Professional Documents
Culture Documents
Cardio Ms Hand Out
Uploaded by
Victor ShonOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Cardio Ms Hand Out
Uploaded by
Victor ShonCopyright:
Available Formats
CARDIOVASCULAR SYSTEM CONDITIONS CORONARY ARTERY DISEASES Non Modifiable Risk Factors Age Gender Family History Modifiable
ble Risk Factors Smoking Hypertension Obesity Elevated ________________ Stress Angina Pectoris Pain in the chest from coronary insufficiency, in the absence of myocardial infarction Signs and symptoms: Pain Pallor Diaphoresis Faintness Palpitations Collaborative Management Medications: ________________ (drug of choice) Anticipate postural hypotension Take maximum of 3 doses at 5 min interval SL prep has burning or stinging sensation SL route has onset of 1-2 min, duration of 30 min Sips of H2O improves absorption SL Avoid ________________ Advise client to carry 3 tabs in his pocket Store nitroglycerine in a cool, dry, dark place; replace stock q 6 months Observe for side effects Nitropatch applied OD in AM, rotating sites Evaluate effectiveness B-adrenergic blocking agents propanolol, metoprolol, etc Ca-channel blocker verapamil, nifedipine, diltiazem Platelet-aggregating inhibitors ASA, dypiridamole, ticlopidine Anticoagulants heparin Na, Warfarin Na (Coumadin), dicumarol
Types: ________________ Predictable pattern 4 Es Relieved by rest ________________ ("pre-infarction", "crescendo", "acute coronary insufficiency") Attacks accelerate in frequency intensity and duration Relieved by NTG Leads to MI ________________ ("variant") is primarily attributable to vasospasm
Surgeries: Percutaneous Transluminal Coronary Angioplasty (PTCA) Compresses the plaque by using balloon tipped catheter under fluoroscopic guidance.
Page 1 of 10
Lecture Aid: Medical-Surgical Nursing
Ideal in ________________ vessel coronary artery disease Intravascular Stenting - done to prevent restenosis after PTCA
Coronary Artery Bypass Graft (CABG) Reduce angina and improve activity tolerance Recommended for ________________ or multivessel involvement Main purpose is myocardial revascularization Common source of graft are saphenous vein and internal mammary artery
Nursing Interventions Administer, as ordered: o Oxygen o Nitroglycerin Rest Diet o Low fat, low Na, low cholesterol diet o Avoid saturated fats o Read food labels Activity restriction within patients limitation Myocardial Infarction ischemic myocardial cell necrosis Caused by coronary artery obstruction due to: o progressive development of atherosclerosis o coronary artery spasm o embolism Occlusion leads to ________________ glycolysis
Page 2 of 10
Lecture Aid: Medical-Surgical Nursing
Manifestations Dsypnea Changes in heart area Nausea and vomiting Increased WBC and ESR Diagnostic Studies Enzymes: _______________ elevates in 30 minutes _______________ elevates in 2 to 4 hours AST peaks in 24 to 36 hours LDH peaks in 48 to 72 hours.
o Oxygen o IVF to run KVO CBR Monitor: o vital signs every ________________ hours. o cardiac rhythm for dsyrhythmias o signs of congestive heart failure
ECG changes: o ST elevation = myocardial injury o ST depression = ischemia o T wave inversion = myocardial ischemia o large Q waves = necrosis
CONGESTIVE HEART FAILURE Is the inability of the heart to maintain an adequate output of blood from one or more ventricles resulting to an inadequate supply of blood to the vital parts of the body.
