Professional Documents
Culture Documents
Redictable and Precise Tooth Preparation Techniques For Porcelain Laminate Veneers in Complex Cases
Uploaded by
nobelcyrilOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Redictable and Precise Tooth Preparation Techniques For Porcelain Laminate Veneers in Complex Cases
Uploaded by
nobelcyrilCopyright:
Available Formats
CLINICAL
PREDICTABLE
AND PRECISE TOOTH PREPARATION TECHNIQUES FOR PORCELAIN LAMINATE VENEERS IN COMPLEX CASES
GALIP GREL
orcelain laminate veneers (PLVs) are one of the most conservative and aesthetic techniques that can be applied when restoring the mouth for improved aesthetics. The longevity of the veneers is good and they are durable, especially if the right indications are in place and the correct techniques are applied (Horn HR, 1983). The fundamental concept in any restorative case is to keep it simple and to concentrate on just one objective conservation of the sound tooth structure. Where the dentine-enamel junctions (DEJ) meet is very important in terms of the structural strength of the tooth: a complex fusion occurs at the DEJ that can be regarded as a fibre-reinforced bond (Lin CP, Douglas WH, Erlandsen SL, 1993). If preparation is limited to the enamel, there would be insufficient flexibility in the teeth (Magne P, Douglas WH, 1999). If the preparation line passes through the DEJ margin and enters into dentine, while it wont create a major problem, a number of difficulties may occur if one ends up finishing the preparation on large amounts of dentine. This will not only create complex bonding issues on dentine but will also free the flexing factor on the tooth structure (Noack MJ, Roulet J-F, 1987; Van Meerbeek B et al, 1996; Van Meerbeek B et al, 1998). When the tooth starts flexing, a new phenomenon occurs. Firstly, a tooth that has been aggressively prepared has a tendency to bend and the intention is to bond a veneer a porcelain material that is very rigid on top of that. Adhesive luting resin will be used in between those two structures, which will try to absorb all the stresses. If the tooth is subject to different occlusal forces and continues to flex, the luting resin at the margin will slowly start to peel off, and the clinician is likely to be faced with micro-leakage or de-lamination. To minimise these effects and problems, precision and care must be taken with case selection and tooth preparation (Belser UC, Magne P, Magne M, 1997). The best situation in which to place veneers is when the teeth are perfectly aligned on the
dental arch and the facial structures of the teeth are not worn, which happens with age.
Standard preparation technique
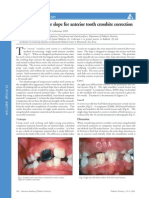
An amount of tooth structure, equivalent to the thickness of the veneer that will be placed on the tooth, should be removed. Since the shape, volume or contours of the tooth will not be changed, standard tooth preparation techniques can be used (Figures 1a, 1b and 1c) (Strub JR, Trp JC, 1999). When the exact depth needed for the porcelain build-up is removed, finishing the restoration should not pose any problems (Figures 2a, 2b and 2c). The procedure should begin with the use of a depth cutter (Garber DA, Goldstein RE, Feinman RA, 1988; Nixon RL, 1990; Garber DA, 1993), which indicates the exact depth that is to be prepared and which depends on the material selection or the colour of the tooth to be restored (Figures 3a and 3b). Once this is established, the surface of the tooth should be painted a different colour, after which a round-ended fissure bur is used to finalise the facial reduction. The important factor here is that the bur is used at three different angles in order to conform to the facial convexity of the tooth structure. It is only in this way that the dentist can achieve consistent thickness of the porcelain material, i.e. the porcelain build-up. Once this reduction has been performed, the preparation is finished at the gingival margin and then extended towards the papilla to finish the interproximal elbow preparation. This is important, especially when dealing with discolouration. If the depth is not prepared correctly, the connection between the dark-coloured tooth and the light-coloured porcelain will be visible when seen from an angle, which is clearly not aesthetically pleasing. To set up for this dogleg preparation, the bur is held at an angle of almost 60 towards the palate. Once the exact depth has been achieved, the bur should be held in an upright position to finish the interproximal preparation (Morley J, 1999). The butt joint preparation of the incisal edge should be omitted to give the laboratory technician enough room to build up the artistic, translucent, opalescence effects, incisal silhouette, etc (Figures 4a and 4b). As in every PLV case, the
Dr Galip Grel Private Practice, Istanbul, Turkey
30
INTERNATIONAL DENTISTRY SA VOL. 9, NO. 1
CLINICAL
1a
1b
1c
2a
2b
3a
3b
2c
4a
4b
Figure 1a: Teeth exhibiting large composite fillings. Figure 1b: Teeth are bleached. Note the colour difference between the bleached parts of the incisors and the existing composite fillings. Figure 1c: Note the existing large composites and cavity on the palatal side. Figures 2a and 2b: Finished and bonded veneers with facial and lingual view after two years. Figure 2c: Full smile and facial integration. Figure 3a: The retraction cord is placed in the sulcus to prevent soft tissue damage during tooth preparation and for better margin displacement during impression taking. First the depth cutters are used for exacting the depth of the preparation. Figure 3b: Standard tooth preparation. Figure 4a: The last reduction is from the incisal edges. The necessary depth is created with a fissure bur of choice by creating some ditches and then these are connected to each other to create a butt joint. Figure 4b: To finish the preparation the existing composites are removed and the margins are rounded. Figure 5: Previously built shell provisionals are tried in the mouth, then filled with composite and temporarily bonded onto the prepared teeth.
direct or prefabricated provisionals are placed after the impression has been taken (Figure 5).
