Professional Documents
Culture Documents
CDH Modern MX
Uploaded by
phobicmdOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
CDH Modern MX
Uploaded by
phobicmdCopyright:
Available Formats
Seminars in Pediatric Surgery (2008) 17, 244-254
Congenital diaphragmatic hernia: a modern day approach
Karl-Ludwig Waag, MD,a Steffan Loff, MD,a Katrin Zahn, Mansour Ali, MD,a Steffen Hien, MD,b Markus Kratz, MD,b Wolfgang Neff, MD,c Regine Schaffelder, MD,d Thomas Schaible, MDb
From the Department of aPediatric Surgery, University Hospital, Mannheim, Germany; b Department of Pediatrics, University Hospital, Mannheim, Germany; c Department of Radiology, University Hospital, Mannheim, Germany; and the d Department of Obstetrics, University Hospital, Mannheim, Germany. KEYWORDS
Congenital diaphragmatic hernia; CDH; Prognostic factors; ECMO; Treatment Centralization of all complicated congenital diaphragmatic hernias (CDH) was organized in Germany from 1998, collecting 325 consecutive patients with striking increasing survival rates. This series report 244 patients from 2002 to 2007. Today, large defects are detected early in pregnancy by ultrasound and magnetic resonance imaging (MRI). In extracorporeal membrane oxygenation (ECMO) patients, prenatal lung head ratio (LHR) was 1.2 (median) at the 34th week of gestation or less than 25 ml lung tissue in MRI. This means that all patients below LHR of 1.4 should be transferred prenatally in a tertiary center. High risk group for survival was dened as LHR below 0.9, ie, 10 ml in MRI planimetry. Inborn patients show better results than outborns. In algorithm therapy, gentle ventilation plays an important role in preventing damage to the lung tissue and avoiding long term ventilation. When PaCO2 was more than 75 mmHg, ventilation was changed to high frequency oscillatory ventilation (HFOV). Indication for ECMO was seen in preductal PaO2 less than 50 mmHg over 2-4 h or less than 40 mmHg over 2 h. ECMO related risks included intracerebral bleeding (9%), intrapulmonary bleeding (14%), and convulsions (16%). Surgically, a longitudinal midline incision for exposure of the defect, the duodenal kinking, and probably for abdominal patching was perfect. A cone formed goretex patch provided more abdominal space and reduced abundant intrathoracical cavity. No drain was used. Postoperatve complications were described. Overall survival in 244 consecutive patients was 86.5% for all patients born alive. All those who needed ECMO survived in 71%, underlining ECMO as a treatment of last choice. Follow-up for quality of life after CDH is described. 2008 Published by Elsevier Inc.
Embryologically, the diaphragm develops during the 8th and 12th weeks of gestation. A membrane (septum transversum) separates the thoracic from the abdominal cavity. Septum transversum growth starts anteriorly and dorsally. The pleurocardial space is then divided from the peritoneal area. These pleuroperitoneal folds consist primarily of pleural membrane and peritoneum. Later, musAddress reprint requests and correspondence: Karl-Ludwig Waag, MD, University Hospital, Department of Pediatric Surgery, Theodor Kutzer Ufer 1-3, Mannheim 68167, Germany. E-mail: karl-ludwig.waag@kch.ma.uni-heidelberg.de. 1055-8586/$ -see front matter 2008 Published by Elsevier Inc. doi:10.1053/j.sempedsurg.2008.07.009
cle bers migrate into this membrane from anterior to posterior. Due to the late closure of this membrane on the left side, left diaphragmatic hernias are more common (87% left versus 11% right, 2% are bilateral) and are predominantly posterior. The last to close is called the pleuroperitoneal canal. Dorsal defects are called Bochdalek hernia, and anterior defects are named Morgagni hernia. Larrey described a rare form of sternocostal defect. Esophageal lengthening occurs at the same time as the growth of the septum transversum. Any delay results in a wide open hiatus and short esophagus.
Waag et al.
Congenital Diaphragmatic Hernia
245
Figure 3 Different thickness of muscle bers under normal, CDH, and ECMO conditions.
Etiology
Figure 1 Specimens of the lung in control and CDH, showing rarication of all bronchi and hypoplasia. (Color version of gure is available online.)
When there is a defect in muscle ber growth and bers do not move into the pleuroperitoneal membrane sufciently, the result will be a true diaphragmatic hernia. In these cases, there is a hernial sac, or in case of hypoplastic muscle bers, a congenital diaphragmatic eventration. The timing of the development of the defect is important because of the duration of compressing the ipsi- and contralateral lung. In large defects, the intrathoracic position of the left liver lobe, stomach, spleen, and gut leads to early compression of lung tissue and mediastinal shift. These are the cases that are detected early in pregnancy.
Most defects develop as isolated defects, ie, sporadically (70%). There are other factors involved in about 20% detected on experiments, such as in relation to medications like thalidomide or nitrofen and vitamin-A deciency. Diaphragmatic defects are seen as well in trisomy 13, 18, or 21 in 8%, such as in Beckwith Wiedemann and Danny Drash syndrome. Familial conditions are rare (2%). Here, chromosomal deviations are located on chromosome 15q26. Gene mutation is seen in deletion of 4p, 8q, 15q or as duplication of 8p and as tetrasomy 12p.