Collaborative Management: "O BATMAN!": ________________ Beta blocker ASA ________________ Morphine ACE Nitroglycerin Nursing Interventions Administer, as ordered: o Morphine sulfate
Lecture Aid: Medical-Surgical Nursing
Types: Left-sided CHF: usually pulmonary by nature Right-sided CHF: CHF: affects the periphery in general Pathway of Blood Oxygenation In The Heart
Page 3 of 10
Peripheral edema Ascites Rapid weight gain (fluid retention) Anorexia, N/V Lightheadedness, dizzy spells or fainting spells Difficulty concentrating or decreased alertness Irregular or rapid heartbeat
Diagnostic Procedures Chest X-ray ECG Echocardiogram Coronary Catheterization Blood Test
Causes Coronary Artery Disease Faulty Heart Valves Cardiomyopathy Congenital Heart Defects Heart Arrythmias Kidney Failure Hypertension (or related increase in BV) Signs and Symptoms Fatigue and weakness DOE Persistent wheezing or cough with white or pink blood-tinged phlegm Pronounced neck veins
Management DIGITALIS THERAPY The major therapy for CHF (+)________________, (-)________________ effects Nsg. Implication: check for HR below 60 and above 120 Monitor serum potassium (Normal 3.5-5.5 mEq/L) Examples: Lanoxin (Digoxin), Crystodigin (Digitoxin), Lanatoside (Cedilanid C), Deslanoside (Cedilanid D) Beware of Digitalis Toxicity!!! G.I. Manifestations: Anorexia, N & V
Lecture Aid: Medical-Surgical Nursing
Page 4 of 10
Bradycardia ________________ (most dangerous) Yellow / green visions; halos around the light (elderly) In males: gynecomastia, decreased libido and impotence
Captopril (an antihypertensive agent with vasodilator effect)
DIURETIC THERAPY To decrease cardiac workload by ________________circulating BV Nsg. Implications: o Assess for s/sx of hypokalemia when giving thiazides and loop diuretics o Give potassium supplements Best given early AM or early PM If thiazides are ineffective, a potassium sparing diuretic may be given. Examples of Diuretics: Thiazides o Chlorthiazide (Diuril) o Hyrochlorthiazide (Esixdrix o Hyrdodiuril) Loop Diuretics o Furosemide (Lasix) o Bumetamide (Burmex) Potassim-sparing o Spironolactone (Aldactone) o Triamterene (Dyrenium)
Teaching Plan Diet: o Sodium-restricted o Limit fats and cholesterol o Limit alcohol and fluids Stop ________________ NURSING MANAGEMENT Provide ________________ Promote rest and activity Decrease anxiety Facilitate fluid balance Provide skin care Promote nutrition Promote elimination Facilitate learning
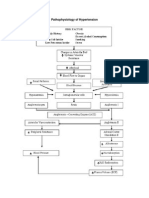
HYPERTENSION ________________ elevation of the arterial blood pressure CO x TPR Increased pressure may be the: o systolic o diastolic o both pressures A sustained pressure = hypertension: o systolic = 140 mmHg
VASODILATORS Decreases resistance to ventricular emptying, thereby decreasing ________________ Most commonly used as follows: o Nitroprusside (Nipride) o Hydralazine (Apresoline) o Nifedipine (a Calcium-channel blocker with vasodilator effect)
Lecture Aid: Medical-Surgical Nursing
Page 5 of 10
o Types:
diastolic = 90 mmHg
Antihypertensive drug therapy
Nursing Interventions ________________ / Essential / Idiopathic Unknown etiology Predisposing factors o Heredity o Age o Stress Secondary / Non-essential Secondary to other diseases Alcoholism Prolonged use of oral contraceptives ________________ crisis sudden elevation in blood pressure life-threatening Isolated systolic hypertension an elevation in systole only (>140 mmHg) affects elderly persons Record baseline BP in 3 positions (lying, sitting, standing) and in both arms Continuously assess BP and report any erratic change Administer antihypertensive agents as ordered o monitor closely and assess for S/E Monitor I & O Client teaching and discharge planning: o risk factors o dietary instructions o compliance of antihypertensive medications o routine follow up physician Report symptoms of complications: o Visual disturbances o Decreased urine output o Chest pains o Weakness or paresthesia