What if the teeth are not aligned properly?
One of the major indications for using PLV is space management. It becomes more of a challenge if the teeth are spaced or not properly aligned on the dental arch - for example, in the case of crowding. The dentist is afced with two problems when the teeth are not aligned properly on the dental arch: 1. Visualising the aesthetic outcome 2. Tooth preparation.
Aesthetic communication
Creating natural-looking smiles When considering the approach for smile design, the dentist
undertakes to create a new, but natural aesthetic effect. With each restoration the patient must be considered as a whole, rather than focusing merely on one or two teeth. Each tooth exists as part of the mouth and face, contributing to the formation of a smile that reflects the patients personality. When creating a restoration, harmony in the size, shape and arrangement of the teeth is required to enhance each individual patients facial features. Once the teeth, the surrounding soft tissue and the patients facial characteristics are taken into consideration, a three-dimensional overview is needed. The dentist must be aware of the ratio between the anterior teeth and the surrounding tissue, and to analyse them to achieve the desired result. An aesthetic case may vary from the simple aesthetic contouring of a corner of a single tooth to the complete
INTERNATIONAL DENTISTRY SA VOL. 9, NO. 1 31
CLINICAL
Figure 6: The unaesthetic appearance of the smile, which is relatively dark in colour, has short crowns, uneven gingival levels, crowded incisors, an uneven incisal silhouette and a deciduous canine on the second quadrant.
Figure 7: Analysing the smile at an angle shows the crowding of the centrals.
Figure 8: From this view the AOP can easily be evaluated. The deciduous canines display a distinct concavity.
recreation of a new smile involving the entire dentition. The mouth and its physiological make-up for each individual patient must be studied carefully by the aesthetic dentist, who should analyse and anticipate any problems that may arise during the treatment. The first hurdle involves managing the patients expectations. What the patient wants and what the clinician can achieve needs to be successfully communicated. This communication and co-operation between the patient and the dentist will determine the success or failure of the treatment. The aesthetic dentist needs to be completely attuned to the patient, interpreting both verbal requests and the less obvious non-verbal cues. The dentist who is able to generate a confident, competent and observant manner will inspire confidence in the proposed treatment and help the patient to feel relaxed. The dentists perception of a desirable smile and the type of design should be discussed with the patient and be considered with their personal thoughts on their appearance. The patient may wish to reinstate a look that has been established over a long period of time or may request an alteration that is totally unrealistic for their face. Perhaps one of the most difficult tasks is selecting the right treatment in order to achieve successful aesthetic dentistry. It should be noted that one setback can easily erase many brilliant and successful procedures. The ability to say no will prevent problems. If the aesthetic dentist and patient find it difficult to agree on the propsed objectives, it is in the best interests of both parties not to begin the treatment.
even to people with no dental knowledge. Proportionally speaking, the existing teeth are short for the face and the gingival levels are uneven (Figure 6). 45 angle view (checking buccal-lingual dimension) This angle allows the dentist to check the crowding in a more reliable manner. In this case it is evident that the mesial incisal tip of 1 L is more buccally placed relative to tooth 1 L (Figure 7). However, at this very early stage it may not be possible to decide which incisal edge position to use as a reference point in a buccal-lingual dimension. Should tooth 1 be built up buccally or should tooth 1 L be brought L lingually? Aesthetic occlusal plane (AOP) The third dimension to be checked in the aesthetic evaluation is the AOP, which can simply be done from a saggital view. In this particular case, a deciduous canine exists (tooth L c ), which creates a problem related to the AOP since it is too short (Figure 8). At this point, it is preferable if the angulation of the centrals is perpendicular to the AOP.
Functional evaluation
Since the final restorations must be long lasting, their foundation is of great importance. When the root of the deciduous tooth L c was checked on the X-ray, it was obvious that it would not be able to withstand the lateral forces, especially during occlusion. Nor would it survive if canineguided occlusion is planned.
Analysing the smile
In order to have a clear visual idea of the final outcome, the existing smile should be analysed three-dimensionally. The facial view When the smile is analysed from a full-face perspective, only mesio-distal or vertical problems can be dealt with. In the second illustrated case it is evident that the centrals overlap, causing a vertical canting of the mid-line that is visible
32 INTERNATIONAL DENTISTRY SA VOL. 9, NO. 1
Treatment planning
At this stage, It is almost impossible to be sure of the final outcome just by looking at this case intra or extra-orally. With all these problems or imperfections in the mouth, the aesthetic final outcome should initially be visualised and realised and this knowledge or information shared with the patient. The first step towards achieving this is the composite mock-up (Dietschi D, 1995; Vanini L, 1996; Baratieri LN et al, 1998).
CLINICAL
10
11
Figure 9: The incisal edges are aligned with a composite mock-up and the incisal edge position is defined. Then a reverse mock-up is applied over the soft tissues in order to determine where the soft tissues should be after the perio operation. Meanwhile the length to width ratio of the teeth are carefully worked out. Figure 10: After perio surgery, a new mock-up is produced in order to gauge the new proportions and relations among the teeth more successfully. Figure 11: Teeth are bleached after crown lengthening. Note the altered gingival margins.
12
13
14
Figure 12: The final wax-up. Figure 13: A silicone index (SI) according to this wax-up is built to be used during the preparation stage. This SI is tried on the teeth. Note that SI can not be seated on the arch passively, due to the protruded position of the mesio-incisal corner of tooth 1 . Figure 14: In such situations, APR (aesthetic pre-recontouring) is carried out. The protruding surfaces of teeth that are positioned labially relative to the final contours of the finished PLVs are trimmed down until the silicone index can be passively seated on the dental arch. Note the trimmed mesio-incisal edge of tooth 1 and how passively the index is seated on the arch after the APR. In order to test the final outcome of the proposed smile design, the APTs (aesthetic preevaluative temporaries) have to be tested.
