Professional Documents
Culture Documents
Central Venous Catheterization: To The Editor
Uploaded by
drpiratheepan42740 ratings0% found this document useful (0 votes)
18 views3 pagesMEDICINE
Original Title
MEDICAL PROCEDURE
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentMEDICINE
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
18 views3 pagesCentral Venous Catheterization: To The Editor
Uploaded by
drpiratheepan4274MEDICINE
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 3
correspondence
n engl j med 357;9 www.nejm.org august 30, 2007
943
Central Venous Catheterization
To the Editor: I have three concerns about the
description of central venous catheterization in
the video by Graham et al. (May 24 issue).
1
First,
it is misleading to describe the risk of hemotho-
rax as not applicable when the internal jugular
approach is used, since hemothorax is a known
complication.
2
Second, head rotation of 45 de-
grees increases the overlap of the carotid artery
by the internal jugular vein,
3
increasing the risk
of arterial puncture.
4
For this reason, most au-
thors recommend a near-midline position of the
head. Third, the manometer technique that is
shown is inadequate. Blood rising more than 30
cm in the vertical tube indicates arterial cathe-
terization; however, the absence of this increase
does not exclude the possibility of arterial punc-
ture if the needle tip abuts the artery wall. Arte-
rial puncture can be excluded only by filling the
horizontal catheter with more than 30 cm of
blood and then holding it upright and observing
a fall in the column. Finally, in light of the po-
tential for serious or fatal complications, it is
difficult to justify an attempt at central venous
catheterization without an experienced operator
present.
Michael C. Reade, M.B., B.S., D.Phil.
University of Pittsburgh
Pittsburgh, PA 15261
mreade@doctors.net.uk
Graham AS, Ozment C, Tegtmeyer K, Lai S, Braner DAV.
Central venous catheterization. N Engl J Med 2007;356:e21
(Web only). (Available at http://content.nejm.org/cgi/content/
short/356/21/e21/.)
Eisen LA, Narasimhan M, Berger JS, Mayo PH, Rosen MJ,
Schneider RF. Mechanical complications of central venous cath-
eters. J Intensive Care Med 2006;21:40-6.
Wang R, Snoey ER, Clements RC, Hern HG, Price D. Effect
of head rotation on vascular anatomy of the neck: an ultrasound
study. J Emerg Med 2006;31:283-6.
Sulek CA, Gravenstein N, Blackshear RH, Weiss L. Head
rotation during internal jugular vein cannulation and the risk of
carotid artery puncture. Anesth Analg 1996;82:125-8.
To the Editor: We welcome the emphasis on
sterility in the instructional video by Graham et
al., given the association of central venous cath-
eterization with bacteremia,
1
including infection
with methicillin-resistant Staphylococcus aureus.
2
However, we wish to emphasize the significant
variation in position of the jugular veins.
We undertook an audit of 100 patients who
were awaiting coronary angiography and found
1.
2.
3.
4.
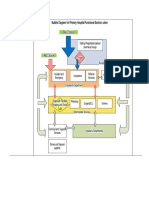
that 11% of right internal jugular veins and 24%
of left internal jugular veins were anterior and
medial to the carotid artery (Fig. 1). With the
use of the landmark technique described in the
video, safe catheterization of these veins will
probably be difficult, if not impossible. There-
fore, it is not surprising that the landmark tech-
nique carries a 9% risk of arterial puncture.
3
Furthermore, the degree of head rotation recom-
mended can have a significant effect on the posi-
tion of the vein.
4
Ultrasonography accurately locates the target
vein and also provides information about venous
pressure and the presence of intravascular throm-
bus. Its use should therefore be an integral part
of central venous catheterization.
James D. Newton, M.B., Ch.B.
David C. Sprigings, B.M., B.Ch.
Northampton General Hospital
Northampton NN1 5BD, United Kingdom
jdn1@le.ac.uk
Coello R, Charlett A, Ward V, et al. Device-related sources of
bacteraemia in English hospitals opportunities for the pre-
vention of hospital-acquired bacteraemia. J Hosp Infect 2003;53:
46-57.
Carnicer-Pont D, Bailey KA, Mason BW, Walker AM, Evans
MR, Salmon RL. Risk factors for hospital-acquired methicillin-
resistant Staphylococcus aureus bacteraemia: a case-control study.