Collaborative Management Diet and weight reduction o restricted sodium o low cholesterol Lifestyle changes o alcohol moderation o exercise regimen o cessation of smoking ANEURYSM ________________ of blood vessel wall Types: o ________________ - involving all three layers of the vessel wall o ________________ - one side only
Lecture Aid: Medical-Surgical Nursing
Page 6 of 10
Collaborative Management Hypertension control Surgery o resection of the aneurysm and replacement with a Teflon/Dacron graft Nursing Interventions Prepare for surgery and implement postop care Watch out for signs of shock Advise client to prevent increased IAP RAYNAUDS DISEASE / RAYNAUDS PHENOMENON Characterized by intermittent ________________ with resultant ischemia in the extremities
Etiology and Incidence Commonly affected: ________________ ______________, 50-70 May be caused by: o Arteriosclerosis o Syphilis o Hypertension o Infection o Trauma to the BV
Manifestations Often asymptomatic Deep, diffuse chest pain Hoarseness Dysphagia Dyspnea Pallor Rupture = ________________
Etiology and Incidence Commonly affects digits of the hands ________________, 18 and 40 Risk factor: o Chemical pollutants o Cold environment o Cigarette smoking o Emotional stress Raynauds disease ____________ cause Hereditary 2 years history Raynauds phenomenon secondary to other disorders: o Occlusive arterial diseases o Connective tissue diseases
Diagnostic Test Aortography - exact location X-rays o chest film abnormal widening of aorta o abdominal film - calcification within walls of aneurysm
Lecture Aid: Medical-Surgical Nursing
Page 7 of 10
o o o
Primary pulmonary hypertension Hypothyroidism Neurologic diseases
o need to maintain warmth o Protection of the hands (gloves) Administer vasodilators as ordered THROMBOANGITIIS OBLITERANS (BUERGERS DISEASE)
Characterized by inflammatory changes in both ____________ and veins resulting in destruction of small and medium vessels Usually affects the ___________ extremities
Etiology and Incidence Exact cause: Unknown Men ages 25-40 Cigarette smoking Manifestations Intermittent ________________ Sensitivity to cold (skin may at first be white, changing to blue then red) Pulselessness Ulceration and gangrene (advanced) Collaborative Management Drugs: o Vasodilators - improve arterial circulation o Analgesics - relieve ischemic pain o Anticoagulants - prevent thrombus formation o Lipid reducing drug: cholestyramine, colestipol HCl, lovastatin (Mevacor), atorvastatin
Manifestations Pain (secondary to ischemia) Paresthesia Coldness Tingling in one or more digits Intermittent color changes (pallor, cyanosis) Small ulcerations Gangrene tips of digits Nursing Interventions Client teaching o importance of stopping smoking
Surgery o bypass grafting
Lecture Aid: Medical-Surgical Nursing
Page 8 of 10
o o
balloon catheter dilation amputation (if necessary)
Nursing Interventions Health teachings o stop smoking o Maintaining warmth Administer medications, as ordered. Prepare for surgery, if indicated. VENOUS THROMBOSIS (THROMBOPHLEBITIS) Refers to inflammation of a vein Precipitated by a thrombus formation Commonly occurs in the veins of the extremities: o Saphenous o Femoral o Popliteal
o o o o o o o o o o o o
Obesity CHF Immobility MI Pregnancy Oral contraceptives Trauma Sepsis Cigarette smoking Dehydration Severe anemias Complication of surgery
Types ______________________ o A stationary clot in deeper veins of the legs Superficial thrombophlebitis o inflammation of a vein closer to the surface o accompanied by formation of a stationary clot within the vein Phlebitis o inflammation of one or more veins without resultant clot formation.