Mock-up
A simple freehand carved composite can be used to visualise the final outcome of the veneers, and one can see how the smile will look when these composites are placed (Figure 9). This does not need to be as precise as a wax-up but it will give the dentist an idea of how/where the length of these teeth should be, where to place the facial bulkiness and its effect on the lip structure, on phonetics and on occlusion (Peumans M et al 1998; Chiche GJ, Pinault A, 1994; Romano R, Bichacho N, Touati B, 2005). This mock-up will be a great tool or guide for the lab technician to build up his wax-up. At the end of the process, this information should be shared with the patient to confirm the first step towards a functional and aesthetic outcome (Dawson PE, 1989).
Second mock-up
However, in cases where the gingival levels need to be altered (which will change the length of the crown apically), it is always more reliable to make a second mock-up. This will illustrate the new proportions and the smile design more successfully than a reverse mock-up. Six to eight weeks after the perio surgery is finished, a new mock-up is produced (Figure 10). This second mock-up following the perio surgery will help the dentist and the ceramist design the teeth proportions in relation to the position of the new gingival margins. The new impression based on this mock-up is then sent to the ceramist for the wax-up. The new mock-up will provide the ceramist with more reliable information for the final wax-up.
34 INTERNATIONAL DENTISTRY SA VOL. 9, NO. 1
Another decision that can be made at this point is to prepare the deciduous canine L c and toothL 4 for crowns and connect them to each other for better support. This will result in a small group function (instead of canine only) through the canine and first premolar, which will also affect the design of the final wax-up. If necessary, the teeth can be bleached during this period (Figure 11). It is now evident that the incisal-mesial corner of tooth 1 L has to be positioned and restored lingually. The best choice of treatment would be to pull it back with orthodontics first and then to continue with minimal invasive techniques. However, time limitations for this specific case did not allow for such treatment planning. However, this situation should be communicated to the lab so that they know to trim that corner slightly inwards during the wax-up. At this stage, two impressions of the patient's dental arches must be taken: one of the original existing tooth structure with all diastemas and misaligned teeth, and the second with the mock-up. The lab technician should relate these two using a silicone index and finalise his wax-up with all the details, as though building up the porcelain restorations. The technician is now free to reduce the facial surface of the protruding teeth (in this case tooth 1 ) and then finish the wax-up according to the guidelines of the mock-up (Figure 12).
APR (aesthetic pre-recontouring)
At the next appointment when the patient comes for the tooth
CLINICAL
15a
15b
16
Figures 15a and b: An impression taken of the wax-up is filled with a flowable composite (or any material of choice) and placed on the unprepared teeth Figure 16: Completed smile design, before any tooth preparation is carried out (APT). This should now mimic the exact final contours, texture and shape of the final PLVs
preparation, the dentist should be provided with a silicone index (made from the wax-up model) that will indicate the final contours of the teeth. The index is then placed over the dental arch in order to visualise the existing positions of those teeth on the dental arch, relative to the final outcome of the wax-up and veneers (Figure 13). It may be possible to detect one problem at this stage: one or few teeth may touch or push the silicone index bucally, indicating that these teeth are either rotated or positioned more labially than the expected final outcome. Those teeth must then be trimmed down in order to place the silicone index passively on the dental arch in a process called APR (aesthetic pre-recontouring) (Gurel G, 2003a) (Figure 14).
APT (aesthetic pre-evaluative temporaries)
The wax-up can then be applied to the tooth structure while the provisionals are being made. The technique used is to make a transparent silicone impression from the wax-up and in the mouth, fill it with the flowable composite, then place it on the unprepared teeth; light cure it and take the translucent impression material out of the mouth (Figures 15a and b). This would not have been possible had the teeth been rotated or
positioned buccally, nor been recontoured with APR as the transparent impression wouldnt fit on those teeth. The gingival margins are then trimmed slightly to create, in plastic, the exact expected final outcome of the porcelain. Because the patient is not numbed, this is the best way to assess the aesthetic outcome (Figure 16). The lip support of these restorations and the aesthetic length can be evaluated easily, and should be approved by the patient. The functional movements of the patient must also be evaluated to see whether an anterior constriction is present, and if phonetics may be a problem in the future. Once this is approved by the patient, the dentist can move onto the next stage. The APT (aesthetic pre-evaluative temporaries) are no different from a provisional on the tooth structure before the teeth have been touched (Gurel G, 2003a; Gurel G 2003b; Gurel G, 2003c). These provisionals can then be double checked with silicone index to make sure that they are placed in the mouth correctly.
Tooth preparation in complicated cases
There is a second potential problem at this stage: what if the standard preparation technique cannot be used? When the teeth
17
18
19
Figure 17: Since the APT resembles the exact facial contours of the proposed smile design, now the tooth operation can be done through the APT. This will give the dentist and the ceramist the exact volume of reduction, hence being minimally invasive. Figure 18: Incisal reduction finished through the APT Figure 19: The final preparation. Note how the mesio-incisal corner of the tooth 1 had to be reduced more than all the other teeth due to its protrusive. position. Hence all the other teeth are minimally prepped with almost all the enamel left intact on their surfaces
20
21
22
Figure 20: The deciduous canine c and the premolar 4 are prepped to receive crowns connected to each other in order to support the functional loads, especially during the excursions. Note the 360 champher all around the gingival margin. Figure 21: The final check for preparation depth of the veneers as well as the crowns with the SI. Figure 22: Provisional temporarily bonded in the mouth, replicating the final result exactly.