Pathophysiology
The pathophysiology of this condition is thought to be as follows: Loss of lung function can be explained by loss of space to develop. But other structural deciencies are added, like rarication of bronchi and lung vessels (Figure 1). Thickening of alveolar membrane is veried histologically. Hypertrophy of media can be found in periphery of lung vessels resulting in smaller lumina, whereas these media muscle bers are regulating blood ow only in central, big lung vessels (Figures 2 and 3). These alterations are found not only in ipsilateral but also in contralateral lung. Thus, mechanical reasons cannot explain the structural maldevelopment of contralateral lung. All children suffer from persistent pulmonary hypertension, which plays an important factor for treatment. In respect to reduced lung function, the effect of additional surfactant treatment is still controversial. It is possible that surfactant becomes inactivated during mechanical ventilation.1,2 Calculating end diastolic and left ventricular volume gives information that ejection fraction of the left ventricle is reduced measuring arterial pulmonary ow at the same time. Therefore, it may be helpful in these cases to keep the ductus arteriosus open by administration of prostaglandins. Another strategy is lowering pulmonary vascu-
Figure 2 Distribution of muscular bers in the wall of pulmonary vessels normally and in CDH. (Color version of gure is available online.)
246 lar resistance by using vasoactive drugs like nitric oxide, sildenale, and milrinone. Because of transposition of liver, spleen and gut into thorax early in pregnancy, the abdominal cavity will not will grow as much. Thus, after surgical closure of the diaphragm, it may be difcult to reduce all organs inside the abdominal cavity without pressure on the vena cava and diaphragm, and to affect the mesenteric blood ow. Early diaphragmatic defect goes along with nonrotation and nonxation of mesentery. In a nonrotated position of the gut, the duodenal passage may be blocked due to kinking. This may not allow early regular feeding regime after closure of diaphragm. Similar to late closure of dorsal diaphragmatic area, the dorsal rim of musculature is very weak and may be hidden. In larger defects, it may be not be present at all.
Seminars in Pediatric Surgery, Vol 17, No 4, November 2008
Incidence
The incidence is 1:2500-3000 per live births. These gures may be inaccurate, because of the unknown factor of the hidden mortality in this malformation. Hidden mortality in this respect means that only 40 of 100 fetuses with prenatal diagnosis will survive. In other words, there must be a high mortality in utero. Even in advanced neonatal intensive care, the survival rate remained at around 50% for decades. The normal size of a growing lung is shown in Figure 4 as well as the lung volume of those patients who did not survive.3 It should be realized that today the prognosis is more and more related to associated malformations, which are found in 40%.
Figure 4 Fetal lung volume versus gestational age, and dead patients due to CDH and controls.
Symptoms after birth
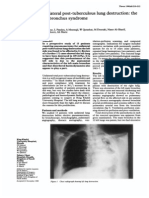
The size of the diaphragmatic defect and the timing of transposition of intraabdominal structures intrathoracically is an important factor in early presentation with symptoms after birth. The abdomen seems to be empty and could even be scaphoid. A newborn in respiratory distress is usually treated with oxygen and ventilation primarily using a mask. Typically, this measure leads to deterioration of oxygenation by inating the stomach and the gut, leading to more compression of the lung and to increasing mediastinal shift. Risk of producing pneumothorax is high. In any case of sudden deterioration, a pneumothorax should be suspected. Small or slit-like defects of the diaphragm may not be apparent at birth, as long as there is no herniated gut. After weeks or months often during coughing elevated intraabdominal pressure forces the gut through the defect, accompanied by pain and problems of passage. In these situations, mediastinal shifts are hardly ever found. In the x-ray, a round, air-lled structure possibly with uid may be seen. The differential diagnosis from a lung cyst can be difcult. Contrast studies may help.
Diagnosis
High-quality ultrasound (prenatal magnetic resonance even more) can demonstrate congenital diaphragmatic hernia (CDH) early in pregnancy. In ultrasound, identication of liver or lung tissue may be difcult or unclear, especially in cases of maternal obesity. It is of prognostic importance to know whether left liver lobe is lying intrathoracically or not. In right-sided CDH, the exact position of the gall bladder may show liver site in ultrasound. Prenatal lung head ratio (LHR) as an important factor of prognosis is widely accepted. Whenever this ratio is less than
Figure 5 position.
Fetal MRI demonstrating normal lung volume and
Waag et al.
Congenital Diaphragmatic Hernia
247 presence of stomach and left liver above the diaphragm. Statistically, 93% of the affected newborns are surviving whenever liver is down. If left liver lobe is up, the survival declines to 43%.4 LHR in accordance to age is well dened. At 28th WG, this LHR 1.2 0.38 means borderline to high-risk group. In MRI, lung volume of the affected side should not be less than 10 ml.5 LHR in 34th WG is 1.8-3.0 normally. Patients who do not need ECMO and have liver down show an LHR of more than 1.5 (Figure 8).
LHR and lung volume measurements (34th WG)
Figure 6 Fetal MRI in a CDH patient showing the small left lung and the small gut in the left thorax. (Color version of gure is available online.)