Manifestations Pain in the affected extremity Superficial vein o Tenderness o Redness o Induration along course of the vein Deep vein o Swelling o Venous distension of limb o (+)____________ sign DVT and phlebitis may result in pulmonary embolism (when clot break off) o Sudden chest pain o Dyspnea o Decreased blood oxygen (Po2) o Agitation o Cyanosis o Tachycardia
Risk factors:
Lecture Aid: Medical-Surgical Nursing
Page 9 of 10
Collaborative Management Anticoagulants: Heparin Warfarin (coumadin) Nursing Interventions Deep Vein Thrombosis Assess respiratory and circulatory functions Admister medications, as prescribed: o Anticoagulant therapy o Thrombolytic therapy Avoid manipulation (eg. massage) Elevate the extremity Observe the extremity for edema Superficial thrombophlebitis Apply warm compresses over the affected site. Elevate the extremity. Administer anti-inflammatory agents, as prescribed. Health Teaching Avoid: o Standing & sitting for long periods o Constrictive clothing o Crossing legs at the knees o Smoking o Oral contraceptives Importance of adequate hydration Use of elastic stockings when ambulatory Importance of: o planned rest with elevation of feet
o weight reduction and exercise Institute postop care
Lecture Aid: Medical-Surgical Nursing
Page 10 of 10
You might also like
- Pathophysiology of HypertensionDocument54 pagesPathophysiology of HypertensionKaloy Kamao100% (3)
- Question 1 of 10: AAFP Board Review Clinchers Cardio Quiz 1Document53 pagesQuestion 1 of 10: AAFP Board Review Clinchers Cardio Quiz 1angel_sagun_1No ratings yet
- The Amazing Way to Reverse Heart Disease Naturally: Beyond the Hypertension Hype: Why Drugs Are Not the AnswerFrom EverandThe Amazing Way to Reverse Heart Disease Naturally: Beyond the Hypertension Hype: Why Drugs Are Not the AnswerRating: 5 out of 5 stars5/5 (2)
- U World Cardiac FinalDocument15 pagesU World Cardiac FinalAcohCChaoNo ratings yet
- Hyper+&+Hypothyroid+ +patho,+s S+causes+Document1 pageHyper+&+Hypothyroid+ +patho,+s S+causes+Bianca WelchNo ratings yet
- 1700 Subject Wise by PLAB Zillas (Bookmarked)Document380 pages1700 Subject Wise by PLAB Zillas (Bookmarked)hackchild100% (1)
- Understanding POTS - The Invisible IllnessDocument10 pagesUnderstanding POTS - The Invisible IllnessSpencer100% (1)
- Coronary Artery DiseaseDocument22 pagesCoronary Artery DiseaseMamoon RashidNo ratings yet
- Nails Diagnosis, Therapy, Surgery Richard K Scher MD, C Ralph DanielDocument319 pagesNails Diagnosis, Therapy, Surgery Richard K Scher MD, C Ralph DanieldrNo ratings yet
- Congestive Heart FailureDocument6 pagesCongestive Heart Failureseigelystic100% (1)
- Tell Me What to Eat If I Suffer from Heart Disease: Nutrition You Can Live WithFrom EverandTell Me What to Eat If I Suffer from Heart Disease: Nutrition You Can Live WithNo ratings yet
- Case Study (Heart Failure)Document18 pagesCase Study (Heart Failure)Maria Vanessa Lopez - BSN Level 3 A100% (1)
- User's Guide to Policosanol & Other Natural Ways to Lower Cholesterol: Learn about the Many Safe Ways to Reduce Your Cholesterol and Lower Your Risk of Heart DiseaseFrom EverandUser's Guide to Policosanol & Other Natural Ways to Lower Cholesterol: Learn about the Many Safe Ways to Reduce Your Cholesterol and Lower Your Risk of Heart DiseaseNo ratings yet
- Geria - CardioDocument4 pagesGeria - CardioLeah GordoncilloNo ratings yet
- Coronary Heart Disease (CHD) : By: Doaa Nassar, Saha Olama, Aidana Orazbay, Siba Al GumaDocument17 pagesCoronary Heart Disease (CHD) : By: Doaa Nassar, Saha Olama, Aidana Orazbay, Siba Al GumaDoaa NassarNo ratings yet
- CHN Non Communicable Diseases and OthersDocument90 pagesCHN Non Communicable Diseases and OthersEllenare Racion100% (1)
- Coronary Heart DiseaseDocument13 pagesCoronary Heart DiseaseLea Recto VinuyaNo ratings yet
- Coronary Artery DiseaseDocument33 pagesCoronary Artery DiseaseAlma Rifa'Ana LiskaNo ratings yet
- Peripheral Neuropathies in Clinical PracticeDocument398 pagesPeripheral Neuropathies in Clinical PracticeIka Gultom100% (1)