36
INTERNATIONAL DENTISTRY SA VOL. 9, NO. 1
CLINICAL
23a
23b
Figures 23a and b: The smile from different angles.
are not aligned properly into the dental arch (the teeth may have rotations or may be placed lingually or buccally), how can the final success of that case be assessed and the teeth prepared precisely and predictably every time?
Tooth preparation through APT
The beauty of these aesthetic provisional temporaries, besides the evaluation of aesthetic functions and phonetic aspects, is that the dentists have a great tool at their disposal to prepare the teeth. They can simply use these APTs as a guideline for preparing tooth structure. APT resembles the exact contours of the final outcome. such as the incisal edge position and the facial volume (contours) of the teeth. Since everything is already set in advance, preparation of the teeth through the APT can begin as if though dealing with a simple case where the teeth are aligned properly, . At this point, it is of no consequence how the teeth are aligned underneath (Gurel G, 2003a) (Figures 17 and 18). In some situations, the tooth surface may not be prepared if, for example, the tooth is too palately placed (i.e. more than 0.6 mm away from the facial contours of the APT). Once the major reduction with the depth cutters is made, followed by the round ended fissure burs, the major facial volume reduction will be completed. The gingival margins and interproximal lines can then be finished. With rare cases such as this, if a substractive correction was done on the wax-up stage, far more tooth structure would be removed than would for a standard preparation depth, and tooth 1 L gets a substractive correction. The mesial incisal corner is prepared aggressively in order to align it properly, while the facial contours of the expected dental arch are formed as planned after the veneers are finished. As mentioned previously, the best way of handling such a case is to prealign the position of such teeth orthodontically before beginning the preparations. The same reduction will be carried out on the incisal edge and surprisingly, most of the time, it is unnecessary to prepare too much incisal healthy tooth structure (Castelnuovo J et al, 2000) (Figure 19). In PLV preparation the dentists tend to finish the gingival champher supragingivally unless they are dealing with a severe discolouration or with spaced dentition. After finishing the tooth preparation for the veneers, deciduous canine L c and first premolar tooth L 4 can be prepared for the all ceramic crowns. They will then be connected to each other for functional support and a small group function for the lateral excursions (Figure 20).
38 INTERNATIONAL DENTISTRY SA VOL. 9, NO. 1
Once the preparation is finished, the same silicone index is used once more to check and verify the correct preparation depths (Figure 21). The impression is made and the provisionals are fabricated. The provisionals should be exactly the same as the APT as this will be a second chance for the patient to assess the final outcome during the fabrication (Figure 14).
The lab procedures
The veneers can be fabricated with feldspathic porcelain on a refractory die, or on platinum foil. Alternatively, one can use pressable ceramics with external staining or layering techniques. In this case, the pressable porcelain will be used with the layering technique. Whichever technique is used, it is important that the ceramist uses the same silicone index that was used in the mouth, which fits perfectly on the APT that was approved as the final outcome. The rest is down to the ceramists knowledge, ability and talent for integrating the colours, form, shape and texture.
Try in
When the veneers arrive from the lab, they should first be tried in the mouth. Preferably, the provisionals should be taken out and PLVs tried in without anaesthesia, making it easier to check the lip support and the incisal edge position relative to the upper lip. The veneers should initially be tried one by one in order to check the marginal fit accurately, and then together, to see their overall integration with each other, with the lips and finally, with the face.
Bonding
The author prefers a sectional rubber dam placed in the mouth. Once the teeth and the inside of the veneers are surface treated they can be bonded two by two. Preferably, the bonding should start with the centrals, proceeding with the lateral, canine on one side and then the lateral, canine on the other side. The soft tissues should be handled very gently. The easiest way to do that is to place the veneer on the tooth and once it is completely seated, spot tack it from the middle third with a 2mm turbo tip; this will hold the veneer in place. Then switch the tip of the light source to a larger diameter such as 13mm and light cure the excess flesh around the gingiva for only one or two seconds. This will not fully polymerise the luting resin but bring it to a jelly-like consistency, which can be easily cleaned with an explorer dipped
CLINICAL
24
25
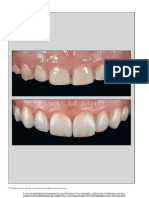
Figures 24 and 25: Full face before and after.
into an adhesive liquid. The interproximal contacts can then be cleansed using dental floss between the veneers. Once everything is completed, the luting resin can be fully polymerised. In order to finalise the bonding procedure, a # 12 blade will help to clean the undetected remaining composite on the margins. If necessary, the margins can be polished with a rubber cup. Using a diamond bur should be avoided as it would totally ruin the glaze and polish of the porcelain on the margins. The PLVs final position, form, phonetics, lip support is guaranteed as the same aesthetic, functional and phonetic results established during the APT and provisionalisation will be the same after the PLVs are bonded (Figures 15a and 15b).
Summary
The PLV is one of the most common aesthetic restorations. Even though it is one of the most conservative of treatment options, some rules have to be followed. Aesthetics is a very objective subject and necessitates excellent communication between the dentist, patient and ceramist. The case has to be carefully selected and treatment planned. The use of the mock-ups, followed by a wax-up, APT and silicone index will not only allow the dentist to achieve the best aesthetic, phonetic and functional outcome, but also to communicate this to the patient. More importantly, it results in minimum invasion of the recipient tooth. The use of PDP (permanent diagnostic provisionals) will have a further impact on this solid communication. That way, the patient will have a chance to evaluate the aesthetics, function and phonetics themselves as well as within their immediate circles (Figures 24 and 25).