Epidemiol Infect 2006;134:1167-73.
McGee DC, Gould MK. Preventing complications of central
venous catheterization. N Engl J Med 2003;348:1123-33.
Sulek CA, Gravenstein N, Blackshear RH, Weiss L. Head
rotation during internal jugular vein cannulation and the risk of
carotid artery puncture. Anesth Analg 1996;82:125-8.
To the Editor: The video by Graham et al.
shows a guidewire inducing premature ventricu-
1.
2.
3.
4.
33p9
AUTHOR:
FIGURE:
JOB: ISSUE:
4-C
H/T
RETAKE
SIZE
ICM
CASE
Line
H/T
Combo
Revised
AUTHOR, PLEASE NOTE:
Figure has been redrawn and type has been reset.
Please check carefully.
REG F
Enon
1st
2nd
3rd
Newton
1 of 1
08-30-07
ARTIST: ts
35709
R L
16%
60%
22%
2%
11%
62%
26%
1%
Figure 1. Distribution of Internal Jugular Vein According to
Quadrant.
The view is from the head of the bed, with the patients
head turned to the contralateral side. L denotes left
carotid artery, and R right carotid artery.
Downloaded from www.nejm.org on December 29, 2007 . Copyright 2007 Massachusetts Medical Society. All rights reserved.
T h e new engl and j ournal o f medicine
n engl j med 357;9 www.nejm.org august 30, 2007
944
lar contractions, illustrating a common problem
during insertion of central venous catheters: over-
insertion of guidewires. Intravenous guidewires,
commercially available in kits, are generally twice
as long as the catheters they guide, a length that
easily allows entry into cardiac chambers and re-
sults in arrhythmias.
1
We have observed transient
right bundle-branch block and ventricular fibril-
lation when overinserted guidewires entered the
right ventricle.
Overinsertion of guidewires occurs during the
initial placement of the wire and during advance-
ment of the catheter over the guidewire. We teach
that the distal end of the guidewire should never
be inserted past the top of the patients head
during catheterization of the right internal jugu-
lar vein and that the wire should be kept at this
position during advancement of the catheter. If a
guidewire requires withdrawal through the cath-
eter for control of the distal end, the guidewire
was inserted into the patient farther than neces-
sary. Avoidance of guidewire overinsertion can
be lifesaving in some patients.
Lisa T. Newsome, M.D.
Benjamin L. Antonio, D.O.
Roger L. Royster, M.D.
Wake Forest University School of Medicine
Winston-Salem, NC 27157-1009
Royster RL, Johnston WE, Gravlee GP, Brauer S, Richards D.
Arrhythmias during venous cannulation prior to pulmonary ar-
tery catheter insertion. Anesth Analg 1985;64:1214-6.
To the Editor: Sometimes ultrasonographic
guidance is not available for central venous cath-
eterization, so the operator must rely on surface
landmarks alone. In this situation it may be safer
if the patients head is in the neutral position. Head
rotation can cause the internal jugular vein to move
laterally in relation to surface landmarks and be-
come more difficult to locate.
1
Furthermore, the
vein can lie directly above the carotid artery,
2
in-
creasing the risk of arterial puncture. Using a
22-gauge needle to find and anchor the vein is
also useful.
3
This needle can be left in the vein to
guide the insertion of the introducer needle.
Another recognized complication is damage to
the guidewire.
4
This is avoided by nicking the
skin while the needle is in place and by retract-
ing the skin while inserting the dilator.
Finally, use of an introducer cannula rather
than the introducer needle minimizes the risk of
1.
laceration of the vein if the needle moves. This is
particularly useful if pressure transduction is re-
quired to check location before insertion of the
catheter.
Shaumik Adhya, M.B., B.S.
Conquest Hospital
St. Leonards-on-Sea TN37 7RD, United Kingdom
shaumik@doctors.org.uk
Shondipon K. Laha, M.A., F.R.C.A.
Lancashire Teaching Hospitals NHS Foundation Trust
Preston PR1 9HT, United Kingdom
Khatri VP, Wagner-Sevy S, Espinosa MH, Fisher JB. The in-
ternal jugular vein maintains its regional anatomy and patency
after carotid endarterectomy: a prospective study. Ann Surg 2001;
233:282-6.