- Coronary Heart DiseaseDocument23 pagesCoronary Heart DiseaseBEA RADANo ratings yet
- Coronary Artery DiseaseDocument33 pagesCoronary Artery DiseasePratiwi AyuningtyasNo ratings yet
- CHD With NCPDocument10 pagesCHD With NCPJohanna Kirsten F. DaguioNo ratings yet
- Tallant ProjectDocument9 pagesTallant Projectapi-286576611No ratings yet
- CADword - Mam Jelu NogoyDocument15 pagesCADword - Mam Jelu Nogoyhan_angelaNo ratings yet
- Med Surg Unit 3 Exam ReviewDocument10 pagesMed Surg Unit 3 Exam ReviewIfy OhansonNo ratings yet
- Clinical Exposure Vi Assignment: Faculty of Medicine Universitas Pelita HarapanDocument16 pagesClinical Exposure Vi Assignment: Faculty of Medicine Universitas Pelita HarapanSteven MatualiNo ratings yet
- Prof - Dr.Medhat Ashmawy Professor of Cardiology, Tanta UniversityDocument104 pagesProf - Dr.Medhat Ashmawy Professor of Cardiology, Tanta UniversityIvana LmsNo ratings yet
- Cardiovascular DiseaseDocument9 pagesCardiovascular DiseaselizNo ratings yet
- PAD Handout 4thDocument27 pagesPAD Handout 4thdawitNo ratings yet
- Case Study 9Document7 pagesCase Study 9Lindsay WishmierNo ratings yet
- Geron CardioDocument45 pagesGeron CardioApril AlomiaNo ratings yet
- Lewis: Medical-Surgical Nursing, 8th EditionDocument7 pagesLewis: Medical-Surgical Nursing, 8th EditionJoyzoeyNo ratings yet
- Clinical Symptoms Due To Fluid CongestionDocument5 pagesClinical Symptoms Due To Fluid CongestionBrandedlovers OnlineshopNo ratings yet
- Nursing 4 Final ReviewDocument41 pagesNursing 4 Final Reviewemeraldwxyz100% (1)
- Coronary Artery Disease-Cad OR Ischaemic Heart Disease - IhdDocument99 pagesCoronary Artery Disease-Cad OR Ischaemic Heart Disease - IhdMwanja MosesNo ratings yet
- Coronary Artery Disease-Cad OR Ischaemic Heart Disease - IhdDocument99 pagesCoronary Artery Disease-Cad OR Ischaemic Heart Disease - IhdMwanja MosesNo ratings yet
- ARTHOSCLEROSISDocument7 pagesARTHOSCLEROSISMS AntikaNo ratings yet
- Coronary Atherosclerosis: Cardiovascular System: Coronary Vascular Disease Topics Discussed Here AreDocument6 pagesCoronary Atherosclerosis: Cardiovascular System: Coronary Vascular Disease Topics Discussed Here AreKamx MohammedNo ratings yet
- Coronary Heart DiseaseDocument12 pagesCoronary Heart DiseaseandeishaferminNo ratings yet
- Chapter 13 CirculationDocument27 pagesChapter 13 CirculationHerman ZoletaNo ratings yet
- Peripheral Vascular Disease: Dr. Fouzal Aswad, SPJPDocument46 pagesPeripheral Vascular Disease: Dr. Fouzal Aswad, SPJPRudy LusmiandaNo ratings yet
- Cardiac Lecture NotesDocument10 pagesCardiac Lecture NotesKateNo ratings yet
- Cardiovascular Agents: Florianne E. Adlawan, R.NDocument31 pagesCardiovascular Agents: Florianne E. Adlawan, R.NadlawanflorianneNo ratings yet
- Deep Vein Thrombosis (DVT)Document15 pagesDeep Vein Thrombosis (DVT)arcci balinasNo ratings yet
- Vascular Exam 4Document8 pagesVascular Exam 4SamanthaJonesNo ratings yet
- Prof - Dr.Medhat Ashmawy Professor of Cardiology, Tanta UniversityDocument104 pagesProf - Dr.Medhat Ashmawy Professor of Cardiology, Tanta UniversityThe department of cardiovascular medicineNo ratings yet
- PH CES For CAD Jan2018 FinalDocument28 pagesPH CES For CAD Jan2018 FinalrumasadraunaNo ratings yet
- Bhs Inggrs TransletDocument6 pagesBhs Inggrs TransletArif AshariNo ratings yet
- MR Moray BluntDocument7 pagesMR Moray Bluntbri ngNo ratings yet
- TOPIC1Chronic Forms of Coronary Heart DiseaseDocument3 pagesTOPIC1Chronic Forms of Coronary Heart DiseaseAdi PomeranzNo ratings yet
- Congestive Heart FailureDocument37 pagesCongestive Heart FailurePierre Aseron ManuelNo ratings yet
- Arterial Diseases 1Document32 pagesArterial Diseases 1ningappaNo ratings yet
- CVD DiscussionDocument6 pagesCVD Discussioncataleya mesaNo ratings yet