1.2 at 28 weeks of gestation (WG) in ultrasound, MRI is more accurate (Figures 5-7). After the 20th WG, it shows accurate measurements of lung volume, giving time to plan a delivery in a tertiary referral center with extracorporeal membrane oxygenation (ECMO) possibilities, whenever in doubt.
Prenatal prognostic factors
High-risk group As mentioned before, diagnosis of CDH before 25th WG means a large defect and a worse prognosis is related to the
According to literature, mortality is believed to be the same whether CDH is right- or left-sided, but some authors see more mortality in right-sided defects.6 Measuring fetal hemodynamics and reaction to oxygen support to the mother by inuencing fetal pulmonary lung perfusion may become a prognostic factor. Dextroposition of fetal heart is found often at the same time as left liver lobe up. In these patients, ductus venosus joins the right atrium atypically leading to volume load of pulmonary artery and to insufcient lling of the left heart. Left ventricle stays too small consecutively with low-ejection fraction. So, in respect to prognosis, small left ventricle and relationship of aorta to pulmonary artery are valuable. Low birth weight, polyhydramnios, or hydrops are further discussed as bad factors for prognosis, but the presence of other associated malformations reduced survival rates.4,6-8
Figure 7
Lung volume calculation by planimetry.
248
Seminars in Pediatric Surgery, Vol 17, No 4, November 2008 gut in 3 patients were found as well as polycystic kidney and hydronephrosis.9
Fetal surgery
Harrison and Soper have been the pioneers in developing techniques for fetal correction and conservation of pregnancy despite surgery. Tocolysis at the end was the outstanding problem.10-12 Experimentally, occlusion of trachea in fetal lambs blocked outow of pulmonary secretion, which is produced inside the lung. This accumulation of secretion leads to expansion of the lung. But it is mainly not a structural growth of the number of acini.13,14 Tracheal occlusion is done between 26th and 28th WG and increases LHR from 0.7 to 1.8. Duration of the plug should be 6 weeks in the opinion of the Eurofetus group. This success may be diminished again when occlusion is terminated 2 weeks before delivery. Plugging trachea by a balloon endoscopically is of clinical relevance. Deprest is one of the very few who has experiences in 20 fetuses in positioning the balloon endoscopically through mothers abdominal wall and uterus via fetal mouth into the fetal trachea (fetoscopic endoluminal tracheal occlusion, FETO).10,11,15 After sufcient pulmonary growth, the intratracheal balloon can be unblocked via some route (Figure 10). Timing and duration of this procedure is still under discussion. Taking the balloon out at the time of delivery is called ex utero intrapartum (EXIT) procedure. Further experiences have to be collected before evaluating whether patients with LHR or lung volumes of high-risk group will prot from this highly sophisticated treatment.11
Figure 8 Correspondence of liver up and liver down to the necessity of ECMO therapy and the need of patch in CDH patients.
In born patients suffering from CDH show better outcome than out born. Logistic advantages are obvious. Transport of the baby in utero is much safer as well as delivery in a tertiary center providing ECMO. Prenatal referral is advised in all features showing LHR below 1.4. LHR below 1.2 makes ECMO necessity very likely, so does a lung volume below 25 ml in MRI. Our own results proved that all newborns with lung volumes of 31.8 ml in average did not need ECMO. Highrisk group depending on ECMO showed LHR of 0.92, ie, 10.38 ml lung volume. Proper evaluation of prognostic factors will reect results (Figure 9). Our survival rate overall is 86.5% of all newborns admitted; 71% of all patients needing ECMO survived in our series.
Postnatal diagnosis
There are no breath sounds over the affected thorax, but bowel sounds may be heard instead. Because of mediastinal shift, the apex of the heart is displaced. A plain x-ray makes the diagnosis of CDH as well as indicating whether the stomach and other organs are lying in the chest. A nasogastric tube shows mediastinal shift and denes the position of stomach. Compression of contralateral lung is demonstrable. CDH is associated with cardiac malformations in 30-40%, mainly arterial and ventricular septum defects and pulmonary stenosis. Cerebral alterations are mostly found in patients with chromosomal aberrations, like in syndromes such as Pallister Kilian, BeckwithWiedemann, and DenysDrash. Nonrotation induces duodenal kinks, and relevant clinical signs are realized in 20-30%. Small hiatus muscles in big defects explain gastroesophageal reux. Additional malformations can be described in our series of 177 left-sided defects: lung sequestration of the 5 patients, accessory spleen in 5, and duplication of
Therapy algorithm
For prenatal planning, estimation of lung volume at the 34th WG is important. Whenever lung volume is more than 20 ml and no factor of bad prognosis like liver up is present, spontaneous delivery should be the mode of treatment.
Figure 9 Signicance is shown between lung volumes in MRI needing ECMO or not and as well borderline volumes for survival.
Waag et al.
Congenital Diaphragmatic Hernia
249
Figure 10
Endoscopic pictures of the obstructing balloon inside the fetal trachea. (Color version of gure is available online.)