Sulek CA, Gravenstein N, Blackshear RH, Weiss L. Head ro-
tation during internal jugular vein cannulation and the risk of
carotid artery puncture. Anesth Analg 1996;82:125-8.
Tripathi M, Pandey M. Anchoring of the internal jugular vein
with a pilot needle to facilitate its puncture with a wide bore
needle: a randomised, prospective, clinical study. Anaesthesia
2006;61:15-9.
Monaca E, Trojan S, Lynch J, Doehn M, Wappler F. Broken
guide wire a fault of design? Can J Anaesth 2005;52:801-4.
The authors reply: We regret that although our
video stresses not over-rotating the head, our text
refers to the classic teaching of positioning the
patient with the head rotated away from neutral.
1
It has become clear that as the head rotates away
from neutral, there is an increase in both the
overlap and proximity of the internal jugular vein
and carotid artery,
2
which increases the risk of
carotid puncture.
We agree that ultrasonography enhances the
rate of success of internal jugular venous catheter-
ization, speeds the process, demonstrates impor-
tant anatomical variations, demonstrates vessel
thromboses, and decreases complications, includ-
ing catheter-related bloodstream infections.
3
We
appreciate Reades comment that hemothorax is
a rare but potentially serious complication of
internal jugular venous catheterization. Ultrason-
ographic guidance may reduce the risk of hemo-
thorax from 1.7% to zero.
3
Unfortunately, ultra-
sonography is not universally available and
ultrasound devices may fail to operate; there-
fore, knowledge of the landmark technique re-
mains essential.
We agree with Newsome et al. that guidewire
overinsertion can be dangerous. The wire needs
to be advanced only far enough to maintain reli-
able control of the tract from the skin surface to
the intravascular space.
1.
2.
3.
4.
Downloaded from www.nejm.org on December 29, 2007 . Copyright 2007 Massachusetts Medical Society. All rights reserved.
correspondence
n engl j med 357;9 www.nejm.org august 30, 2007
945
Adhya and Laha suggest nicking the skin while
the needle remains in place, which may prove
useful as long as the operator takes care not to
cause damage by inadvertent movement of the
indwelling needle during the process. They also
refer to an interesting study that describes the use
of a small-gauge pilot needle to locate the internal
jugular vein and an innovative technique to then
stabilize it.
4
This small-gauge pilot needle may be
particularly useful when patients have coagulop-
athy or when ultrasonography is not available.
We agree that, ideally, an experienced opera-
tor should be present for all central venous cath-
eterization procedures. This is especially impor-
tant for patients with known risk factors for
difficult catheterization.
Alan S. Graham, M.D.
Ken Tegtmeyer, M.D.
Dana Braner, M.D.
Oregon Health and Science University
Portland, OR 97239
grahamal@ohsu.edu
McGee DC, Gould MK. Preventing complications of central
venous catheterization. N Engl J Med 2003;348:1123-33.
Wang R, Snoey ER, Clements RC, Hern HG, Price D. Effect
of head rotation on vascular anatomy of the neck: an ultrasound
study. J Emerg Med 2006;31:283-6.
Karakitsos D, Labropoulos N, De Groot E, et al. Real-time
ultrasound-guided catheterisation of the internal jugular vein:
a prospective comparison with the landmark technique in criti-
cal care patients. Crit Care 2006;10:R162.
Tripathi M, Pandey M. Anchoring of the internal jugular vein
with a pilot needle to facilitate its puncture with a wide bore
needle: a randomised, prospective, clinical study. Anaesthesia
2006;61:15-9.
1.
2.
3.
4.
Long-Term Follow-up after Treatment of Rabies
by Induction of Coma
To the Editor: In 2005, Willoughby and col-
leagues
1
reported on a 15-year-old girls survival
from rabies encephalitis the sixth such case
that had been reported in humans after treat-
ment with a novel therapeutic regimen that in-
cluded ketamine, ribavirin, and amantadine. Five
months after exposure, she still had dysarthria,
weakness in the left hand and foot, bilateral ex-
tensor plantar response, generalized choreoath-
etosis, intermittent dystonia, and a lurching gait.
Here we report on the functional outcomes 18
months and 27 months after her initial exposure
to a rabid bat.