Acknowledgements
Special thanks to Ulrich Werder MDT for the first case and Shigeo Kataoka RDT for the second case.
Baratieri LN et al (eds) (1998) Direct Adhesive Restorations on Fractured Anterior Teeth. Chicago: Quintessence Belser UC, Magne P, Magne M (1997) Ceramic laminate veneers: Continuous evolution of indications. J Esthet Dent; 9: 197-207 Castelnuovo J, Tjan AH, Phillips K, Nicholls JI, Kois JC (2000) Fracture load and mode of failure of ceramic veneers with
References
different preparations. J Prosthet Dent; 83:171-180 Chiche GJ, Pinault A (1994) Esthetics of Anterior Fixed Prosthodontics. Chicago: Quintessence Dawson PE (1989) Evaluation, Diagnosis and Treatment of Occlusal Problems (2nd edition). St Louis: Mosby Dietschi D (1995) Free-hand composite resin restorations: A key to anterior aesthetics. Pract Periodont Aesthet Dent; 7:15-25 Garber DA (1993) Porcelain laminate veneers: 10 years later. Part 1. Tooth preparation. J Esthet Dent; 5: 56-62 Garber DA, Goldstein RE, Feinman RA (1998) Porcelain laminate veneers. Chicago: Quintessence Gurel G (2003a) The Science and Art of Porcelain Laminate Veneers. Chicago: Quintessence Gurel G (2003b) Predictable, precise and repeatable preparation for porcelain laminate veneers. Pract Proced Aesthet Dent; 15(1):17-24 Gurel G (2003c) Predictable tooth preparation for porcelain laminate veneers in complicated cases. Quint Dent Tech; 26:99-111 Horn HR (1983) Porcelain laminate veneers bonded to etched enamel. Dent Clin North Am; 27: 67-684 Lin CP, Douglas WH, Erlandsen SL (1993) Scanning electron microscopy of type I collagen at the dentin-enamel junction of human teeth. J Histochem Cytochem; 41: 381-388 Magne P. Douglas WH (1999) Porcelain veneers: Dentin bonding optimization and biomimetic recovery of the crown. Int J Prosthodont; 12: 111-121 Morley J (1999) The role of cosmetic dentistry in restoring a youthful appearance. J Am Dent Assoc; 130: 1166-1172 Nixon RL (1990) Porcelain veneers. An esthetic therapeutic alternative. In: Rufenacht CR. Fundamentals of Esthetics. Chicago: Quintessence, pp329-68 Noack MJ, Roulet J-F (1987) Rasterelelektronenmikroskopische Beurteilung der Atzwirkung verschiedener Atzgele auf Schmelz. Dtsch Zahnarztl Z; 42: 953-959 Peumans M, Van Meerbeek B, Lambrechts P, Vanherle G, Quirynen M (1998) The influence of direct composite additions for the correction of tooth form and/or position on periodontal health: A retrospective study. J Periodontal; 69:422-427 Romano R, Bichacho N, Touati B (eds) (2005) The Art of the Smile. Chicago: Quintessence Strub JR, Trp JC (1999) Esthetics in dental prosthetics. In: Fischer J, Esthetics and Prosthetics. Chicago: Quintessence Vanini L (1996) Light and color in anterior composite restorations. Pract Periodont Aesthet Dent; 8:673-682Van Meerbeek B, Peumans M, Gladys S et al (1996) Three-year clinical effectiveness of four total-etch dentinal adhesive systems in cervical lesions. Quint Int; 27: 775-784 Van Meerbeek B, Perdigao J, Lambrechts P et al (1998) The clinical performance of adhesives. J Dent; 26: 1-20
40
INTERNATIONAL DENTISTRY SA VOL. 9, NO. 1
You might also like
- 10 1016@j Cden 2007 03 007 PDFDocument13 pages10 1016@j Cden 2007 03 007 PDFsnehal jaiswalNo ratings yet
- Minimall Tooth Preparation Garil GurelDocument13 pagesMinimall Tooth Preparation Garil GurelMónica BecerraNo ratings yet
- Mclaren Smile AnalysisDocument15 pagesMclaren Smile AnalysisXavier Vargas PerezNo ratings yet
- Faculty of Dentistry Prosthodontic DepartmentDocument23 pagesFaculty of Dentistry Prosthodontic DepartmentKarim MagdiNo ratings yet
- Smile DesignDocument7 pagesSmile DesignDanilo Macam100% (1)
- Guideline For Veneer PrepDocument8 pagesGuideline For Veneer Prepnobelcyril100% (1)
- Class 4 Composite RepairDocument8 pagesClass 4 Composite RepairventynataliaNo ratings yet
- Factores Macroesteticos en El Diseño de SonrisaDocument7 pagesFactores Macroesteticos en El Diseño de SonrisaJassel DurdenNo ratings yet
- Orthodontically Assisted Restorative Dentistry: Donald F. Reikie, DDS, MSDocument5 pagesOrthodontically Assisted Restorative Dentistry: Donald F. Reikie, DDS, MSAdityaNo ratings yet
- Diastema Closure A Restorative Design and Treatment ChallengeDocument10 pagesDiastema Closure A Restorative Design and Treatment ChallengeDiana SuhartiNo ratings yet
- Discovering The Artist Inside A Three-Step Approach To Predictable Aesthetic Smile Designs, Part 1Document13 pagesDiscovering The Artist Inside A Three-Step Approach To Predictable Aesthetic Smile Designs, Part 1ilich sevillaNo ratings yet