But if the lung volume is below 20 ml and an additional bad factor is present, follow-up should be given to a tertiary center, expecting cesarean section in the 37th WG followed by advanced treatment, including providing ECMO therapy (Figure 11). In uncomplicated cases after 38th WG spontaneous delivery (Figure 12), the following therapy treatment is suggested: 1. 2. 3. 4. 5. Primary intubation Conventional gentle ventilation NO inhalation if PaO2 80 mm Hg postductal HFOV if PaCO2 75 mm Hg ECMO if PaO2 50 mm Hg preductal, PaO2 40 mm Hg postductal
6. Surgery for defect closure after stabilization 7. Surgery for defect closure after ECMO In uncomplicated cases, there are no objections against spontaneous delivery. Direct intubation avoids additional lling of gut with air, increasing mediastinal shift and lung compression. Surfactant application seems to have an effect only in preterms. Ventilation pressures above 25 cm H2O as well as positive endexspiratoric pressure (PEEP) over 3-5 cm H2O induce damage to lung structure. Ventilation frequencies of 80/min and inspiration/expiration ratio of 1:2 without auto-PEEP should be sufcient. These are the rules of what is called gentle ventilation.1,9,14-16 Whenever this ventilation is not sufcient, high-frequency ventilation (HFOV) is the next step. Hypercapnia
Figure 11 Algorithm of CDH diagnosis and prenatal planning in Mannheim.
Figure 12
Algorithm of CDH therapy postnatally in Mannheim.
250 can be tolerated up to PaCO2 of 70 mm Hg and respiratory acidosis until a pH of 7.2. So far, there is no evidence for any therapy for lung maturation later than 34th WG. NO inhalation (10 ppm) is applied whenever PaO2 falls postductally below 80 mm Hg. But there is no evidencebased effect for NO in literature.9 Pre- and postductal oxygenation and arterial pressure have to be monitored continuously by umbilical arterial catheter placement. However, umbilical veins are not suitable, because the tip may easily be positioned in the hepatic veins or ductus venosus. Drug administration, like catecholamine, may produce liver cell necrosis. The most efcient catecholamine is suprarenin (dose up to maximally 0.2 g/kg/min), not increasing resistance of pulmonary vessels. For continuous analog sedation, fentanyl (2-3 g/kg/h) and midazolam (0.05 g/kg/h) reduce oxygen consumption. Relaxation of musculature (vecuronium 0.05 mg/kg/h) may inuence resistance of pulmonary vessels during days 1-3. When patients reach PaO2 above 80 mm Hg and reduced ow on the ductus arteriosus, they can be kept on this regime until normo-capnia is reached; 24-48 hours later, surgery can be started. The honeymoon period is dened as the time after birth when the newborn seems to be in a good status primarily before (may be after or around 12 hours) oxygenation and circulation is breaking down. An explanation for this is very likely exhausting pumping force of left ventricle,16 which is too small and not developed sufciently.
Seminars in Pediatric Surgery, Vol 17, No 4, November 2008
Figure 14 ECMO in action on ICU. (Color version of gure is available online.)
PaO2 postductally 40 mm Hg over 2 hours PaO2 preductally 50 mm Hg over 2-4 hours PaO2 postductally 50 mm Hg over 12 hours PaCO2 70 mm HG under HFOV Indication for ECMO in our opinion is not only a question of survival but also quality of life because of secondary damage. Preductal PaO2 should always be above 50 mm Hg and exceed at least 10 mm Hg postductal values. Differences of pre- and postductal gures allow an estimate of blood ow through the ductus. Whenever both values of pre- and postductal PaCO2 are not approaching a minimum of 5 mm Hg, there is likely a need for ECMO. If PaCO2 is increasing above 70 mm Hg despite HFOV, there is no other chance than ECMO. Persistent PaCO2 of more than 100 mg Hg or PaO2 less than 40 mm Hg does not allow survival even on ECMO.
ECMO indication
It is still under debate whether ECMO is the last option in critical cases. There is no evidence-based study with comparable conditions. Indication for the need of ECMO nowadays after 15 years of experience in our institution and after more than 240 patients on ECMO for CDH is dened as follows:
Risks under ECMO
Newborns younger than 34th WG or under 1800 g body weight show signicant problems getting cannulas big enough for sufcient ow. V. cava, V. saphena, V. femoralis, and the carotid artery may rupture and bleed. Further risks, seen in our institution are: blood clots and air bubbles induce embolization or infarctions of lung or brain. Heparin in ECMO machines is still necessary but is also the reason for cerebral bleed (9%) or bleeding into lung tissue (14%). Convulsions are registered in 16%. Even after reconstruction, the carotid artery may thrombose later. Catheter-related local bleeding 7.5% Intracerebral bleeding 9% Intrapulmonary bleeding 14% Convulsions 16%
Figure 13 Principle of ECMO in details. (Color version of gure is available online.)
Waag et al.