Her generalized choreoathetosis completely re-
solved by 2006. A trial of therapy with carbidopa
levodopa caused worsening of abnormalities in
her gait. A cerebrospinal fluid analysis in Sep-
tember 2005 showed normalization of the pro-
tein level and the white-cell count, with decreased
levels of biopterin. Eighteen months after her
exposure to rabies, her dysarthria and gait ab-
normalities had significantly improved, but she
could not return to her previous level of partici-
pation in sports. She resumed classes full time
in high school without having difficulties with
either learning or memory.
On neurologic examination, the patient showed
no choreoathetoid movements during four sepa-
rate visits with three neurologists and two reha-
bilitation specialists. She had normal affect and
cognition, ataxic dysarthria (see video, available
with the full text of this letter at www.nejm.org),
and normal cranial-nerve functions. Also evi-
dent in the video are both mild weakness in the
left foot dorsiflexor and mild dystonia in the left
hand, without weakness on surface electromy-
ography. She also had slowed alternating move-
ments in the left hand and fingers and paresthe-
sia in the region of the bat bite. Her deep-tendon
reflexes were symmetric throughout, and her
plantar responses were flexor. She had mild
ataxia, especially during running (see video).
Analysis of the cerebrospinal fluid showed six
unique oligoclonal bands. A mildly elevated
level of neopterin and decreased levels of 5-hy-
droxyindoleacetic acid and homovanillic acid
suggested decreased turnover of dopamine and
serotonin. Magnetic resonance imaging of the
brain showed resolution of the hyperintensities
in the basal ganglia that had been seen on T
2
-
weighted images in November 2004.
Twenty-seven months after exposure, the pa-
tient continued to have fluctuating dysarthria and
gait difficulties, plus an intermittent sensation
of cold in the feet. She had no difficulties with
her instrumental activities of daily living, includ-
ing driving. In high school, she took college-level
courses in English, physics, and calculus. She
scored above average on a national college achieve-
ment test, graduated from high school in 2007,
Downloaded from www.nejm.org on December 29, 2007 . Copyright 2007 Massachusetts Medical Society. All rights reserved.
You might also like
- Clinical Handbook of Cardiac ElectrophysiologyFrom EverandClinical Handbook of Cardiac ElectrophysiologyBenedict M. GloverNo ratings yet
- Cardiac Surgical Operative AtlasFrom EverandCardiac Surgical Operative AtlasThorsten WahlersNo ratings yet
- Ultrasound Guided Internal Jugular Vein Nejm 2010Document4 pagesUltrasound Guided Internal Jugular Vein Nejm 2010Flávio VillaNo ratings yet
- Retained Catheter Fragment From A Fractured Tunneled Catheter-A Rare and Potentially Lethal ComplicationDocument4 pagesRetained Catheter Fragment From A Fractured Tunneled Catheter-A Rare and Potentially Lethal ComplicationMahmoud DiaaNo ratings yet
- HematopneumothoraxDocument13 pagesHematopneumothoraxtri_budi_20No ratings yet
- Accepted Manuscript: 10.1016/j.cjtee.2015.12.015Document8 pagesAccepted Manuscript: 10.1016/j.cjtee.2015.12.015Desak PramestiNo ratings yet
- Interventional Radiology In-Training Test Questions For Diagnostic Radiology ResidentsDocument8 pagesInterventional Radiology In-Training Test Questions For Diagnostic Radiology ResidentsMark M. AlipioNo ratings yet
- Placement of Arterial Line: Renae Stafford, MDDocument7 pagesPlacement of Arterial Line: Renae Stafford, MDBotond LukacsNo ratings yet
