ratings yet
- Neumonia PediatricaDocument11 pagesNeumonia PediatricapaolaNo ratings yet
- Marco TeóricoDocument6 pagesMarco TeóricoSara Sinai MoraNo ratings yet
- CEFALEA TENSIONAL: ETIOPATOGENIA Y TRATAMIENTODocument8 pagesCEFALEA TENSIONAL: ETIOPATOGENIA Y TRATAMIENTOAdler Hinostroza HuamanNo ratings yet
- Dine - 5ta Edición - Visa Digital ConciergeDocument42 pagesDine - 5ta Edición - Visa Digital ConciergeFelipe Cea100% (1)
- EUNACOM - Guias OftalmologicasDocument59 pagesEUNACOM - Guias OftalmologicasMario Felipe Sepúlveda Ávila100% (1)
- Apuntes de OftalmologiaDocument28 pagesApuntes de OftalmologiaFelipe CeaNo ratings yet
- Documento de ConsensoDocument127 pagesDocumento de ConsensoNelson MendietaNo ratings yet
- Compilado Guías GESDocument548 pagesCompilado Guías GESFlorangel Escalante Uzcategui0% (1)
- Dolor FacialDocument14 pagesDolor FacialFelipe CeaNo ratings yet
- Signos Vitales PediatriaDocument17 pagesSignos Vitales PediatriaFelipe CeaNo ratings yet
- VI 3 AnticoagulacionOralDocument3 pagesVI 3 AnticoagulacionOralFelipe CeaNo ratings yet
- Medicine - Cardiologia - 38 - Arritmias 1 PDFDocument53 pagesMedicine - Cardiologia - 38 - Arritmias 1 PDFFelipe CeaNo ratings yet
- Amir ReumatologiaDocument68 pagesAmir ReumatologiaAngie MirandaNo ratings yet
- Manual Oftalmológico de SupervivenciaDocument55 pagesManual Oftalmológico de SupervivenciaFelipe CeaNo ratings yet
- IAMDocument44 pagesIAMRodrigo Hemmelmann100% (2)
- GPC Mba Adulto HLC 2011Document27 pagesGPC Mba Adulto HLC 2011Felipe CeaNo ratings yet
- Endocrinologia AMIRDocument64 pagesEndocrinologia AMIRdantex_2029100% (10)
- Glomerulonefritis - Concepto y ClasificacionDocument7 pagesGlomerulonefritis - Concepto y ClasificacionFelipe Cea100% (1)
- Contenidos Examen Practico 2012Document1 pageContenidos Examen Practico 2012Felipe CeaNo ratings yet
- Displasias OseasDocument8 pagesDisplasias OseasFelipe Cea100% (1)
- Mini Manual Med. InternaDocument115 pagesMini Manual Med. InternaCamilaUgarteHumeres100% (6)
- Arancel Clinico 2019 PDF 745 KBDocument45 pagesArancel Clinico 2019 PDF 745 KBJean Pierre Fica100% (1)
- Medidas AntropometricasDocument37 pagesMedidas AntropometricasRuby Celeste BermúdezNo ratings yet
- Actualizaciones en FotoproteccionDocument9 pagesActualizaciones en FotoproteccionPriscillaNo ratings yet
- La Primera Infancia - El Desarrollo BiosocialDocument3 pagesLa Primera Infancia - El Desarrollo BiosocialANDREA mNo ratings yet
- Todo Sobre Sulfato de ApropinaDocument5 pagesTodo Sobre Sulfato de ApropinaeliastqNo ratings yet
- Psicología y CienciaDocument21 pagesPsicología y CienciaAnonymous 5tEhx3JNo ratings yet
- LLANTÉN - Quechua ExposicionDocument4 pagesLLANTÉN - Quechua ExposicionHM OmarNo ratings yet
- Simulacro UPCDocument8 pagesSimulacro UPCacarlinrNo ratings yet
- Prevencion y Manejo TVPDocument15 pagesPrevencion y Manejo TVPCristhian Camilo Martinez Torres100% (1)
- Lista de FarmacosDocument30 pagesLista de FarmacosKevin CastillaNo ratings yet
- Complicaciones Hipotiroidismo 1Document11 pagesComplicaciones Hipotiroidismo 1Yhogerlys LucenaNo ratings yet
- Signos Vitales en GeriatriaDocument22 pagesSignos Vitales en GeriatriaJulio Roberto Reyes Gordillo100% (2)