Congenital Diaphragmatic Hernia
251
Operative steps of closure
A longitudinal midline laparotomy is the best approach for sufcient exposure of the diaphragmatic defect. A dorsal muscular rim may be hidden primarily, but often can be found except in large defects (Figure 16). Primary closure needs incising rims for better healing. Nonabsorbable sutures 3 to 0 or 4 to 0 are used. Whenever primary closure of the diaphragm is performed under tension, the intrathoracic space is enlarged and less volume exists intraabdominally as seen often on postop radiograph (Figure 17, left in comparison to right side). This is the opposite of what is needed; ie, tension on the diaphragm increases as a result of raised intraabdominal pressure. This is caused by a small peritoneal cavity trying to accommodate all the abdominal viscera, which was occupying space in the chest. Early patching is better than primary closure under tension, and cone-forming gives more intraabdominal space than a at patch (Figure 18). Fixating patch near aorta and hiatus is fragile in big defects prone to recurrent hernia. Therefore, the patch should be bigger than the defect and is xed with mattress sutures (Figure 19). Our learning curve showed that problems of duodenal kinking are not rare (16%). Whenever this is realized, duodenum is dissected free and may be splinted by a gastric tube fed through. Analog in respect to likelihood of gastroesophageal reux (20%), it is discussed to perform in big defects a fundo-esophagopexy as a Thal procedure, for example, prophylactically.9,17-20 Most experts of CDH are no longer using drainage of pleura. In a big defect with a big volume to be brought to the abdomen, it is necessary to stretch the abdominal wall or even to patch abdominal incision for adequate closure. Too much intraabdominal pressure extends the diaphragm and compresses venous backow through vena cava to the heart.
Figure 15 Plain x-ray of the thorax demonstrating the thick venous canula in the v. cava superior, massively diverted by the mediastinal shift.
ECMO technique (Figure 13)
ECMO machine is prelled with blood and connected to cannulas implanted into the carotid artery and through internal jugular and superior vena cava just in front of the right atrium. Veno-venous technique by double lumen catheter is abandoned because oxygen supply is not sufcient in CDH patients and a good functioning right ventricle is necessary. Heparinization is controlled as well as the number of thrombocytes, which should be above 80000-100000 l. Because of reduced ventilation and activation of cytokines, lung will white out in x-ray. Capillary leak and general edema are usual, needing additional volume and diuretics. Normally after 3 days, recreation starts (Figure 14). As soon as blood ow on ECMO can be reduced to 20% of patients cardiac output and oxygen saturation on venous side (SvO2) is falling below 70% for 24 hours (called idling phase), ECMO can be terminated. ECMO results came up to survival rates of around 70% in recent years.9,17
Technique of ECMO cannulation
The right carotid artery is dissected as well as internal jugular vein, taking care of vagal nerve and ansa cervicalis. Skin incision is vertical along anterior sternocleido muscle, to have better access for reconstruction of vessels after ECMO. Dilation of vessel is precarious but necessary from time to time to implant cannulas as big as possible (10-12 Ch for the vein and 8-10 for the carotid artery). The tip of the venous cannula has to be placed at right atrium and arterial cannula should join aorta controlled by x-ray to provide sufcient ow. It has to be taken into account that turning the head back postoperatively, tips will be pushed forward additionally (Figure 15).
Figure 16 This diaphragmatic defect shows a good anterior diaphragmatic muscle and hiatus muscle and a small dorsal diaphragmatic rim; the lung is fully ventilated but hypoplastic. (Color version of gure is available online.)
You might also like
- What Is A Diaphragmatic Hernia?Document55 pagesWhat Is A Diaphragmatic Hernia?Shikha AcharyaNo ratings yet
- Pediatrics StridorDocument13 pagesPediatrics StridorEmaNo ratings yet
- Diaphragmatic HerniaDocument8 pagesDiaphragmatic HerniaAnonymous 9xHTwHYNo ratings yet
- Pediatric Surgery 2 (Respiratory and Gastrointestinal Conditions) PDFDocument12 pagesPediatric Surgery 2 (Respiratory and Gastrointestinal Conditions) PDFRenatoCosmeGalvanJunior100% (1)