- Central Venous Catheters in Children and Neonates - What Is ImportantDocument8 pagesCentral Venous Catheters in Children and Neonates - What Is ImportantangelicaNo ratings yet
- 2017 Ultrasound-Guided Central Venous CatheterizationDocument14 pages2017 Ultrasound-Guided Central Venous Catheterizationeswin yoelNo ratings yet
- Hemoglobinuria Aortic Valve Bypass For Aortic Stenosis in A Patient With Paroxysmal NocturnalDocument5 pagesHemoglobinuria Aortic Valve Bypass For Aortic Stenosis in A Patient With Paroxysmal NocturnalmoplkiNo ratings yet
- American Journal of Emergency Medicine - Cardiac TamponadeDocument3 pagesAmerican Journal of Emergency Medicine - Cardiac TamponadefloNo ratings yet
- ArtigosDocument6 pagesArtigosIgor PiresNo ratings yet
- Accepted Manuscript: Cardiovascular Revascularization MedicineDocument19 pagesAccepted Manuscript: Cardiovascular Revascularization MedicineNasriNo ratings yet
- Slide, Tracheal BronchusDocument4 pagesSlide, Tracheal Bronchusemmanuel le bretNo ratings yet
- A Case of Intra-Operative Injury To Left Main Pulmonary Artery Repaired With A Pericardial PatchDocument7 pagesA Case of Intra-Operative Injury To Left Main Pulmonary Artery Repaired With A Pericardial PatchIJAR JOURNALNo ratings yet
- Surgical Management of Tracheal Compression Caused by Mediastinal Goiter: Is Extracorporeal Circulation Requisite钥Document3 pagesSurgical Management of Tracheal Compression Caused by Mediastinal Goiter: Is Extracorporeal Circulation Requisite钥Indra W SaputraNo ratings yet
- Placement of An Arterial LineDocument2 pagesPlacement of An Arterial Linem0ka7No ratings yet
- Modi Fied Blalock Taussig Shunt: A Not-So-Simple Palliative ProcedureDocument7 pagesModi Fied Blalock Taussig Shunt: A Not-So-Simple Palliative ProcedureJakler NicheleNo ratings yet
- ICU Imaging: Joshua R. Hill, MD, Peder E. Horner, MD, Steven L. Primack, MDDocument18 pagesICU Imaging: Joshua R. Hill, MD, Peder E. Horner, MD, Steven L. Primack, MDJackee_BlackNo ratings yet
- Case Report - Late Mitral Valve Regurgitation After Bullet Wound To The Heart (Short Communication)Document3 pagesCase Report - Late Mitral Valve Regurgitation After Bullet Wound To The Heart (Short Communication)fluid_man_brazilNo ratings yet
- Echocardiography Dissertation IdeasDocument8 pagesEchocardiography Dissertation IdeasWhoCanWriteMyPaperForMeCanada100% (1)
- A Rare Case of Vertebral Artery Pseudoaneurysmas An Iatrogenic ComplicationDocument4 pagesA Rare Case of Vertebral Artery Pseudoaneurysmas An Iatrogenic ComplicationIOSRjournalNo ratings yet
- Title:-Re-entrant Ventricular Tachycardia in A Post-Operative Case of Tetralogy of Fallot - Ablated Successfully UnderDocument10 pagesTitle:-Re-entrant Ventricular Tachycardia in A Post-Operative Case of Tetralogy of Fallot - Ablated Successfully UnderpaidisuriNo ratings yet
- Medical Devices of The ChestDocument22 pagesMedical Devices of The ChestJose David Flores PérezNo ratings yet
- Subclavian Vein Catheter Extravasation-Insufficient Catheter Length As A Probable Causal FactorDocument7 pagesSubclavian Vein Catheter Extravasation-Insufficient Catheter Length As A Probable Causal Factorwouter PieteraerensNo ratings yet
- Thyroid MetsDocument3 pagesThyroid MetsQusai Al JarrahNo ratings yet
- Symptomatic Central Venous Stenosis in A Hemodialysis Patient Leading To Loss of Arteriovenous Access: A Case Report and Literature ReviewDocument5 pagesSymptomatic Central Venous Stenosis in A Hemodialysis Patient Leading To Loss of Arteriovenous Access: A Case Report and Literature ReviewDivara SyautaNo ratings yet