- Diagnosis and Treatment of Peripheral Arterial DiseaseDocument5 pagesDiagnosis and Treatment of Peripheral Arterial Diseasedrpiratheepan4274No ratings yet
- Hypertension: Medlineplus TopicsDocument31 pagesHypertension: Medlineplus TopicsMcNover Catlin OsamNo ratings yet
- Arterial ThrombosisDocument4 pagesArterial ThrombosisFaraida Jilzani ArsadNo ratings yet
- NSG 210 Study GuideDocument25 pagesNSG 210 Study GuideyasserNo ratings yet
- Ischemic Stroke g6Document8 pagesIschemic Stroke g6Kistnah Cassandra GapolNo ratings yet
- Coronary Artery Bypass Grafting: Coronary Bypass Surgery Is An Open-Heart Surgery, You MightDocument17 pagesCoronary Artery Bypass Grafting: Coronary Bypass Surgery Is An Open-Heart Surgery, You MightNuzhat FatimaNo ratings yet
- Courtney Broton Job 42 Flyer 1Document1 pageCourtney Broton Job 42 Flyer 1api-550569140No ratings yet
- Cardiovascular Lec DisordersDocument5 pagesCardiovascular Lec DisordersmagnacumlaudeNo ratings yet
- Pathologies Affecting Blood VesselDocument11 pagesPathologies Affecting Blood VesselroselynroukayaNo ratings yet
- PrelimsDocument11 pagesPrelimsJess Fabra100% (1)
- Advance Concept in Nursing Unit 3Document34 pagesAdvance Concept in Nursing Unit 3Kamran AltafNo ratings yet
- Unveiling the Unseen: A Journey Into the Hearts Labyrinth SeanFrom EverandUnveiling the Unseen: A Journey Into the Hearts Labyrinth SeanNo ratings yet
- For TzarsDocument8 pagesFor TzarsSyed Mohammed AfzalNo ratings yet
- New Microsoft Word DocumentDocument19 pagesNew Microsoft Word DocumentAisha FakhryNo ratings yet
- NOVA Vaccines Calling The ShotsDocument7 pagesNOVA Vaccines Calling The Shotslu naeNo ratings yet
- LegionellaDocument17 pagesLegionellaShubham Pareshkumar KadiwalaNo ratings yet
- Heart Gcse Qs OnlyDocument6 pagesHeart Gcse Qs OnlygriggansNo ratings yet
- Violence at WorkDocument20 pagesViolence at WorkNahmeshNo ratings yet
- ASEAN Diagnostic Criteria For Occupational Diseases PDFDocument60 pagesASEAN Diagnostic Criteria For Occupational Diseases PDFxpetronum100% (1)
- What If My Body Is BrilliantDocument39 pagesWhat If My Body Is BrilliantMaria SNo ratings yet
- Handbook of Low-Cost Interventions To Promote Physical and Mental Health: Theory, Research and Practice, in PressDocument24 pagesHandbook of Low-Cost Interventions To Promote Physical and Mental Health: Theory, Research and Practice, in PressVheey WattimenaNo ratings yet
- Define VitaminsDocument22 pagesDefine Vitaminsantesar reheemNo ratings yet
- Oncol Article JCRC 18Document9 pagesOncol Article JCRC 18EliDavidNo ratings yet
- ADA Cal en DT ADS001150 Rev01Document1 pageADA Cal en DT ADS001150 Rev01vijayramaswamyNo ratings yet
- Ppe 160505183246 PDFDocument38 pagesPpe 160505183246 PDFLakshmi PavaniNo ratings yet
- History of Abnormal Psychology Chap 2Document20 pagesHistory of Abnormal Psychology Chap 2ahmadNo ratings yet
- James Hupp, Head, Neck and Orofacial Infections. 2016-60-67Document11 pagesJames Hupp, Head, Neck and Orofacial Infections. 2016-60-67Hukjvccx JjyfdxxvbNo ratings yet
- Case of Nuclear SclerosisDocument32 pagesCase of Nuclear Sclerosismayan005No ratings yet
- Cancer Case StudyDocument3 pagesCancer Case Studyapi-311163159No ratings yet
- Module 4: Drug Education: Week 6Document62 pagesModule 4: Drug Education: Week 6Alyssa Joanna LlorinNo ratings yet
- Glaucoma OverviewDocument4 pagesGlaucoma OverviewSurya Cahyadi JunusNo ratings yet
- Acute Iron Poisoning - PharmacologyDocument10 pagesAcute Iron Poisoning - PharmacologyAmmaarah IsaacsNo ratings yet
- WJG 27 1691Document26 pagesWJG 27 1691Valentina QuinteroNo ratings yet
- Morning ReportDocument14 pagesMorning ReportAyu KristinaNo ratings yet
- PathophysiologyDocument5 pagesPathophysiologyJessyl GirayNo ratings yet
- Location Risk Assessment Form-Part A: Basic Information &: Hazard ListDocument4 pagesLocation Risk Assessment Form-Part A: Basic Information &: Hazard Listapi-330575448No ratings yet