- Disaster Readiness Risk Reduction: Quarter 2-Module 13: DRR-related Laws and PoliciesDocument16 pagesDisaster Readiness Risk Reduction: Quarter 2-Module 13: DRR-related Laws and PoliciesUel Cabz LaquihonNo ratings yet
- Accupressure Points Chart PDFDocument20 pagesAccupressure Points Chart PDFshule1100% (2)
- Difficult Airway in Obstetric AnesthesiaDocument3 pagesDifficult Airway in Obstetric AnesthesiaRoman AureliaNo ratings yet
- Cultural Landscape An Introduction To Human Geography 11th Edition Rubenstein Solutions ManualDocument16 pagesCultural Landscape An Introduction To Human Geography 11th Edition Rubenstein Solutions Manualheathergarciafbqedgosyp100% (13)
- Pediatric Radiology ShortDocument95 pagesPediatric Radiology ShortNelly ChinelliNo ratings yet
- DR Varsha Atul Shah Senior Consultant Dept of Neonatal and Devt Medicine, SGH Visiting Consultant Dept of Child Devt, KKHDocument47 pagesDR Varsha Atul Shah Senior Consultant Dept of Neonatal and Devt Medicine, SGH Visiting Consultant Dept of Child Devt, KKHJennifer MrjNo ratings yet
- 2022 India Accessibility Standards and Guidelines For Civil Aviation - EnglishDocument110 pages2022 India Accessibility Standards and Guidelines For Civil Aviation - EnglishDisability Rights AllianceNo ratings yet
- Patrick Callaghan, Helen Waldock-Emergencies in Mental Health Nursing-Oxford University Press (2013)Document195 pagesPatrick Callaghan, Helen Waldock-Emergencies in Mental Health Nursing-Oxford University Press (2013)VidákZsigmond100% (2)
- Pleural EffusionDocument10 pagesPleural EffusionShane PangilinanNo ratings yet
- Congenital Anomalies of Airway and Lung ParenchymaDocument71 pagesCongenital Anomalies of Airway and Lung ParenchymaGopal ChawlaNo ratings yet
- Export of SpicesDocument57 pagesExport of SpicesJunaid MultaniNo ratings yet
- Vstep Tests B1 B2 C1 Full KeyDocument162 pagesVstep Tests B1 B2 C1 Full KeyLe Hoang LinhNo ratings yet
- CDH Modern MX PDFDocument12 pagesCDH Modern MX PDFThia SanjayaNo ratings yet
- Paediatric AnsDocument142 pagesPaediatric AnsAbdulkadir HasanNo ratings yet
- Hernia DiafragmaDocument7 pagesHernia Diafragmasentaro2100% (1)
- Comparison of Transverse and Vertical Skin Incision ForDocument6 pagesComparison of Transverse and Vertical Skin Incision ForHerry SasukeNo ratings yet
- Diaphragmatic HerniaDocument42 pagesDiaphragmatic Herniahayssam rashwan50% (2)
- CDH ReviewDocument12 pagesCDH ReviewDene DeneNo ratings yet
- Diaphragmatic HerniaDocument9 pagesDiaphragmatic HerniaFatimaNo ratings yet
- Congenital Diaphragmatic Hernia: Pathogenesis, Prenatal Diagnosis and Management - Literature ReviewDocument7 pagesCongenital Diaphragmatic Hernia: Pathogenesis, Prenatal Diagnosis and Management - Literature ReviewPritariantiNo ratings yet
- Management of Neonates With Oesophageal Atresia and TR - 2022 - Early Human DeveDocument6 pagesManagement of Neonates With Oesophageal Atresia and TR - 2022 - Early Human DeveJUAN HIMMEL ESPINOZA ANDIANo ratings yet
- Sabitson - Appendiks EngDocument17 pagesSabitson - Appendiks Engzeek powerNo ratings yet
- Ped CXRDocument17 pagesPed CXRSupitcha ThongchaiNo ratings yet
- Congenital Diaphragmatic HerniaDocument2 pagesCongenital Diaphragmatic HerniaHisham100% (1)
- Airway AnomaliesDocument11 pagesAirway AnomaliesDariki CampbellNo ratings yet
- Neonatal Tracheostomy - JonathanWalsh 2018Document12 pagesNeonatal Tracheostomy - JonathanWalsh 2018Ismael Erazo AstudilloNo ratings yet
- Congenital Eventration of The Diaphragm+++Document13 pagesCongenital Eventration of The Diaphragm+++TommyNo ratings yet
- Acute Gyna 2Document9 pagesAcute Gyna 2zoya virjiNo ratings yet
- Congenital Diaphragmatic HerniasDocument20 pagesCongenital Diaphragmatic HerniasRahma Tya AnwarNo ratings yet
- Congenital Diaphragmatic HerniaDocument4 pagesCongenital Diaphragmatic HerniaJulio AltamiranoNo ratings yet
- Diaphragmatic HerniaDocument5 pagesDiaphragmatic HerniaRamesh Martha100% (1)
- Surgical Techniques: Plication of The DiaphragmDocument14 pagesSurgical Techniques: Plication of The DiaphragmFranciscoJ.ReynaSepúlvedaNo ratings yet
- Jurnal THTDocument46 pagesJurnal THTShida ZakariaNo ratings yet
- Acquired Diaphragmatic HerniaDocument8 pagesAcquired Diaphragmatic HerniaAmirul Zakiya BraveryNo ratings yet
- Anesthetic Management of An Undiagnosed Advanced Extrauterine Pregnancy Under Combined Spinal-Epidural AnesthesiaDocument4 pagesAnesthetic Management of An Undiagnosed Advanced Extrauterine Pregnancy Under Combined Spinal-Epidural AnesthesiaHanayuki VizureiNo ratings yet