- Ansiedad y angustia: causas, síntomas y trastornos enDocument5 pagesAnsiedad y angustia: causas, síntomas y trastornos enRominaNo ratings yet
- ATLS Preguntas BásicasDocument7 pagesATLS Preguntas BásicasDaniel MorochoNo ratings yet
- Seguridad Primeros Auxilios - IIDocument88 pagesSeguridad Primeros Auxilios - IIJosé AbantoNo ratings yet
- TO vs FT: Una simple diferenciaDocument6 pagesTO vs FT: Una simple diferenciaAmarilis PalaciosNo ratings yet
- Contraindicaciones y advertencias de MikesanDocument2 pagesContraindicaciones y advertencias de MikesanDaiana Garcia VillarroelNo ratings yet
- Casos - Clinico - 1 - Depresion - y - Ansiedad - 17-I - 208 - 0 (Autoguardado)Document12 pagesCasos - Clinico - 1 - Depresion - y - Ansiedad - 17-I - 208 - 0 (Autoguardado)Anonymous iuy4yz4No ratings yet
- Consenso Hernia InguinalDocument24 pagesConsenso Hernia InguinalJuan Francisco Alvarez100% (1)
- ANXIA - NUM26 - PAG19articulo Ana AzarDocument7 pagesANXIA - NUM26 - PAG19articulo Ana Azarsofia valloryNo ratings yet
- Fármacos Modificadores Del Equilibrio de Sodio y AguaDocument2 pagesFármacos Modificadores Del Equilibrio de Sodio y AguaAmerico Hernandez HNo ratings yet
- Bronco AspiracionDocument32 pagesBronco AspiracionMarcos Manuel Vásquez MendozaNo ratings yet
- Fisioterapia PulmonarDocument5 pagesFisioterapia PulmonarJesús Fuentes100% (1)
- Hierba de San JuanDocument15 pagesHierba de San JuanLuis NagueraNo ratings yet
- Botiquin de EmergenciaDocument94 pagesBotiquin de EmergenciaMariano FernandezNo ratings yet
- QuemadurasDocument43 pagesQuemadurasSandra Giménez100% (1)
- Listado Formulas Magistrales y Preparados Oficinales 08 2019-1Document2 pagesListado Formulas Magistrales y Preparados Oficinales 08 2019-1Alexander EMendezNo ratings yet
- Resume NDocument2 pagesResume NalejandraNo ratings yet
- TF Plus Tri FormulaDocument2 pagesTF Plus Tri FormulaDelvis LeonNo ratings yet
- Anàlisis Apgar FamiliarDocument7 pagesAnàlisis Apgar FamiliarPeggy VtNo ratings yet
- Viaje a través del libro de ejercicios de un curso de milagros. Volumen 1From EverandViaje a través del libro de ejercicios de un curso de milagros. Volumen 1Rating: 4 out of 5 stars4/5 (8)
- El Monje Que Vendio Su Ferrari: Una Fábula EspiritualFrom EverandEl Monje Que Vendio Su Ferrari: Una Fábula EspiritualRating: 4.5 out of 5 stars4.5/5 (1696)
- Resetea tu mente. Descubre de lo que eres capazFrom EverandResetea tu mente. Descubre de lo que eres capazRating: 5 out of 5 stars5/5 (196)
- Disciplina con amor para adolescentes (Discipline With Love for Adolescents): Guía para llevarte bien con tu adolescente (A Guide for Getting Along Well With Your Adolescent)From EverandDisciplina con amor para adolescentes (Discipline With Love for Adolescents): Guía para llevarte bien con tu adolescente (A Guide for Getting Along Well With Your Adolescent)Rating: 5 out of 5 stars5/5 (10)
- Las seis etapas definitivas para superar tu divorcioFrom EverandLas seis etapas definitivas para superar tu divorcioRating: 4.5 out of 5 stars4.5/5 (10)