- Correspondence: Christophe Acar, MDDocument5 pagesCorrespondence: Christophe Acar, MDRouçadi WafaaNo ratings yet
- Tmp30e6 TMPDocument4 pagesTmp30e6 TMPFrontiersNo ratings yet
- Case Report: Middle Aortic Syndrome Treated by Implantation of An Advanta V12 Large Diameter StentDocument3 pagesCase Report: Middle Aortic Syndrome Treated by Implantation of An Advanta V12 Large Diameter StentLenardR.ApazaNo ratings yet
- Jurnal Coronary Artery FistulaDocument3 pagesJurnal Coronary Artery FistulaRistinyaUnuyNo ratings yet
- Resuscitativeendovascular Balloonocclusionofthe Aorta:: A Practical ReviewDocument18 pagesResuscitativeendovascular Balloonocclusionofthe Aorta:: A Practical ReviewJulian SanchezNo ratings yet
- Lung BiopsyDocument8 pagesLung BiopsySiya PatilNo ratings yet
- Althoff 2023Document2 pagesAlthoff 2023Marcos DuarteNo ratings yet
- Central Shunting For Tetralogy of Fallot After Original Blalock Taussig Shunt in A 34 Year Old WomanDocument4 pagesCentral Shunting For Tetralogy of Fallot After Original Blalock Taussig Shunt in A 34 Year Old WomanAthenaeum Scientific PublishersNo ratings yet
- Aaa RotoDocument11 pagesAaa RotoKarely TapiaNo ratings yet
- Letters: Safety of Angioplasty For Intracranial Artery ReferencesDocument5 pagesLetters: Safety of Angioplasty For Intracranial Artery Referencesaula nisafitriNo ratings yet
- Anatomical Considerations and Emerging StrategiesDocument21 pagesAnatomical Considerations and Emerging StrategiesPatus QuakusNo ratings yet
- Er Medicine ReviewDocument16 pagesEr Medicine Reviewsdb10cNo ratings yet
- Materials and MethodsDocument6 pagesMaterials and MethodsJoannah D.S. Del RosarioNo ratings yet
- Cardiac SurgeryDocument41 pagesCardiac Surgeryapi-3840195100% (4)
- J HLC 2020 09 872Document2 pagesJ HLC 2020 09 872aswedi nersNo ratings yet
- (FEU) Central Venous Pressure Notes PDFDocument25 pages(FEU) Central Venous Pressure Notes PDFBryJos tiongsonNo ratings yet
- Caso Clinico Sp3Document4 pagesCaso Clinico Sp3eduardoNo ratings yet
- MJMHS 1316Document3 pagesMJMHS 1316prima ningratNo ratings yet
- Ultrasound-Guided Interventions of The Cervical Spine and NervesDocument12 pagesUltrasound-Guided Interventions of The Cervical Spine and NervestriNo ratings yet
- Letters To The EditorDocument2 pagesLetters To The EditorRajan KarmakarNo ratings yet
- Blunt Thoracic TraumaDocument3 pagesBlunt Thoracic TraumaNetta LionoraNo ratings yet
- Basicultrasound-Guided Procedures: Laurel Barr,, Nicholas Hatch,, Pedro J. Roque,, Teresa S. WuDocument30 pagesBasicultrasound-Guided Procedures: Laurel Barr,, Nicholas Hatch,, Pedro J. Roque,, Teresa S. WuKenzo HongThanhNo ratings yet
- Saline Flush TestDocument5 pagesSaline Flush TestHandrian RahmanNo ratings yet
- Hollehorst PlaquesDocument3 pagesHollehorst PlaquesErick Roa GandicaNo ratings yet
- The Expanding Role of Peri Procedural EchocardiogrDocument2 pagesThe Expanding Role of Peri Procedural Echocardiogrxrszbkr77dNo ratings yet
- Pleural Procedures in Critically Ill PatientsDocument9 pagesPleural Procedures in Critically Ill PatientsFlávio VillaNo ratings yet
- Congenital Anomalies of The Aortic Arch A Comprehensive ReviewDocument5 pagesCongenital Anomalies of The Aortic Arch A Comprehensive ReviewWeb ResearchNo ratings yet
- 394 Endovascular Hunterian LigationDocument6 pages394 Endovascular Hunterian Ligationlonsilord17No ratings yet
- Arab Board Exam 2 With AnswersDocument31 pagesArab Board Exam 2 With Answersahmed.farag.ali2020No ratings yet