- Diaphragm: Surgical Anatomy of The DiaphragmDocument14 pagesDiaphragm: Surgical Anatomy of The DiaphragmOlga CerlatNo ratings yet
- Management of Congenital Lung Malformations 2022 Clinic PerinatolDocument20 pagesManagement of Congenital Lung Malformations 2022 Clinic PerinatolAna Maria Fidelis Silva camposNo ratings yet
- 1 s2.0 S0039610903001191 MainDocument15 pages1 s2.0 S0039610903001191 MainJuan Jos� Beltr�n Hern�ndezNo ratings yet
- Doppler en ObstetriciaDocument8 pagesDoppler en Obstetriciapopman41No ratings yet
- Fetoscopic Endoluminal Tracheal Occlusion and ReesDocument9 pagesFetoscopic Endoluminal Tracheal Occlusion and ReesnNo ratings yet
- Anesthesia For Foetal Surgery: Dr. Athira S MadhuDocument98 pagesAnesthesia For Foetal Surgery: Dr. Athira S MadhuAthira S MadhuNo ratings yet
- Vaginal Extrusion of A Ventriculoperitoneal Shunt A Case Report and Review ofDocument10 pagesVaginal Extrusion of A Ventriculoperitoneal Shunt A Case Report and Review ofDian AdiNo ratings yet
- 1 PBDocument9 pages1 PBMariiaNo ratings yet
- 9 Anaesthetic Considerations For Laparoscopic Surgery in Neonates and Infants: A Practical ReviewDocument13 pages9 Anaesthetic Considerations For Laparoscopic Surgery in Neonates and Infants: A Practical Reviewdiomer123No ratings yet
- Herberg 2014Document8 pagesHerberg 2014ANA HERNÁNDEZNo ratings yet
- Ectopic Pregnancy 2022 Edited 3Document40 pagesEctopic Pregnancy 2022 Edited 3apule geraldhumbleNo ratings yet
- MRI Findings in Fetuses With An Abdominal Wall Defect: Gastroschisis, Omphalocele, and Cloacal ExstrophyDocument7 pagesMRI Findings in Fetuses With An Abdominal Wall Defect: Gastroschisis, Omphalocele, and Cloacal ExstrophyIngrid TanasaNo ratings yet
- Tuberculosis of The Chest Wall With Massive Tuberculous Pleural EffusionDocument3 pagesTuberculosis of The Chest Wall With Massive Tuberculous Pleural EffusionwulanNo ratings yet
- BautistajournDocument3 pagesBautistajournbomcorNo ratings yet
- Ectopic PregenancyDocument69 pagesEctopic PregenancyMahmoud AbbasNo ratings yet
- Cervicval Shortening / Cervical Insufficiency: EtiologyDocument3 pagesCervicval Shortening / Cervical Insufficiency: EtiologyMiska RaihanaNo ratings yet
- Topics For Oral Exam Thypoid FeverDrownTEFDocument2 pagesTopics For Oral Exam Thypoid FeverDrownTEFPCRMNo ratings yet
- 3rd Trimester Bleeding and Postpartum HemorrhageDocument100 pages3rd Trimester Bleeding and Postpartum Hemorrhagepeanutbutter ohNo ratings yet
- Trapped Lung - StatPearls - NCBI BookshelfDocument7 pagesTrapped Lung - StatPearls - NCBI BookshelfVinna KusumawatiNo ratings yet
- Congenital Diaphragmatic HerniaDocument3 pagesCongenital Diaphragmatic HerniaMahmoud SalmanNo ratings yet
- Congenital Diaphragmatic Hernia: Pediatric Surgery DepartmentDocument32 pagesCongenital Diaphragmatic Hernia: Pediatric Surgery DepartmentTuan Ahamed CassimNo ratings yet
- Kayatsha - Gastroschisis and Omphalocele A Case ReportDocument4 pagesKayatsha - Gastroschisis and Omphalocele A Case ReportAffannul HakimNo ratings yet
- Respiratory Distress in The Neonate and InfantDocument8 pagesRespiratory Distress in The Neonate and InfantMikey ZhitnitskyNo ratings yet
- Congenital AnomaliesDocument22 pagesCongenital Anomaliesjessy100% (1)
- Journal of Pediatric Surgery CASE REPORTSDocument4 pagesJournal of Pediatric Surgery CASE REPORTSwidyaNo ratings yet
- Research Paper On PneumothoraxDocument7 pagesResearch Paper On Pneumothoraxgz8xbnex100% (1)
- Antepartum HemorrhageDocument12 pagesAntepartum HemorrhageMohammed AbdNo ratings yet
- Diseases of the Liver and Biliary TreeFrom EverandDiseases of the Liver and Biliary TreeAnnarosa FloreaniNo ratings yet
- Protocol 1 Hypoglycemia 2006Document7 pagesProtocol 1 Hypoglycemia 2006Aprilian Ayu SitaNo ratings yet
- Diagnosis of Tuberculosis in Children: Increased Need For Better MethodsDocument9 pagesDiagnosis of Tuberculosis in Children: Increased Need For Better MethodsphobicmdNo ratings yet
- Pneumococcal Conjugate Vaccine (PCV) Catch-Up Guidance For Children 4 Months Through 18 Years of Age 2015Document3 pagesPneumococcal Conjugate Vaccine (PCV) Catch-Up Guidance For Children 4 Months Through 18 Years of Age 2015phobicmdNo ratings yet
- Paediatric Empyema: A Case Report and Literature ReviewDocument5 pagesPaediatric Empyema: A Case Report and Literature ReviewphobicmdNo ratings yet