- Esthetic in Complete DentureDocument14 pagesEsthetic in Complete DentureNidhi KatochNo ratings yet
- Smile Design Dental PhotographyDocument3 pagesSmile Design Dental Photographydranilshinde100% (2)
- Advanced Smile Design ArticleDocument4 pagesAdvanced Smile Design ArticleShounak GhoshNo ratings yet
- ORTHODONTIADocument10 pagesORTHODONTIArbNo ratings yet
- Case ReportDocument10 pagesCase ReportwidhariyaniNo ratings yet
- Dental Wax UpDocument4 pagesDental Wax UpJoselyn RodriguezNo ratings yet
- 12-Aesthetics in Removable Prosthodontics - MahmoudDocument39 pages12-Aesthetics in Removable Prosthodontics - Mahmoudhassan.h.h.elhusseinyNo ratings yet
- Smile Design With Composites: A Case Study: ClinicalDocument5 pagesSmile Design With Composites: A Case Study: ClinicalDavid ColonNo ratings yet
- Complete Denture Fabrication For Old Denture Wearer in One DayDocument3 pagesComplete Denture Fabrication For Old Denture Wearer in One DayAsma Akram - ProsthodonticsNo ratings yet
- Principles of Composit Restoration: Written By: DR Aakash Bari BDSDocument9 pagesPrinciples of Composit Restoration: Written By: DR Aakash Bari BDSBari AakashNo ratings yet
- Additive Contour of Porcelain Veneers A Key Element in Enamel PreservationDocument13 pagesAdditive Contour of Porcelain Veneers A Key Element in Enamel PreservationPablo BenitezNo ratings yet
- IRA Klein,: Mmedmte Denture ServiceDocument11 pagesIRA Klein,: Mmedmte Denture ServiceClaudia AngNo ratings yet
- Smile DesignDocument104 pagesSmile DesignEazhil Raj100% (3)
- Dentist-Ceramist Communication Protocols For An Effective Esthetic Team Finkel2020Document12 pagesDentist-Ceramist Communication Protocols For An Effective Esthetic Team Finkel2020everaldocruzNo ratings yet
- Orthodontic Treatment of Mandibular Anterior Crowding: Key Words: Crowding, Malocclusion, Labial FlaringDocument4 pagesOrthodontic Treatment of Mandibular Anterior Crowding: Key Words: Crowding, Malocclusion, Labial FlaringDunia Medisku OnlineShopNo ratings yet
- Instant OrthoDocument4 pagesInstant OrthoSmart DentalNo ratings yet
- AbcDocument4 pagesAbcAquinnaNo ratings yet
- Single Complete DentureDocument55 pagesSingle Complete DentureFie ZainNo ratings yet
- Individual Tooth Selection Process: ExchangeDocument3 pagesIndividual Tooth Selection Process: ExchangeAlfredo RamzNo ratings yet
- Periodontal Plastic Surgery For Treatment of GummyDocument6 pagesPeriodontal Plastic Surgery For Treatment of GummyLilian CalianiNo ratings yet
- Lecture No8 Drnidhal 2017 Treatment PlaningDocument9 pagesLecture No8 Drnidhal 2017 Treatment PlaningQueen LiveNo ratings yet
- ContentServer Asp-6Document9 pagesContentServer Asp-6ValentinaNo ratings yet
- The Orthodontics Effective RoleDocument31 pagesThe Orthodontics Effective RoleHamza BelhajNo ratings yet
- Smile Design Pada Penutupan Diastema Menggunakan Veneer PorselinDocument4 pagesSmile Design Pada Penutupan Diastema Menggunakan Veneer Porselinmaharani spNo ratings yet
- Format JurnalDocument14 pagesFormat JurnalAnonymous HtTD0BNo ratings yet
- QDT 2001 PDFDocument239 pagesQDT 2001 PDFAlex BurdeNo ratings yet
- Veneers. Fantasy. Risk. Success SampleDocument59 pagesVeneers. Fantasy. Risk. Success SampleDental Technician ЗУБНЫЕ ТЕХНИКИ100% (1)
- ORTODONCIADocument10 pagesORTODONCIAOrlando RodríguezNo ratings yet
- Improving Aesthetics in Patients With Complete DenturesDocument4 pagesImproving Aesthetics in Patients With Complete DenturesMohsin HabibNo ratings yet
- Increasing Vertical DimensionDocument6 pagesIncreasing Vertical DimensionAriel AcevedoNo ratings yet
- Anterior Esthetic Restorations Using Direct Composite Restoration A Case ReportDocument6 pagesAnterior Esthetic Restorations Using Direct Composite Restoration A Case ReportkinayungNo ratings yet
- VeneerDocument48 pagesVeneerAli IhsanNo ratings yet
- Porcelain VeneersDocument42 pagesPorcelain VeneersShu Nser100% (1)
- 54.individualizing A Smile Makeover. Cur PDFDocument14 pages54.individualizing A Smile Makeover. Cur PDFEduardo AyubNo ratings yet
- Smile Design Concepts and RequirementsDocument7 pagesSmile Design Concepts and RequirementsZahra ZaNo ratings yet
- Smile DesignDocument20 pagesSmile DesignAmit100% (1)
- Article-PDF-sandeep Garg Sushant Garg Mohit Mehta Sangeeta Goyal-286Document3 pagesArticle-PDF-sandeep Garg Sushant Garg Mohit Mehta Sangeeta Goyal-286Mrunal DoiphodeNo ratings yet