- Pulmonary Endarterectomy: Experience and Lessons Learned in 1,500 CasesDocument8 pagesPulmonary Endarterectomy: Experience and Lessons Learned in 1,500 CasesRoxana Maria MunteanuNo ratings yet
- Cardiac CatheterizationDocument9 pagesCardiac CatheterizationAnurag Gupta100% (1)
- Trial of Endovascular Thrombectomy For Large Ischemic StrokesDocument13 pagesTrial of Endovascular Thrombectomy For Large Ischemic StrokesMABEL LUCERO OLARTE JURADONo ratings yet
- Congental Adrenal HyperplasiaDocument19 pagesCongental Adrenal Hyperplasiadrpiratheepan4274No ratings yet
- Spirometer Handbook NacaDocument24 pagesSpirometer Handbook NacaebrycNo ratings yet
- PACES - Abdominal MarksheetsDocument2 pagesPACES - Abdominal Marksheetsdrpiratheepan4274No ratings yet
- 6th Central Pay Commission Salary CalculatorDocument15 pages6th Central Pay Commission Salary Calculatorrakhonde100% (436)
- Licorice AbuseDocument14 pagesLicorice Abusedrpiratheepan4274No ratings yet
- Spirometer Handbook NacaDocument24 pagesSpirometer Handbook NacaebrycNo ratings yet
- Adrenal GuidelinesDocument20 pagesAdrenal GuidelinesUtziel Abel Carrillo GonzalezNo ratings yet
- Adrenal GuidelinesDocument20 pagesAdrenal GuidelinesUtziel Abel Carrillo GonzalezNo ratings yet
- DM in Aids PatientDocument10 pagesDM in Aids Patientdrpiratheepan4274No ratings yet
- EndocrinologyDocument60 pagesEndocrinologyrinahn100% (1)
- Insuline Tolerance TestDocument2 pagesInsuline Tolerance Testdrpiratheepan4274No ratings yet
- Blue Book - Guidelines For The Control of Infectious DiseaseDocument271 pagesBlue Book - Guidelines For The Control of Infectious DiseaseavarathunnyNo ratings yet
- TFT Guideline Final Version July 2006Document86 pagesTFT Guideline Final Version July 2006Boris Miguel HernándezNo ratings yet
- Metabolic Syndrome DiagnosisDocument4 pagesMetabolic Syndrome Diagnosisdrpiratheepan4274No ratings yet
- Intubation Review: SFC HillDocument26 pagesIntubation Review: SFC Hilldrpiratheepan4274No ratings yet
- Australian Doctor Flying and HealthDocument6 pagesAustralian Doctor Flying and Healthdrpiratheepan4274No ratings yet
- Familial Hyperlipidaemia Risk AssessmentDocument7 pagesFamilial Hyperlipidaemia Risk Assessmentdrpiratheepan4274No ratings yet
- DM NewDocument8 pagesDM Newdrpiratheepan4274No ratings yet
- LongActingGLP-1RAgonists 2011Document6 pagesLongActingGLP-1RAgonists 2011madelosriosNo ratings yet
- Diagnosis and Treatment of Peripheral Arterial DiseaseDocument5 pagesDiagnosis and Treatment of Peripheral Arterial Diseasedrpiratheepan4274No ratings yet
- Intubacion OrotraquealDocument5 pagesIntubacion OrotraquealEduardo SantosNo ratings yet
- Positive-Pressure Ventilation With A Face Mask and A Bag-Valve DeviceDocument3 pagesPositive-Pressure Ventilation With A Face Mask and A Bag-Valve Devicedrpiratheepan4274No ratings yet
- Gestatational DMDocument65 pagesGestatational DMdrpiratheepan4274No ratings yet
- 'S Assessment SeriesDocument22 pages'S Assessment Seriesdrpiratheepan4274No ratings yet
- BUDDHIST ERA 2556 - 2557: Victory Belongs To The Most PerseveringDocument1 pageBUDDHIST ERA 2556 - 2557: Victory Belongs To The Most Perseveringsamitha505No ratings yet
- CEM4719 Noradrenaline v2Document1 pageCEM4719 Noradrenaline v2drpiratheepan4274No ratings yet
- Adrenaline Intravenous Infusion CalculationsDocument1 pageAdrenaline Intravenous Infusion Calculationsdrpiratheepan4274No ratings yet
- Technical Comparison of On-Line vs. Line-Interactive UPS DesignsDocument14 pagesTechnical Comparison of On-Line vs. Line-Interactive UPS Designsdrpiratheepan4274No ratings yet
- Drug Infusions For Intensive CareDocument2 pagesDrug Infusions For Intensive CarejaionlyNo ratings yet