- ¡Tómate un respiro! Mindfulness: El arte de mantener la calma en medio de la tempestadFrom Everand¡Tómate un respiro! Mindfulness: El arte de mantener la calma en medio de la tempestadRating: 5 out of 5 stars5/5 (198)
- ¡Basta ya de ser un Tipo Lindo! (No More Mr. Nice Guy): Un Plan Probado para Que Obtengas Lo Que Quieras en La Vida El Sexo y El Amor (A Proven Plan for Getting What You Want in Love, Sex and Life)From Everand¡Basta ya de ser un Tipo Lindo! (No More Mr. Nice Guy): Un Plan Probado para Que Obtengas Lo Que Quieras en La Vida El Sexo y El Amor (A Proven Plan for Getting What You Want in Love, Sex and Life)Rating: 5 out of 5 stars5/5 (47)
- La Tabla Esmeralda: Incluye varias versiones y explicacionesFrom EverandLa Tabla Esmeralda: Incluye varias versiones y explicacionesRating: 4.5 out of 5 stars4.5/5 (7)
- Los 12 chakras: Desbloquea tus dones espiritualesFrom EverandLos 12 chakras: Desbloquea tus dones espiritualesRating: 4 out of 5 stars4/5 (14)
- Solo quiero que sepas: Lo que hemos aprendido y descubierto acerca de las relaciones amorosasFrom EverandSolo quiero que sepas: Lo que hemos aprendido y descubierto acerca de las relaciones amorosasRating: 5 out of 5 stars5/5 (38)
- Fuerza de voluntad: Cómo practicar y dominar el autocontrolFrom EverandFuerza de voluntad: Cómo practicar y dominar el autocontrolRating: 4.5 out of 5 stars4.5/5 (88)
- La Dieta Antiinflamatoria: Haz estos cambios simples y económicos en tu dieta y comienza a sentirte mejor dentro de 24 horas! (Spanish Edition)From EverandLa Dieta Antiinflamatoria: Haz estos cambios simples y económicos en tu dieta y comienza a sentirte mejor dentro de 24 horas! (Spanish Edition)Rating: 5 out of 5 stars5/5 (4)
- Despierta tu Energía Femenina: Secretos de Energía de la Diosa y Cómo Acceder a Tu Poder DivinoFrom EverandDespierta tu Energía Femenina: Secretos de Energía de la Diosa y Cómo Acceder a Tu Poder DivinoRating: 4 out of 5 stars4/5 (5)
- Cómo Conversar Con Cualquier Persona: Mejora tus habilidades sociales, desarrolla tu carisma, domina las conversaciones triviales y conviértete en una persona sociable para hacer verdaderos amigos y construir relaciones significativas.From EverandCómo Conversar Con Cualquier Persona: Mejora tus habilidades sociales, desarrolla tu carisma, domina las conversaciones triviales y conviértete en una persona sociable para hacer verdaderos amigos y construir relaciones significativas.Rating: 5 out of 5 stars5/5 (54)
- Aprende a poner límites: Cómo quererse a sí mismo sin lastimar a los demásFrom EverandAprende a poner límites: Cómo quererse a sí mismo sin lastimar a los demásRating: 4.5 out of 5 stars4.5/5 (225)
- La metamedicina. Cada síntoma es un mensaje: La curación a tu alcanceFrom EverandLa metamedicina. Cada síntoma es un mensaje: La curación a tu alcanceRating: 5 out of 5 stars5/5 (8)
- Entrenamiento Científico con pesas: Fitness InteligenteFrom EverandEntrenamiento Científico con pesas: Fitness InteligenteRating: 5 out of 5 stars5/5 (3)
- LOS ARCANOS DE NACIMIENTO: EL TAROT DEL ALMA: ¿CÓMO CALCULAR TU ARCANO PERSONAL O DE ALMA?From EverandLOS ARCANOS DE NACIMIENTO: EL TAROT DEL ALMA: ¿CÓMO CALCULAR TU ARCANO PERSONAL O DE ALMA?Rating: 5 out of 5 stars5/5 (8)