- 13.esthetic Rehabilitation of Maxillary Anterior Teeth - A Case ReportDocument3 pages13.esthetic Rehabilitation of Maxillary Anterior Teeth - A Case ReportnadeemNo ratings yet
- Planning and Orthodontic Preparation For Maxillary Incisors ReshapingDocument39 pagesPlanning and Orthodontic Preparation For Maxillary Incisors ReshapingJuliana SalasNo ratings yet
- Crown Preparation For StudentDocument6 pagesCrown Preparation For StudentadindayokopNo ratings yet
- Polack2013 BiotypechangePolackMahnDocument10 pagesPolack2013 BiotypechangePolackMahnAndré Pinheiro de AraújoNo ratings yet
- The Single-Tooth RestorationDocument5 pagesThe Single-Tooth Restorationumerjaved86No ratings yet
- Treatment Planning Single Maxillary Anterior Implants for DentistsFrom EverandTreatment Planning Single Maxillary Anterior Implants for DentistsNo ratings yet
- Smile Design: Nicholas C. Davis, DDS, MAGDDocument20 pagesSmile Design: Nicholas C. Davis, DDS, MAGDPriyanka GandhiNo ratings yet
- Non Preparation VeneersDocument24 pagesNon Preparation VeneersastinejenniferNo ratings yet
- Compomer CrownDocument2 pagesCompomer CrownIndah SimamoraNo ratings yet
- Fisa Observatie ProteticaDocument5 pagesFisa Observatie ProteticaBuzatu IonelNo ratings yet
- Esthetic Oral Rehabilitation with Veneers: A Guide to Treatment Preparation and Clinical ConceptsFrom EverandEsthetic Oral Rehabilitation with Veneers: A Guide to Treatment Preparation and Clinical ConceptsRichard D. TrushkowskyNo ratings yet
- Adin Catalog PDFDocument88 pagesAdin Catalog PDFnobelcyrilNo ratings yet
- 2 Pediatric EndodonticsDocument12 pages2 Pediatric EndodonticsnobelcyrilNo ratings yet
- 3 Recent Advances in Irrigation SystemsDocument12 pages3 Recent Advances in Irrigation SystemsnobelcyrilNo ratings yet
- Endodontic InstrumentssDocument35 pagesEndodontic InstrumentssnobelcyrilNo ratings yet
- Journal of Advanced Clinical and Research InsightsDocument6 pagesJournal of Advanced Clinical and Research InsightsJeliny Bintan MaisuriNo ratings yet
- A OcclusionDocument112 pagesA OcclusionSaowalak Koosriteppratan100% (1)
- Journal of Advanced Clinical and Research InsightsDocument6 pagesJournal of Advanced Clinical and Research InsightsJeliny Bintan MaisuriNo ratings yet
- Implant Abutment NeckDocument7 pagesImplant Abutment NecknobelcyrilNo ratings yet
- Bone Augmentation TechniquesDocument20 pagesBone Augmentation TechniquesGabriela Ciornei100% (1)
- Journal of Advanced Clinical and Research InsightsDocument6 pagesJournal of Advanced Clinical and Research InsightsJeliny Bintan MaisuriNo ratings yet
- Comparative Study Between Three Different Conections For Dental ImplantsDocument10 pagesComparative Study Between Three Different Conections For Dental ImplantsnobelcyrilNo ratings yet
- Bacterial Seal ConnectionDocument6 pagesBacterial Seal ConnectionnobelcyrilNo ratings yet
- Journal of Advanced Clinical and Research InsightsDocument6 pagesJournal of Advanced Clinical and Research InsightsJeliny Bintan MaisuriNo ratings yet
- Jaw AnatomyDocument17 pagesJaw AnatomynobelcyrilNo ratings yet
- History and Bone PropertiesDocument59 pagesHistory and Bone PropertiesnobelcyrilNo ratings yet
- Good Bone GraftDocument24 pagesGood Bone GraftnobelcyrilNo ratings yet
- More Detailed Bone Healing MachanismDocument24 pagesMore Detailed Bone Healing MachanismnobelcyrilNo ratings yet
- Obtaining Impressions For The Clinically Successful Implant-Supported RestorationDocument6 pagesObtaining Impressions For The Clinically Successful Implant-Supported RestorationnobelcyrilNo ratings yet
- Biology of Implant OsseointegrationDocument11 pagesBiology of Implant OsseointegrationAmIrNo ratings yet
- Easy Graft: "The Bone Graft Substitute Beta-TCP in Oral Surgery and Dental Applications"Document21 pagesEasy Graft: "The Bone Graft Substitute Beta-TCP in Oral Surgery and Dental Applications"Dentapex ThailandNo ratings yet
- Easy Graft: "The Bone Graft Substitute Beta-TCP in Oral Surgery and Dental Applications"Document21 pagesEasy Graft: "The Bone Graft Substitute Beta-TCP in Oral Surgery and Dental Applications"Dentapex ThailandNo ratings yet
- Designing AbutmentsDocument5 pagesDesigning AbutmentsnobelcyrilNo ratings yet
- Alveolar Distraction For ImplantsDocument17 pagesAlveolar Distraction For ImplantsPoornima SoujanyaNo ratings yet
- Full Mouth Rehabilitation of The Patient With Severly Worn Out Dentition A Case Report.Document5 pagesFull Mouth Rehabilitation of The Patient With Severly Worn Out Dentition A Case Report.sivak_198100% (1)