- Medimanet: Recent Achievements in Drug Library and Safety TechnologyDocument2 pagesMedimanet: Recent Achievements in Drug Library and Safety TechnologyDiani VargasNo ratings yet
- Maternal Collapse During PregnancyDocument57 pagesMaternal Collapse During PregnancytapayanaNo ratings yet
- Response in OppositionDocument36 pagesResponse in OppositionForeclosure FraudNo ratings yet
- Plazma Ionizarot CP 212 Eng ManualDocument1 pagePlazma Ionizarot CP 212 Eng ManualVladimirDulaNo ratings yet
- Ammonia SafetyDocument46 pagesAmmonia SafetyMikechal AwacayNo ratings yet
- Jurnal GadarDocument6 pagesJurnal GadarLycia Dwi LindiyaniNo ratings yet
- Surgical Handicraft Manual For Surgical Residents 2015 PDFDocument295 pagesSurgical Handicraft Manual For Surgical Residents 2015 PDFNamerahN100% (3)
- Project PrimaryDocument7 pagesProject PrimaryLisanwork HonseboNo ratings yet
- REPORT ON YOGA RESEARCH STUDIES AT ACYTER, JIPMER: 2008 To 2012.Document126 pagesREPORT ON YOGA RESEARCH STUDIES AT ACYTER, JIPMER: 2008 To 2012.Yogacharya Dr Ananda Balayogi BhavananiNo ratings yet
- Bereavement SupportDocument26 pagesBereavement SupportAdiAri RosiuNo ratings yet
- Tiger Paint Remover SDSDocument10 pagesTiger Paint Remover SDSBernard YongNo ratings yet
- Segmentos Ica 2022 PDFDocument9 pagesSegmentos Ica 2022 PDFRoberto RodríguezNo ratings yet
- Dictation. Fill in The Gaps With A Word From The ListeningDocument1 pageDictation. Fill in The Gaps With A Word From The ListeningNU MaseNo ratings yet
- Fundamentals of Nursing Part 1Document8 pagesFundamentals of Nursing Part 1Evergreen Verds100% (1)
- Capa SopDocument23 pagesCapa SopHaroon Rasheed100% (3)
- M265 Lec 13 - Epidemiology and Public HealthDocument10 pagesM265 Lec 13 - Epidemiology and Public HealthSawsan Z. JwaiedNo ratings yet
- Addis Ababa Science and Technology University (AASTU)Document24 pagesAddis Ababa Science and Technology University (AASTU)Wasihun DanielNo ratings yet
- Cats and BatsDocument1 pageCats and BatsTâniaNo ratings yet
- UltraCal XS PDFDocument2 pagesUltraCal XS PDFKarina OjedaNo ratings yet
- QA/QC of Nuclear Medicine Imaging Equipment - Current PracticesDocument38 pagesQA/QC of Nuclear Medicine Imaging Equipment - Current PracticesRosendo DacuyanNo ratings yet
- Female Foeticide in India A Bitter Truth FinalDocument22 pagesFemale Foeticide in India A Bitter Truth Finalaman manderNo ratings yet
- Triamcinolone AcetonideDocument12 pagesTriamcinolone Acetonideawais khanNo ratings yet
- Mh25 Borderline Personality GuidelineDocument182 pagesMh25 Borderline Personality GuidelineAbdul Hakim Abdul KadirNo ratings yet
- Caz 4Document17 pagesCaz 4Marinela MeliszekNo ratings yet
- MSDS STA Neoplastine CI PlusDocument8 pagesMSDS STA Neoplastine CI Plusasmaul husnahNo ratings yet
- What Does A QHSE Engineer or Safety Officer Job Description Include?Document2 pagesWhat Does A QHSE Engineer or Safety Officer Job Description Include?Sohail Ayub ButtNo ratings yet
- Physiology Practical 2: Toad HeartDocument10 pagesPhysiology Practical 2: Toad HeartAdams OdanjiNo ratings yet
- Caries Risk Assesment: Disha Jandial Mds 1 Year Deptt. of Pediatrics and Preventive DentistryDocument134 pagesCaries Risk Assesment: Disha Jandial Mds 1 Year Deptt. of Pediatrics and Preventive Dentistrydisha 146jandial100% (1)
- Course 1.2: What You Should KnowDocument27 pagesCourse 1.2: What You Should KnowGeorgios MilitsisNo ratings yet
- Risk Management in Military AviationDocument16 pagesRisk Management in Military AviationSp AndaNo ratings yet