- 1B Draft Annce-Wshop 020113.amendedDocument1 page1B Draft Annce-Wshop 020113.amendedphobicmdNo ratings yet
- Wet CoughDocument2 pagesWet CoughphobicmdNo ratings yet
- 1A Draft Annce-CME Course 020113.amendedDocument1 page1A Draft Annce-CME Course 020113.amendedphobicmdNo ratings yet
- Pediatrics 2013 Andrews S36Document3 pagesPediatrics 2013 Andrews S36phobicmdNo ratings yet
- AsthmaDocument17 pagesAsthmaphobicmdNo ratings yet
- The Difficult Coughing Child: Prolonged Acute Cough in ChildrenDocument5 pagesThe Difficult Coughing Child: Prolonged Acute Cough in ChildrenphobicmdNo ratings yet
- Left Bronchus SyndromeDocument3 pagesLeft Bronchus SyndromephobicmdNo ratings yet
- Empyema 2Document9 pagesEmpyema 2phobicmdNo ratings yet
- Diagnostic Assessment of Patients With Interstitial Lung DiseaseDocument8 pagesDiagnostic Assessment of Patients With Interstitial Lung DiseasephobicmdNo ratings yet
- Pediatrics 2013 Iwamoto E817 24Document10 pagesPediatrics 2013 Iwamoto E817 24phobicmdNo ratings yet
- Pediatrics 2013 Bivins S47Document3 pagesPediatrics 2013 Bivins S47phobicmdNo ratings yet
- Pediatrics 2013 E1089 104Document18 pagesPediatrics 2013 E1089 104phobicmdNo ratings yet
- Pediatrics 2013 Davis S5Document3 pagesPediatrics 2013 Davis S5phobicmdNo ratings yet
- Pi Is 0954611105000491Document5 pagesPi Is 0954611105000491phobicmdNo ratings yet
- CP Guideline Ats ILDDocument19 pagesCP Guideline Ats ILDphobicmdNo ratings yet
- CV - Mahbub MishuDocument3 pagesCV - Mahbub MishuMahbub Chowdhury MishuNo ratings yet
- Coca Cola Fairlife CaseDocument4 pagesCoca Cola Fairlife Caseapi-315994561No ratings yet
- Climbing Training Log - TemplateDocument19 pagesClimbing Training Log - TemplateKam Iqar ZeNo ratings yet
- Lecture Notes:: Accident and Incident InvestigationDocument10 pagesLecture Notes:: Accident and Incident InvestigationajayikayodeNo ratings yet
- NPD Phase 1Document2 pagesNPD Phase 1Abdullah ZahidNo ratings yet
- Jurnal Asli PBL 3 Blok 9Document6 pagesJurnal Asli PBL 3 Blok 9Annisa FadilasariNo ratings yet
- Enucleation Surgery-Orbital Implants and Surgical Techniques - 1Document3 pagesEnucleation Surgery-Orbital Implants and Surgical Techniques - 1Satria Adi MarhendraNo ratings yet
- 5.3.1 Distinguish Between Learning and Performance: Skill in SportDocument48 pages5.3.1 Distinguish Between Learning and Performance: Skill in SportAiham AltayehNo ratings yet
- Form 1 ADocument2 pagesForm 1 ARohit Jain100% (2)
- Health Information On The Internet: The Case of GreeceDocument12 pagesHealth Information On The Internet: The Case of GreecemaryNo ratings yet
- Ufgs 01 57 19.01 20Document63 pagesUfgs 01 57 19.01 20jackcan501No ratings yet
- Jeehp 12 06Document4 pagesJeehp 12 06Sohini KhushiNo ratings yet
- Objectives of The Nairobi SummitDocument12 pagesObjectives of The Nairobi SummitJoachim ChijideNo ratings yet
- Clinico-Pathological Conference: Presented by The Department of Internal MedicineDocument3 pagesClinico-Pathological Conference: Presented by The Department of Internal MedicineCloudy ClaudNo ratings yet
- Recist Criteria - Respon Solid Tumor Pada TerapiDocument18 pagesRecist Criteria - Respon Solid Tumor Pada TerapiBhayu Dharma SuryanaNo ratings yet
- Q3-Las-Health10-Module 3-Weeks 6-8Document6 pagesQ3-Las-Health10-Module 3-Weeks 6-8MA TEODORA CABEZADANo ratings yet
- Diastasis Recti Ebook DownloadDocument19 pagesDiastasis Recti Ebook DownloadMertcan DamatNo ratings yet
- Scholarship Application Motivation Letter ExampleDocument2 pagesScholarship Application Motivation Letter ExampleColoNo ratings yet
- LPV Fault Detection of Glucose-Insulin System: Cite This PaperDocument6 pagesLPV Fault Detection of Glucose-Insulin System: Cite This PaperfatihaNo ratings yet
- Steps To Reduce Drug Abuse 1800 11 0031 National Toll Free Drug de Addiction Helpline NumberDocument4 pagesSteps To Reduce Drug Abuse 1800 11 0031 National Toll Free Drug de Addiction Helpline NumberimranNo ratings yet
- Poe Edgar Allan The Premature BurialDocument10 pagesPoe Edgar Allan The Premature BurialUntold TearNo ratings yet
- Name: Reymark Mutia Narrative Reporting (Doctool) - Edong Permites Chapter - 1 To Start, Type in The Local Server Url Inside The BrowserDocument65 pagesName: Reymark Mutia Narrative Reporting (Doctool) - Edong Permites Chapter - 1 To Start, Type in The Local Server Url Inside The BrowserReymark MutiaNo ratings yet
- Starlight ProgramsDocument12 pagesStarlight Programsllacara@nncogannett.comNo ratings yet