- Altering VR in Full Mouth RehabiltationDocument7 pagesAltering VR in Full Mouth RehabiltationnobelcyrilNo ratings yet
- Alveolar Distraction For ImplantsDocument17 pagesAlveolar Distraction For ImplantsPoornima SoujanyaNo ratings yet
- Bone Augmentation TechniquesDocument20 pagesBone Augmentation TechniquesGabriela Ciornei100% (1)
- SuturesDocument20 pagesSutureskirank_11No ratings yet
- Jada 2003 Vernillo 24S 33SDocument10 pagesJada 2003 Vernillo 24S 33SnobelcyrilNo ratings yet
- Ferrule EffectDocument5 pagesFerrule EffectnobelcyrilNo ratings yet
- The Transcendent ManDocument48 pagesThe Transcendent Manapi-26032005No ratings yet
- Removable Partial Denture SurveyorDocument73 pagesRemovable Partial Denture SurveyorJay-r Deraya Don100% (2)
- How To Bond Zirconia - The APC Concept PDFDocument9 pagesHow To Bond Zirconia - The APC Concept PDFKelly Katherine0% (1)
- Composite Resin Layering and Placement TechniquesDocument7 pagesComposite Resin Layering and Placement TechniquesenimaNo ratings yet
- Crowns and Other Extra-Coronal RestorationDocument116 pagesCrowns and Other Extra-Coronal RestorationDennis La Torre Zea100% (4)
- Partial Porcelain Veneer Restoring Maxillary Incisor With Class II CavityDocument6 pagesPartial Porcelain Veneer Restoring Maxillary Incisor With Class II Cavityfanny rizky andriyaniNo ratings yet
- The Road To HollywoodDocument48 pagesThe Road To Hollywoodapi-26032005No ratings yet
- Nixon Porcelain Veneer Kit II: Technique GuideDocument6 pagesNixon Porcelain Veneer Kit II: Technique GuideYuttapol PimpisonNo ratings yet
- Manuale HRI Rondoni Ing v.2.2!11!2010 - MQDocument24 pagesManuale HRI Rondoni Ing v.2.2!11!2010 - MQDiego ArriagadaNo ratings yet
- Recent Advances in Materials For All-Ceramic RestorationsDocument19 pagesRecent Advances in Materials For All-Ceramic RestorationsManishak YessayanNo ratings yet
- Fixed Prosthetics WorkbookDocument23 pagesFixed Prosthetics WorkbookEliza EllieNo ratings yet
- The Art and Science of Aesthetic Dentistry. Part One: Smile DesignDocument6 pagesThe Art and Science of Aesthetic Dentistry. Part One: Smile DesignMohamed EladawyNo ratings yet
- RelyX UltimateDocument16 pagesRelyX UltimatedwNo ratings yet
- Ceramic in DentistryDocument6 pagesCeramic in DentistryDilesh PradhanNo ratings yet
- Venus Fahl PPAD 20061018Document6 pagesVenus Fahl PPAD 20061018RedhabAbbassNo ratings yet
- Evolution of Aesthetic DentistryDocument11 pagesEvolution of Aesthetic DentistrySMART SMARNo ratings yet
- 1 4990365184607387726 PDFDocument3,277 pages1 4990365184607387726 PDFAnurtha Anu75% (4)
- Aesthetic Rehabilitation According To The Visagism Concept: Dimitar Filtchev Indirect AnteriorsDocument23 pagesAesthetic Rehabilitation According To The Visagism Concept: Dimitar Filtchev Indirect Anteriorsmaroun ghalebNo ratings yet
- A Simplified Approach For Restoration of Worn Dentition Using The Full MockDocument10 pagesA Simplified Approach For Restoration of Worn Dentition Using The Full MockHaCem SahbaniNo ratings yet
- Esthetic Excellence PDFDocument32 pagesEsthetic Excellence PDFZomba ZombariraNo ratings yet
- Estudio Ce - Novation ZirconioDocument8 pagesEstudio Ce - Novation ZirconioHugo MoralesNo ratings yet
- Vailati Masterclass: Course Program ITDocument13 pagesVailati Masterclass: Course Program ITItalo TorresNo ratings yet
- VeneerDocument48 pagesVeneerAli IhsanNo ratings yet
- Closure of Midline Diastema by Direct Composite Resin Build-Up Using A Customized Matrix Technique - A Case ReportDocument4 pagesClosure of Midline Diastema by Direct Composite Resin Build-Up Using A Customized Matrix Technique - A Case ReportMuchlis Fauzi ENo ratings yet
- Ideal For Combined Restorations Vivid Individual Esthetics: Neo - LignDocument6 pagesIdeal For Combined Restorations Vivid Individual Esthetics: Neo - LignDumitru CrîşmariNo ratings yet
- Integrating Esthetic Dentistry and Space Closure in Patients With Missing Maxillary Lateral IncisorsDocument14 pagesIntegrating Esthetic Dentistry and Space Closure in Patients With Missing Maxillary Lateral IncisorsAly OsmanNo ratings yet
- Consent Cosmetic TreatmentDocument2 pagesConsent Cosmetic Treatmentd. g.No ratings yet
- Laminate VeneerDocument51 pagesLaminate VeneerZiad OthmanNo ratings yet
- Adhesive Ceramic Restorations: A Conservative Journey in Fixed ProsthodonticsDocument3 pagesAdhesive Ceramic Restorations: A Conservative Journey in Fixed ProsthodonticsCynthia PerezNo ratings yet
- Smile DesignDocument104 pagesSmile DesignEazhil Raj100% (3)